Abstract
Flap reconstruction of surgical defects of the face offers unsurpassed aesthetic and functional outcomes. The V-Y flap is a modification of the traditional advancement that improves the flap’s vascular support and results. Island pedicle flaps are axial-pattern flaps that rely upon identified vessels for vascular support. Both are aesthetic and reproducible flaps, and the applications and surgical technique of each are detailed.
Keywords
flap, facial flap, V-Y flap, island pedicle flap
Many variables must be considered when examining a surgical defect and considering reconstructive options. The effective restoration of soft tissue contours improves results by reducing the visual impact of the reconstructive scars. Closure options for soft tissue defects include primary closure (side-to-side repair), split- or full-thickness skin grafts, and local or distant skin flaps. For smaller and less complex defects in areas with adequate regional tissue laxity, primary closure may often be a suitable repair choice. To achieve good cosmetic results with primary closure, the surgeon must recognize the limitations of adjacent tissue reservoirs. The mobility of nearby facial structures and their tolerance for movement must be determined prior to initiating the surgical repair. When the defect is too large to rely on local tissue laxity to close the wound in a side-by-side fashion, a skin graft or flap may be considered. Both full- and split-thickness skin grafts may be used to repair cutaneous wounds in a wide variety of locations; the uses of skin grafts are discussed elsewhere in this text. Although skin grafts may sometimes provide excellent final cosmetic results, they suffer from several limitations. To achieve excellence in cutaneous reconstruction, the surgeon must replace the missing tissue with tissue of identical or nearly identical character. When compared with the recipient site skin, the donor site skin should have a similar amount of sun damage, sebaceous glands, terminal hair, etc. Because skin grafts are usually harvested from sites not adjacent to the surgical defect, the harvested skin’s character is often unlike that of the missing skin. Moreover, to ensure the survival of a full-thickness skin graft, all of the subcutaneous fat and portions of the dermis must be removed from the graft prior to its placement. The graft, therefore, may lack sufficient volume to adequately fill the surgical wound or avoid the forces of postoperative wound contraction. For these reasons, flap repairs may be better suited for many wounds.
The flap repair of soft tissue defects is unsurpassed in its ability to provide functional preservation, contour restoration, and overall cosmetically appropriate reconstruction. A cutaneous flap is defined as a mobile attached unit of skin and soft tissue with its associated blood supply. Flaps are used extensively to repair a wide variety of soft tissue defects following skin cancer surgery in all anatomic locations. Flaps are widely used because they can often overcome many of the pitfalls seen with alternative repair options. Cutaneous flap surgery is safe and reproducible. Although cutaneous flaps may yield excellent results, they are not without the potential for some surgical risks and operative complications. It is important that the cutaneous surgeon have a firm knowledge of relevant anatomy, flap physiology, and flap design to maximize the opportunity for success. The nuances of proper surgical technique prove to influence operative outcomes significantly. Care must be extended to flap choice, flap design, incision and flap harvesting, and suture technique.
Cutaneous flaps are typically classified based on one of two systems: either the type of principal movement (rotation, transposition, advancement, or interpolation) or blood supply (random or axial patterned). Because the majority of flaps performed by dermatologists are random-pattern cutaneous flaps, skin flaps are more commonly classified on the basis of movement. Random-pattern flaps of varied design are supplied by the richly anastomotic dermal vasculature; they lack the axial-pattern flaps’ larger-caliber, named vessels in their bases. When these flaps are properly designed and executed, the abundant vascular supply of the dermis affords random-patterned flaps optimal chances for survival.
Advancement flaps are technically straightforward flaps; they are important in cutaneous reconstruction. The classical advancement flap is a sliding flap formed by a U -shaped incision. While this flap design has some reconstructive utility, it is prone to distal flap necrosis if the length is excessive or the flap is inset under excessive closure tensions. There are several modifications of the classical advancement flap that have expanded the flap’s utility. These include, among others, the O-T, A-T, Burow advancement, and V-Y flaps. All of these rely on the linear advancement of adjacent skin and soft tissue to allow surgical repair.
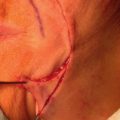
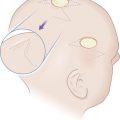
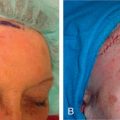
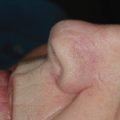
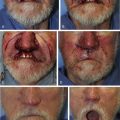
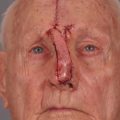
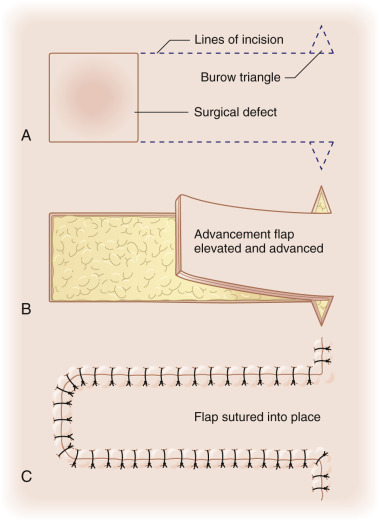
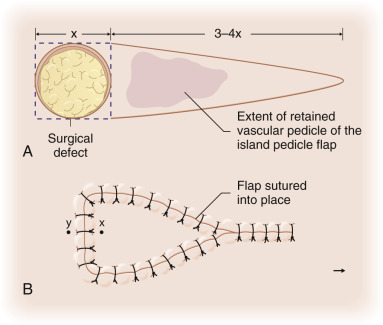
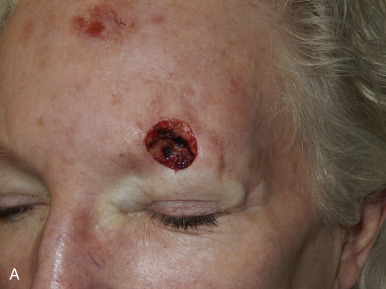
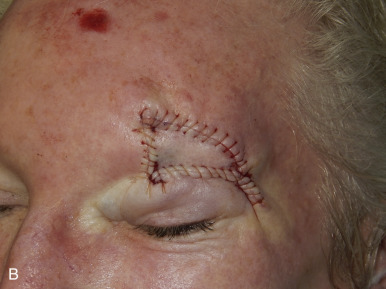
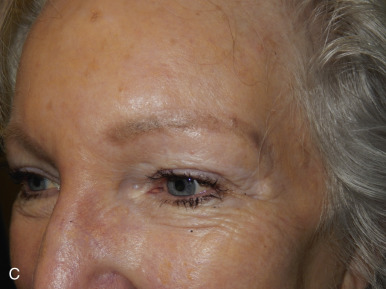
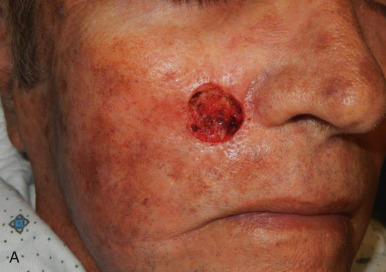
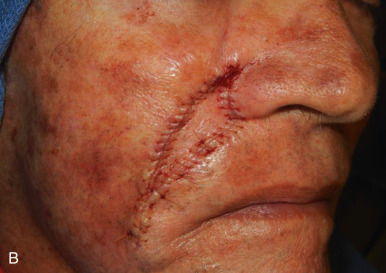
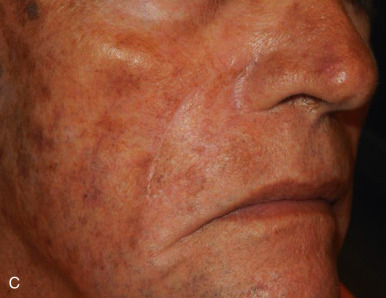
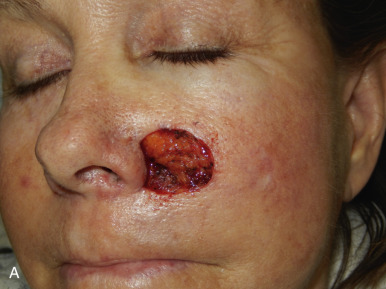
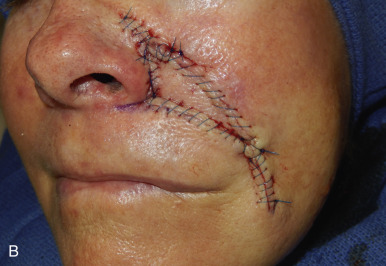
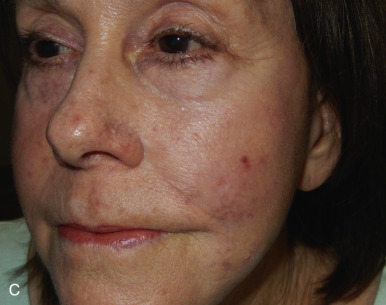
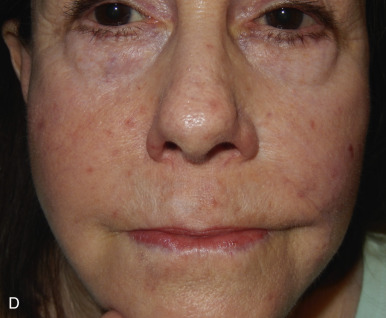
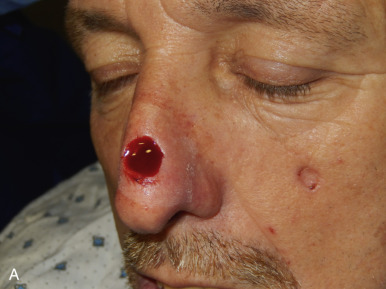
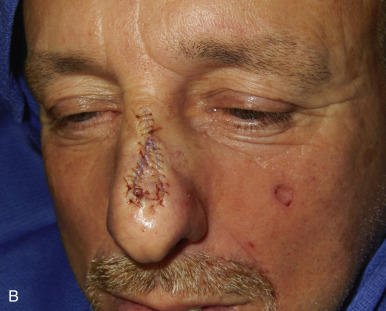
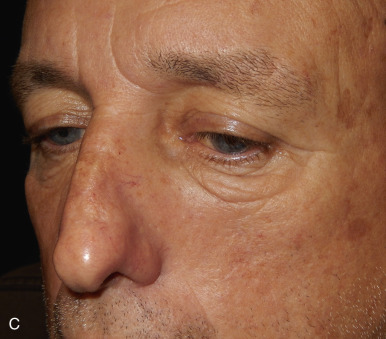
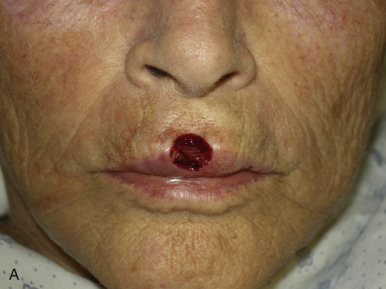
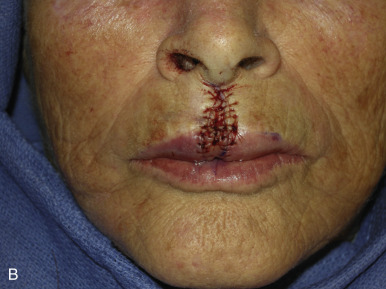
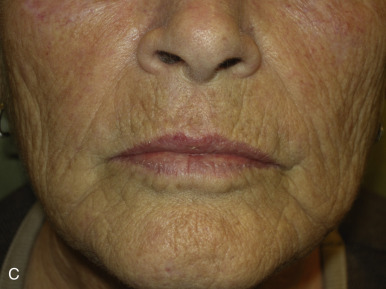
The V-Y advancement flap is a random-pattern cutaneous flap that is useful in repairing small- to medium-sized facial wounds. The classical advancement flap recruits contiguous tissue to repair an adjacent defect by creating a flap elevated to its base after two parallel incisions are made ( Fig. 6.1 ). The traditional advancement flap, in this regard, is limited by the mechanics of the flap’s design. With the simple advancement flap, a length:width ratio of less than 3 : 1 must usually be maintained to ensure perfusion of the distal portion of the elevated flap. The highest-tension portion of the flap is most distal to the flap’s vascular input. Advancement flaps designed with length:width ratios exceeding 3 : 1 or flaps inserted under significantly elevated wound closure tensions may be subject to an inordinately high risk of distal ischemic necrosis. The V-Y flap has surmounted this pitfall, which has sometimes limited the usefulness and success of the classical advancement flap. The V-Y flap is designed with the nutrient vascular pedicle closer to the flap’s leading edge so as to provide a greater and more predictable vascular supply ( Fig. 6.2 ). The preserved central vascular pedicle significantly improves the perfusion of the flap’s anterior margin and eliminates the relative ischemia at the leading edge of the longer traditional advancement flap. Because it has an abundantly perfused central pedicle, the flap can tolerate longer incisions and greater closure tensions than the classical advancement flap. The careful identification and preservation of a nutrient vascular pedicle in the V-Y flap is therefore critical for the success of the flap. The classic design of the V-Y flap is best used to repair defects where the long incisions may be camouflaged (e.g., upper cutaneous lip, cheek near anatomic borders, and brow) ( Figs. 6.3–6.5 ). The flap may also be used to effectively repair defects of the nasal dorsum, nasal ala, forehead, and nonfacial locations. In the classic design of the V-Y flap, the preserved nutrient vascular pedicle is directly underneath the central portion of the mobile flap. Variations of the flap with the vascular pedicle relocated to a lateral margin, a de-epithelialized distal flap, and a flap with bilevel muscular pedicles have been described previously ( Fig. 6.6 ). At times, opposing V-Y flaps may be used ( Figs. 6.7 and 6.8 ). However, in the author’s opinion, none of these modifications can surpass the predictably reproducible results seen with the classic design of the flap with a central vascular pedicle.
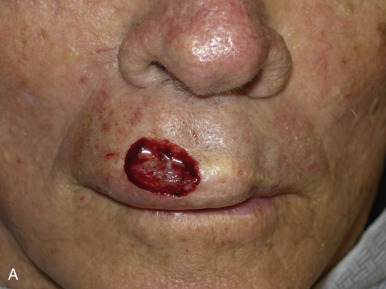
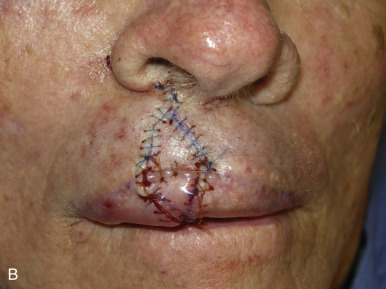
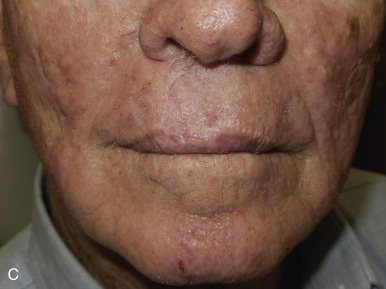
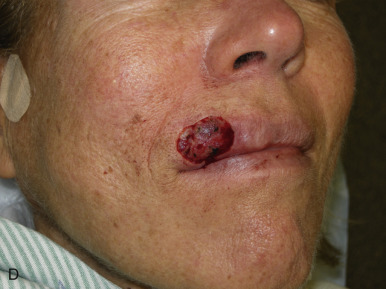
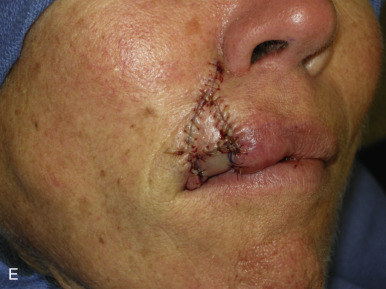
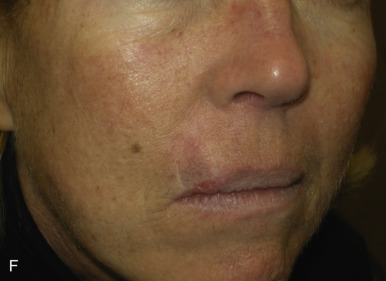
The V-Y advancement flap has been commonly referred to (and billed) as an island pedicle flap. Centers for Medicare and Medicaid Services (CMS) has recently redefined and restricted the use of the term island pedicle flap to those flaps requiring identification and dissection of an anatomically named axial vessel. Since the majority of the flaps used in dermatologic surgery are local flaps not based on named vessels, they should be referred to and billed as V-Y advancement flaps.
Technique
The proper design and execution of the V-Y flap is obviously critical to achieving reproducible aesthetic results with minimal operative risk. Once a defect has been selected for repair with a V-Y flap, operative consent is obtained from the patient. Routine prepping, draping, and infiltration with a local anesthetic then follow. The flap is designed as a V-Y tissue advancement. Although usually depicted as an isosceles triangle with straight edges, the flap’s long axes may be curved so as to place the resultant incision lines along the borders of the facial cosmetic units (e.g., curvilinear incisions in the melo-labial fold and along the vermilion border for a flap used in upper lip reconstruction). The flap may also be designed with the initial lines coming off the defect running straight for a short distance before tapering into the V shape. This displaces the area of tension farther away from the defect and may be useful in areas where there is no tissue laxity in the immediate area of the defect.
The flap has a robust central vascular pedicle that consists of dermis, subcutaneous tissue, and underlying facial musculature. This pedicle nourishes the flap with a predictable vascular support available in few other random-pattern cutaneous flaps. Although categorically a random-pattern cutaneous flap, the V-Y flap has a more abundant and predictable blood supply than that of many other alternative flap reconstructive options. This improved vascular support may be beneficial in patients with increased risks of tissue ischemia (smokers, patients with prior exposure to radiation therapy, etc.). Moreover, the limited amount of required undermining and tissue mobilization associated with the execution of the V-Y flap may make this flap an excellent choice in patients taking anticoagulants or those with bleeding diatheses. As compared with a rotation or advancement flap used to repair similarly sized defects, the V-Y flap typically requires less undermining, which may lead to a lower risk of postoperative bleeding complications.
Following adequate tumor extirpation, the defect to be repaired with the island pedicle flap is thoroughly analyzed. The flap produces the best results when it is harvested from within the same cosmetic unit as the surgical wound. This, however, is not an absolute requirement for flap success. The flap is classically designed as an isosceles triangle adjacent to the primary defect. The length of the triangle is typically 3 to 4 times the width of the surgical defect. The apex of the triangle’s long sides is an angle of approximately 30 degrees. After the flap is designed, if the wound has resulted from a Mohs extirpation, the circular surgical defect is converted to a square and the beveled dermis removed. It is the opinion of the author that a squared-off island flap inserted into a squared-off surgical defect has less chance of elevation (trap-dooring) and resultant failure of contour restoration than a rounded flap placed into a rounded defect. The phenomenon of trap-dooring is poorly understood. As a flap contracts in the postoperative period, circumferential movement of incipient scar tissue may force the flap to become elevated above the surrounding skin. Although this elevation may prove aesthetically displeasing, it can usually be corrected with massage, intralesional corticosteroids, and simple observation, thereby avoiding the need for additional operative procedures. Despite previously published recommendations to oversize the flap, the best surgical results are obtained when the flap is slightly undersized. For that reason the width of the properly designed V-Y flap should be slightly smaller than the width of the primary surgical defect. Although this minimal undersizing requires some degree of secondary tissue movement from around the borders of the primary surgical defect, it reduces the risk of postoperative flap protuberance. Oversizing or equivalent sizing the V-Y flap to the defect simply stuffs too much flap into the surgical defect, and the flap, when cicatricial forces begin to contract, decompresses anteriorly, producing an unsightly, redundant flap that will detract from the typical aesthetic success seen with the smaller flap’s design.
After the flap has been designed with attention to anatomic boundaries and flap geometry, the flap is sharply incised. The margins of the flap’s donor area are then undermined to facilitate flap advancement and donor-site closure. It is important to recognize the degree of secondary tissue movement that will be required in all cases in order to avoid unwanted anatomic distortion. The primary defect’s peripheral margins are also undermined at an identical depth. Undermining the pedicle of the V-Y flap itself presents the most risky portion of the reconstruction. If undermining is inadequate, the flap will prove difficult to mobilize and thus excessive tensions may be required for closure. These inappropriately elevated tensions increase the risk of flap ischemia and may produce associated anatomic distortion. Conversely, if the flap is undermined without careful attention to the preservation of the central vascular pedicle, insufficient vascular supply may fail to nourish the nascent flap. Although facial flaps may have a greater and more predictable vascularity than similarly designed flaps in other locations, the V-Y flap may be used in nonfacial reconstruction with identical design. A central pedicle of 40% to 50% of the flap’s area is typically adequate to ensure the flap’s survival. A significant restriction to the linear advancement of the flap may originate at the narrow apex (tail) of the flap. The apex of the flap may be incised and elevated to increase the forward sliding motion of the flap. This undermining and elevation of the flap’s tail greatly improve the flap’s mobility, but it should be limited to the exact extent necessary to advance the flap. Increasing the extent of undermining reduces the size of the nutrient vascular pedicle and therefore increases the risk of ischemic flap necrosis. The advancing margin of the flap is also undermined for several millimeters, principally to assist with accurate reapproximation of the wound edges. This small amount of undermining also significantly improves flap movement, particularly when the tail of the flap has also been liberated from its underlying attachments.
After undermining of the recipient site, the donor site, and the anterior and posterior margins of the flap, the flap and surrounding skin are elevated and hemostasis is achieved. After the achievement of adequate hemostasis, the flap is advanced in a V-Y manner to fill the surgical defect. The initial suture (the key stitch) is placed at the midpoint of the flap’s anterior margin to a corresponding point along the opposite margin of the primary surgical defect. This suture is placed with particular care to make sure that the flap is carefully aligned and thus to minimize the risk of subsequent anatomic distortion. Suture technique is critical to achieve operative success. To compensate for the inevitable wound contraction seen in the postoperative period, the flap must be sutured into place with care. Buried vertical mattress sutures of absorbable material are placed in the mid-dermis. If placed correctly, each successively placed buried suture will lower the central portion of the slightly undersized island pedicle flap. Once the buried sutures have been placed, the center of the flap should be depressed 2 to 3 mm below the surrounding skin. This slight flap recession is important to provide a well-contoured flap after wound healing has been completed, since the flap will inevitably rise to a small extent as wound contraction occurs at the flap’s bed in the early postoperative period. The author has never observed a recessed flap that failed to eventually elevate to a proper position.
After the flap has been secured with properly placed buried sutures, the epidermis is reapproximated with a running cuticular suture. Drains are rarely used, even with larger flap procedures. Tip stitches at the apex of the flap are not typically required. The wound is bandaged and wound care instructions are given to the patient. Oral antibiotics may be prescribed as needed. The sutures are removed at an appropriate postoperative interval, typically at 5 to 7 days for facial flaps. The V-Y flap repair rarely needs any postoperative refinement such as scar revision, debulking, or dermabrasion.
The classically designed V-Y flap is a hearty flap that may be used to repair a wide variety of facial defects with elegance and minimal procedural morbidity. The flap repairs wounds with skin of excellent color and textural match. The advancement V-Y flap should be viewed as an ideal reconstructive choice for soft tissue defects of the cutaneous lip, eyebrow, and medial cheek. Although previous authors have championed the flap as a viable reconstruction choice for distal nasal defects, the flap may prove problematic on the lower nose if the mobility of the nasal skin is limited or misjudged. In such a case, prominent nasal distortion may result after inadequate flap advancement because a reliance on secondary tissue movement to close the primary surgical defect is required. For small- to medium-sized distal nasal wounds, alternative reconstructive choices (the bilobed and other flaps) may prove to be superior selections.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree