14 Laser Treatment of Facial Scars
Key Concepts
Lasers interact with tissue chromophores (hemoglobin, water, and melanin) to selectively target cutaneous structures.
Lasers induce tissue remodeling to smooth the contour of both hypertrophic (thickened) and atrophic (depressed) scars.
The vascular-specific pulsed dye laser (PDL) is useful for hypertrophic scars, keloids, and erythematous traumatic and acne scars. The PDL can be combined with fractional laser resurfacing to maximize improvement in skin texture.
Atrophic scars are best treated by resurfacing with nonablative or ablative lasers. Fractional resurfacing modalities are associated with shorter recovery times and lower risk of complications than nonfractional laser techniques. Clinical efficacy increases as repeat treatments are applied.
Patients should be carefully selected and treated at appropriate intervals to ensure gradual improvement in their scars with low risk of complications. Meticulous attention to preand postoperative care is essential.
Introduction
Cutaneous injury from acne, surgery, trauma, or any inflammatory process may result in scarring and disfigurement. Most importantly, scars lower self-esteem and limit a patient′s social interaction. Effective treatment for scars is essential because it can greatly improve a patient′s quality of life. Treatments for scars have included various physical, chemical, and surgical options and, in the past few decades, laser technology has dramatically improved treatment outcomes for all types of cutaneous scars.
The first lasers used to resurface scars were continuous-wave argon, neodymium:yttrium-aluminum-garnet (Nd:YAG), and carbon dioxide (CO2) systems. These devices resulted in an unacceptably high risk of tissue necrosis and scar recurrence. In the 1980s, pulsed lasers were developed that allowed for selective absorption of laser light by target chromophores (e.g., hemoglobin, melanin) in the skin to induce temperature-controlled, target-specific injury without damage to surrounding healthy tissue.1 The first series of clinical studies published in the early 1990s showed sustained improvements in erythematous, hypertrophic scars and keloids using the pulsed dye laser (PDL).2–6 Additionally, laser skin resurfacing with CO2 and erbium systems has been used successfully over the past 15 years to improve atrophic scars and other textural abnormalities. Recent improvements in technology have introduced fractionated laser systems that deliver energy in microscopic columns within islands of nontreated skin, thereby maximizing clinical efficacy and improving the recovery time and side-effect profile of earlier pulsed laser skin resurfacing techniques.7
Several factors determine the outcome of scar treatment with lasers, notably the type, color, and anatomical location of the scar. Scars are broadly classified as atrophic, flat, hypertrophic, or keloidal. The degree of induration and underlying fibrosis varies, and colors can range from red, purple, and pink to white and brown hues. The scar type and color dictate the appropriate treatment modality, with resurfacing lasers targeting textural abnormalities and PDL systems addressing keloidal, hypertrophic, and erythematous scars. Scars located on the anterior chest, scapula, and mandible are notoriously difficult to treat due to their propensity for further fibrosis, as are patients with Fitzpatrick skin phototypes (SPT) IV through VI because of their susceptibility to dyspigmentation after laser treatment. Other important variables in laser scar revision include operator experience, realistic patient expectations, and compliance with pre- and postoperative care.
Background: Basic Science of Procedure
Cutaneous injury causing interruption of the epidermis, dermis, and/or subcutaneous tissue initiates a cascade of events to repair the wound. The three stages of wound repair are inflammation, proliferation (neoangiogenesis, granulation, reepithelialization), and remodeling or maturation.8,9 The remodeling phase can last up to a year after initial injury and includes continuous synthesis, degradation, and reorientation of collagen fibers to develop the mature scar. Early wounds are composed of ~ 80% type III collagen and 20% type I collagen, whereas mature scars transition to ~ 80% type I collagen and only 20% type III collagen (similar to unwounded skin).8,9 Both hypertrophic scars and keloids are results of abnormal fibroproliferative wound repair during the remodeling phase.10 One important time-dependent cytokine that stimulates fibroblast proliferation and differentiation is fibroblast growth factor (FGF). FGF is upregulated early in the initial injury and quickly decreases to baseline. If it does not decrease, excessive proliferation and collagen production rates may lead to hypertrophic scarring or keloid formation.
There are several mechanisms by which the PDL treats hypertrophic scars and keloids. Kuo et al provide evidence that the 585 nm PDL alters signaling pathways involved with keloid formation by suppressing AP-1 transcription and transforming growth factor (TGF)-β1 expression via the mitogen-activated protein kinase (MAPK) pathway, thus reducing the proliferation of fibroblasts and type III collagen deposition.11–13 This induces keloid regression via fibroblast apoptosis during the remodeling phase of wound healing. The heat produced by the PDL may also result in collagenase release and the breakage of disulfide bonds, which initiates remodeling of collagen fibers.6 By targeting hemoglobin, the PDL causes photothermolysis of the vasculature, leading to local hypoxia and decreased cell function. It has also been shown that mast cells are increased in scar tissue after PDL irradiation, which may account for significant scar remodeling attributed to the effect of histamine and interleukins on fibroblasts that could affect collagen metabolism.5
Early pulsed ablative CO2 erbium lasers yielded impressive improvements in scars not only because of controlled tissue vaporization but because of the presence of residual thermal damage (RTD) that resulted from light penetration of 20 to 30 µm to ~ 100 to 150 µm into the dermis and by stimulation of collagen contracture, remodeling, and skin tightening.14–17 Newer fractional laser technology delivers laser energy to regularly spaced microthermal zones (MTZs), or columns of skin, with intervening areas of nontreated skin, which initiates the cascade of collagen remodeling while leaving an adequate reservoir of healthy keratinocytes for rapid wound healing.7 This technology allows delivery of ablative or nonablative wavelengths deep into the dermis (up to 1.5 mm) but maintains a more desirable safety profile by reducing the overall density (or percentage of tissue) treated.
Pertinent Anatomy
The skin is composed of the superficial epidermis; the dermal–epidermal junction, which anchors the epidermis to the deeper dermis; and the underlying subcutaneous (subdermal) fat. The epidermis consists of keratinocytes, melanocytes, and Langerhans cells, whereas the thicker dermis (~ 1 to 2 mm) is composed of mucopolysaccharides, collagen, elastin, and vasculature within a fibrous matrix. The other main components of the dermis are macrophages, fibroblasts, and dermal dendritic cells, which are responsible for inflammation and healing after disruption of the dermis or subcutaneous fat.
The interaction of lasers with tissue is explained by the theory of selective photothermolysis.1 At a given wavelength, the energy is absorbed by a specific target, or chromophore, in the skin. The pulse duration (time over which the energy is delivered) must be long enough to adequately heat the target but short enough to prevent nonselective heating of surrounding structures. Three cutaneous chromophores govern these interactions—hemoglobin, water, and melanin.
Hemoglobin in the dermal blood vessels strongly absorbs 585, 595, and 1,064 nm wavelengths. The PDL reaches these dermal blood vessels adequately, and the longer-wavelength 1,064 nm Nd:YAG penetrates more deeply to reach larger vessels. Reduction in scar vasculature may reduce erythema, but PDL effects on dermal fibroblasts are likely more important for the treatment of scars than chromophore-specific vascular effects.11–13 Laser resurfacing of textural abnormalities relies on absorption of laser energy by the chromophore water.14–20 At laser wavelengths longer than 1,300 nm, there is strong absorption by water-containing tissue. Ablative wavelengths, such as the 2,940 nm erbium or the 10,600 nm CO2 laser, vaporize skin, whereas nonablative wavelengths, such as the 1,550 nm erbium-doped laser fiber, heat the skin without vaporizing the epidermis.7,21–23 Both ablative and nonablative lasers induce collagen remodeling to smooth the skin texture. Melanin is located in the basal layer of the epidermis and also in dermal melanophages or traumatic foreign bodies (e.g., gravel, gunpowder) that can be introduced into a scar during trauma. Quality-switched (Q-switched or QS) lasers that deliver short pulses of energy in the nanosecond range are most effective for the destruction of pigment at 694, 755, and 1,064 nm wavelengths.24
Patient Selection
Before laser treatment of scars, patients must have a complete skin examination as well as a full discussion of the range of laser techniques available. The ultimate treatment recommendation should be based on achieving the best clinical outcome with the lowest possible risk. It is also important to uncover personality traits and lifestyle characteristics that would influence the patient′s candidacy for more aggressive procedures. Patients should be questioned about their activities of daily living, including work, child-care, and home responsibilities that could impact or interfere with the healing process. Those who cannot tolerate or schedule for a significant recovery period are better suited for nonablative laser treatments, even if clinical efficacy is somewhat compromised.
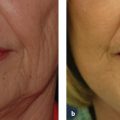
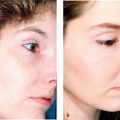
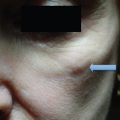
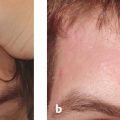
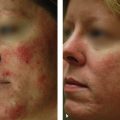
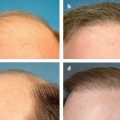
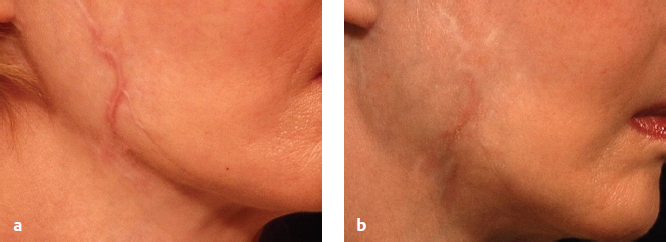
Careful assessment of Fitzpatrick SPT, anatomical location, and scar type is essential. Those with SPT IV through VI and scars on more sensitive locations (e.g., chest, scapula, mandible) are at higher risk of complication due to slower wound healing in these areas.24,25 Finally, classification of scar type will ultimately dictate choice of laser modality. Patients with hypertrophic scars or keloids have scars that are red, thick, and firm. Hypertrophic scars remain confined to the area of original injury and may slowly improve over time, whereas keloids extend beyond the border of the lesion, causing distortion of the original wound. Histologically, keloids are characterized by a unique pattern of haphazard, thickened, hyalinized collagen bundles arranged in whorls. This pattern is attributed to an inherited alteration in fibroblast response to stimuli and continued production of excessive collagen. Collagen fibers in hypertrophic scars are arranged parallel to the long axis of the inciting wounds.10 The vascular-specific PDL remains the first-line laser for treatment of hypertrophic scars and keloids.26–28 Several studies have shown remarkable improvements in scar color, height, pliability, texture, and symptomatology after one to several treatments using low energy densities and short pulse durations ( Fig. 14.1 ).2–6,29,30
Atrophic scars appear as indentations in the skin, wrinkled depressions resembling “cigarette paper,” or bulges where the subcutaneous fat herniates through the thinned dermis. These scars are the result of inadequate collagen replacement during the remodeling phase of wound healing. The goal of treatment for atrophic surgical and acne scars is to soften the scar borders and blend the texture with the surrounding skin. Acne scars are commonly atrophic and are best classified, according to the system described by Jacob et al,31 into three types: rolling, boxcar, and icepick. Rolling scars are wide undulating depressions with sloping borders where the depression is often associated with deep fibrous tethering. Boxcar scars have sharply marginated borders with marked “step-offs,” and icepick scars are narrow, tapered pits 1 to 2 mm in diameter. Deep boxcar and icepick scars are likely to require surgical revision in addition to laser resurfacing. The 10,600 nm CO2 and 2,940 nm erbium:yttrium-aluminum-garnet (Er:YAG) lasers allow precise, controlled vaporization of superficial tissue and a deeper zone of RTD to stimulate neocollagenesis, thereby filling depressions and softening irregular scar borders.14–20 Fractional devices, with their improved safety profile over pulsed ablative lasers, are currently the most popular systems used for resurfacing atrophic traumatic, surgical, or acne scars Video 14.1.21–23,32–40 An overview of laser resurfacing and fractional devices is presented in Tables 14.1 and 14.2 .
Prescar is a term used to describe early erythematous wounds in scar-prone skin. During the active healing phase, mild textural change is often present. These prescars have the potential to heal poorly and should be considered for intervention with early laser therapy.28,29 The 585 nm PDL can be used to treat early scars (prescars) within the first few weeks after wounding. This system is also the treatment of choice for surgical sites, traumatic wounds, or ulcerations to improve the quality of scarring and to prevent excessive scar formation.41–46 Studies confirm that scars treated early will ultimately heal more favorably than if left untreated.29,41–43,45,47 New fractional laser systems may also be successful at preventing unfavorable scar formation in surgical patients starting on the day of suture removal.48 Intraoperative vaporization of wound edges with either a CO2 or an Er:YAG laser, before primary surgical closure, has also been reported to enhance cosmesis.49
Technical Aspects of Procedure
Pulsed Dye Laser
PDL is the treatment of choice for hypertrophic scars and keloids, as well as prescars and erythematous shallow boxcar-type acne scars. The 585 nm PDL is slightly superior to the 595 nm PDL for this purpose.42 Although there appears to be no difference between the 0.45 and 1.5 millisecond pulse durations,43 it is essential to use short pulse durations, low fluences, and longer treatment intervals (every 6 to 8 weeks) to avoid scar worsening or aggravation of the scar.26
Scar revision with the PDL is typically performed in an outpatient setting without anesthesia. If topical anesthesia is desired, a lidocaine-containing cream or gel can be applied to the areas to be treated 15 to 30 minutes before laser irradiation. The skin should be cleansed with soap and water to remove makeup, powder, or creams that could potentially interfere with laser penetration. Flammable solutions, such as alcohol, should be avoided, and skin must dry thoroughly before the procedure is initiated. Wet gauze may be used to protect hair-bearing areas during treatment and to protect nontargeted skin. All individuals present in the treatment room must wear protective eyewear capable of filtering the appropriate wavelength to avoid retinal damage.
The entire surface of the scar should be treated with adjacent, nonoverlapping laser pulses. The fluences chosen are determined by the skin phototype of the patient, the type of scar, and previous treatments applied to the area. In general, hypertrophic scars and keloids are treated with low-energy densities ranging from 6.0 to 7.5 J/cm2 with a spot size of 5 or 7 mm and 4.0 to 5.5 J/cm2 with a spot size of 10 mm.26 Pulse durations ranging from 0.45 to 1.5 milliseconds are most effective.43 Energy densities should be lowered by at least 0.5 J/cm2 or more in patients with darker skin and for scars in more delicate or thin body locations (such as the chest or neck).24,26 It is important to start treatments at the lowest effective energy and only increase when it appears that the outcome of previous treatments is suboptimal. Any concern regarding patient response to treatment should prompt a test spot or patch in a small area before irradiation of the entire lesion. If postoperative oozing, crusting, or vesiculation is observed, the fluence used on subsequent visits must be decreased and retreatment postponed until the skin has completely healed.
Adjunctive use of intralesional corticosteroids, 5-fluorouracil (5-FU) or surgical debulking should be considered for extremely thick (> 5 mm), nodular or rapidly proliferative scars. Use of adjunctive therapy should be considered early for large/aggressive scars because laser energy will not penetrate the lesion. Otherwise, PDL treatment alone has been shown to be sufficient.30 Intralesional injections of corticosteroids (20 to 40 mg/mL triamcinolone) are more easily delivered immediately after (rather than before) laser irradiation because the treated scar becomes edematous (making infiltration easier). An additional consideration is that when steroid injection is performed before laser irradiation, the skin blanches, rendering the skin a potentially less amenable target for vascular-specific irradiation.
Keloids often require more treatment sessions to achieve significant improvement, but some may prove unresponsive altogether. The CO2 laser has also been used to vaporize keloids, particularly on the earlobes and posterior neck, but scar recurrences are common.50
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree