13 Trigger Finger/Thumb Release
Abstract
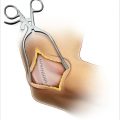
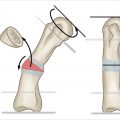
Release of the A1 pulley relieves the triggering phenomena and allows for improved range of motion of the digit in cases of limited and restricted flexor tendon excursion. This condition is also termed stenosing tenosynovitis or tendovaginitis. This procedure can, in most cases, relieve finger locking, catching, and allows for improved range of motion of the digit. The indication for this procedure is a triggering finger or thumb that is refractory to conservative treatment in the form of activity modification, anti-inflammatory medication, and corticosteroid injections.
13.1 Description
Technique for the surgical correction of triggering fingers and thumbs with release of the A1 pulley.
13.2 Key Principles
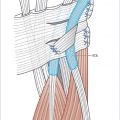
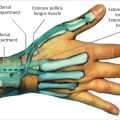
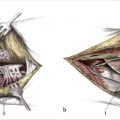
Identifying proper external and internal landmarks will keep this routine procedure consistent and avoid pitfalls.
13.3 Expectations
This procedure can, in most cases, relieve finger locking, catching, and allows for improved range of motion of the digit in cases of limited and restricted flexor tendon excursion. Some patients with triggering fingers may develop flexion contractures of the proximal interphalangeal (PIP) joint of the same digit. Such contractures will not directly correct with this procedure, but may have an opportunity to improve with postoperative stretching exercises once the restriction of the flexor tendon excursion has been relieved with surgery. For the more severe contractures, removal of one of the slips of the flexor digitorum superficialis (FDS) tendon can help improve the contracture at the PIP joint.
13.4 Indications
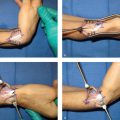
The most common indication for this procedure is the surgical correction of a triggering finger or thumb that is refractory to conservative treatment in the form of activity modification, anti-inflammatory medication, and corticosteroid injections (► Fig. 13.1). This exposure and technique can also be utilized for as part of other procedures that necessitate exposure of the proximal flexor sheath, such as:

Decompression of the proximal flexor sheath in cases of flexor sheath infection
Proximal pull-through testing of the flexor tendons in cases of flexor tenolysis or flexor tendon repair to confirm flexor tendon slide
Debridement or biopsy of the flexor tenosynovium
Distal release of the FDS tendon for tendon transfer
Release of flexor tendon entrapment in cases of complex/irreducible dorsal metacarpophalangeal (MP) joint dislocation
13.5 Contraindications
A1 pulley release in the face of ulnar drifting of fingers secondary to rheumatoid arthritis may exacerbate and worsen the progression of the ulnar drift deformity and volar subluxation at the MP joint. In such cases, resection of the ulnar slip of the FDS flexor tendon while maintaining the A1 pulley integrity may be a better choice.
13.6 Special Considerations
Digits that click and pop for reasons that are not related to catching of the flexor tendon at the A1 pulley will not be corrected with an A1 pulley trigger release. One must consider other common reasons for digital clicking and popping when selecting patients for this procedure. Other causes for digital clicking and popping can include instability of the extensor tendon over the dorsal MP joint due to rupture or instability of the sagittal bands. Additionally, instability or congenital laxity of the PIP joint volar plate can allow the PIP joint to assume a hyperextended position when the finger is extended and the PIP joint may then click as it initiates flexion from its hyperextended position.
Treatment of the thumb requires special consideration to the radial digital nerve, as it is often found directly in the middle of the incision or centrally over the flexor tendon. Similarly, the index and small fingers require a bit more attention as the trajectory of the flexor tendons, nerves, and arteries is more angled to these fingers as compared to the central long and ring fingers. Additionally, the small finger, especially in a small patient, may have a small A1 pulley, necessitating careful attention to landmarks and to the anticipated A1 pulley size so as to avoid an inadvertent A2 pulley release.
13.7 Special Instructions, Positioning, and Anesthesia
Patient participation can be helpful to confirm that there is no longer any flexor tendon catching or triggering with active digital motion. The procedure can be performed with local anesthesia alone or in combination with light sedation.
Lidocaine can be combined with Marcaine in a single syringe for an anesthetic solution that provides a quick acting and a longer lasting anesthetic effect. Alternatively, drawing an additional milliliter of bicarbonate solution into a 10 milliliter Lidocaine syringe makes the infiltration of the local anesthesia more comfortable for the patient.
A lead hand is helpful for trigger release of the fingers, but has no role for the treatment of a trigger thumb. Surgery for the thumb requires special positioning with a rolled towel behind the patient’s hand and an assistant holding the wrist in flexion so as to rotate the palmar aspect of the thumb toward the surgeon.
Considering the routine frequency of this short procedure, the efficiency of the surgery can be improved by eliminating the need for transfer of the patient to and from the standard operating room bed. The patient can be left on the transport gurney and the surgery performed with the patient’s upper extremity supported on a hand surgery table that can be rolled to the gurney edge or slid beneath the gurney pad.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree