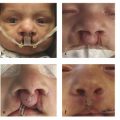
17 Secondary Cleft Lip and Nasal Reconstruction
Summary
Secondary cleft lip and nasal deformities following primary cleft surgery represent some of the greatest reconstructive challenges and have inspired a multitude of creative technical solutions. Each secondary deformity is unique and must be evaluated independently with reconstructive plans grounded in principles rather than a formulaic approach. The number of described techniques is vast with limited evidence-based research to validate one method over another. However, techniques that are reliable in the experience of the authors will be presented to guide the plastic surgeon.
This review will discuss the important preoperative considerations in cleft lip and nose repair. Key physical exam findings will be presented. The philosophy of timing on secondary reconstruction will be explained including what the authors consider to be the major pitfalls in surgical approach.
Principles of secondary cleft lip reconstruction for unilateral and bilateral cleft deformities will be discussed followed by principles of secondary cleft nasal reconstruction of unilateral and bilateral cleft deformities. While an exhaustive review is impossible given the space limitations, this review will acquaint the reader with the major challenges and the available techniques in this field.
17.1 Influence of Primary Cleft Lip and Nasal Surgery
The first cleft operation is the best opportunity to achieve optimal results. Any revisionary surgery will be compromised by previously existing scars and violated tissue planes. When results are suboptimal at the initial surgery, revisionary surgeries become more challenging. Therefore, it is imperative to achieve the most aesthetic, functional, and lasting results at the first operation.
Our center has benefited from the implementation of nasoalveolar molding (NAM) into our presurgical treatment plan. NAM rotates the displaced alveolar segments into orthotopic position, lengthens the columella, increases nasal tip projection, folds the lower lateral cartilage toward its native form, medially transposes the lower lip and alar base, and stretches the intranasal lining. Multiple studies have documented the lasting benefit to nasal aesthetics following NAM and primary cleft lip and nasal reconstruction. Patients with unilateral cleft lip who undergo NAM demonstrate greater nasal symmetry through age 9. Patients with bilateral cleft lip who undergo NAM have a longer columella and near normal nasal morphology through 12.5 years of age.
Presurgical orthopaedics facilitates gingivoperiosteoplasty (GPP) and primary nasolabial fistula repair; however, NAM requires frequent follow-up and diligent care on the part of both the parents and the orthodontist. Alternative dentofacial orthopaedics such as the Latham device are preferred by other centers. As described by Millard, dentofacial orthopaedics drives closer to completion the failed embryonic migration.
At the time of primary repair, exact intraoperative markings, precise incisions, and gentle handling of the tissue are all crucial for an optimal result. Cleft care delivered by high-volume centers with a multidisciplinary team approach is critical to maintaining excellent results. Minimum guidelines for cleft teams have been created jointly by the American Cleft Palate-Craniofacial Association and Cleft Palate Foundation.
Reports by McComb and Salyer demonstrated the safety and aesthetic advantage to primary cleft rhinoplasty. Long-term follow-up supports the overall safety of primary rhinoplasty on subsequent nasal growth. Although primary and revision cleft rhinoplasty are standard practice, great variability exists in approach. Plastic surgeons must remember that all primary repairs must consider the final on-table result in the context of long-term changes or the “fourth dimension” of time. Mulliken and LaBrie have characterized the specific anthropometric measurements that are altered in the fourth dimension. Cleft-side alar base drifts laterally (sn-al distance) and should be positioned more medially at cleft repair. Labial height (sn-cphi distance) lags on the cleft side and should be slightly greater on the cleft side at the time of repair. Finally, transverse labial width (cphi-ch) grows more on the cleft side and should be set shorter on the cleft side.
17.2 Timing of Secondary Cleft Lip and Nasal Surgery
In this chapter, we define rhinoplasty as primary when performed during the initial cleft lip repair, immature when performed after primary rhinoplasty but prior to facial maturity, and mature when performed at or after the time of facial maturity. Limited secondary cleft lip revision and immature rhinoplasty can be performed as early as age 5 or 6 prior to the child’s entry into school to reduce social stigma during peer interactions. Early reconstruction is considered when patients have significant deformity or are suffering socially in peer interactions.
Because the nose grows until adolescence, rhinoplasty was often deferred until the later teen years. Ortiz-Monasterio and others have demonstrated excellent long-term follow-up even when rhinoplasty was performed prior to age 12. However, at this early age rhinoplasty precedes orthognathic surgery. Maxillary advancement alters the anthropometric dimensions of the nose, increases tip projection and nasolabial angle, and restores aesthetic balance to the face. As facial proportions are evolving and future rhinoplasty may still be required, the authors caution against comprehensive nasal surgery prior to facial maturity. Furthermore, patients prior to skeletal maturity may not have the cognitive maturity to verbalize their goals and concerns in immature rhinoplasty. At the time of facial maturity, patients become willing participants in their own care.
The great enemy of the refined soft-tissue repair is scar. Therefore, primary cleft rhinoplasty should achieve an aesthetic and lasting change using the least amount of dissection. The ideal is one rhinoplasty surgery during primary cleft lip repair and a second at the time of facial maturity. Active cleft surgeons are familiar with the scarred nasal tip resulting from excessive operations that resists the most elaborate technical maneuvers. The underoperated nose can be predictably improved although perfection is elusive. The overoperated, scarred nose can produce unfortunate, complex, and irreversible hurdles to an already challenging operation which, in many cases, can be avoided with proper planning, and an appreciation of the larger picture. Ultimately, the surgical philosophy of the authors is to effect the greatest change with the fewest number of surgeries and new scars. Diligence at the primary cleft lip and nose repair can reduce the number of surgeries required and avoid school-age interventions.
17.3 Secondary Correction of Unilateral Cleft Lip Deformities
Treatment of unilateral cleft lip deformities varies depending on the etiology of the deformity. Obtaining operative reports when the patient had the repair elsewhere may help with surgical planning, but in the authors’ experience these reports add limited value compared to a good history and physical exam. Deficiencies can occur at each segment of the repair. Techniques will be characterized by vermilion deficiency, white roll misalignment, and a vertically short lip. When the deformity is significant, revising the entire cleft lip repair is the better intervention.
17.3.1 Vermilion Deficiency
Vermilion deficiency can result from insufficient attention during reconstructive planning of a primary lip repair, inadequate or incomplete repair of the orbicularis oris, or wound breakdown in the area of the vermilion. The two main categories of vermilion deficiency are loss of the vertical height of the vermilion and misalignment of the red line separating the dry from the wet vermilion. In Asians, African Americans, and Latino patients, discrepancies of the red line can be quite noticeable and therefore should be addressed at the time of lip repair. A modification of Noordhoff’s triangular flap can restore the vertical height of the vermilion and reposition the red line.
During reconstruction, attention should be directed to careful repair of the orbicularis oris. Incomplete muscle repairs can result in loss of vertical height of the upper lip and vermillion. As scars in the vermilion tend to heal well, there should be a low threshold for excision of the affected vermilion and upper lip as part of the reconstructive plan.
For minor deficiencies isolated to the vermilion, fat grafting to the lip is a useful and minimally invasive technique that can be performed in the office. Overcorrection is preferred with an expectation that some fat will resorb, even in a well-vascularized bed such as the lip. Although the technique is reproducible, patients should be aware of the possible need for repeat surgery, particularly in the scarred vermilion.
Dermal grafting to the deficient vermilion also can restore volume. The most common criticism of dermal grafting is firmness and poor integration with the surrounding lip architecture. Local mucosal flaps have limited application outside mild deformities as deficiencies in this area are rarely isolated to the mucosa alone.
17.3.2 White Roll Misalignment
Misalignments of the white roll as small as 1 mm are noticeable at conversational distance. The step-off can be corrected with asymmetric Z-plasty or a diamond-shaped excision. Asymmetric Z-plasty can effectively align the two borders of the vermilion, but introduces a new oblique scar along nonanatomic landmarks of the upper lip. Patients with a predisposition for poor scarring are at risk for additional morbidity.
Diamond-shaped excision effectively lowers the white roll border to provide an upper lip height match in small discrepancies. As the incision line is hidden within the scar line of the previous lip repair, no new scars are formed. For this reason, the diamond excision technique is favored by the authors to correct minor discrepancies of the white roll.
White roll discrepancies of greater than 2 mm require re-creating the cleft deformity and repairing the cleft de novo. In these cases, the lip should be treated as a vertically short lip.
17.3.3 Vertically Short Lip
The vertically short lip can result from a planning error, technical error, or poor scar formation. Poor scar formation is related to patient biology and unlikely to be affected by revisionary surgery. Because poor scarring can haunt the cleft surgeon, careful physical examination should evaluate the presence of scar in other parts of the body or cleft repair. Poor upper lip scars share features of widening, placement lateral to the philtral line, and have wide areas of white roll disruption.
When there is a vertical discrepancy of greater than 2 mm between the cleft and noncleft philtral columns or when scars are wide and prominent, a cleft lip re-repair is advocated in the form of either a rotation-advancement or a straight-line repair.
Up to 25% of the upper lip can be excised without causing a disturbance in lip dynamics. Every effort should be made to completely excise all scarred areas of skin and muscle, restore vertical height of the lip, and locate the final scar along the philtral line.
Widened and prominent scars of the lip skin commonly overlie wide scars of the orbicularis oris. Incomplete muscular repair at the time of cleft repair may result in bulging of the affected upper lip with animation or vertical shortening. The surgeon should have a low threshold for resection of scar tissue in the orbicularis oris and complete reconstruction of the vertical height of the muscle.
17.4 Secondary Correction of Bilateral Cleft Lip Deformities
The secondary deformities affecting the unilateral cleft lip can occur in the bilateral cleft lip. However, the anatomic derangement is more complicated, as are the surgical techniques required for correction. Due to space limitations, deformities related to alveolar clefts, displacement of the premaxilla, and oronasal fistulae will not be covered in this review. A malpositioned maxilla can have profound effects on nasal and upper lip form. The underlying bony foundation should be addressed prior to definitive lip or nose surgery.
Common bilateral cleft lip deformities include excessive scarring, a vertically short upper lip, and discontinuity of the white roll. Bilateral cleft lip repair requires the formation of two parallel, closely apposed incisions. Therefore, patients predisposed to excessive scarring will be at risk for suboptimal results even in the best of hands.
Some bilateral cleft lip repair techniques do not adequately reconstruct the entire orbicularis oris. In some cases, the muscle is not reconstructed at all. Absence of an intact oral sphincter interferes with creation of an appropriate prolabial width, adequate vertical height of the upper lip, and alar base position. The absence of orbicularis oris continuity is highlighted during puckering or whistling.
The midline tubercle of the vermillion should be assessed for presence and fullness. The height and width of the prolabium and the quality, location and area of the philtral scars are scrutinized and documented. Manchester reconstructions of the midline tubercle are antiquated, unaesthetic techniques that should be abandoned.
If enough unscarred philtrum exists, a bilateral cleft lip re-repair can adequately address the secondary deformities of the bilateral cleft upper lip. Provided that there is adequate tissue to create a columella-based philtral flap, surrounding scar affecting the upper lip skin, muscle, and mucosa is completely resected. If the lower lip is protrusive after orthognathic correction, the patient may be better served by an Abbe flap.
During bilateral cleft lip re-repair, vermillion turndown flaps are created from the lateral lip elements similar to primary lip repair. Care should be taken to reconstruct the entire length of the orbicularis oris at the midline. Wide dissection across the face of the maxilla may be necessary to relieve tension at the midline. Through this controlled reconstruction, vertical height of the upper lip and vermilion tubercle can be restored and unaesthetic scars replaced. Surgeons must anticipate additional widening of the prolabium with time. Philtral width is set narrower than desired to allow for stretching of skin with healing and activation of the orbicularis oris muscle. As will be discussed later, the forked flap advocated by Millard for primary bilateral cleft lip repair has no role in the modern techniques in cleft nasal reconstruction.
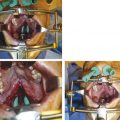
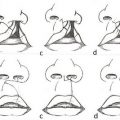
An Abbe flap can restore composite deficiencies in skin, muscle, vermilion, and mucosa to the midline upper lip in cases of excessively scarred or short philtrum (Fig. 17‑1). The Abbe flap serves to both augment the upper lip and reduce the lower lip volume, thereby restoring aesthetic balance to the mouth. The authors’ preference is to perform the Abbe flap following definitive orthognathic surgery and secondary cleft rhinoplasty revision except in cases of severe distortion of the upper lip. The preference of the authors is to extend the Abbe flap onto the columella to avoid a depressed scar at the lip–columella junction. The fibrofatty tissue at the base of the prolabium is rolled onto itself superiorly to provide bulk and take the place of an absent anterior nasal spine.
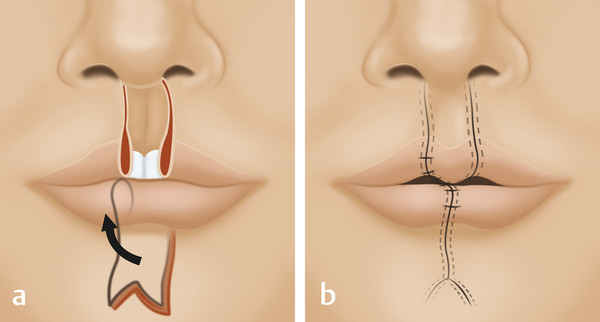
The Abbe flap is designed narrower than needed for the same reason that the prolabial segment is created narrower at the initial bilateral cleft lip repair. Care is taken to prevent any vermilion misalignment of either the upper or lower lip during flap inset and donor site closure. Loosely tied wires can be placed between the maxillary and mandibular teeth if there is any concern regarding patient compliance. However, given this procedure is typically performed in patients who are at least adolescents, there should be active involvement and investment on the part of the patient. Flap division is performed in an office setting one to two weeks later. The preference of the authors is to perform an Abbe flap in isolation without any other concomitant adjustments to preserve the integrity of the final result. However, other centers advocate combining the Abbe flap with a secondary rhinoplasty in the same stage.
As in unilateral deformities, fat and dermal grafting may be utilized for minor vermilion deficiencies that exist in isolation of other upper lip deformities. Similarly, V-Y advancement can be used to lengthen a deficient mucosa or vermilion although with limited efficacy.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree