12Surgical Treatment of Lesser Occipital Migraine Headaches (Site VI)
Bahman Guyuron
Salient Points
• The lesser occipital trigger site is the most anatomically unpredictable site.
• A Doppler vascular signal can often be identified in the headache-onset site.
• A nerve block can only be reliable if the patient is experiencing headache at the time of office visit.
• A negative nerve block does not rule out the presence of a lesser occipital trigger site.
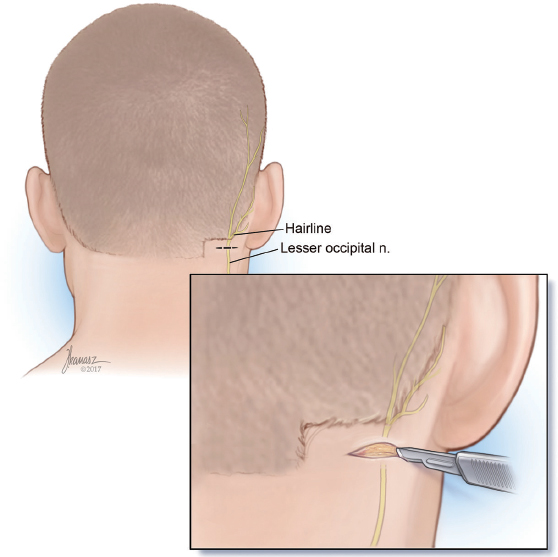
• This site is more caudal and lateral to the greater occipital trigger site and it is close to the lateral occipital hairline.
• The surgery is often done under local anesthesia unless some other sites are being decompressed at the same time, mandating the use of general anesthesia.
• A horizontal incision about 1.5-2 cm in length is used to find the nerve and the vessel.
• A fine (mosquito) hemostat is used to continue the dissection with a spreading technique.
• The vessel is dissected to an extent of 1 to 2 cm and cauterized or ligated and excised.
• A nerve decompression or neurectomy could be selected for deactivation of this trigger site.
• If a neurectomy is preferred, the nerve end is buried in the adjacent muscle to reduce the potential for a neuroma formation.
• The patient can return to work the same day or the next day if the dissection is not extensive.
12.1 Introduction
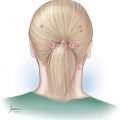
The lesser occipital trigger site is the most problematic of all the migraine sites when it comes to locating the nerve. This is due to the tremendous variation in the anatomy and presentation of the headache site as well as branching pattern of this nerve.1 Any headache lateral and caudal to the greater occipital nerve territory is likely to be related to the lesser occipital nerve. Commonly, a Doppler vascular signal can be identified at the trigger site. A positive nerve block could prove very informative only if the patient experiences a migraine headache (MH) at the time of the examination. However, when the pain is chronic in nature, the block may not result in cessation of the MH.
12.2 Surgical Technique
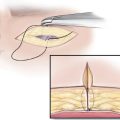
With the patient in a sitting position, the most tender spot is identified by the patient and is marked. Ultrasound Doppler vascular signal is searched for to confirm the presence of a vessel. Additionally, the headaches site is confirmed with the patient in a supine position and the head tilted to the side. These two sites in the sitting and supine positions may not always match. One may have to repeat the examination a few times before designing the incision.
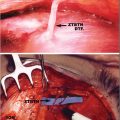
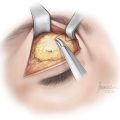
A horizontal incision about 1.5 to 2 cm in length is designed and about 1 cm of the surrounding hair is shaved on each side ofthe incision (► Fig. 12.1; see ► Video 12.1). The area is infiltrated with Xylocaine containing 1:100,000 epinephrine. If the patient is having MH at the time of surgery, the patient is queried about the level of the pain before and after the injection. While complete disappearance of the pain is often experienced, not having thorough elimination of the MH after injection of the local anesthesia is not prohibitive of surgery. The incision is made and taken down as deep as possible in the subcutaneous plane. A fine (mosquito) hemostat is used to continue the dissection with a spreading technique (►Fig. 12.2). Immediately below the trapezius fascia, the nerve, the vessel, or both are identified and a rubber band is placed around the nerve (►Fig. 12.3). The vessel is dissected to an extent of 1 to 2 cm and cauterized (►Fig. 12.4). If a compression site is identified, the fascia is released. However, in most instances, finding a distinct compression site is unlikely. If the exploration fails to detect a compression site, the nerve is isolated, dissected, and transected to a length of approximately 1.5 cm (►Fig. 12.5). A pocket is created in the adjacent trapezius muscle large enough to accommodate the nerve (►Figs. 12.6, 12.7). A 5-0 blue Prolene suture is passed through the muscle, retrieved through the created tunnel, then passed through the end of the nerve (►Fig. 12.8), brought back through the pocket and the muscle, and tied over the muscle (►Fig. 12.9). As the suture is tied, the nerve end is watched to be pulled into the muscle pocket (►Fig. 12.10). Minute amount of 0.1- to 0.2-mL Kenalog (40 mg/mL) is injected in the area around the nerve end. A 5-0 Monocryl suture is then passed through the deeper layers while catching the base of the dissected area and deeper portion of the subcutaneous tissues, and then through the superficial portion of the subcutaneous tissues and tied to eliminate the dead space (►Fig. 12.11). The superficial portion of the skin is repaired using a 5-0 plain catgut. The wound is covered with Bacitracin ointment.