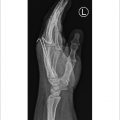
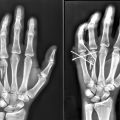
33 Middle/Proximal Phalanx (Open Reduction and Internal Fixation)
Abstract
Proximal and middle phalangeal fractures can usually be treated with nonsurgical methods. However, in cases when rotational or angular deformity is noted, or an unstable fracture pattern is seen, operative fixation is recommended. A dorsal or midlateral approach can be used. Plate fixation with locking or nonlocking screws can restore excellent stability and allow for early motion. Percutaneous or open-lag screw fixation can avoid the need for plate fixation in long oblique or spiral fracture patterns. Shortterm immobilization with early occupational therapist supervised motion protocol is started. Splinting is discontinued at 4 to 6 weeks or when fracture healing is confirmed radiographically.
33.1 Introduction
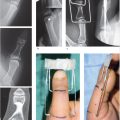
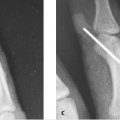
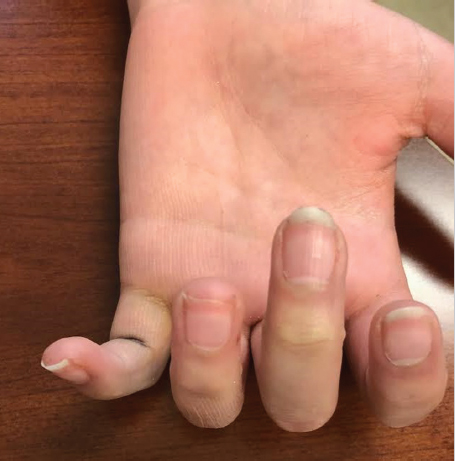
Proximal and middle phalangeal fractures often cause rotational or angular deformity (► Fig. 33.1). Cascade preservation is important for appropriate restoration of hand function. As little as 5 degrees of rotational malalignment can lead to significant finger overlap. The proper tendon balance relies on anatomical length of the phalanx to avoid extensor lag or incomplete flexion. Multiple fixation options exist for middle and proximal phalangeal fractures.
33.2 Goals
As union and healing of osseous structures completes with high success in the hand, goals are focused on restoring anatomical alignment and allowing early motion. Injuries involving the fingers can lead to stiffness even with a brief period of immobilization; hence, motion that allows tendon gliding and joint range should be started as soon as bony stability allows.
33.3 Indications
Open reduction and internal fixation should be considered in cases where nonsurgical management or percutaneous treatment would not allow adequate stability for bone healing. Proper evaluation of bony alignment is paramount in deciding to treat phalangeal injuries surgically. This requires adequate radiographic imaging with X-rays and scrutinizing the digital cascade through the full range of motion. Displaced condylar fractures, unstable spiral fractures, basilar fractures with joint incongruence and displacement or articular involvement, as well as appreciated angular deformity affecting the digital cascade should be operatively treated. More than 5-10 degrees of malrotation or coronal malalignment should be corrected. Sagittal plane deformities are much better tolerated and apex dorsal angle of up to 30 degrees and apex volar angle of 20 degrees may be acceptable if overall motion is preserved. Greater than 1mm articular incongruence should be reduced to restore the joint line. 1
33.4 Contraindications
Contaminated wounds and inadequate tissue coverage are reasons to avoid fixation with permanent implants such as screws and plates. In the case of infected tissues, without the prior eradication of pathogenic materials implant use should be avoided. Although not an absolute contraindication, in the case of digital replantation and other complex procedures, open reduction and internal fixation with plates and screws is generally avoided dude to the length of time it takes to perform this procedure.
33.5 Alternate Procedures
Alternate fixation techniques are recommended in cases where implant fixation is not desired, such as in pediatric patients, grossly contaminated or infected fractures, and injuries with large soft tissue defects or lack of coverage. In these cases, pin or Kirschner wire (K-wire) fixation is generally preferred. In cases where the zone of fracture is to be avoided, external fixators can play a role.
33.6 Operative Detail
33.6.1 Preparation: Planning/Special Equipment
Preoperative planning is essential in deciding the type of fixation, implant selection and approach. Mini C-arm availability is required. Instrumentation for K-wire fixation is needed as well. Even in the case of planned closed reduction pin fixation, implants for open reduction and internal fixation (ORIF) should be present if the fracture requires open treatment with internal fixation. Some implants allow for nonlocking constructs, whereas others allow for locked screw fixation that is helpful in periarticular fractures. Fixed or variable angle fixation options are available depending on the implant manufacturer. Furthermore, various size screw options exist. Based on the size of the bone, screw size ranging from 1.0 to 2.5mm diameter may be used.
Local anesthesia with sedation can be utilized for the ORIF of the finger. General or regional anesthesia may be needed if patient factors dictate.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree