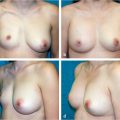
10 Fat Grafting to the Breast in Prepectoral Breast Reconstruction—A Current Overview
Summary
Autologous fat grafting has become the preferred technique for volume/soft tissue restoration and aesthetic enhancement in breast reconstruction. Fat offers numerous clinical benefits when injected as a graft, including thicker and enhanced mastectomy skin flaps, improvement of soft tissue quality through high stem cell concentrations, and reversal of some sequelae associated with radiation fibrosis. Successful outcomes in fat grafting are heavily dependent on proper technique being used for donor site planning and preparation, fat harvest and processing, and reinjection methods and strategy. When this is done, there will be maximal survival of injected fat, with minimal complications. Using such techniques, a variety of breasts can be treated with autologous fat grafting, including those that have undergone breast conservation, and those patients with postmastectomy reconstruction utilizing either prepectoral, subpectoral, or autologous reconstruction methods. In cases of delayed reconstruction, fat grafting can be used as a “preconditioning” procedure, to improve the quality of the chest wall soft tissue envelope, allowing it to better tolerate eventual tissue expansion and placement of a permanent prosthesis. In this way, fat grafting carries benefits in many clinical scenarios, and is now a critical and mandatory component of most breast reconstruction procedures.
Key Teaching Points
Fat grafting is a critical component of all types of breast reconstruction, as it allows for volume restoration and aesthetic improvement, using fully autologous tissue that integrates permanently.
Fat contains large concentrations of mesenchymal stem cells, and thus fat grafting also can function to improve the quality and condition of devascularized breast skin, particularly following postmastectomy radiation.
Technique is the critical component determining fat graft take rates, and the optimal fat harvest sites are the infraumbilical abdomen, and the medial thighs.
Following harvest, minimal processing techniques employing light rinsing and filtration result in highest densities of viable fat cells, as they remove blood and oil, without lysing fat cells.
Injection of fat must always be performed into well-vascularized host tissue beds or skin, in long thin strands, ensuring that all injected fat is directly contacting a surrounding blood supply, and can revascularize and survive.
When performed using proper technique, fat grafting will result in minimal risk of complications such as fat necrosis and oil cysts and has been shown to still safely allow for future breast screening surveillance.
10.1 Fat, the Ideal Filler
Volume restoration is a critical component of reconstructive breast surgery. Both implants and autologous flaps function well to restore the majority of volume to breasts, following oncologic treatment with either complete or partial mastectomy. This restores the aesthetic breast mound and helps to maintain the female chest wall and breast appearance. However, the success of these techniques lies heavily in the viability and quality of the overlying skin and soft tissue envelope. Without adequate and viable soft tissue coverage, most forms of breast reconstruction cannot be performed with predictable success, heal successfully, or withstand long-term complications.
Autologous fat grafting has emerged as a critical component of breast reconstruction, due to its powerful ability to restore volume to the soft tissue envelope of the breast and improve its quality. Unlike other fillers, fat has the ability to revascularize from surrounding tissue, and live permanently in the injected region, surviving on its new blood supply. In addition to adding thickness and volume to the soft tissue envelope, fat also improves the quality of this tissue, through rejuvenation and softening. This is due to the high concentration of stem cells in human adipocytes. Multiple studies have confirmed the regenerative properties of grafted fat, attributing this to the regenerative potential of the adipose-derived mesenchymal stem cells (ASCs) found in the stromal vascular fraction of lipoaspirate. These cells allow the grafted fat to improve tissue quality at the recipient site, and even reverse some of the damaging characteristics of radiation fibrosis, such as vascular depletion and abnormal collagen arrangement.
10.1.1 Clinical Applications and Safety
Over the past 10 years, autologous fat grafting has become a routine part of breast surgery in the majority of patients, both as a primary procedure, and as an adjunct procedure for rejuvenation and repair of contour deformities. This technique can be utilized in implant-based, autologous, and postlumpectomy reconstruction, has been incorporated into aesthetic breast procedures such as augmentation mammoplasty, and has been used for correction of developmental breast asymmetries, such as Poland’s syndrome and tuberous breast deformity.
The benefits of fat grafting are numerous, attributed to its biocompatibility, availability, versatility, and ability to integrate into host tissues and survive. It has become essential in correcting intractable aesthetic deformities and minor asymmetries that were previously difficult to address. Furthermore, fat grafting has demonstrated low infection rates and has been shown to be oncologically safe in breast cancer patients. Because ASCs are not specifically isolated and purified prior to injection, there is no increased risk of breast cancer recurrence. Fat grafting carries the added benefit of being a minimally invasive technique, with minimal risk of donor site or recipient site morbidity. Furthermore, because fat harvest is performed with standard liposuction techniques, it carries the added aesthetic benefit of donor site contouring.
For grafted fat to survive and revascularize at high rates, and result in volume restoration, it must be harvested, processed, and reinjected with very precise surgical technique. These specific techniques allow for maintenance of living fat cells, with intact molecular structure, that can then reestablish blood flow as a graft when injected into a new environment. When fat is incorrectly injected, or damaged/lysed fat cells are injected, this leads to higher rates of fat necrosis, oil cysts, and calcification. The ability to avoid this is critical to successful breast rejuvenation. Recommended surgical techniques for all these steps are presented in the following sections.
10.2 Fat Grafting Technique
Surgical technique is the key element determining successful outcomes in autologous fat grafting. It ensures that viable cells are being injected, and that all cells are given a vascularized environment in which they can survive at the highest rates.
10.2.1 Preoperative Planning
In assessing a patient for autologous fat grafting, the surgeon must first select the correct donor sites for fat harvest. The infraumbilical abdomen and thighs are the most commonly chosen donor sites, due to their accessibility with a patient in the supine position, as well as the high concentration of viable adipocytes in these areas. Thus, it is advisable that these areas be used as the primary option for fat harvest when available.
Preoperatively, the surgeon must carefully mark the zones of planned liposuction, with the patient standing, such that all donor site areas are used equally and symmetrically, to avoid a donor site defect (▶Fig. 10.1). Fat harvest should be thought of not only to obtain fat, but to improve the aesthetic appearance of all donor sites utilized. The most frequent cause of patient dissatisfaction with autologous fat grafting comes from donor site contour deformities, such as hollowing or deflation, from excessive liposuction. This can be avoided by symmetric harvest from all sites, and avoidance of the traditional liposuction danger zones when harvesting.
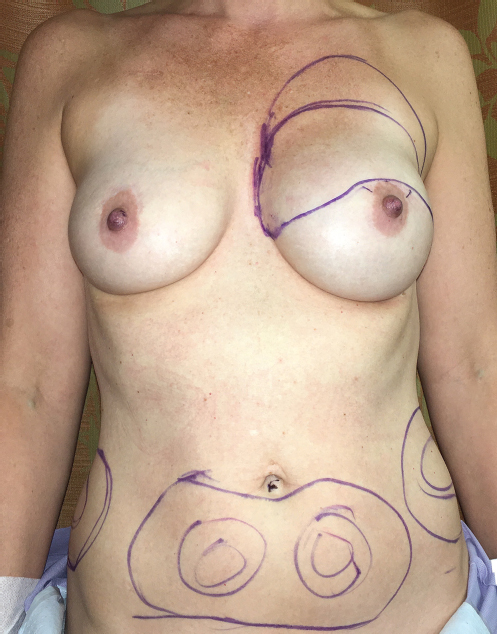
Additionally, the surgeon must precisely identify the areas of planned fat injection preoperatively, again with the patient standing. They also must plan the proper cannula entry points and direction of fat injection. The planned skin injection sites must allow access to the entire breast mound, and also allow for concealed scars. For most cases of breast injection, it is helpful to have a minimum of two sites for injection on each breast, one medial and one lateral. This gives complete access to the entire breast in opposing directions, allowing for thorough injection. This is imperative for ensuring uniform fat distribution. Some surgeons prefer to use computer-assisted planning based on two-dimensional photographs and/or three-dimensional surface and volumetric models, but this is not necessary to ensure a uniform and symmetric result.
Clinical Pearl
When planning locations for fat harvest, it is advisable to choose a combination of donor sites that will not require a position change in the operating room. Those donor sites accessible with the patient in the supine position are easiest and allow for the most efficient and effective surgical procedures.
10.2.2 Donor Site Preparation
Intraoperatively, the donor sites must first be prepared for fat harvest. The targeted areas should be infused with standard tumescent solution, consisting of an isotonic fluid mixed with epinephrine and lidocaine at safe concentrations. This allows for harvest of lipoaspirate with minimal blood content, and with minimal discomfort. The components of the tumescent solution have been shown to have no alteration on fat graft take rates or adipocyte viability in subsequent fat grafting.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree