3 Oncological Aspects of Nipple-Sparing Mastectomy
Summary
Nipple-sparing mastectomy (NSM) is the result of patient- and surgeon-driven progression in breast conservation to improve reconstructive cosmesis. Patient selection criteria include small, early-stage cancer with tumor location more than 2 cm from the nipple. With this criterion, the incidence of occult nipple–areolar complex (NAC) involvement is very low (3–8%).
The surgical treatment of nipple involvement is dependent on the careful pathologic sampling. Unless there is involvement of the retroareolar tissue, re-excision of the nipple margin or nipple papilla excision can be performed. The incidence of NAC recurrence after therapeutic NSM is low. Studies of oncological safety are hindered by short follow-up and variations in indications and surgical technique. A recent Cochrane analysis could not conclude whether local recurrence or survival was similar to traditional and skin-sparing mastectomy.
Key Teaching Points
The incidence of occult nipple–areolar complex (NAC) involvement after therapeutic nipple-sparing mastectomy (NSM) is very low (3–8%). Tumor size and distance from the NAC are predictors of occult involvement. Many centers now consider NSM in all patients without clinical or imaging of direct nipple involvement.
The use of frozen-section analysis of nipple margins is hindered by modest sensitivity, sampling errors, processing artifact, and interpretation difficulties. Careful sampling of the retroareolar tissue and excision of the nipple ducts within the papilla submitted for permanent histology allows more accurate pathologic assessment.
The surgical treatment of nipple involvement is dependent on the careful pathologic sampling. Unless there is involvement of the retroareolar tissue, re-excision of the nipple margin or nipple papilla excision can be performed. The majority of positive re-excisions are ductal carcinoma in situ. Radiation therapy is an option for occult nipple involvement if other tumor characteristics warrant its use.
The incidence of NAC recurrence after therapeutic NSM is low. Studies of oncological safety are hindered by short follow-up and variations in indications and surgical technique. A recent Cochrane analysis could not conclude whether local recurrence or survival was similar to traditional and skin-sparing mastectomy.
3.1 Introduction
Nipple-sparing or total skin-sparing mastectomy (NSM or SSM) evolved through two different pathways. The subcutaneous mastectomy was first described by Freeman in 1962 for treating benign breast lesions with immediate or delayed prosthetic replacement. It utilized an inframammary fold incision that differed from the NSM performed today by the thickness of the skin flaps and the presence of retroareolar tissue. Subcutaneous mastectomy was popularized by Woods at the Mayo Clinic for the treatment of women at high risk of developing breast cancer. Hartmann et al first demonstrated the safety of prophylactic subcutaneous mastectomy in a cohort of 575 women at moderate-to-high risk of developing breast cancer. Seven patients (1.2%) developed breast cancer and only one case occurred in the NAC (0.2%) after a median follow-up of 14 years. A subgroup of 23 of these patients carried the BRCA gene mutation with none of these developing cancers in the retained nipple.
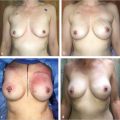
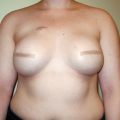
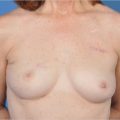
In the 1990s, the emergence of SSM facilitated immediate breast reconstruction technique and outcomes by allowing for retention of the native skin envelope and the inframammary fold. The oncological safety of SSM was confirmed after large clinical experience and became the standard of care in early-stage breast cancer when immediate reconstruction was performed. Going one step further, nipple preservation during mastectomy represents the latest development in the ongoing patient- and surgeon-driven progression in breast conservation to improve reconstructive cosmesis (▶Fig. 3.1). In 1999, Laronga et al published a feasibility study of NAC preservation in breast cancer patients treated by SSM. At the start of the new millennium, clinical reports of NSM for cancer appeared. Gerber et al reported 61 patients treated by NSM for cancer. The authors compared them to women having SSM. At a mean follow-up of 59 months, the local recurrence rate was the same (5%). The following year, Crowe et al reported 44 patients having NSM for cancer or prophylaxis.
Studies have shown that NSM reduces the feeling of mutilation, improves cosmesis, and has higher psychosocial and sexual well-being compared to SSM and nipple reconstruction. Dissatisfaction with conventional methods of nipple reconstruction after mastectomy and increase in incidence of prophylactic mastectomy in high-risk patients of younger age also contribute to growing interest in NSM. Other touted advantages include superior symmetry, potential maintained sensation, and possible single-step immediate reconstruction. Nevertheless, restricted indication, difficult exposure, nipple ischemia risk, and unproven oncological safety represent current limitations.
3.2 Occult Nipple—Areolar Complex Involvement
While gross NAC involvement is an obvious contraindication to NSM, occult disease has been observed in 10 to 24% of mastectomy specimens. Predictors of occult NAC invasion include tumor proximity, tumor size, axillary lymph node involvement and HER2 amplification (▶Table 3.1). The wide range of percentages illustrates the heterogeneity of patient selection and histological analysis in existing literature. Nonetheless, out of the collective experience emerge guidelines generally used in selection of patients for NSM: small, early cancers (stage 0 or 1) with tumor location more than 2 cm from the nipple. With these more stringent criteria, the reported incidence of NAC involvement after NSM is 3 to 8%.
With the increasing popularity of breast magnetic resonance imaging (MRI), its potential to precisely depict tumor size and relative location has led to its use in the preoperative workup for NSM candidates. However, the superiority of MRI to clinical evaluation in this setting is not clear. Steen et al evaluated 77 breasts, of which 23% had tumor involving or within 1 cm of the NAC. The sensitivity of detecting histopathologically confirmed NAC disease was not higher with MRI (56%) as compared with that attained with clinical assessment alone (61%). However, MRI-measured tumor size (> 2 cm) and distance from tumor edge to NAC (< 2 cm) correlated with risk of NAC involvement. Although tumor-to-NAC distances as short as 1 cm on MRI has been proposed an adequate threshold for NSM, many centers now consider NSM in all patients without clinical or imaging evidence of direct nipple involvement.
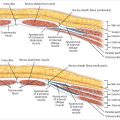
The retroareolar tissue just deep to the NAC skin is thought to be an indicator of NAC carcinoma involvement, as contiguous tumor spread occurs with direct extension from the retroareolar tissue into the terminal ducts and papillae. In Brachtel et al’s analysis of 45 cases of carcinoma involving nipples, the retroareolar tissue likewise contained disease in 36 cases. Nine cases with negative retroareolar tissue had nipple involvement, while eight cases with positive retroareolar tissue had no nipple involvement. Use of the retroareolar margin to reflect nipple disease yielded a sensitivity of 0.8 and negative predictive value of 0.96. Simmons et al analyzed nipple and areolar involvement with cancer after SSM. The authors found that 10.6% of patients were found to have malignant nipple involvement but only 0.9% was found to have involvement of the areola. These findings predated the work of Brachtel et al but supports areolar preservation in cases of nipple involvement.
Many institutions routinely perform frozen-section analysis of the nipple margin at the time of NSM. This potentially could reduce the number of surgeries required. Intraoperative frozen section has high specificity but only modest sensitivity. Sampling errors, processing artifact, and interpretation difficulties are limiting factors. Distinguishing atypical hyperplasia from ductal carcinoma in situ (DCIS) can be very difficult even on permanent section analysis. In cases of positive nipple involvement, it has the potential to reduce the number of operations. That being said, it can be very anxiety provoking for a woman to undergo general anesthesia not knowing whether she is going to have her nipple removed or not.
Accordingly, intraoperative determination of NAC salvageability via frozen-section analysis of the retroareolar tissue is often performed. Kneubil et al reported the outcomes of 88 patients (of 948 total NSMs) who had false-negative frozen-section analysis of the nipple base and 10 patients who had close surgical nipple margins. The overall false-negative rate of frozen-section analysis of nipple margin was 9.2%. Ninety-three patients (94.9%) received intraoperative radiotherapy. The 5-year cumulative incidence of NAC recurrence was 2.4% (2/98). Both cases were noninvasive recurrences. In their analysis of 52 NSM cases, Luo et al found that frozen section yielded 10% positive results (13 or 25% positive on permanent sections). The overall false-negative rate of frozen section was 15%. The sensitivity and specificity of intraoperative frozen section were 38 and 100%, respectively.
Alperovich et al described the use of intraoperative frozen section in 307NSMs. Twelve cases (3.9%) were found to be positive on permanent section analysis, five had a false-negative frozen section. The sensitivity and specificity were 0.58 and 1, respectively.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree