13 Unilateral Cleft Lip
Summary
Careful preoperative preparation of an infant with a cleft lip requires addressing feeding issues and ensuring that there are no comorbidities. If a complete cleft lip is present, preoperative dentofacial orthopedics will aid in preferred arch and alar base alignment. A lip adhesion may be pursued to address the arch and alar base alignment, decrease the tension at the repair site, and increase length of the medial element. Meticulous measurements and markings for a rotation–advancement repair allows for accurate placement of the nasal sill, philtrum, Cupid’s bow, vermilion, and mucosa of the upper lip. Synchronous nasal correction of the alar cartilage, alar base, caudal septum, as well as the vestibular web is imperative for removing the stigma associated with a cleft.
13.1 Introduction
The commonly quoted incidence of cleft lip and/or palate of 1 in 1,000 live births does not reveal the complexity of treatment of this congenital anomaly. As a result of a genetic or environmental mishap, the lip, alveolus, and palate may fail to fuse and result in a cleft lip and palate. This cleft may cause problems with breathing, chewing, sucking, speaking, hearing, swallowing, and appearance. It takes a combined effort of teams of health care professionals to undo the effects of this deformity.
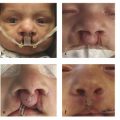
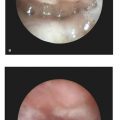
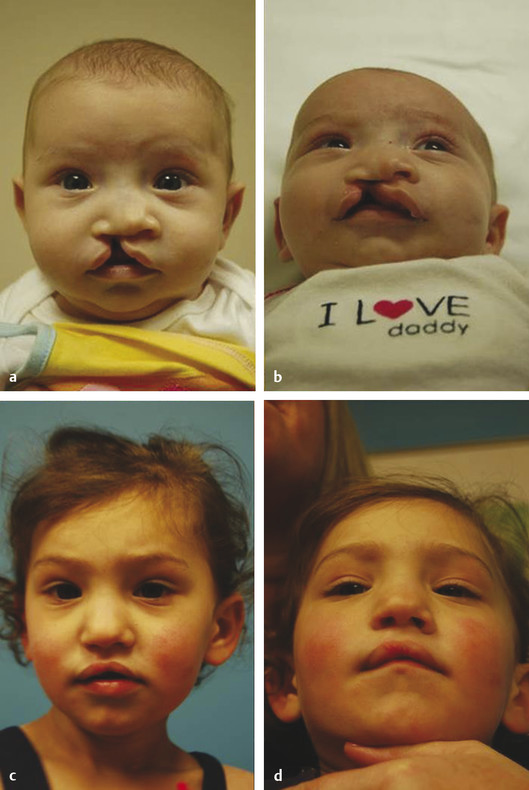
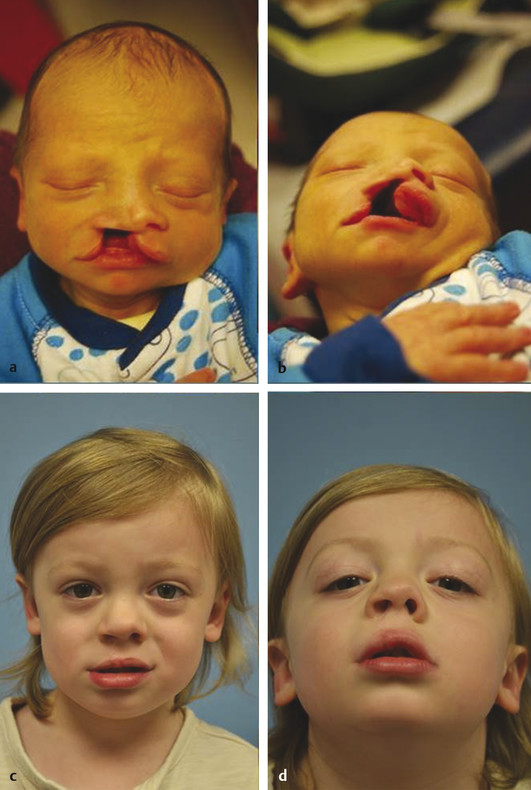
Cleft lip represents a failure of the medial nasal process to fuse with the maxillary processes on each side. Several genes are activated and deactivated in the first 3 to 8 weeks of life, which are critical to formation of the lip and nose. Genetic variability of this process of migration results in phenotypic heterogeneity. Consequently, clefts of the lip may be unilateral or bilateral and complete or incomplete. A complete cleft lip may have a skin bridge between the medial edges of the nasal floor, known as a “Simonart’s band.” A minor form of an incomplete cleft is referred to as a microform cleft lip (Fig. 13‑1 and Fig. 13‑2).

It is important to realize that the origin of the cleft can also produce other congenital anomalies. In fact, 35% of all infants with cleft lip and palate have additional associated anomalies. This incidence rises to 54% for infants with a cleft palate alone. Therefore, when evaluating a patient with cleft lip and palate, it is necessary to perform complete physical and genetic workup.
Periodically, such anomalies occur together and are named after their descriptor, given there is no apparent singular cause. Presumably, the multiple anomalies that make up the syndrome are related. Numerous syndromes that involve orofacial clefting have been delineated. As research in genetics grows, the source of some of these syndromes has been isolated. Common syndromes associated with cleft lip include Shprintzen’s (velocardiofacial syndrome; 22q11 microdeletion) and van der Woude’s (IRF6 mutation) syndromes.
With the increasing sophistication of ultrasonography, the anatomy of the lip can now be discerned prenatally. If a complete cleft is present, it may be detected by 16 weeks, and an incomplete cleft can be detected by 27 weeks. A prenatal consultation with the mother can help allay her fears and offer expectations for surgical treatment. Obstetric anxiety can also be reduced with a simple statement of hope, describing accomplishments of other children with cleft lip and palate.
Once a child is born with a cleft, the most pressing concern is feeding. Since such infants are unable to form a seal around the nipple to produce adequate negative pressure required for sucking, they are faced with an immediate problem. This can be ameliorated by using a modified nipple (wider aperture and squeeze chamber), such as a Mead Johnson’s or Haberman’s nipple, as well as several others that are commercially available. Our team uses Dr. Brown’s nipple as a first-line measure, which relies on alveolar compression to open the aperture. This allows the infant to control the flow to some extent.
After the baby is able to feed and demonstrates growth, surgical correction can be pursued. Although not supported by scientific evidence, Wilhelmsen and Musgrave emphasized the “rule of 10”: weight 10 lb, hemoglobin 10 grams, and age 10 weeks. However, in some cases, the option of a lip adhesion may be considered before definitive lip and nasal correction. If the lip adhesion is performed after 10 weeks, a definitive repair may be scheduled 2 to 3 months later.
13.2 Evolution of Care
The first cleft lip repair was reportedly performed by an unidentified Chinese physician in 390 AD. It was not until 1310 when Jehan Yperman (1295–1351), a Flemish surgeon, provided the first description of the procedure. In his repair, Yperman recommended a straight-line closure reinforced by passing a long needle through each side of the lip and fixing the needle shaft with a figure-of-eight suture. This was refined by French surgeon Ambroise Pare, who, in 1575, provided the first illustration of the lip correction with a similar technique. Early techniques in cleft lip repair mostly involved a straight-line closure. Later, these evolved to include other methods using geometric advancement flaps and Z-plasties. By the mid-20th century, the two most widely used repairs were those of LeMesurier and Tennison.
While stationed as a Navy surgeon during the Korean War, Dr. Ralph Millard grew dissatisfied with the results he obtained from the LeMesurier technique. He noted that although most of the Cupid’s bow, one philtral column, and the philtral dimple were all intact on the medial side of the cleft, they were all rotated upward. Rather than disturbing these structures as in previous repairs, he believed that these only need to be released from their attachments and rotated downward to achieve normal position. These observations led Millard to develop the rotation–advancement technique, which to this day remains the basic foundation for unilateral cleft lip repair in most cleft centers throughout the world.
13.3 Normal and Cleft Lip Anatomy
Successful correction of a cleft lip is directly related to the ability to restore the appearance and functionality of the upper lip, through proper mobilization and accurate repair of the orbicularis oris muscle. The orbicularis oris is a fanlike structure with a superficial component and a deep component. The former, in association with extrinsic facial muscles, serves as a retractor of the upper lip. The deep component of the orbicularis oris, subdivided into pars marginalis and pars peripheralis, is responsible for the sphincteric action of the mouth. The pars marginalis forms the innermost layer of the oral fissure and is surrounded by the pars peripheralis in a concentric manner.
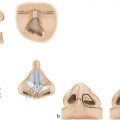
Abnormalities in muscular anatomy vary, depending on the severity of the cleft lip. The deficiency of the orbicularis is more marked on the medial side than on the lateral side. In incomplete clefts, even though some muscular fibers remain in the upper portion of the lip, these seem to be attenuated and lacking sphincteric action. In the complete cleft lip, the general direction of muscle fibers parallels the cleft margins. The pars marginalis is interrupted on either side of the cleft at the point where the vermilion–cutaneous junction becomes thin. The peripheralis on the lateral side has abnormal insertions to the alar base and the periosteum of the piriform aperture. Similarly, on the medial side, it has insertions to the columella, nasal septum, and anterior nasal spine (Fig. 13‑3).
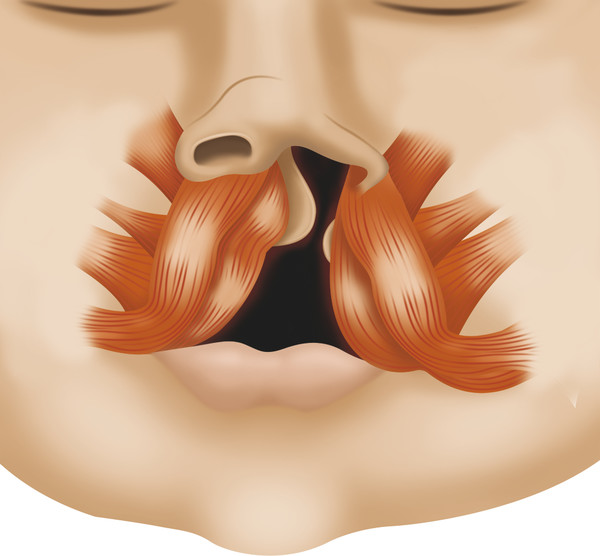
Mulliken noted that in the normal Cupid’s bow, the anterior projection of the pars marginalis gives rise to the white roll or vermilion–cutaneous junction. However, in the affected lip, the pars marginalis was found to be both hypoplastic and disoriented adjacent to the cleft. Furthermore, the vermilion width, though normal on the lateral side, was significantly deficient on the medial side of the cleft lip.
Emphasizing on the importance of the natural-appearing philtral column during cleft lip correction, Mohler (1987) created a classification of philtral configuration. Type 1 is most common, with some degree of divergence of the philtral column at the base of the columella. Type 2 has a degree of convergence at the base of the columella. Lastly, type 3 has a convergence below the base of the columella.
13.4 Anthropometry of the Lip
Before any attempt to correct a deformity, the norm has to be correctly understood. Farkas has documented the normal anthropometry of the face in detail. Such measurements offer valuable insight into the structural growth of the nasolabial complex. By using this guide, a lip may be constructed to achieve optimal results. It is crucial to maintain photographic and numeric records, so that an accurate assessment can be done on the results of a surgeon’s protocol. Newer three-dimensional anthropometry systems are particularly convenient, as they can record accurate measurements in a split second.
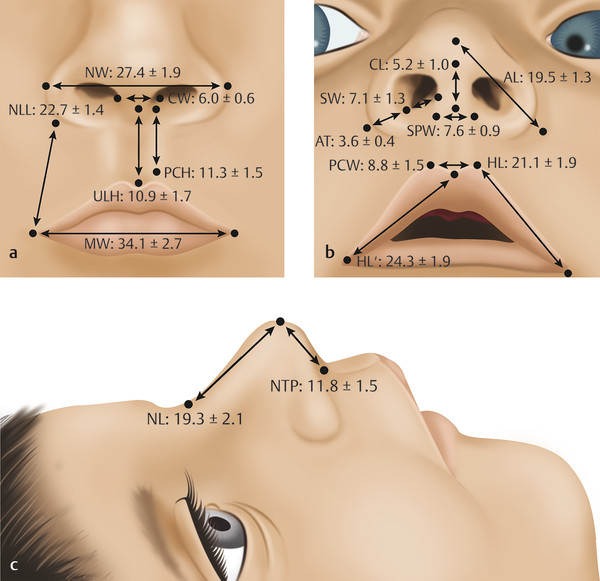
Farkas et al (1992) found that cutaneous upper lip height reached approximately 80% of its growth potential by 1 year of age and 94% by 5 years of age. Likewise, upper lip height and nasal and prolabial width show rapid growth early in life. This is in contrast to the columellar length and nasal tip projection, which show slow growth. Measurements should be made to intentionally overcorrect the slow-growing structures, as opposed to the fast-growing structures. Such distinction between fast- and slow-growing nasolabial elements is the key to planning a correction in the fourth dimension. Using anthropometric measurements, Thomas et al (2013) recently reported on normal nasolabial anatomy in infants younger than 1 year (Fig. 13‑4).
13.5 Anatomy of the Cleft Nasal Deformity
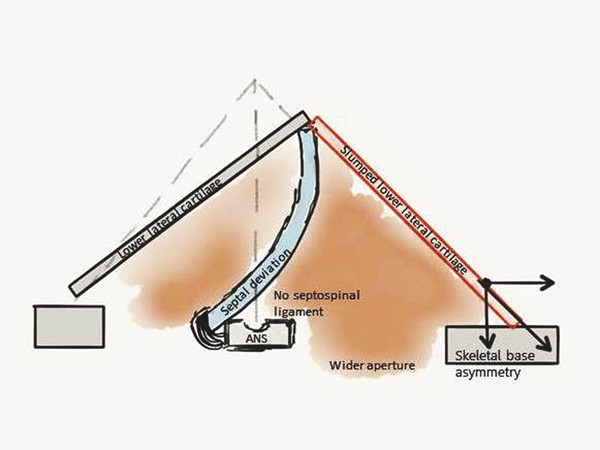
Pathogenesis of the cleft nasal deformity can be attributed to three major factors: (1) muscle imbalance, (2) septal deformity, and (3) asymmetry of the skeletal base. The extrinsic muscles of facial expression, attached to the orbicularis oris muscle on the cleft side, are responsible for the lateral pull of the alar base. Contraction of the unopposed orbicularis muscle insertion on the medial side results in pulling of both the septum and the columella to the noncleft side. Further contributing to the septal deformity is the septospinal ligament, which is also unopposed on the normal side, fanning from the caudal border of the septum to the anterior nasal spine. This causes the caudal septum to be hypertrophied and dislocated off the spine, away from the cleft.
Hypoplasia (or posterior location) of the lesser maxillary segment and an asymmetric skeletal base contribute to a generalized displacement of the nasal pyramid toward the cleft side and to the resultant stretching and flattening of the dome of the alar cartilage. The lower lateral cartilage is inferiorly distracted, and its normal overlapped relationship with the upper lateral cartilage is distorted. As a result, a buckling deformity of this cartilage is usually noted. The orientation of the medial and lateral crura of the alar cartilage on the cleft side is also affected. The medial crus is inferiorly displaced on the cleft side, whereas the lateral crus is usually rotated inferiorly (Fig. 13‑5). The nasal vestibular mucosa is also stretched secondary to the width of the cleft. A combination of excess mucosa and displacement of the lateral crus of the lower lateral cartilage can result in a vestibular web after correction of the cleft lip.
13.6 Preoperative Management
13.6.1 Dentofacial Orthopedics
There are a variety of options for presurgical treatment of the alveolus. They vary depending on expertise, accessibility, finances, and individual protocols. There are three basic methods of presurgical molding: taping, passive molding, and active orthopedic devices. Taping is the simplest method, with external force placed by gradual approximation of the cleft edges of the lip with adhesive tape. A dental plate may be used in conjunction with taping to prevent collapse of the lesser segment. However, accurate alignment is challenging, and dermatitis and epidermolysis from frequent tape removal can be annoying. Alveolar approximation is also possible by progressive molding of a dental plate. The dental plate is held in place with an adhesive and gradually shaved on the palatal surface. External force by taping assists in moving the arches along this molded surface. Since infant cartilage can be molded nonsurgically, a nasal phalange is added when the interalveolar distance is less than 6 mm. This nasal molding bulb is progressively straightened to achieve an excellent preoperative position of the affected lower lateral cartilage. Usually, this process takes 10 to 12 weeks. A simultaneous correction of the lip, nose, and alveolus (gingivoperiosteoplasty) is possible after nasoalveolar molding (NAM).
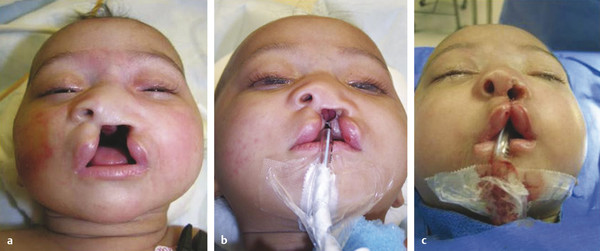
An active dentomaxillary or Latham appliance accomplishes alveolar alignment much more quickly (4–6 weeks). A custom-made prosthesis is secured to the palate with pins (under a brief anesthetic). A screw is turned weekly to activate an arm that moves the lesser segment anteriorly along the radius of the arm. An auxiliary elastic chain can be engaged to assist in decreasing the interalveolar gap. A stronger force is applied on the maxillary segments for proper positioning. Presurgical orthopedics effectively narrows the cleft, facilitating primary repair and decreasing the need for secondary repair. No long-term effects have been noted with use of dentofacial orthopedics (Fig. 13‑6). Proponents of active dentofacial orthopedics tout the ability to move the lesser segment anteriorly in infants with significant anteroposterior (AP) discrepancy (Fig. 13‑7).

13.7 Operative Treatment
13.7.1 Lip Adhesion
A lip adhesion can be a useful adjunct in the treatment of a complete cleft lip. An adhesion may be used instead of or in conjunction with dentofacial orthopedics. If access to presurgical orthopedics is unavailable, a lip adhesion can be performed as a staged procedure to narrow the cleft and approximate the dental arches, allowing for staged correction of the nasal deformity (Fig. 13‑8). This may decrease the number of secondary procedures necessary. However, many centers have abandoned a preliminary adhesion, given that it may lead to exposure to anesthesia complications and scarring, and may add to cost.
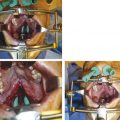
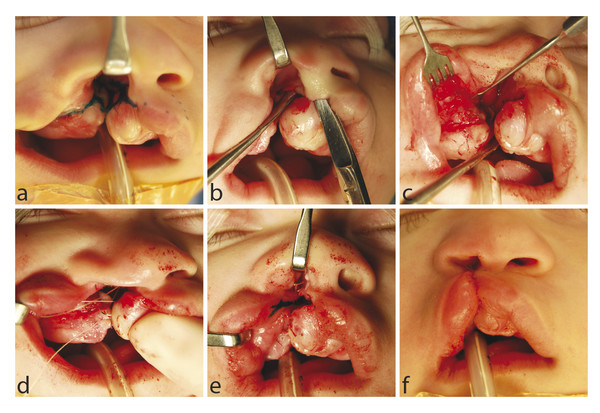
Markings for a lip adhesion are made beyond any landmarks that are important for the eventual cleft lip correction. On the medial side, a linear incision is marked 2 mm beyond the vermilion–cutaneous junction that extends along the base of the caudal septum. On the lateral side, a similar, corresponding incision is marked in the lip (beyond the vermilion–cutaneous junction) to the level of the piriform. A perpendicular incision is marked from the vestibular–piriform margin along the lateral buccal sulcus. The lip incisions are made to the level of the submucosa, until the underlying muscle is visualized. However, the muscle is not dissected. The cheek is elevated along the supraperiosteal plane, so it may be advanced across the cleft for a tension-free closure. A back cut in the mucosa greatly assists in advancing the flap along the buccal sulcus, and the posterior mucosa of the adhesion is closed. The nasal floor is constructed by apposing the septal mucoperichondrium and the lateral vestibular mucosa. Interrupted sutures are placed in the muscular layer, and the anterior mucosa is carefully approximated. Thin adhesive skin-closure strips (Steri-Strips) reduce the tension across the adhesion in the immediate postoperative period. Typically, the final correction of the cleft lip is delayed for 2 to 3 months after the adhesion (Fig. 13‑9).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree