2 Basic and Advanced Skin Care
Key Concepts
Skin typing with the Baumann Skin Typing System (BSTS) allows for effective skin care by accounting for important variations in each individual patient.
Specific cosmeceutical ingredients are useful for each skin type; practitioners and patients alike should be familiar with the myriad possibilities.
Retinoids, antioxidants, and sunscreens are keystones to any good skin-care regimen.
Minimally invasive procedures, such as superficial peels, microdermabrasion, and intense pulsed light (IPL), are helpful adjuncts for improving skin appearance—particularly unwanted pigment and redness.
Introduction
The traditional skin-type designations (i.e., dry, oily, combination, and sensitive) are insufficient in terms of directing physicians and consumers to proper product selection because these labels do not address various cutaneous characteristics, including the tendency to develop wrinkling or pigmentation. In the opinion of the authors, the BSTS is a better option for identifying skin type using a wider range of cutaneous factors based on four main skin parameters: oily versus dry; sensitive versus resistant; pigmented versus nonpigmented; and wrinkled versus tight (un-wrinkled). Evaluating the skin using all four parameters results in 16 potential skin-type permutations, because these dichotomies are not mutually exclusive ( Table 2.1 ). The BSTS can guide both physicians and patients/consumers in finding the most appropriate skin products. The Baumann Skin Type (BST) acts as a standardized forum in which to informatively discuss skin care. The BST is derived from a scientifically validated questionnaire, the Baumann Skin Type Indicator (BSTI), intended to ascertain baseline skin type.1 The resulting data can be used to help identify the most suitable products and procedures for patients. This chapter briefly touches on skin-care science according to the format of the BSTS, before discussing selected minimally invasive techniques.
Background: Basic Science of Procedure
Dry skin is characterized by an impaired barrier, lack of natural moisturizing factor (NMF), or decreased sebum production; whereas oily skin is characterized by increased sebum production. A higher BSTI score indicates increased sebum production (oily skin); a lower score indicates reduced skin hydration (dry skin); and a score in the middle of this parameter indicates “normal” skin. Changes in climate, or traveling from one climate to another, can result in fluctuations between oily and dry skin.
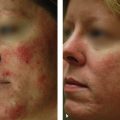
Sensitive skin is characterized by inflammation and presents as acne, rosacea, burning and stinging sensations, or skin rashes. Individuals who receive a high score in the “S” portion of the BSTI are more likely to have more than one type of sensitive skin. Resistant skin is typified by a strong stratum corneum (SC) that confers cutaneous protection from allergens, other environmental factors, and water loss. Although resistant skin—as compared with sensitive skin—is less prone to acne, it is also less amenable to topical treatments, thus requiring stronger skin-care products and in-office procedures.
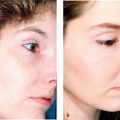
Pigmented skin within the BSTS framework refers not to skin color, but to the tendency to develop hyperpigmentation—particularly preventable or treatable with skin-care products and/or procedures (i.e., ephelides, melasma, postinflammatory hyperpigmentation, and solar lentigines). Nonpigmented skin is often seen in people with light skin who do not tan easily. Knowing a patient′s “P” score can guide practitioners in adjusting chemical-peel strengths and laser settings to prevent the development of postinflammatory hyperpigmentation.
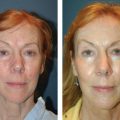
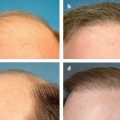
The fourth parameter (wrinkled versus unwrinkled skin) is inextricably linked to aging. Cutaneous aging results from the complex intersection of intrinsic and extrinsic factors. Intrinsic aging derives from individual heredity and the natural effects of the passage of time. Extrinsic aging results from exogenous insults and manifests in premature skin aging, especially in the face. Rhytid formation, engendered by changes in the dermal layer of skin, is the primary manifestation of skin aging. Importantly, despite myriad false claims to the contrary, few skin care products are proven to adequately penetrate the dermis to improve deep wrinkles; therefore, preventing rhytids is the goal of dermatologic antiaging skin care.2 Unwrinkled skin is skin that has been largely protected from exogenous aging factors. The remainder of this chapter focuses on specific aspects of the four BSTS parameters, as well as selected facial cosmetic procedures.
Technical Aspects of Procedure
Dry Skin
Basic Skin Care Formulations
Dry skin can be treated by augmenting SC hydration with occlusive or humectant ingredients and smoothing rough surfaces with an emollient. Occlusives coat the SC and decelerate transepidermal water loss (TEWL); humectants attract water from the atmosphere and the epidermis; emollients soften and smooth the skin. Cleansing agents are used by people of all skin types. Surfactants are the primary active ingredients in cleansers. Cleansing products include bar surfactants, superfatted soaps, transparent soaps, combination bars, synthetic detergent bars, and liquid surfactants. Patients with dry skin should be advised to select nonfoaming agents, such as a cleansing milk, oil, or cream.
Moisturizers
Moisturizers raise water content in the SC by inhibiting TEWL through occlusive ingredients or by enhancing the integrity of the skin barrier. This is achieved via delivery of fatty acids, ceramides, and cholesterol to the skin, and controlling the calcium gradient. Moisturization is also achieved by augmenting NMF levels, glycerol (glycerin), and other humectants (e.g., hyaluronic acid). In addition, skin hydration is improved by fostering epidermal capacity to absorb important circulatory components, such as glycerol and water through aquaporin channels. Most moisturizers, which are designed to improve skin hydration, are oil-in-water emulsions (e.g., creams and lotions) or water-in-oil emulsions (e.g., hand creams).
Occlusives
Widely used in skin-care cosmetics, occlusives are oily substances that can dissolve fats and coat the SC to inhibit TEWL, resulting in an emollient effect. Petrolatum and mineral oil are among the most effective occlusives. A purified mixture of hydrocarbons derived from petroleum (crude oil) and used as a skin-care product since 1872, petrolatum, the gold standard of occlusives, displays a water vapor loss resistance 170 times that of olive oil.3 The hydrocarbon molecules present in petrolatum prevent oxidation, giving it a long shelf life.4 However, petrolatum has a greasy texture that many patients find unappealing. Cosmetic-grade mineral oil, a noncomedogenic agent derived from the distillation of petroleum in gasoline production, has been available for more than 100 years and is one of the more commonly used oils in skin products.5 It is important to note that occlusives are effective only while on the skin; TEWL returns to prior levels upon removal of the agent. In moisturizers, occlusives are often combined with humectants. Lanolin, paraffin, squalene, dimethicone, propylene glycol, beeswax, soybean oil, grapeseed oil,6 and other “natural” oils (e.g., sunflower seed, evening primrose, olive oil, and jojoba oils) are also among typically used occlusive ingredients.7–11 Linoleic acid, an omega-6 fatty acid present in sunflower, safflower, and other oils, is an essential fatty acid, obtained from the diet or through topical application, necessary for the production of ceramide in the skin′s barrier.
Humectants
Humectants are water-soluble substances with high water-absorption capacity. These compounds can attract water from the deeper epidermis and dermis in low-humidity conditions, which can aggravate dry skin.8 Consequently, humectants are combined with occlusive ingredients to achieve the desired effect. In cosmetic moisturizers, humectant ingredients protect against evaporation and thickening of the product, thus extending the shelf life. Humectants can also change skin appearance by drawing water into the skin, causing mild SC swelling that makes the skin look smoother and less wrinkled. Manufacturers often capitalize on this phenomenon in touting some moisturizers as “antiwrinkle creams” even though no long-term antiwrinkling effects are imparted. Glycerin, urea, sorbitol, sodium hyaluronate, propylene glycol, alpha hydroxy acids (AHAs), and sugars are among the normally used humectant ingredients. Glycerin (glycerol) is a potent humectant with hygroscopic ability comparable to NMF,9 paving the way for the SC to retain a significant amount of water even in a dry environment. Urea, included in hand creams since the 1940s,10 is a constituent of the NMF and displays mild antipruritic activity.11 Notably, the humectant hyaluronic acid does not penetrate into the dermis when applied topically.
Emollients
Emollients render a smooth appearance by filling the spaces between desquamating corneocytes and increasing cohesion, resulting in a flattening of the curled edges of the individual corneocytes. In addition, several emollients exhibit humectant and occlusive qualities. Occlusives that also confer an emollient effect include lanolin, mineral oil, and petrolatum. Several natural ingredients also impart such benefits. These include oatmeal, shea butter, vitamins C and E, coffeeberry, green tea, coenzyme Q10, niacinamide, soy, and glycyl-L-histidyl-L-lysineCu2+ (GHK-Cu), a copper tripeptide complex used for many years to enhance wound healing and more recently shown to augment collagen synthesis.12,13
Ideal moisturizers contain both humectant and occlusive ingredients. Glycerin is one of the better humectants because it can cross aquaporin channels and penetrate into the dermis. The best occlusive ingredients are oils that contain antioxidants and/or linoleic acid, including safflower, sunflower, olive, walnut, peanut, and grapeseed oils.
Sensitive Skin
Sensitive skin has defied easy characterization. Two classification systems have been proffered in the last 10 years, but a definitive typing system for sensitive skin remains elusive.24,25 Nevertheless, sensitive skin is classified in the BSTS based on clinical manifestations: Type 1 (open and closed comedones and pimples; the acne or S1 type); Type 2 (facial flushing due to heat, spicy food, emotion, or vasodilation; the flushing rosacea or S2 type); Type 3 (burning, itching, or stinging; the S3 type); and Type 4 (developing contact dermatitis and irritant dermatitis and often associated with an impaired SC; the S4 type) ( Table 2.2 ). Individuals can suffer from combinations of sensitive skin subtypes. The following discussion focuses on the primary topical treatments for sensitive skin.
Topical Treatments for Sensitive Skin
Corticosteroids
Corticosteroids block proinflammatory genes that encode cytokines, cell adhesion molecules, and other mediators, thus inhibiting the inflammatory process.26 In particular, corticosteroids selectively induce anti-inflammatory proteins such as MAPK phosphatase and annexin I, which physically interact with and suppress cytosolic phospholipase A2a (cPLA2a).27 Consequently, corticosteroids inhibit arachidonic acid release and a subsequent conversion to eicosanoids.28 The use of topical corticosteroids is generally safe for short-term treatment of inflammatory skin diseases. However, long-term use can produce adverse cutaneous effects (e.g., acne, folliculitis, hirsutism, purpura, pigmentary changes, skin atrophy, striae, and telangiectasia).29,30 Chronic topical corticosteroid use has also led to more serious systemic side effects, such as avascular osteonecrosis, glaucoma, hyperglycemia, hypothalamic-pituitary axis (HPA) suppression, and posterior subcapsular cataracts.31–39 Although corticosteroids can effectively treat rosacea, they should be avoided for this indication because their use engenders compensatory redness upon discontinuation and their protracted use can thin the skin.
S1—Acne S2—Rosacea S3—Burning and stinging S4—Susceptibility to contact and irritant dermatitis |
Cyclooxygenase Inhibitors
Several nonsteroidal anti-inflammatory drugs (NSAIDs) specifically target the bioactive lipids produced by arachidonic acid. For example, ibuprofen has shown success in treating acne because inflammatory acne lesions are infiltrated with neutrophils, and ibuprofen inhibits leukocyte chemotaxis.32 Sun-burn can also be treated with NSAIDs. In a randomized double-blind crossover study of 19 psoriatic patients receiving ultraviolet B (UVB) phototherapy conducted more than 30 years ago, researchers compared ibuprofen with placebo and evaluated signs and symptoms of UVB-induced inflammation. A statistically significant difference was found only in the technician′s assessment of erythema; however, findings suggested that ibuprofen was more effective than placebo in delivering symptomatic relief of UVB-induced inflammation following high doses of UVB-phototherapy for psoriasis. Based on the observation that dermal prostaglandins are increased after UVB irradiation, it is thought that an NSAID that interrupts prostaglandin synthesis may attenuate UVB-induced inflammation.33
Salicylic Acid
Salicylates have demonstrated anti-inflammatory and antimicrobial activity in experimental as well as clinical settings.34 Salicylic acid, a member of the aspirin family, interrupts the arachidonic acid cascade, thus exerting analgesic and anti-inflammatory effects. Salicylates control inflammation by inhibiting proinflammatory gene expression. Salicylic acid decreases the frequency and severity of acne eruptions by mitigating acne-related inflammation and delivering exfoliating activity to the pores. Because it is lipophilic, it is better able than glycolic acid to penetrate the sebum in skin pores, which accounts for its popularity in OTC acne products. Salicylic acid 2% cleansers are effective treatment options for rosacea patients with oily skin.
Sulfur/Sulfacetamide
Sulfur, usually an adjuvant therapy, is used primarily to treat acne, seborrheic dermatitis, rosacea, scabies, and tinea versicolor.35 Elemental sulfur and its various forms (e.g., sulfides, sulfites, and mercaptans) act as anti-inflammatory agents and reportedly display antifungal, antimicrobial, and antiparasitic activity.36 Sulfur is often combined with sodium sulfacetamide, a sulfonamide agent with antibacterial properties, specifically acting as a competitive antagonist to para-aminobenzoic acid (PABA), an essential component for bacterial growth,37 and Propionibacterium acnes.38 The keratolytic and anti-inflammatory activity of sulfur and the antibacterial properties of sulfacetamide in a topical formulation render an effective treatment for acne vulgaris, rosacea, and seborrheic dermatitis.39 Sulfur is often found with sodium sulfacetamide in cream, lotion, gel topical suspension, cleanser, and silica-based mask preparations. However, the odor of many of these products has been likened to rotten eggs, thus limiting their popularity.
Natural Ingredients
In the past 20 years, botanically derived products have gained widespread use and interest in the United States.40 Indeed, several such ingredients, including aloe vera,41,42 chamomile,43,44 feverfew,45,46 ginseng,47,48 licorice extract,49,50 mushrooms,51,52 oatmeal,53 selenium,54,55 and turmeric, have been shown in recent years to impart anti-inflammatory activity.56,57
Pigmented Skin
Skin color is derived fundamentally from the incorporation of melanin-containing melanosomes, produced by the melanocytes, into epidermal keratinocytes and their subsequent degradation. The focus of the BSTS system regarding this skin parameter is on general treatments for hyperpigmentation.
Tyrosinase Inhibitors
Tyrosinase is the enzyme that controls melanin production, as it is the rate-limiting enzyme for the biosynthesis of melanin in epidermal melanocytes. Given what appears to be its pivotal role in melanogenesis, tyrosinase activity is targeted in various products designed to decrease melanin formation by suppressing tyrosinase.
Hydroquinone
The use of hydroquinone (HQ) leads to the reversible suppression of cellular metabolism by affecting both DNA and RNA synthesis. In addition, HQ efficiently inhibits tyrosinase, diminishing its activity by 90 %.58 Although HQ is effective alone, it is usually combined with other agents (e.g., azelaic, glycolic, and kojic acids, and tretinoin).59 For many years, HQ was the first-line therapy for postinflammatory hyperpigmentation and melasma.60 Concerns about its safety, however, led to a ban for general cosmetic purposes in Europe in 2000. In Asia, HQ is legal but highly regulated. In the United States, the FDA has long been considering the status of HQ, but it has not yet decided whether to ban it in OTC products. HQ has never been etiologically linked with human cancer. Pigmentation of the eye and permanent corneal damage are the most serious adverse health effects seen in workers exposed to HQ.61 Exogenous ochronosis is also associated with topically applied HQ,62 although only 30 cases of ochronosis have been ascribed to HQ use in North America.63 Skin rashes and nail discoloration have also been linked to HQ use. The safety debate within the FDA about this standard-bearing tyrosinase inhibitor has provided the impetus for manufacturers to research and develop newer, less problematic skin-lightening agents.
Aloesin
Derived from aloe vera, aloesin inhibits the hydroxylation of tyrosine to DOPA, as well as the oxidation of DOPA to DOPAchinone, and it suppresses melanin production in cultured normal melanocytes.64 In a 2002 study on the inhibitory effect of aloesin and/or arbutin on pigmentation in human skin after UV radiation, investigators determined that pigmentation was inhibited compared with control: 34% by aloesin, 43.5% by arbutin, and 63.3% by the co-treatment with aloesin and arbutin.65 A study published that same year indicated that aloesin and some chemically related chromones inhibit tyrosinase more effectively than arbutin and kojic acid.66
Arbutin
Arbutin, a naturally occurring B-D glucopyranoside composed of a molecule of HQ bound to glucose, is found in the leaves of pear trees and herbs such as wheat and bearberry. The depigmenting mechanism of arbutin involves a reversible inhibition of melanosomal tyrosinase activity, rather than blocking the expression and production of tyrosinase.67 Traditionally used in Japan for depigmenting purposes, arbutin is now thought to be less effective than a synthetic derivative. Indeed, deoxyarbutin has shown, in vitro and in vivo, greater suppression of tyrosinase than arbutin.68
Kojic Acid
Kojic acid (5-hydroxy-2-hydroxymethyl-gamma-pyrone), a fungal metabolite of various species of Aspergillus, Acetobacter, and Penicillium,69 inhibits tyrosinase activity, mainly by chelating copper, leading to a cutaneous whitening effect.70 The combination of kojic and glycolic acids has been shown to be more effective than 10% glycolic acid and 4% HQ for the treatment of hyperpigmentation.71,72 Kojic acid 1% products are usually suggested for twice-daily use for 1 to 2 months or until the desired cosmetic result is achieved; however, sensitization to 1% creams has been reported.73 Kojic acid derivatives have been reported to exhibit enhanced efficiency by dint of greater skin penetration.74 They have been extensively used in cosmetic products, especially in Japan.75
Licorice Extract
Glabridin (Glycyrrhiza glabra), a key active ingredient in licorice extract, suppresses tyrosinase activity in cell cultures without altering DNA synthesis. In guinea pig skin, topical applications of 0.5% glabridin have exhibited the capacity to suppress UVB-induced pigmentation and erythema.76 In the clinical setting, glabridin has been used effectively to treat melasma77 and has also displayed a depigmenting benefit greater than HQ.78
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree