27 Hair Transplantation in East Asians
Pearls
The East Asian skull tends to be rounder in circumference and to have a larger and wider forehead compared with its Caucasian counterpart, which results in rounded frontotemporal angles and a flatter hairline.
Asians have fewer hairs and a lower multi-hair follicular unit (FU) count than Caucasians. The follicle length from epidermis to dermal papilla is longer and the average hair shaft diameter is thicker.
Asians are prone to keloid and hypertrophic scarring, which is more common in younger patients due to their higher rate of collagen synthesis.
Even after patients receive hair transplantation, the loss of existing hair continues as time goes on. Therefore, additional medical treatment is necessary to prevent or limit further hair loss.
“Depth-controlled transplantation” according to graft length can help to yield a superior result and help to minimize complications such as folliculitis, pitting, and poor survival.
Applying the vibrator and ice pack during local anesthesia can be very helpful in reducing pain. Allowing the patient to grasp the assistant’s hand or arm can also help to minimize the reaction to pain.
Vitamin E, omega-3, and herbal medications should be avoided for at least two weeks prior to surgery to reduce bleeding during hair transplantation.
Preoperative oral diazepam may limit the incidence of syncope and fainting. Taking a break and consuming cookies and juice would be helpful to the patient in reducing discomfort during the hourslong operation.
Follicular unit extraction (FUE) should be performed with care in Asians because of their idiopathic tissue fibrosis, lower FU density and hair-graft ratio, high hair-skin color contrast, and a higher risk of transection due to their longer hair follicle.
Several factors should be evaluated during consultation. These include the age of the patient, donor density, donor hair thickness, extent of hair loss, and the patient’s expectations.
Introduction
In hair transplantation, the term Asian encompasses individuals from a wide area located geographically from what Europeans call the Middle East to the Far East. Ethnic groups have different hair and facial characteristics depending on their country of origin. In this chapter, the word Asian will mainly be used in reference to the peoples of East Asia, such as the Koreans, Japanese, and Han Chinese.
Historically, Asians have been concerned less about male pattern hair loss (MPHL) than Caucasians. This is mainly because MPHL was associated with wealth, the wisdom due to age, and the upper classes.1,2 In today’s society, Asians are becoming more concerned about their external features and appearance than they have been in the past. For example, it is becoming more difficult for Korean males with a Norwood type IV or greater level of baldness to get married or obtain employment because these individuals look older than their actual age. This can lead to feelings of insecurity and shame. To overcome this, more and more Asians are becoming interested in hair transplantation surgery.
Hair transplantation among East Asians and Caucasians is similar in many aspects, but there are several differences that must be discussed.
Characteristics of the Asian Scalp and Hair
Shape and Hairline
The shape of the Asian skull appears rounder in circumference than the usually ovoid Caucasian skull. The forehead area of the Asian skull also tends to be larger and wider than its Caucasian counterpart (Fig. 27.1). These differences result in rounded fronto-temporal angles and a head that is flatter across the hairline in East Asians.3
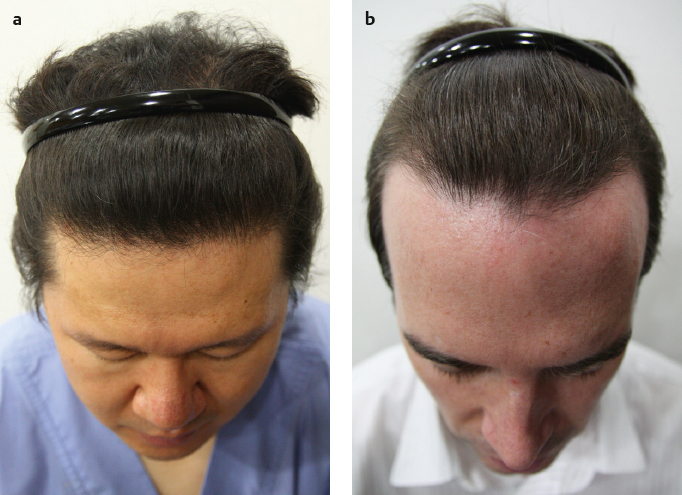
Clinical consultations with Asian males have found that most prefer a low, straight hairline with a rounded frontotemporal angle. Surgeons occasionally recommend a frontal recession to patients for a better cosmetic result, as it is sometimes necessary to modify the patient’s desired hairline to produce an aesthetically acceptable cosmetic result. For patients with Norwood class VI or VII hair loss, a frontal forelock design connecting the temple areas will produce aesthetically acceptable results for most Asian patients, although true isolated frontal forelocks are not well accepted by the majority of Asians.
Hair Characteristics
Compared with Caucasians, Asian hair is coarser, has a larger caliber, and is usually straighter. The average hair shaft diameter of an Asian is ~ 100 mm, versus a maximum of ~ 70 mm for that of Caucasians.1,2 The larger-caliber hair shaft contributes to the appearance of greater hair density. Furthermore, the color contrast between black hair and light skin is high. Skin color varies from white to dark across Asia (e.g., Koreans and Japanese tend to have white skin, whereas Malaysians and Indians tend to have darker skin). This high skin/hair color contrast also makes it very difficult to achieve the illusion of fullness, because the scalp can be clearly seen through the straight black hair. As a result, the high color contrast coupled with the larger-caliber hair makes a transplant more noticeable when mini or punch grafts are used. Therefore, follicular unit transplantation (FUT) is the method of choice for Asians for producing a more natural look.4,5
The follicle length from epidermis to dermal papilla is 5.5 mm on average in Asians compared with ~ 4.5 mm in Caucasians. This results in a higher risk of transection of grafts during donor harvesting and graft dissection.6
Hair Density
The hair density of the donor area of an Asian male is usually lower than that of Caucasian males. Caucasians have hair density of an average of 200 hairs/cm2 in the donor area,7 whereas Koreans have ~ 137 hairs/cm2 in the occipital area and 118 hairs/cm2 in the temporal area.1 Ezaki estimates that the average hair density in Japanese men is 130 hairs/cm2, while Pathomvanich reports that Thai men have 170 hairs/cm2 in the occipital and 127 hairs/cm2 in the parietal area.8,9 In general, males in the Far East of Asia have a lower hair density than those in the Middle East or Southeast Asia.
The occipital follicular units of Koreans are ~ 37% singlehaired, 38% twohaired, and 25% threehaired. According to Imagawa, the scalp hairs of Japanese men are made up of 30% singlehair, 50 to 55% twohair, and 15 to 20% threehair FUs on average.1 Pathomvanich states that the scalp hair of Thai men has 24% singlehair, 64% twohair, and 13% threehair FUs.9 In addition, Thai men have 90 FU/cm2 or 170 hairs/cm2 in the occipital area while in the parietal zone, they have 70 FU/cm2 or 127 hairs/cm2. This represents 1.8 hairs/FU. Bernstein found that Caucasian men have an average of 25% one-hair FUs, 50% twohair FUs, and 25% threehair FUs.4,5 Caucasians have a similar density of FUs, but have 2.3 hairs/FU, resulting in a greater total number of hairs.
In general, hair transplantation doctors count the number of “grafts” transplanted. However, Korean doctors count the number of “hairs” transplanted. This is because the ratio of singlehair FUs to multi-hair FUs varies greatly among patients, and the results are dependent on the number of hairs and not on the number of grafts.
Scar Formation
The Asian scalp is thicker and less elastic than the Caucasian scalp and suffers a higher incidence of keloid or hypertrophic scarring at the donor site.1,2,9 These scars occur less commonly in Asians than those from African descent, but at a higher rate than in Caucasians.1,2 These scars occur in the donor area and are very rare in the recipient area. The main cause for hypertrophic scarring in Asians is genetic, and the problem occurs more commonly in younger patients, due to their higher rates of collagen synthesis. These scars can also be aided by excessive tension during donor site closure. The risk increases if multiple hair transplantation sessions are necessary, so surgeons should avoid the use of wide strips and minimize tension during closure.
The Importance of Medications in Asians
Compared with Caucasians, usually fewer hairs on the East Asian head are available for harvesting.1 Also, a higher rate of scarring on the donor site limits the number of procedures available to East Asians.9 Even after patients receive hair transplantation, the ongoing loss of hair continues as time goes on. Therefore, it is essential to maintain existing hair in East Asian patients with medications like oral finasteride and topical minoxidil, which can slow future hair loss.10,11,12,13 In addition, by maintaining existing hair through the use of medication, a patient’s self-esteem can be greater due to the hair’s higher density.
Patient Evaluation
The following points should be discussed during consultation with patients.2
Patients need to be informed about the procedure, expected course after the procedure, and possible complications.
Realistic expectations regarding the number of hairs and areas to be transplanted need to be explained, as well as achievable longterm results.
It is helpful to draw the achievable hairline with a colored pencil to show the patient.
It is helpful to grade expected results based on the age, severity, family history, and densitometer result of the patient.
It is important to explain the necessity of medical treatment to prevent further hair loss.
Discussion about future hairstyle can aid patient satisfaction. A short hairstyle can result in lower patient satisfaction, while parting can be more satisfactory cosmetically.
Patients who have been wearing wigs should be informed that the hair transplant will not result in the same appearance as that of donning a wig.
In the event that a patient received an unsatisfactory procedure from another clinic, it is important not to criticize the previous clinic. It is more beneficial for the patient to receive a detailed explanation about the improvements achievable from an additional procedure.
Since the aim of a procedure can differ between a doctor and a patient, it is beneficial to show before and after photos of previous patients.
Though patients prefer to have the maximum number of hairs to be transplanted, transplantable hair numbers should be based on scalp elasticity, family history, and likely future progression.
Many Asians routinely consume various herbs such as ginseng, garlic, and onion, as well as other supplements. These herbs and supplements may increase bleeding during hair transplantation surgery and therefore should be avoided for at least 2 weeks prior to surgery.14
A complete blood count, a routine urinalysis, tests for hepatitis B and C antigen and human immunodeficiency virus (HIV), and tests for liver and kidney function should be performed before the surgery.
To evaluate whether a patient is a good candidate for hair transplantation, we need to take several factors into consideration.2
Age: Among all age groups, patients under the age of 25 years are the most difficult to satisfy. Experienced hair surgeons usually avoid or delay hair transplantation for young patients. Male-pattern hair loss starts after adolescence. Therefore, many patients with advanced hair loss in their 20s request hair transplantation. In severe cases, performing the transplant is inevitable. If the hair loss is not very advanced, it is advisable to delay the transplant as long as possible, and the donor site should be preserved as much as possible for further transplantation in the future, even if the transplant is performed. Donor site scarring is more common in younger patients, so it is necessary to discuss scarring. Also, special consideration needs to be given concerning closure, including smaller widths and internal sutures. Middle-aged or older patients, however, rarely develop significant scarring on donor sites, and their expectations about the transplant tend to be lower. Therefore, their satisfaction tends to be greater and they are more suitable for the transplant.
Donor density: The hair density of the patient’s donor area should be evaluated using a densitometer.15 This procedure assesses the number of single-, two-, and threehair FUs that will be obtained from the donor area. Koreans have an average of 130 hairs per square meter on the occipital scalp. Greater hair number with higher density tends to have 2- and 3- hair FU, resulting in a better outcome after the transplant. If the density is much lower than average in patients with severe hair loss, hair transplantation should be avoided because the patient will not be satisfied with the results.
Hair thickness: Thicker hairs on the donor site result in greater volume and better cosmesis after the transplant. It is helpful, therefore, to measure the thickness of the hair during the consultation. If the hair thickness is less than 60 mm, the outcome of the hair transplantation will not be as good and patients usually will not be able to achieve the expected fullness.
Patient’s expectations: Patients with early malepattern hair loss tend to have higher expectations, resulting in lower patient satisfaction. Also, the progression of alopecia and the survival of transplanted hairs can result in unusual and unacceptable hair patterns. In contrast, advanced malepattern hair loss patients tend to have lower expectations, resulting in higher satisfaction. It is very important to assess the patient’s expectations from the surgery. Unrealistic expectations will result in unhappy patients. It is important to adjust the patient’s expectations prior to the surgery, and it is wise to delay the surgery if the expectations do not change.
Scalp laxity: A thick and immobile scalp is described as “tight scalp,” and it can be difficult to close the donor site wound if the width is greater than 1 cm. It is safer to operate multiple times with small widths in cases of tight scalp since a width of 1.5 cm can result in necrosis and severe scarring. With tight scalp, the width should be small and the number of harvested hair follicles lower than usual, or else satisfaction with the outcome of transplantation also will be low. Therefore, a scalp that is too tight is a contraindication for hair transplantation.
Past history and family history regarding scarring: East Asians are genetically susceptible to abnormal donor area scarring, which affects their suitability for hair transplantation. In particular, they are prone to keloid scarring, which occurs when the fibrous tissue expands beyond the boundaries of the incisional scar, and hypertrophic scarring, which is characterized by exuberant fibrous growth that does not cross the wound margin. These problems occur more commonly in younger patients, due to their higher rates of collagen synthesis. During the consultation, East Asian patients should be carefully screened for these problems, and old wounds should be examined. Patients with a personal history of keloid scar formation are not good candidates for hair restoration surgery, while those with a family history of keloid scarring, or a personal history of hypertrophic scarring, should be cautioned on the increased risk of abnormal healing.
Surgical Techniques
Preparation on the Day of Surgery
When the patient arrives for surgery, the author begins by taking preoperative photographs. If a patient has high blood pressure, this can lead to excessive bleeding during surgery. Transient high blood pressure may be caused by emotional stress, so preoperative sedatives such as diazepam and/or sublingual nifedipine are useful in reducing or normalizing the patient’s blood pressure. Assistants should shampoo the scalp before donor harvesting to reduce the bacterial colony counts in the scalp, thus helping to prevent or reduce infections that may be associated with surgery.
Hairline Design
The shape of the scalp is generally round and wide among East Asians. The hairline design in East Asians should be a wide arc with less central convexity, and frontotemporal recession should be less prominent compared with the Caucasian’s round, convex hairline.3
The design of the frontal hairline is made using standard distances and anatomical landmarks. The principle of three equal distances is the balance between chin and nasal tip, nasal tip and glabella, and glabella and midfrontal point of the hairline. In general, the distance between the glabella and the midfrontal point of the hairline ranges from 6.5 to 8.5 cm.16 A 7.0 to 7.5 cm hairline works well in the majority of patients, and this is where the author places most hairlines. When designing the hairline it is important to remember the hairline consists of the frontal hairline and temples. The frontal hairline has to balance with the temples to achieve a balanced, natural look. If the temples are receded and hair transplantation on the temple area is not indicated because of insufficient donor hair, then a higher hairline, with an upslope, will create balance.
Generally, in patients with mild hair loss and better donor hair on average, placing the frontal hairline at 7 to 8 cm is safe. If the patient does not object, the author generally prefers to design in a small amount of upslope, thus making it easier to tie the top hairline to the temples without having it extend too far into the temple area. Younger patients will often push for a lower hairline or a downsloping (juvenile) hairline. On an adult Asian this design looks odd, is difficult to correct, and should be avoided.
Hair shafts of East Asians are coarse, dark, and straight. It is usually not easy to make a soft and naturallooking hairline in East Asian patients. Therefore, Asians require more singlehair units to create a naturallooking hairline. The author prefers to place a minimum of 400 singlehair FUs at the frontal hairline.
The routine that the author uses to create the hairline is simple and is as follows (Fig. 27.2):
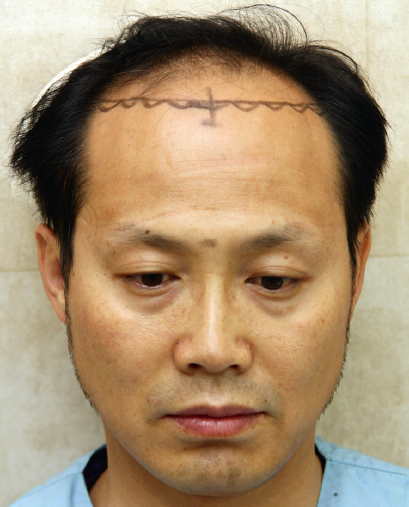
Note the distance between the chin and nasal tip, between the nasal tip and glabella, and between the right and left temples. Using the reference, mark a short horizontal line 6.5 to 8.5 cm above the midbrow level.
Mark a point on this line dividing the face into equal left and right halves. This can be done easily by holding the marking pen over the nose and bisecting the face into equal halves.
From this midpoint draw the top hairline laterally, keeping it on a horizontal plane or a slight upslope when viewed from the front.
Check from the front to make sure the two sides are even and from the side to see if the line that has been drawn balances the existing temples. If the frontal hairline looks low when viewed from the sides, you will have to move the top lines up slightly and redraw the top line with a slight upslope.
The straight line looks unnatural. Add a zigzag pattern line on the straight hairline and implant the singlehair FUs on the zigzag line to make a naturalappearing hairline.
Donor Harvesting
Strip Surgery
Strip harvesting is performed by the majority of hair restoration surgeons throughout the world. ISHRS 2013 census results showed 68% for strip harvesting compared with 32% for follicular unit extraction.17
Laxity of scalp can be assessed easily by moving the scalp vertically while holding hairs from the donor site. It can be classified into hyperelastic, normal, and tight scalp. There are other methods to measure the scalp laxity: Mayer’s scalp elasticity scale18 and Mohebi’s laxometer.19 There are different opinions about ideal widths for donor sites. The optimal width of the donor strip in Asians is 1.5 cm or less.1,2,6 It can be difficult to close using a 1-cm width in patients with a tight scalp, so it is advisable to minimize widths. It can be easy to close a hyperelastic scalp with widths of more than 2 cm; however, excess scarring can result from the stretch-back phenomenon.20 Therefore, it is advisable to incise within a 1.5-cm width in patients with hyperelastic scalp. Wide scars tend to occur more readily in younger patients since the rate of collagen synthesis is greater. In young patients, therefore, a long and narrow donor strip is safer than a short, wide strip.
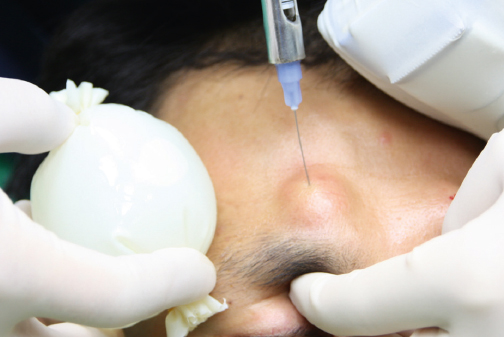
Once this is determined, the hair is trimmed in the donor area, which is located in the midocciput, extending slightly into the temporal region. The hair is trimmed to ~ 2 mm in length when employing the Western method, and 5 to 10 mm in length for the implanter technique.21 Some doctors prefer to use the tumescent technique to anesthetize the donor area, while others favor a buffered solution of 1% lidocaine with 1:100,000 epinephrine without tumescence.2 Allowing the patient to hold the assistant’s hand or arm during local anesthesia can also help to soothe the pain. Applying an ice pack and vibrator near the injection site during local anesthesia can be very helpful to reduce pain (Fig. 27.3).22 Patting the patient’s back is a useful method to make the patient feel comfortable during donor harvesting, especially in the prone position.
To minimize the number of transected follicles, the incision should be parallel to the direction of the hair follicles. This is important because the length of hair follicles is greater in Asians than in Caucasians, and thus the probability of transection is higher among Asians. For this reason, the single-blade knife technique is safer for making an incision than the multi-blade knife technique. More accurate incisional methods include the open technique suggested by Pathomvanich: Four skin hooks and two assistants are required to gain more exposure and to potentially cut faster.6 He minimized the follicular transection at 1% or less.
In addition, bleeding needs to be controlled completely before wound closure. Arterial bleeding needs to be controlled with a hemostat. Smaller vessels can be controlled with a hemostat, but a larger vessel needs ligation with 4–0 Vicryl (Ethicon). It is recommended that the surgeon avoid or reduce the degree of electro-cauterization to control bleeding in the donor area since it damages the tissue and interferes with wound healing. It is best to remove all the damaged follicles to prevent folliculitis or cysts.
The wound may be closed through a variety of methods. However, it is still controversial whether two-layer closure has more benefit than single-layer closure, undermining versus nonundermining, staple versus suture, and other options.16 The majority of surgeons use absorbable stitches (Vicryl or Monocryl, Ethicon) for deep-layer closures and close the skin with either staples or running nonabsorbable or absorbable stitches.
Damkerng reported that two-layered closure from his experience failed to minimize scarring, and instead he closes the wound with 3–0 nylon as retention stitches ~ 1.5 cm apart and a 1-cm bite away from the incision. The skin is then closed with running 4–0 Vicryl Rapide (Ethicon).16 He reported it produced good results in Asian patients. The author also had good results with the retention suture method but prefers nylon suture over Vicryl Rapide because absorbable suture material has more tissue reaction and a tendency to leave a worse scar in East Asians (Fig. 27.4). Retention stitches are usually removed at 3 to 5 days postoperative and skin stitches are removed at 10 days postop.
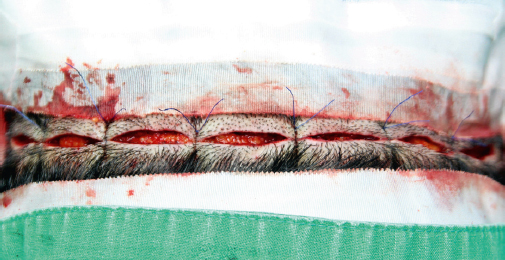
Trichophytic closure is highly recommended in East Asian patients to reduce the donor scarring, especially in younger patients or patients with hyper-elastic scalp. There might be some controversy regarding trimming of the superior or inferior edge, but there has been no visible difference in the appearance of scarring. Trichophytic closure may improve the scar’s appearance, but patients may also experience a slightly higher incidence of cyst or ingrown hair formation on the closure site.23,24,25,26
To avoid significant scarring in the donor area, risk factors such as tension and smoking must be reduced as much as possible; great care must be extended in performing meticulous surgical techniques. Despite these efforts, a small percentage of patients will develop significant scarring, usually due to genetic differences in skin type.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree