26 Gynecomastia
Summary
Gynecomastia is a common finding among healthy adolescent boys. Benign excess glandular breast tissue is the hallmark of gynecomastia. Severity ranges from a puffy appearing nipple areolar complex (NAC) to marked enlargement and ptosis. Gynecomastia may result in significant distress, and diminished self-esteem and mental health.
A comprehensive history and physical examination underpin the assessment of gynecomastia; these may be supplemented by laboratory studies and imaging. A thorough history must include a medications history, an inquiry into recreational and performance enhancing drugs, an exploration of symptoms of endocrine disease, and a systems review. Breast palpation is crucial and should aim to determine the degree of glandular and adipose involvement, and the presence of pain, tenderness and breast masses.
The majority of cases are idiopathic and self-resolving; these patients are managed with reassurance and follow-up until resolution. Other patients experience gynecomastia secondary to pathological processes or pharmacological side effects, which may be amenable to medical intervention. Non-operative interventions include the use of compression shirts, nutritional management, medication review, and referral to endocrine services for specialized treatment. Surgical intervention may be necessary in response to gynecomastia that is severe, distressing, or persistent. Operative treatment may be a combination of mastectomy, mastopexy, liposuction, and lipectomy. Satisfaction with surgery remains high among patients despite relatively frequent minor post operative complications.
26.1 Introduction
Pubertal gynecomastia is a common finding among otherwise healthy adolescent boys. The condition is marked by benign excess glandular breast tissue, although all breast mounds contain gland, fat, and skin to a variable degree. Severity encompasses a broad spectrum of presentations ranging from a puffy appearing nipple areolar complex (NAC) to marked breast enlargement and ptosis. Adolescents with gynecomastia of any severity may suffer from poor mental health and low self-esteem. It should be noted that most boys will exhibit some degree of gynecomastia during adolescence, with the majority of cases self-resolving 2 to 3 years after onset. Although pubertal gynecomastia is largely idiopathic, proper physical examination and workup is essential to rule out potential underlying pathological causes.
Most idiopathic cases of mild gynecomastia can be managed with sympathetic reassurance and yearly follow-up until resolution. The efficacy of medical intervention is variable and dependent on etiology. Persistent or distressing gynecomastia may warrant surgical intervention, with technique determined by the extent of hypertrophy and skin excess. The goal of treatment is to reduce the projection of the breast mound and NAC. Excision of redundant skin and reduction of NAC size may also be performed in cases of moderate to severe gynecomastia. Surgical complications are more common, but typically minor in patients with severe gynecomastia who undergo larger tissue resections.
26.2 Diagnosis
26.2.1 Presentation
Gynecomastia is a common finding among adolescent boys, particularly during Tanner stages 2 and 3. It is estimated that by the age of 14 years, 70% of all adolescent boys will exhibit some degree of gynecomastia. The majority of cases are idiopathic and self-resolving, with over 90% of affected boys showing complete resolution of symptoms within 3 years of onset. As a result, gynecomastia is often managed in the pediatric primary care setting. Referral to the plastic surgeon, however, may be necessary in cases of distressing, persistent, or considerable gynecomastia.
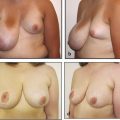
Male breast hypertrophy can be familial and may present unilaterally or with some degree of asymmetry in up to one-third of patients. Unlike macromastia, formal “diagnosis” of gynecomastia does not require meeting a threshold mass of tissue resected. The degree of breast hypertrophy in gynecomastia may instead span a range of mild to severe. As such, gynecomastia is described using a graded scale often used by third-party payors to determine insurance coverage eligibility (Box 26.1; Fig. 26‑1). Grade I gynecomastia is the mildest form, with minimal hypertrophy (<250 g) without ptosis. Grade II gynecomastia is defined by moderate hypertrophy (250–500 g) without ptosis. Grade III gynecomastia (>500 g) describes severe hypertrophy with skin excess, and is marked by mild ptosis. Grade IV gynecomastia (>500 g) is the most severe with considerable hypertrophy, skin excess, and moderate to severe ptosis. It should be noted that gynecomastia of any grade may result in significant distress and diminished self-esteem and mental health.
Box 26.1 Graded Severity of Gynecomastia
Grade I
<250 g hypertrophy excess per side
Minimal glandular, adipose involvement
No skin involvement or ptosis
Grade Ia: breast mound composition primarily adipose tissue
Grade Ib: breast mound composition primarily glandular tissue
Grade II
250–500 g hypertrophy excess per side
Moderate glandular, adipose involvement
No skin involvement
No ptosis
Grade IIa: breast mound composition primarily adipose tissue
Grade IIb: breast mound composition primarily glandular tissue
Grade III
>500 g hypertrophy excess per side
Moderate to severe glandular, adipose involvement
Mild to moderate skin involvement
Mild ptosis (grade 1)
Grade IV
>500 g hypertrophy excess per side
Severe glandular, adipose involvement
Moderate to severe skin involvement
Moderate to severe ptosis (grade II or III)
Source: Adapted from Rohrich RJ, Ha RY, Kenkel JM, Adams WP Jr. Classification and management of gynecomastia: defining the role of ultrasound-assisted liposuction. Plast Reconstr Surg 2003;111:909–923.
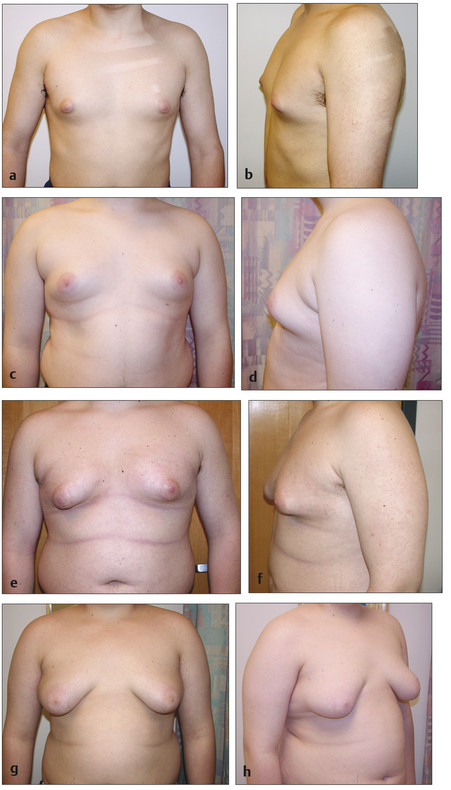
True gynecomastia is a proliferation of male glandular breast tissue, and should be distinguished from pseudogynecomastia in which the majority of the breast mound is secondary to excess adipose tissue. Both tissue types, however, are present to varying degrees in patients with true pubertal gynecomastia. Adolescent gynecomastia is highly associated with obesity. Excess peripheral adipose tissue can contribute directly to the size of the breast mound. Additionally, the presence of elevated aromatase in adipose tissue can result in glandular overgrowth by stimulating the conversion of androgens to estrogen. Regardless, it should be emphasized that it is usually the size and contour of the breast mound rather than its relative composition that is concerning to patients.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree