1. Appropriate certification to perform general surgery
2. Training and experience in gastrointestinal surgery
3. Successful completion of a training course in bariatric surgery
4. Testimonials by mentors (proctors) of satisfactory bariatric surgical ability
5. Careful maintenance of a database of all bariatric cases, including outcomes
6. Commitment to postoperative life-time follow-up of the patients
7. Have performed at least 25 bariatric cases per year (50 cases are required when adjustable gastric banding is most commonly utilized)
8. Be able to perform revisional surgery
9. Attend bariatric meetings regularly and subscribe to at least one bariatric journal
10. Perform at least 25 bariatric cases per year including a number of revisional cases among them (50 cases are required when adjustable gastric banding is most commonly utilized)
11. Be involved in the training and the accreditation of less-experienced bariatric surgeons
12. Follow-up for at least 75 % of the operated patients
7.11 The European Accreditation Council
EAC-BS examines the institutional facilities and the surgeon’s qualifications and experience in order to ensure that they offer safe and efficient management to severely obese and patients with other metabolic disorders. EAC-BS utilizes the requirements set by IFSO [23] for surgeons [7] and institutions (Table 7.2) in order to accept them for participation in the COE program.
Table 7.2
Institution’s requirements
1. Ensure that surgeons performing bariatric surgery have the appropriate certification, training, and experience. |
2. Provide ancillary services such as specialized nursing care, dietary instruction, counseling, and psychological assistance if and when needed |
3. Have readily available consultants in cardiology, pulmonology, psychiatry, and rehabilitation with previous experience in treating bariatric surgery patients |
4. Have trained anesthesiologists with experience in treating bariatric surgery patients |
5. Ensure that a recovery room capable of providing critical care to morbidly obese patients and an intensive care unit with similar capacity are available |
6. Ensure that radiology department facilities can perform emergency chest x-rays with portable machinery, abdominal ultrasonography, and upper GI series |
7. Ensure that blood tests can be performed on a 24-h basis |
8. Ensure that blood bank facilities are available and blood transfusion can be carried out at any time |
9. Have comprehensive and full in-house consultative services required for the care of the bariatric surgical patients, including critical care services |
10. Have the complete line of necessary equipment, instruments, items of furniture, wheel chairs, operating room tables, beds, radiology facilities such as CT scan, lifts, and other facilities specially designed and suitable for morbidly and super obese patients |
11. Have a written informed consent process that informs each patient of the surgical procedure, the risk for complications and mortality rate, alternative treatments, the possibility of failure to lose weight and his/her right to refuse treatment |
12. Maintain details of the treatment and outcome of each patient in a digital database. |
13. Have experienced interventional radiologists available to take over the non-surgical management of possible anastomotic leaks and strictures |
14. Performs at least 50 bariatric surgical cases per year including revisional cases. The peri-operative care and the surgical procedures have to be standardized for each surgeon. |
15. Provides life-time follow-up for the majority and not less than 75 % of all bariatric surgical patients. Patients’ data should be available on request by EAC-BS authorities. |
The management offered to the patients by the participating institutions and surgeons (Table 7.1) is carefully observing patients’ outcome which is recorded in the International Bariatric Registry (IBARTM).
Indexes of excellence, such as intra- and post-operative complications, re-admissions, long-term complications, mortality, excess weight loss and co-morbidities outcome, are evaluated for each participating center.
Finally, a site visit by experienced auditor will follow to verify the reported patients’ data and examine the institutional equipment, facilities, resources and services. The auditor will construct a detailed report which is then forwarded to two Review Committee members for evaluation. Both reviewers will then submit their opinion to the Scientific Board, the final decision-making body. If everything is in order, EAC-BS will suggest to IFSO-EC that the center/surgeon is good enough to receive the COE designation (Table 7.3).
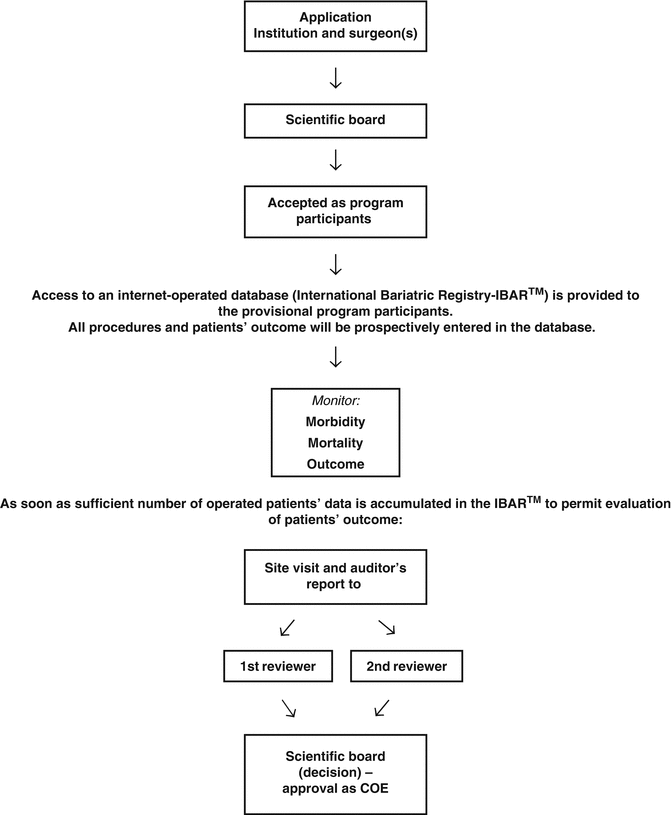
Table 7.3
COE evaluation procedure

7.12 Results of IFSO-EC Center of Excellence Program
The program is evolving in a very satisfactory way. Seventy-two institutions and 118 surgeons from 22 countries from the region of Europe, Middle East, and Africa are participating.
Since January 2010, data from more than 22,881 bariatric patients have been entered in the IBAR. In 84.4 % of them, the applied treatment was a primary bariatric procedure, in 5.9 % a two-stage procedure and in 9.7 % a re-do for failure of the original operation.
From the primary procedures, 55.18 % were gastric bypass, 24.68 % sleeve gastrectomy, 11.52 % band, 0.50 % gastric plication, 1.15 % mini gastric bypass, 0.86 % biliopancreatic diversion (Scopinaro), 2.05 % biliopancreatic diversion (duodenal switch), 0.02 % gastroplasty, and 4.04 % “other” bariatric procedure.
Early (≤30 days) post-operative mortality was as low as 0.07 % for all procedures including the re-operations. Mortality for primary procedures was 0.04 %, for 2-stage 0.30 % and for re-do procedures 0.14 %.
Re-admissions for complications in the early (≤30 days) post-operative period was 1.69 % among all operated patients with primary procedures, and for the late (≥30 days) post-operative period 2.26 %. For the 2-stage and the re-do procedures the incidence of re-admissions for early complications was 1.28 and 4.24 % and for late complications 2.22 and 3.42 %, respectively.
Weight-loss as assessed by % EWL and % EBL for patients subjected to primary bariatric procedures at 12th post-operative month was 68.81 and 70.83 %, respectively. At 24th post-operative month, it was 70.83 and 78.71 %, respectively. Cure or significant improvement of obesity co-morbidities were observed in 79.4 % for diabetes, 77.2 % for hypertension, 84.6 % for osteo-articular diseases, 93.6 % for sleep apnea syndrome, and 80.8 % for dyslipidemia.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








