25 Macromastia
Summary
Macromastia is a common adolescent breast disorder characterized by unilateral or bilateral breast hypertrophy, often resulting in significant functional impairment and negative quality of life. Onset of adolescent macromastia typically occurs shortly after menarche, usually between the ages of 9 and 15, and is distinguished by considerable breast growth out of proportion to the adolescent’s frame. The vast majority of patients with macromastia report musculoskeletal pain, painful bra strap grooving, as well as difficulty exercising and participating in sports. Apart from physical symptoms, many patients experience psychosocial distress manifesting in poor mental health, low self-esteem, and increased disordered eating thoughts and behaviors relative to their peers.
Currently, there are no standardized treatment guidelines for adolescents with macromastia. Available non-operative treatments include physical therapy, weight loss and nutrition counsel, hormonal treatments, and ongoing psychological management. However, the efficacy of these treatments is variable, and they often do not completely alleviate symptoms. Macromastia can be successfully treated with early surgical intervention in the form of reduction mammaplasty, though this option is often hindered by various barriers to treatment specific to the adolescent patient. The most widely employed surgical technique in the United States is the Wise pattern resection around an inferiorly based pedicle. Associated musculoskeletal symptoms improve almost immediately following reduction mammaplasty, with breast appearance continuing to improve for several months. Although a relatively safe operation, minor complications related to wound healing in the early postoperative period are common. Conversely, major complications such as tissue loss, loss of sensation, and hemorrhage are very rare.
25.1 Introduction
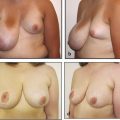
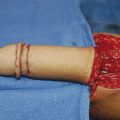
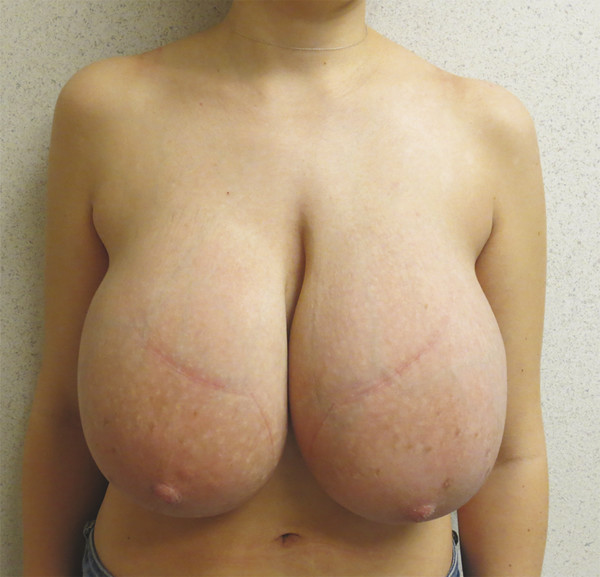
Macromastia is a common adolescent breast disorder in which the glandular tissue of one or both breasts exhibits hypertrophy (Fig. 25‑1). Onset frequently begins shortly after menarche and is marked by considerable breast growth out of proportion to the adolescent’s frame. Aesthetic concerns aside, benign breast overgrowth can result in significant functional impairment and is associated with negative quality of life. The majority of patients present with moderate to severe musculoskeletal pain, bra strap shoulder grooving and bruising, and difficulty when exercising and participating in sports. Adolescents with macromastia are often targets of teasing and harassment and unwanted sexual attention, and as such, many patients suffer from poor mental health and low self-esteem.
Although macromastia can be successfully treated with early surgical intervention, there are several barriers to treatment unique to the adolescent patient. For example, parents, physicians, and surgeons may be reluctant to offer surgery despite debilitating symptoms, and in some cases insurers set age and weight restrictions for the procedure. Reduction mammaplasty is a well-tolerated procedure with a high satisfaction rate in appropriate patients. In general, patients should be nonsmokers with supportive families and also emotionally and intellectually mature enough to understand the risks and benefits of surgery. Although minor complications related to wound healing are common, major complications such as tissue loss, loss of sensation, and hemorrhage are very rare.
25.2 Diagnosis
Onset of adolescent macromastia occurs shortly after menarche, most commonly between the ages of 9 and 15 years. During this time, the breasts may quickly grow disproportionate to the adolescent’s frame and may appear ptotic with striae. In rare cases of virginal breast hypertrophy, rapid and progressive breast development may begin with onset of thelarche and necessitate early surgical intervention. Although breast overgrowth may be noted early by the pediatrician, parent, and patient, the stigmatization of adolescent breast surgery may delay referral of patients with suspected macromastia to the plastic surgeon. By the time the adolescent presents to the plastic surgeon, she may be considerably symptomatic for several years.
Patients with symptoms referable to heavy, ptotic breasts should undergo a complete history, physical examination, and assessment of symptomatology (Box 25.1). A formal “diagnosis” of macromastia can be made using the Schnur Sliding Scale, which examines the relationship between estimated breast resection mass and the patient’s calculated body surface area (BSA), in order to determine whether the indications for reduction mammaplasty are primarily medical or cosmetic. A common threshold for insurance coverage is a minimum 500 g of resected tissue per breast, although this may be less in petite or short-statured women.
Box 25.1 Indications for reduction mammaplasty in adolescents
Breast symptomatology
Shoulder grooving and bruising
Inframammary intertrigo
Breast ptosis
Breast striae
Associated musculoskeletal pain
Lower and upper back
Shoulder
Neck
Arm
Breast
Physical impairment
Daily work, school, life activities
Exercise and sporting activities
Secondary scoliosis or postural defects
Psychosocial impairment
Mental health
Self-esteem
Disordered eating thoughts and behaviors
Difficulty finding appropriately fitting clothes and bras
Anthropometric characteristics
Schnur Sliding Scale threshold for BSA
Abbreviation: BSA, body surface area (m2).
Associated musculoskeletal pain—including, but not limited to, the upper and lower back, shoulders, neck, arms, and breasts—should be documented for insurance purposes. Inframammary fold intertrigo, shoulder grooving and bruising from bra straps, and discomfort when exercising should be assessed and noted. During the physical examination, presence of multiple or giant fibroadenoma should be ruled out, particularly in patients presenting with unilateral macromastia or painful, tender breasts.
Adolescents with macromastia may exhibit poorer mental health, lowered self-esteem, and increased disordered eating thoughts and behaviors relative to their peers. Positive exam findings for diminished mental health status, self-esteem, and disordered eating behaviors and obesity should be addressed. The surgeon should also evaluate the patient’s skeletal and psychological maturity when considering surgical intervention. The potential for additional breast growth in pubertal patients must be considered and discussed with the patient and parent, but should not absolutely preclude surgery.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree