31 Lower Extremity
Summary
Common indications for lower extremity reconstruction in children include the following: constriction ring, lymphedema, syndactyly, defects following skin lesion removal, and trauma. Principles of reconstruction are similar to adults. Management is based on the type of deformity.
31.1 Introduction
In the pediatric population, plastic surgical problems can be congenital or acquired. The most common idiopathic disorders managed by plastic surgeons are syndactyly, macrodactyly, constriction rings, and lymphedema. Acquired disorders of the leg frequently arise from trauma or following extirpation of a lesion. Traumatic injuries are managed similarly to adults. However, because of the young age of the patients and long projected lifespan, aesthetic concerns and function are particularly emphasized by patients/families. We favor managing patients as low on the reconstructive ladder as possible.
31.2 Diagnosis
Diagnosis of lower extremity disorders primarily is made by history and physical examination. Traumatic wounds are evaluated for tissue loss, nerve injury, fractures, and foreign bodies. Usually adequate local tissue is available to cover bone or hardware proximal to the knee. Large areas of exposed bone or hardware involving the knee and midtibia area may be covered using regional gastrocnemius or soleus flaps. However, the threshold to use the flaps is higher in children compared to adults because of the long-term potential of reduced function. Significant tissue loss involving the lower one-third of the leg may require free-tissue transfer. Plain radiography is used to rule out fractures and foreign bodies following major traumatic injuries. X-ray also is used to assess syndactyly and macrodactyly to determine an underlying osseous abnormality.
The diagnosis of lymphedema can be difficult. The term “lymphedema” often is used generically to describe any condition that causes overgrowth of an extremity; one-fourth of patients referred to our lymphedema center do not have the disease. Lymphedema is the chronic, progressive swelling of tissue due to inadequate lymphatic function. In the pediatric population, 97% of cases are due to maldevelopment of the lymphatic system (primary) and 3% are due to inguinal lymphadenectomy/radiation (secondary). Primary lymphedema affects 1/100,000 persons and almost always affects the lower extremity; the genitalia is the second most common site. Males typically exhibit bilateral swelling during infancy, while girls usually present with unilateral edema in puberty.
Lymphedema almost always affects the distal extremity and then progresses proximally. If the hand or foot is not involved, the patient is unlikely to have lymphedema. Over time, subcutaneous lymph stimulates adipose deposition and fibrosis, which causes nonpitting edema and a positive Stemmer sign (the inability to grasp the base of the second toe or finger). Lymphedema is usually painless and does not cause ulceration. Definitive diagnosis of lymphedema requires lymphoscintigraphy; almost all patients referred to our center undergo this imaging study.
31.3 Nonoperative Treatment
Congenital anomalies do not require operative intervention unless they are causing a functional or “cosmetic” problem. Because long-term memory and self-esteem begin to form at approximately 4 years of age, elective correction of deformities not causing a functional problem can be performed at 3 years of age. Alternatively, patients can be observed until they are old enough to request improvement of a deformity (e.g., syndactyly, macrodactyly, benign skin lesion).
Most patients with lymphedema do not require operative intervention. Lymphedema is associated with a high risk for infection; therefore, patients are counseled about washing and moisturizing the affected area regularly to prevent desiccation, skin opening, and cellulitis. Patients are encouraged to participate in all physical activities, including exercise. The first-line therapy for lymphedema is compression garments, which reduce extremity volume and minimizes progression. Pneumatic compression devices provide intermittent pressure via an inflatable sleeve. Pneumatic compression therapy is efficacious, simple, and convenient because it is performed at home and is not dependent on a therapist. Complex decongestive therapy employs skin care, manual lymphatic drainage, compression bandaging, and exercise. We generally do not recommend this intervention because it is particularly difficult in the pediatric population and requires a substantial time commitment for the patient/family and the reliance on a provider.
31.4 Operative Treatment
31.4.1 Constriction Ring
Constriction ring syndrome (CRS) can affect any portion of the lower extremity, though it presents more commonly in the toes. There is a spectrum of involvement, from superficial scarring to deep bands down to bone resulting in functional detriment, growth disturbance, joint deformity (e.g., club foot), and/or distal lymphedema. The most severe manifestation can be congenital amputation at any level.
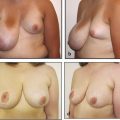
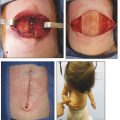
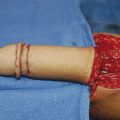
Operative treatment of CRS should address the functional and aesthetic issues of the affected limb. Collaboration with an orthopaedic colleague is vital in cases of joint deformity (e.g., club foot) or where there is significant restriction of joint motion. For bands affecting the legs or thighs, excision and flap advancement are the ideal treatment. Most advocate treatment prior to ambulation to take advantage of the extra soft tissue of an infant and easier immobilization. The authors employ the technique advocated by Upton. An assessment of tissue laxity and movement is performed. Bands that are deep and narrow are ideal as they provide plenty of soft tissue to restore contour. The ring is then marked and the skin is excised. Separate adipofascial and skin flaps are raised. The adipofascial flaps are mobilized and closed and then the skin flaps are approximated ideally away from the line of closure of the adipofascial flaps. This technique provides the best contour. Z-plasties are advocated extensively in the literature but are rarely needed. If the ring is deep or if there are multiple closely spaced rings, then a staged approach may be prudent (Fig. 31‑1).

31.4.2 Lymphedema
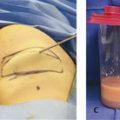
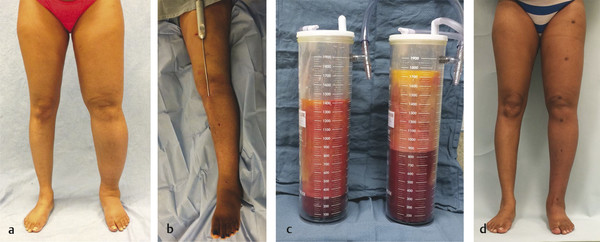
A patient must fail conservative therapy and have significant morbidity before a surgical procedure is considered (e.g., psychosocial distress, recurrent infections, decreased function). Suction-assisted lipectomy is our preferred operative technique for extremity lymphedema because it gives consistently favorable results with minimal morbidity. The technique removes the abnormally hypertrophied subcutaneous adipose tissue and reduces excess extremity volume by approximately 75% (Fig. 31‑2). Liposuction does not cure lymphedema, and patients must continue their compression regimen. Recurrence has not been noted with 15 years of follow-up. Microsurgical procedures have been performed using lymphatic-venous anastomosis (LVA) and vascularized lymph node transfer. These procedures theoretically might have efficacy in mild lymphedema, before fibroadipose deposition has occurred. However, patients with mild lymphedema rarely have significant morbidity and can be managed well with compression. Because patients with primary lymphedema have hypoplastic or absent lymphatics, they are poor candidates for microsurgical procedures. LVA and lymph node transfer have not shown consistent improvement in lymph flow and reduction in extremity volume. Lymph node transfer has been associated with donor site lymphedema following node harvest. Because patients with primary lymphedema are at risk of developing lymphedema in their other limbs, they are at highest risk for developing donor site lymphedema following removal of lymph nodes.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree