Terminology and Classification of Genital Disorders
Peter J. Lynch
Two components are necessary in order to rationally organize genital dermatologic disorders: “terminology” (the definition of terms used in morphologic description of mucocutaneous lesions) and “classification” (the orderly arrangement of these diseases into specific groups, categories, or classes).
Terminology
The definitions included here represent our preferences and are very similar, though not necessarily identical, to those found in standard dermatology textbooks. The minor differences, where they occur, will not interfere with the use of the diagnostic classification that follows. Note specifically that where measurements are given within the definitions regarding the diameter of the lesions, these are not exact and overlap may occur between smaller and larger lesions.
Nouns (i.e., primary lesions)
Macule
A macule is a small (1.5 cm or less), nonelevated, nonpalpable area of color change. The surface of macules is usually smooth, though a small amount of powdery scale may be present.
Patch
A patch is a larger (greater than 1.5 cm), nonelevated, nonpalpable area of color change. It may be considered as a two-dimensional (length and width) increase in the size of a macule. Again, the surface is usually smooth but sometimes a small amount of powdery scale may be present.
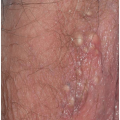
Papule
A papule is a small (1.5 cm or less) palpable lesion. Usually, but not always, a papule is visibly elevated above the surface of the surrounding tissue. A nonelevated, but palpable, lesion contained completely within the skin is still termed a papule. A papule may be considered as a one-dimensional (lesional thickness) increase in the size of a macule. Papules may be either smooth or rough surfaced. Roughness on the surface of a papule is due to the presence of either scale or crust.
Plaque
A plaque is a large (greater than 1.5 cm) flat-topped, palpable lesion. It may be considered as a two-dimensional (length and width) increase in the size of a papule. Plaques are usually, but not always, elevated above the surface of the surrounding tissue. As for papules, intracutaneous lesions that are palpable are termed plaques whether or not they are elevated. Likewise, plaques may be smooth or rough surfaced. Roughness on the surface of a plaque is due to the presence of either scale or crust.
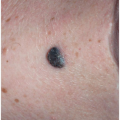
Nodule
A nodule is a large (greater than 1.5 cm) usually domeshaped, palpable lesion. It may be considered as a threedimensional (length, width, and depth) increase in the size of a papule. Nodules are often, but not always, smooth surfaced.
Vesicle
A vesicle is a small (1.0 cm or less) fluid-filled blister. Conceptually, it may be considered as a fluid-filled papule. Usually, the fluid is loculated. Fluid-filled papules in which the fluid is nonloculated are known as wheals. Wheals only occur in urticaria (hives) and urticarial plaques. Vesicles and wheals usually may be differentiated visually but also by the observation that when the surface of a blister is pierced, the fluid runs out and the blister collapses. When a wheal is pierced, a drop of fluid may appear on the surface but the papule remains as it was before the piercing. When the surface of a vesicle has been removed or has disintegrated, the shallow deficit that remains is defined as an erosion. The surface of this erosion may be red, moist, or covered with crust.
Pustule
A pustule is a vesicle that contains visibly purulent (pusfilled) loculated fluid. That is, the lesion appears opaquely white, yellow, or yellow-white. This color occurs as a result of the presence of neutrophils and other white blood cells. Note that a vesicle may turn cloudy as it ages. This change does not make it a pustule. To be a pustule, a blister must have been purulent from the time of its inception. When the surface of a pustule has been removed or has disintegrated, the shallow deficit that remains is defined as an erosion. The surface of this erosion may be red, moist, or covered with crust.
Bulla (Plural: Bullae)
A bulla is a large (greater than 1.0 cm) vesicle. Here, too, the fluid is loculated. Usually, the fluid is found in a single compartment occupying the whole of the lesion, but, uncommonly, coalescence of closely set vesicles occurs to form a multiloculated bulla. As bullae age, they may become cloudy (see Pustule above). When the surface of a bulla has been removed or has disintegrated, the shallow deficit that remains is defined as an erosion. The surface of this erosion may be red, moist, or covered with crust.
Erosion
An erosion is a shallow defect in the surface of the skin. In this context, “shallow” means that the epidermis is missing but that the defect does not extend more deeply into the dermal component of the skin. The base of an erosion may be red and moist or the base may be covered with crust. Any crust that is present is yellow in color. The crust is also crumbly and fairly easily removed. If the crust instead is red, blue or black in color, it usually means that the defect is deeper (see Ulcer below). Erosions occur as the result of two mechanisms. They can develop as a result of trauma, and this trauma is most often due to vigorous scratching. Erosions occurring as a result of trauma are usually linear or angular in configuration. Alternatively, erosions may be nontraumatic. Nontraumatic erosions most often occur when the roof of a vesicle or bulla is removed or has disintegrated. The configuration of nontraumatic erosions is usually round, and often there is a thin peripheral rim of scale. This type of scale is called collarette scale, and it occurs as a result of fragments of the peripheral blister roof that remain intact at the edge of a previous blister.
Fissure
A fissure is a subtype of a nontraumatic erosion in which a thin (less than 1 mm in width), linear crack occurs into or through the epithelium. A fissure appears clinically as a thin red line, and due to its narrowness, it may not be recognized as a true defect in the surface of the skin unless a magnifying lens is used. Fissures generally arise in the setting of an epithelial surface that is too dry. Fissures can be viewed as analogous to the cracked surface that often occurs in the bed of a dried-out pond or stream.
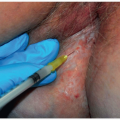
Ulcer
An ulcer is a deep defect in the surface of the skin. The defect is deeper than that of an erosion, and it extends into, or even through, the dermal connective tissue. These deeper defects involve significant blood vessel damage, and as a result, the base of an ulcer may contain crust that includes heme pigment as well as plasma proteins. For this reason, the crust may be red, blue, or black. When considerable fibrin is present as well, the color of the crust may be black and is very adherent to the base of the ulcer; such crust is known as eschar.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree