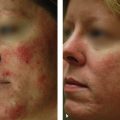
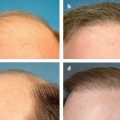
15 Surgical Treatment of Facial Scars
Key Concepts
Scarring occurs when injury extends to the deep dermis.
Unfavorable scar characteristics include excessive width, unfavorable depth, excessive length, and orientation inconsistent with underlying relaxed skin tension lines (RSTLs).
There are several surgical techniques and technologies that can be used to improve an unfavorable scar.
Introduction
Injury to, or disruption of, the deep dermis will result in the formation of scar as the skin heals. The scar appearance following wound healing depends on multiple factors, including genetic predisposition, age of the patient, direction of the scar, depth of the scar and associated tissue loss, technique of wound closure, and wound healing complications, such as infection. The goal in primary wound closure or secondary scar revision is minimizing and camouflaging the scar. The patient should be made aware that plastic surgery will not eliminate scars entirely, but it will help to make them less perceptible.
Background: Basic Science of Procedure
Scar formation is the process by which skin heals after injury in the deep layer of the dermis. Epidermal and papillary dermal injuries typically heal without scar formation. When skin injury extends to the deep papillary and reticular dermis, fibroblastic activity and collagen formation result in a scar. Normal wound healing can be categorized into three phases: inflammatory, transitional repair, and maturation. During the inflammatory phase of wound healing, an initial vasoconstriction is followed by vasodilatation secondary to histamine release. White blood cell migration into the site of injury will lead to phagocytosis of necrotic tissue, neoangiogenesis, and fibroblast stimulation.
The transitional repair phase or the fibroblastic phase usually begins a few days after the injury and lasts 4 weeks. Fibroblasts migrate to the site of injury and begin to produce collagen. Inflammation, continued collagen production, and cross-linkage of collagen fibers result in formation of thick, inelastic scar tissue. Some fibroblasts evolve into myofibroblasts, which express smooth muscle actin (s-SMA), causing tissue contraction. Myofibroblasts generally disappear from wounds within 1 month; their persistence has been noted in abnormal wound healing, such as keloids and hypertrophic scars. The final phase, maturation, begins 6 to 12 weeks after injury. During this period, the healing process is a mixture of new collagen formation and breakdown of old collagen.1
Nearly all scars improve as they mature over a period of 1 year. During the first 6 months, the most significant improvements occur, and the initial scar erythema tends to subside within this period. The scar itself becomes less indurated and softer, allowing better mobilization of the tissues in its vicinity. Scar hypertrophy often improves within a year. The timing of scar revision should take these factors into consideration. Unfavorable scar characteristics that can be improved by scar revision include the direction of the scar, the width of the scar, and the length of the scar, as well as other negative attributes, such as webbing and bowstringing. In general, scars that are greater than 2 cm in length and 2 mm in width may be improved by scar revision.
Pertinent Anatomy
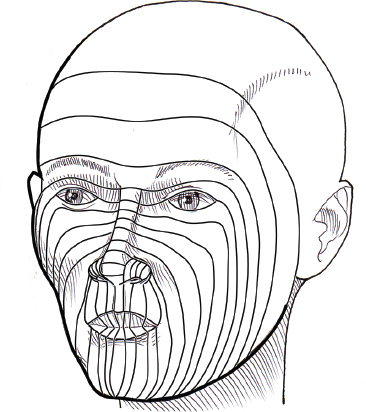
The camouflage of facial scars is most effective when scars can be aligned with the relaxed skin tension lines (RSTLs) or at the junction of the aesthetic subunits of the face. The RSTLs are generally perpendicular to the direction of the facial mimetic muscles. In older patients, the RSTLs are easily visible at rest; younger individuals need to be asked to make facial expressions to demonstrate the direction of the RSTLs. In the forehead and lower neck, the RSTLs are horizontal. In the crow′s feet and around the mouth, the lines are radial in direction. The lines are tangential in the cheeks and the lower eyelid region ( Fig. 15.1 ).2
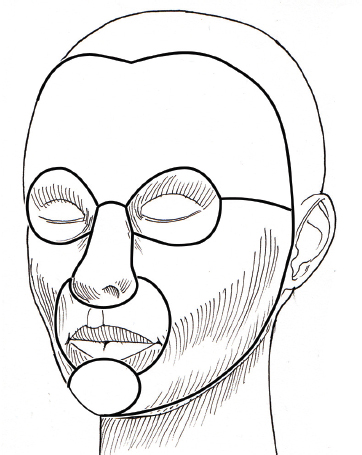
Aesthetic facial units comprise the different features of the face with unique color, texture, and topography. Certain facial units can then be divided into subunits based on skin thickness and anatomical topography. Scars that are located along anatomical facial subunits are less noticeable ( Fig. 15.2 ).
Patient Selection
Facial scars are especially distressing to patients because they cannot be covered with clothing. Women who wear makeup can camouflage scars to a certain degree. Facial scars may be noticeable due to their width, orientation, and distortion of facial features. The ideal facial scar is narrow, flat, and a good color match to surrounding tissues, and it does not distort adjacent anatomy. The scar is preferably aligned with the RSTLs or located at the junction of facial subunits. Prior to the start of treatment, the treating physician should present the options and outline the possible need for multiple procedures. The limitations of scar revision need to be discussed so that the patient can have realistic expectations of treatment.
Additionally, patients who seek scar revision may have suffered psychological trauma from the accident or the assault that caused the injury. In most instances, passage of time will allow the patient to adjust psychologically to the presence of a scar. However, when there are signs of a posttraumatic disorder, the patient should be evaluated and treated by a qualified mental health professional, because healthy psychological adjustment will allow the patient to better cope with recovery from scar revision.
Technical Aspects of Procedure
The scar revision options to be presented can be used serially or concurrently. Generally, surgical scar revision is followed by nonsurgical scar revision maneuvers. Scar revision should result in minimal tension at the wound edges because wound tension increases the risk of scar hypertrophy or keloid formation.
Surgical Scar Revision
During surgical scar revision, anesthesia choice is dependent on the extent of the procedure, the age of the patient, and the level of anxiety. Most scar revisions can be safely and comfortably performed under local anesthesia utilizing 1% lidocaine with 1:100,000 epinephrine. In children or anxious patients, general anesthesia or monitored sedation is more appropriate. Prior to infiltration of local anesthesia, the surgical incisions, the RSTLs, and the borders of the facial subunits should be marked with a surgical marker because infiltration of local anesthesia can distort normal anatomy.
Proper instrumentation, including fine tissue forceps, single and double hooks, and delicate scissors and needle drivers, facilitate nontraumatic tissue handling during facial scar revision. Minimal use of cautery is also advised in an attempt to preserve maximal blood supply to the wound edges. Plastic surgical techniques of minimal tissue injury, appropriate wound undermining, layered skin closure, and effective wound dressing should always be used in facial scar revisions.3
Direct Excision
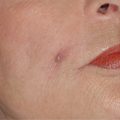
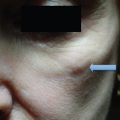
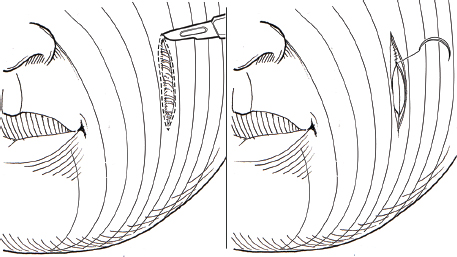
Wide scars can be appreciably improved by simple scar excision and skin repair. The scar is removed in fusiform fashion and wound edges are undermined in a subdermal plane. The incision is then repaired in a layered fashion, resulting in a more refined scar. This simple technique is especially useful in treating traumatic scars that are parallel to the RSTLs ( Fig. 15.3 ).
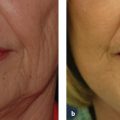
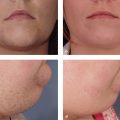
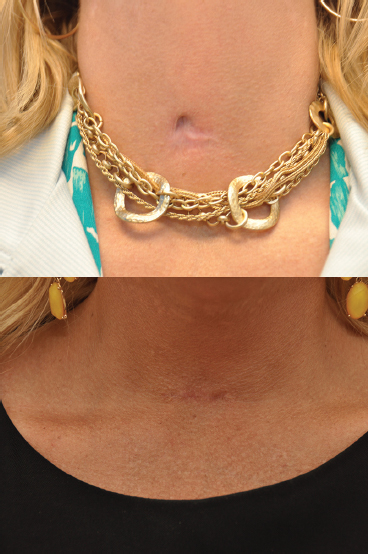
In wider scars where fusiform excision would create a wide defect that would be difficult to close directly, serial excision may be used. Serial excision is often used in removal of large, nonmalignant skin lesions. In this technique, a smaller central portion of the scar is removed, and the narrower scar is allowed to heal. Secondary or tertiary excisions will then be performed to remove the entire scar and allow closure under minimal tension. In Fig. 15.4 , the patient had a tracheotomy scar healed with an excellent result by following the relaxed tension lines of the inferior cervical regions.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree