Red Lesions: Patches and Plaques
Peter J. Lynch
Libby Edwards
Many different rashes present with red plaques and patches. Whereas these conditions on dry, keratinized skin usually exhibit differentiating features on clinical examination that indicate a diagnosis, damp skin folds such as the anogenital skin and axillae more often display nonspecific erythema with no or only subtle scale. Therefore, a history of itching and contactants, an examination of extragenital areas typically affected by some of these diseases, studies for infection, and biopsies are more often needed to sort through the possible diagnoses. Overlap among these conditions is common. For example, a patient who is prone to pruritus may experience itching with the inflammation of psoriasis, and the subsequent rubbing and scratching produce overlying lichen simplex chronicus (LSC). At times, a definitive diagnosis cannot be made; if infection and neoplasm are ruled out, presumptive therapy for an inflammatory dermatosis usually provides comfort, even without a specific diagnosis.
Several common skin diseases of the vulva present as red patches and plaques on anogenital skin. Although these diseases are often easily diagnosable when occurring on dry skin surfaces, these are frequently indistinguishable on genital skin and other damp skin folds. The usually characteristic appearance of individual skin diseases is modified by the environment in skin folds, so that diagnosis by morphology is challenging. Moisture and heat obscure scale. Lichenification (thickening from rubbing) can be white due to hydration. Normally well-demarcated borders of plaques may appear fuzzy. Also, genital skin, even more than dry, keratinized skin, often is affected by more than one disease process, so secondary infection and irritation from sweat, urine, feces, and overwashing can change the appearance of the skin. Finally, redness is difficult to detect when occurring in a patient with a naturally dark complexion; erythema is generally perceived as hyperpigmentation in this population.
Therefore, the correct diagnosis of red genital plaques and patches sometimes requires an evaluation of other skin surfaces for more typical morphology, a history of overwashing or use of common allergen containing products, wet mounts/cultures, and/or biopsies. Unfortunately, a skin biopsy of nonspecific erythema often yields a nonspecific result. However, red lesions that are not diagnosed clinically or do not respond to therapy as expected should be biopsied to rule out the occasional extramammary Paget disease (EMPD) or various forms of squamous cell carcinoma in situ, currently called differentiated intraepithelial neoplasia or high-grade squamous intraepithelial lesion (HSIL); previous names for these include intraepithelial neoplasia, squamous cell carcinoma in situ, bowenoid papulosis, Bowen disease, and erythroplasia of Queyrat.
Often, obtaining a firm diagnosis is not possible, and empiric corticosteroid therapy while monitoring or treating for likely infections is necessary, useful, and adequate.
SECTION A: ECZEMATOUS AND LICHENIFIED DISORDERS
Anogenital pruritus occurs in two settings. It may arise from apparently normal-appearing tissue (“primary” pruritus), or it may occur as a secondary part of a separate disease process occurring on visibly abnormal tissue (“secondary” pruritus). Primary pruritus can be further divided into two subcategories: (a) those instances where it is accompanied by visual signs of prolonged rubbing and scratching (atopic dermatitis and lichen simplex chronicus [LSC]) and (b) those instances where there is little or no rubbing and scratching (idiopathic or “essential” pruritus). The former two conditions are discussed in this chapter, whereas the latter is covered in Chapter 13.
Secondary pruritus occurs when a specific skin disorder is accompanied by pruritus, which may or may not result in the development of the “itch-scratch cycle.” Those conditions that usually present with an eczematous appearance (contact dermatitis and seborrheic dermatitis) are discussed in the first section of this chapter, whereas those disorders that less frequently develop an eczematous appearance secondary to pruritus (such as psoriasis, lichen sclerosus, and tinea cruris) are dealt with as individual disorders throughout the book.
Conceptually, it is worth trying to separate primary from secondary pruritus, but since scratching generally occurs in both settings, the clinical appearance at the time of examination often does not allow one to separate the two processes. When that is the case, treatment specifically directed toward the cessation of scratching and rubbing
will usually allow for correct identification. That is, when the scratching completely stops, the skin will return to its normal appearance if the process is primary or will reveal an underlying disorder if the process is secondary.
will usually allow for correct identification. That is, when the scratching completely stops, the skin will return to its normal appearance if the process is primary or will reveal an underlying disorder if the process is secondary.
That which follows in this paragraph is a short review of terminology for eczematous disorders, which has been covered elsewhere (see Chapter 2). When skin is scratched or rubbed on a continual basis over a period of days or weeks, the tissue takes on an appearance classical for the eczematous (dermatitic) diseases. For this reason, “eczematous” and “dermatitic” (which are synonyms) can be defined morphologically. The morphologic pattern for the eczematous diseases is represented by the presence of red papules and plaques with poorly marginated borders, overlying scale, and evidence of epithelial disruption and/or lichenification. Epithelial disruption is most often recognized by the presence of excoriations, but other signs of epithelial disruption can include weeping, crusting, fissuring, or the presence of yellow-colored scale. (This yellow color is due to the presence of small amounts of plasma that coats the otherwise gray, white, or silver color of scale.) When rubbing is more prominent than scratching, the callus-like response of lichenification may supplant much of the evidence for epithelial disruption. Lichenification is recognized clinically by three features: palpably thickened skin, exaggerated skin markings, and lichen-type scale. Note that lichen-type scale, because of its adherence to the epithelium, is more or less colorless when dry but whitens when it absorbs moisture as is likely to happen owing to retained sweat in the anogenital area.
Lesions possessing an eczematous clinical appearance, as described in the paragraph above, have a characteristic histologic appearance on biopsy. This microscopic appearance demonstrates spongiotic inflammation (inflammatory cells accompanied by intercellular and intracellular edema within the epithelium) when the process is acute and by acanthosis (epithelial thickening often termed “psoriasiform dermatitis”) when the process is chronic. This is the histologic appearance of all of the disorders discussed in Section A of this chapter. Since all of these diseases share a common histologic appearance, pathologists are usually unable to separately identify each of the disorders that exist within the general category of eczematous disease. For this reason, when a pathologist makes a diagnosis of “spongiotic dermatitis” or “psoriasiform dermatitis,” it is necessary for the clinician to make a clinical-pathologic correlation in order to arrive at a more specific diagnosis (1).
Atopic Dermatitis and Lichen Simplex Chronicus
Strictly speaking, atopic dermatitis and LSC are examples of primary pruritus in which the itching most often occurs in clinically normal-appearing tissue and is accompanied by vigorous scratching and rubbing. However, when the “itch-scratch cycle” is superimposed on a preexisting dermatologic disorder, it is common to use the term “secondary eczematization.”
The nomenclature regarding atopic dermatitis and its variants is somewhat complex and controversial. The term “atopy” has been defined in many ways, but most often, the definition includes a genetic predisposition for the development of hypersensitivity allergic IgE reactions to common environmental antigens. Thus, atopic individuals frequently develop allergic rhinitis (hay fever), asthma, and/or atopic dermatitis. A semantic problem arises when an eczematous eruption occurs in an individual who lacks a personal or prominent family history of hay fever or asthma. In this setting, the eczematous process has alternatively been called neurodermatitis, infantile eczema, childhood eczema, or LSC. Given the lack of consensus regarding the diagnostic criteria for atopic dermatitis (2) and in view of the fact that these eczematous eruptions share the presence of the “itch-scratch cycle,” I believe it is appropriate to use the term atopic dermatitis (for the multifocal form) and LSC (for the localized form) of the disease regardless of whether or not the individual has other clinical evidence of atopy. Moreover, since genital eczematous involvement very often occurs in the absence of eczematous disease elsewhere, it will generally be referred to as LSC for the purposes of this chapter.
Clinical Presentation
Atopic dermatitis in its multifocal form is an extremely common disorder affecting about 15% of the population in Western countries. The localized form of atopic dermatitis, anogenital LSC, occurs in both sexes and at all ages. It is most commonly encountered in those who are adults, and in this group, it is found in women a little more frequently than in men. In children, boys are affected somewhat more often than girls. The prevalence and incidence of anogenital LSC are not known with certainty, but in one of the more recent large studies, such patients accounted for 1.5% of all visits to a dermatology clinic (3). Based on a few older studies and discussion at conferences, it is probably the single most common symptomatic condition involving the anogenital area.
History
Possibly because of embarrassment, patients with genital LSC rarely seek medical attention until the problem has been present for weeks or months. Often, the itching arises subtly, but in women, a specific event, most often vaginal discharge (perceived to be a yeast infection), will be identified by the patient as the initial trigger. In either setting, once itching has occurred, scratching almost inevitably follows. Most patients describe the itching as severe and find that nothing in terms of home remedies or over-the-counter medications will relieve it. In the most intractable cases, patients will scratch until pain
caused by excoriation replaces the pruritus. In instances of long-standing duration, patients will often shift from scratching to rubbing since they find they can alleviate some of the itching without causing the pain and tissue damage that arises with excoriation.
caused by excoriation replaces the pruritus. In instances of long-standing duration, patients will often shift from scratching to rubbing since they find they can alleviate some of the itching without causing the pain and tissue damage that arises with excoriation.
In time, a vicious circle of itching followed by scratching, followed by more itching and more scratching, develops. This is termed the “itch-scratch cycle,” and its presence is, I believe, the pathognomonic and defining characteristic of atopic dermatitis and LSC. Sometimes, the patients are conscious of the scratching, and many such individuals continue on with the scratching “because I can’t make myself stop” or “because it feels so good to scratch.” Others are unaware of scratching and tend to think that they scratch very little. This is quite analogous to the personal unawareness that develops with fingernail biting, knuckle cracking, and other such “habit tics.”
Scratching during the daytime primarily occurs after using the toilet, when changing clothes after work, and in the evening when one gets undressed for bed. Scratching almost always also occurs episodically at night during the lighter stages of non-REM sleep, and it is associated with an abnormal increase in the number of partial awakenings (4,5). I have termed this nocturnal scratching the “Penelope phenomenon” based on Homer’s tale of Odysseus (Ulysses) and his wife Penelope (6). When Odysseus tarried for many years on his voyage home from the Trojan War, Penelope was urged to declare him deceased and marry one of her many suitors. She agreed to do so once she had completed weaving a funeral shroud for her dying father-in-law. During the day, she wove the shroud, but at night when everyone was sleeping, she would undo most of the previous day’s weaving. The Penelope phenomenon thus represents the nighttime scratching that undoes the benefits of a good daytime therapeutic program.
Examination
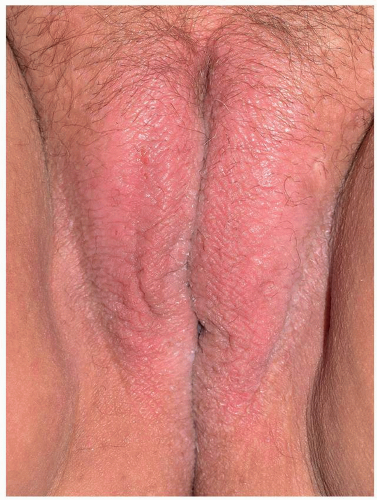
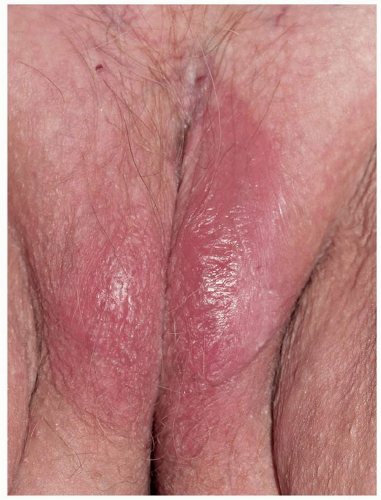
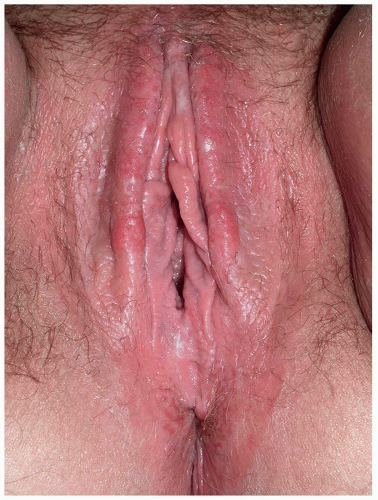
As indicated above, LSC shares the morphologic characteristics of all eczematous diseases. This includes erythematous, poorly marginated, scaling papules and plaques with evidence of epithelial disruption and/or lichenification (Figs. 6.1, 6.2, 6.3, 6.4 and 6.5). But in contrast to other eczematous diseases, the severity of excoriation and/or lichenification often allows for correct clinical identification. This may not be true in mild cases because the warm, moist environment of the anogenital area may obscure some of the characteristic morphologic features. First, scale may not be as visibly apparent (though it can still be recognized by roughness on palpation) as it is with LSC in other locations (Figs. 6.6 and 6.7). Second, scale is
hydrophilic and when it takes up water it whitens. This white color can be fairly prominent when a patient first undresses but decreases as evaporation reduces the moisture content (Fig. 6.8). Third, deep scratching may destroy or remove melanocytes, leaving hypopigmented areas when the scratch marks heal (Figs. 6.9 and 6.10). Fourth, the anogenital area pigments easily. When LSC has been
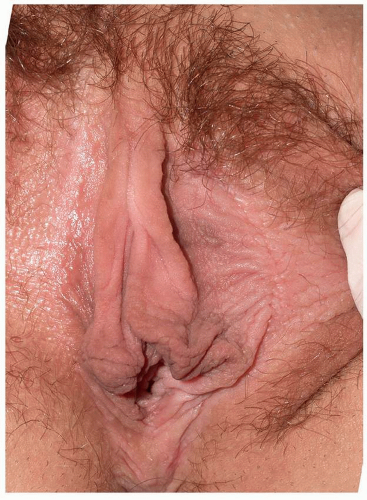
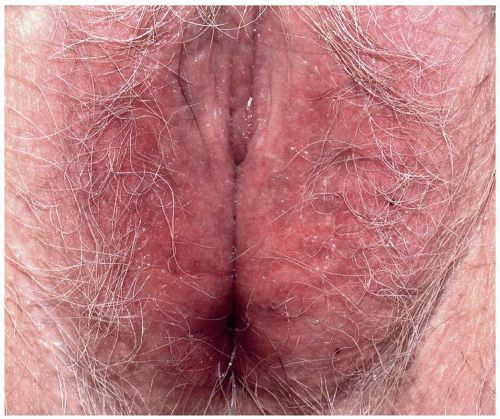
present for a long time, postinflammatory hyperpigmentation often develops. This can decrease the apparentness of erythema, leading one to underestimate the amount of inflammation that is present (Figs. 6.11 and 6.12). This is especially likely in patients with naturally dark skin. Genital LSC in women primarily occurs on the outer aspects of the labia majora though involvement of the labia minora is sometimes seen. In men, the scrotum is the predominant site of involvement, but the base or even the entire shaft of the penis is sometimes affected. Perianal LSC in common in both genders (Fig. 6.13).
hydrophilic and when it takes up water it whitens. This white color can be fairly prominent when a patient first undresses but decreases as evaporation reduces the moisture content (Fig. 6.8). Third, deep scratching may destroy or remove melanocytes, leaving hypopigmented areas when the scratch marks heal (Figs. 6.9 and 6.10). Fourth, the anogenital area pigments easily. When LSC has been
present for a long time, postinflammatory hyperpigmentation often develops. This can decrease the apparentness of erythema, leading one to underestimate the amount of inflammation that is present (Figs. 6.11 and 6.12). This is especially likely in patients with naturally dark skin. Genital LSC in women primarily occurs on the outer aspects of the labia majora though involvement of the labia minora is sometimes seen. In men, the scrotum is the predominant site of involvement, but the base or even the entire shaft of the penis is sometimes affected. Perianal LSC in common in both genders (Fig. 6.13).
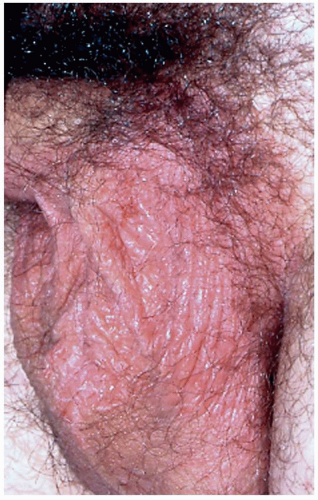
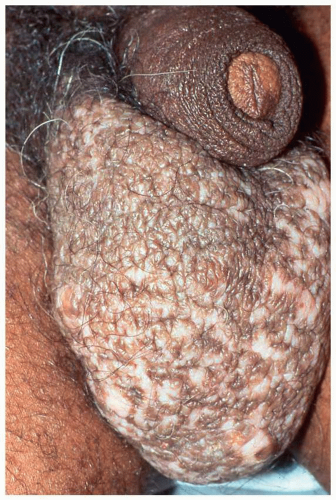
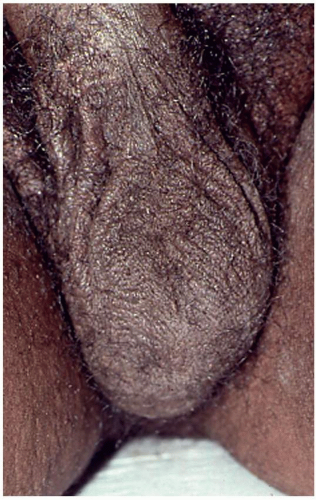
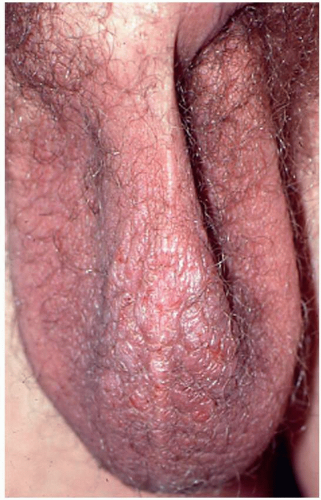 FIG. 6.2. Lichen simplex chronicus of the male genitalia is usually on the scrotum and again exhibits poorly demarcated thickened lichenification produced by chronic rubbing and scratching. |
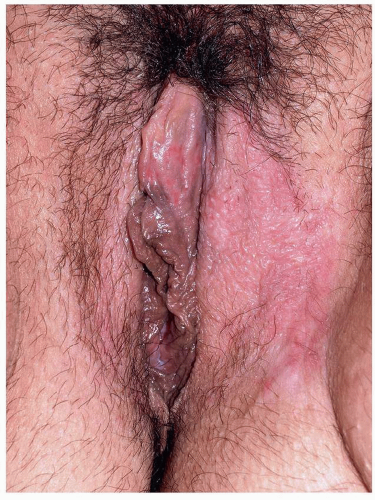
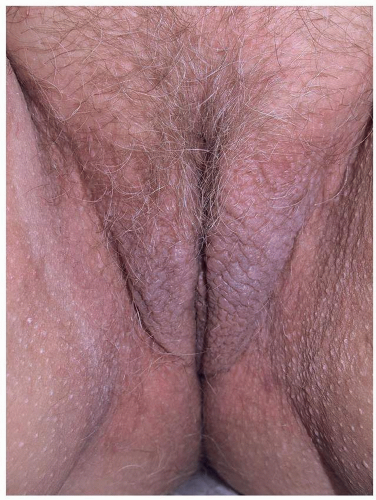 FIG. 6.4. Scale is subtle on this vulva due to the moist environment, although dusky thickening from rubbing is remarkable. |
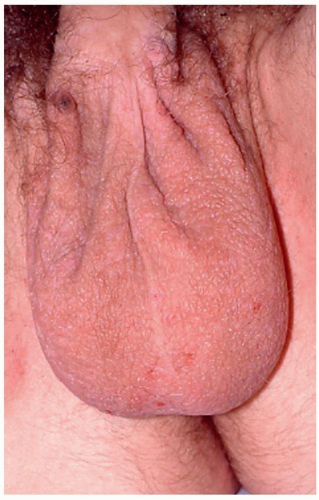 FIG. 6.5. The scrotum is thickened with rough scale from constant rubbing; a few excoriations are also present. |
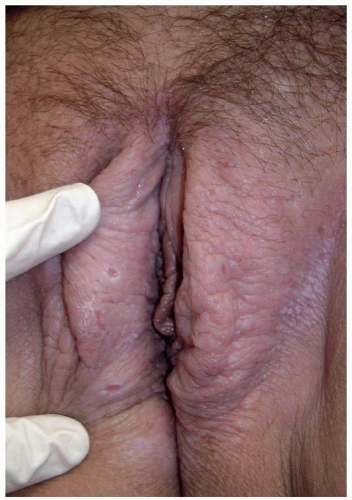 FIG. 6.8. Despite obvious lichenification and irregular excoriations, the expected erythema is overshadowed by the white surface produced by hydration of the epithelium from the moist environment. |
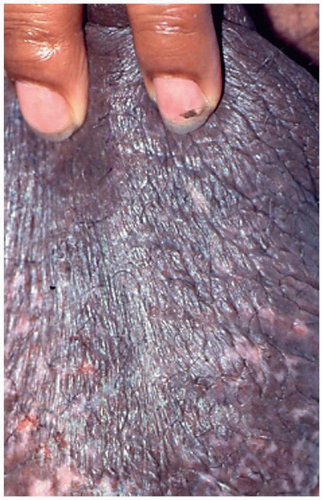 FIG. 6.9. Fairly well-demarcated, irregular white discoloration has resulted from excoriations that remove the normally pigmented skin. |
Diagnosis
The diagnosis of LSC is usually made on the basis of the clinical findings. In some instances, it is not clear whether the LSC is arising de novo (primary LSC) or when the “itch-scratch cycle” is superimposed on another underlying dermatologic problem (secondary LSC). This is particularly likely to happen with genital psoriasis but is also common with tinea cruris in men and lichen sclerosus in women. One might think that biopsy could identify the presence of any underlying problem in the setting of secondary LSC, but often this is not true. In
the acute phase of LSC, spongiotic inflammation will be prominent, and this finding may obscure the presence of an associated disorder. Even more confusion generally occurs when chronic LSC is biopsied. In this situation, the report is often signed out as “psoriasiform dermatitis,” which will not offer the clinician much help in trying to determine whether or not psoriasis is present. If this occurs, the clinician will have to undertake a clinical-pathologic correlation (1). Because candidiasis is the condition most commonly associated with the development of LSC in women, culture and/or KOH examination for associated candidiasis will be worthwhile. In men, if the upper inner thighs are involved, it may be useful to obtain a KOH and/or culture for dermatophyte fungi associated with tinea cruris.
the acute phase of LSC, spongiotic inflammation will be prominent, and this finding may obscure the presence of an associated disorder. Even more confusion generally occurs when chronic LSC is biopsied. In this situation, the report is often signed out as “psoriasiform dermatitis,” which will not offer the clinician much help in trying to determine whether or not psoriasis is present. If this occurs, the clinician will have to undertake a clinical-pathologic correlation (1). Because candidiasis is the condition most commonly associated with the development of LSC in women, culture and/or KOH examination for associated candidiasis will be worthwhile. In men, if the upper inner thighs are involved, it may be useful to obtain a KOH and/or culture for dermatophyte fungi associated with tinea cruris.
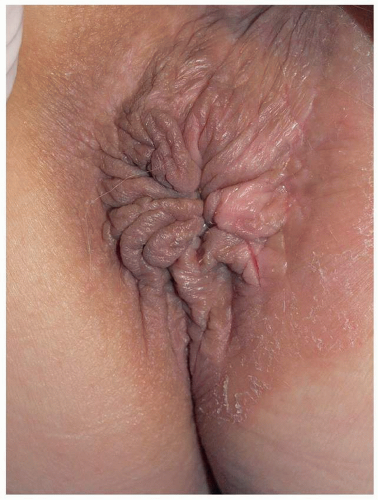
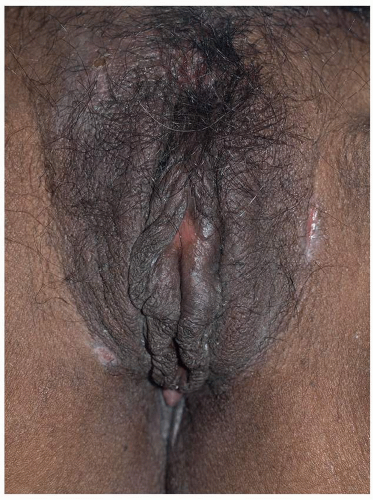 FIG. 6.12. This vulva shows dark brown lichenification, due both erythema seen through dark skin and coexisting postinflammatory hyperpigmentation. |
Psoriasis can be very similar in appearance to LSC, especially in the anogenital area where LSC may be superimposed over psoriasis. Helpful clues to the presence of psoriasis would be the presence of more typical psoriatic plaques in characteristic sites elsewhere, the identification of typical psoriatic nail changes, and the presence of psoriatic arthritis. Unfortunately, as noted above, biopsy may not be helpful in separating psoriasis from LSC. In women, LSC frequently overlies vulvar lichen sclerosus and may obscure the typical clinical characteristics of this condition. However, architectural damage such as the presence of clitoral hooding, loss of the labia minora, or the presence of purpura would help to identify associated lichen sclerosus. Biopsy may or may not be helpful in this situation.
At the histologic level, LSC can be confused with the often rather mundane appearance of the differentiated (non-HPV related) squamous cell intraepithelial neoplasia (see VIN in Chapter 5). Moreover, the frequent histologic presence of epithelial acanthosis, similar to that seen in LSC, immediately adjacent to the carcinoma raises a question of what, if any, relationship might exist between LSC and the development of genital squamous cell carcinoma.
Pathophysiology
The cause of LSC is not known. A large proportion of the patients who develop LSC have a personal or immediate family history of hay fever, asthma, or earlier eczematous skin disease and thus are presumably atopic. But it is still not clear just how atopy results in the development of LSC. There is increasing appreciation that many, if not most, patients with atopic dermatitis possess both filaggrin mutations and lipid disturbances that interfere with the normal development of the outer layer of the epidermis (“the barrier layer”) (7). These barrier layer defects allow easier exposure and processing of both irritants and allergens. Presumably, these defects in the barrier layer also allow easier triggering of the terminal branches of sensory nerves that carry itch and light pain. Even though peripheral eosinophilia and elevated serum IgE levels are frequently present, atopic dermatitis is different from other atopic disorders in that the immune dysfunction associated with it is T-cell mediated rather than occurring as a type 1 IgE-related humoral dysfunction as occurs in hay fever and asthma. Atopic dermatitis appears to involve the TH2 component of the cell-mediated immune system, and this process is presumably responsible for the increased serum IgE levels and peripheral eosinophilia that is often present (8).
In addition to such peripheral abnormalities, it seems likely that there are also important central aspects. Possibly, there is a heightened appreciation for itching at the level of the sensory cortex and maybe an innate tendency for the development of the obsessive-compulsive-like scratching that characterizes the itch-scratch cycle in LSC. Some clinicians also believe that patients with atopic dermatitis, and by extrapolation, some of those with LSC, have mild-to-moderate psychological abnormalities such as heightened anxiety levels, stress vulnerability and obsessive-compulsive traits that may play a role in causation and worsening of the disease (9). Moreover some clinicians, including myself, believe that there is a predilection for internalization of anger and hostility that is distinctive for patients with atopic dermatitis.
At the clinical level, it is apparent that factors in the local environment, such as heat and sweating, trigger both the initiation and the continuation of the process (3). As opposed to this important role for contact irritants, the role of contact allergens is much more controversial. A significant proportion of patients with anogenital dermatitis are reported to have relevant positive patch tests (10). However, data indicating that removal of the offending agent leads to resolution of the problem are lacking. Based on our personal experience, patch testing in patients with LSC is rarely necessary or helpful.
Management
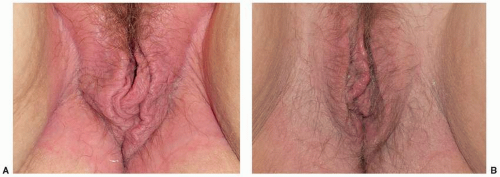
LSC is a chronic disease. Left untreated, the itch-scratch cycle persists indefinitely, although it can be somewhat episodic rather than consistently present. This process is extremely discomforting for the patient, and it may lead to a significant decrement in quality of life (11). Other troublesome sequelae may include hyperpigmentation and hypopigmentation due to activation or destruction of melanocytes, respectively. Treatment for LSC can be extremely effective (Fig. 6.14A, B). Approach to therapy includes five basic steps: (a) improvement in the local environment to reduce the triggering that leads to itching and scratching, (b) restoration of normal barrier layer function, (c) reduction in inflammation, (d) cessation of the itch-scratch cycle, and (e) identification and treatment for any detrimental psychologic factors that may be present.
Improvement in the Local Environment
As mentioned previously, heat and sweat act as provoking factors for the development of both itching and inflammation. Removing or reducing these factors is certainly desirable but is more difficult to do than one might expect. Immediate steps include a change to less occlusive, tight-fitting clothing and the use of materials (such as cotton and cotton blends) that allow for better movement of air. Contrary to decades of physician recommendations, the avoidance of dyes in underwear (“use white underwear only!”) lacks any scientific merit. Other environmental approaches to reduce sweat retention and its consequent contribution to maceration include the avoidance of prolonged sitting, the use of cloth rather than vinyl for seating surfaces, and the use of cooler temperatures in the workspace or home. Weight loss can help those who are particularly obese by way of decreasing intertriginous surface area and reducing frictional rubbing. Note that the use of hair dryers, even on their lowest temperature settings, in an attempt to dry the area is not helpful and in most instances is detrimental.
Other contact irritants include fecal contamination and, for women, the chronic presence of urine and vaginal secretions. Discussion of approaches to fecal and urinary incontinence is outside the scope of this chapter, but additional medical consultation will probably be necessary for ameliorating these two factors. Vaginal discharge needs to be properly diagnosed and treated (see Chapter 15). The regular use of panty liners should be discouraged. Excess hygiene, by way of removing natural skin lubricants, can also be irritating. Asking the patient about the frequency and nature of anogenital hygiene is important because many patients, especially women, think of the anogenital area as a site that is “especially dirty.” Again, contrary to popular opinion, laundering practices for underwear (number of rinses, use of certain detergents, use of antistatic dryer strips, etc.) are for practical purposes never an important triggering factor.
Restoration of Barrier Layer Function
Barrier layer function is never intact in patients with atopic dermatitis and LSC. This dysfunction occurs as a result of genetic factors interfering with epithelial cell differentiation, the irritant factors mentioned above, and the physical disruption of the surface epithelium due to scratching and rubbing. The approach to all three of these factors involves the use of lubrication. Since lubricants are covered in detail in Chapter 3, this material will not be repeated here. Irritants can be dealt with as described in the preceding two paragraphs, and the reduction of scratching is covered below.
Reduction in Inflammation
Steroids, used topically or systemically, are the sine qua non for the treatment of inflammation. This subject is covered in Chapter 3 in the section “Anti-inflammatory Therapy” and, other than discussion of a few important principles, will not be repeated here. First, the strength of the topical steroid must be appropriate for the task at hand. Low- and mid-potency steroids such as hydrocortisone and triamcinolone are usually ineffective in adults. Second, an ointment vehicle, rather than a cream, will be better tolerated and adds a bit of lubrication. Third, topical steroids must be continued for a month or more after the clinical symptoms and signs have regressed. However, after clinical clearing, the frequency of application or the strength of the topical steroid may appropriately be tapered. This long duration of therapy is necessary because microscopic evidence of inflammation remains for a considerable period of time after apparently complete clinical improvement is noted. Fourth, if topical steroids have not been effective after a month of treatment, the use of systemic steroid therapy should be considered. While a “burst” of prednisone can work, it is usually too short to be maximally effective, and, in addition, rebound
often occurs shortly after the last pills are administered. For this reason, we advocate for the use of intramuscularly administered triamcinolone (Kenalog) as described in Chapter 3. The use of nonsteroidal calcineurin inhibitors tacrolimus and pimecrolimus in an attempt to reduce the side effects of prolonged steroid use may be considered, but the stinging on application and an efficacy less than mid- and high-potency represent significant limitations (12). The use of systemic anti-inflammatory therapy, other than the systemic steroids mentioned above, falls outside the scope of this book. Nevertheless, I would be remiss if I failed to mention dupilumab, which blocks IL-4 and IL-13 signaling. In clinical trials, it has shown remarkable efficacy and quite acceptable safety and likely will achieve FDA approval by the time this book is published (13).
often occurs shortly after the last pills are administered. For this reason, we advocate for the use of intramuscularly administered triamcinolone (Kenalog) as described in Chapter 3. The use of nonsteroidal calcineurin inhibitors tacrolimus and pimecrolimus in an attempt to reduce the side effects of prolonged steroid use may be considered, but the stinging on application and an efficacy less than mid- and high-potency represent significant limitations (12). The use of systemic anti-inflammatory therapy, other than the systemic steroids mentioned above, falls outside the scope of this book. Nevertheless, I would be remiss if I failed to mention dupilumab, which blocks IL-4 and IL-13 signaling. In clinical trials, it has shown remarkable efficacy and quite acceptable safety and likely will achieve FDA approval by the time this book is published (13).
Breaking the Itch-Scratch Cycle
This is the single most important aspect in the treatment of LSC. Unfortunately, it is also the most often overlooked. The presence of clothing, a conscious attempt to control scratching, and embarrassment over scratching the genitalia prevents much daytime scratching. However, these constraints are generally not present at night and thus do not prevent the nighttime scratching that characteristically is present. Approaches for the treatment of nighttime rubbing and scratching are thoroughly covered in Chapter 3, but several major principles will be reviewed here. First, nighttime scratching occurs periodically while the patient is in the lighter stages of sleep (4,14). Nonhabituating medications with a sedative effect such as the first generation of antihistamines and certain tricyclics work well for this purpose. Second, the dose of the medication chosen should be increased until nighttime scratching ceases or until the risks of side effects caution against any further increase. Third, the medication should be taken about 2 hours before the expected hour of sleep. This results in the rapid onset of sleep shortly after the patient goes to bed and greatly helps to prevent morning “hangover.” Fourth, the medication should be taken every evening rather than on an “as necessary” basis.
In many instances, sedating therapy for nighttime scratching obviates the need to treat daytime itching with medications, such as hydroxyzine, that can cause sleepiness or dangerous operation of machinery. However, some patients will still experience significant daytime pruritus. Many clinicians prescribe nonsedating antihistamines for these individuals. Unfortunately, this approach does not work well probably because histamine plays only a minor role in the itching associated with atopic dermatitis and LSC. In this situation, I prefer the use of selective serotonin reuptake inhibitors (SSRIs). It is not clear whether these agents work because of their beneficial effect on anxiety and depression or whether they diminish the obsessive-compulsive component of chronic scratching. While I strongly support this use of SSRIs, there is only limited support for this approach in the medical literature (15). Further information on the use of SSRIs can be found in Chapter 3.
Identification and Treatment of Detrimental Psychological Components
Anxiety and/or depression is regularly present in patients with LSC (9). Most patients will not volunteer this information unless it is directly sought by a clinician. Even then, the importance of psychological factors tends to be minimized by patients, and thus questioning in this area should occur not just initially but also periodically at the time of return visits. Some controversy exists as to whether these psychological factors play a role in the etiology of the LSC or whether they occur secondary to the presence of LSC. It is my opinion, supported by some published data, that they are frequently important in causation (9). But, either way, once identified, treatment, most often with SSRIs as described in Chapter 3, is very helpful.
In addition to the common problems of anxiety and depression, patients with eczematous disease such as LSC may also experience sexual dysfunction (16). Although most of us would not consider ourselves as expert in the area of sexual counseling, giving patients an opportunity to discuss this aspect of their lives can also be quite beneficial in the treatment of patients with anogenital LSC.
Irritant Contact Dermatitis
Irritant contact dermatitis is an eczematous reaction that develops in response to an exogenous substance that can cause an inflammatory reaction when applied to the skin of any individual. Thus, all individuals have the potential for developing irritant contact dermatitis, whereas only patients specifically sensitized to an allergen develop allergic contact dermatitis (see next section).
Clinical Presentation
The prevalence of irritant contact dermatitis involving the anogenital area is unknown, although two major studies indicated that irritant contact dermatitis accounted for about 20% of all patients with anogenital problems referred to dermatologists for patch testing (10,17).
Irritant contact dermatitis can be divided into two categories: chronic and acute irritant contact dermatitis.
Chronic irritant contact dermatitis is usually manifested by symptoms of irritation, pain, soreness, or rawness. Note that in some patients, especially those who are atopic, the irritant can also cause itching and can initiate the itch-scratch cycle. Morphologically, the area affected in irritant contact dermatitis depends on where the contact occurred. Generally, this is manifested by a poorly
demarcated slightly scaly erythematous patch or slightly elevated plaque. Little or no edema is present (Fig. 6.15). The red hues sometimes occur at the dusky red or brownred end of the erythema spectrum (Fig. 6.16). Often, there is a dry, glazed, fissured, chapped appearance (Figs. 6.17 and 6.18). If the irritant in question triggered itching and scratching, the morphology will be indistinguishable from that of LSC.
demarcated slightly scaly erythematous patch or slightly elevated plaque. Little or no edema is present (Fig. 6.15). The red hues sometimes occur at the dusky red or brownred end of the erythema spectrum (Fig. 6.16). Often, there is a dry, glazed, fissured, chapped appearance (Figs. 6.17 and 6.18). If the irritant in question triggered itching and scratching, the morphology will be indistinguishable from that of LSC.
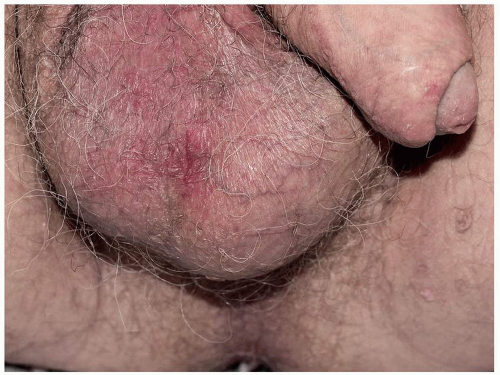 FIG. 6.15. This mild redness and scale of irritant contact dermatitis was caused by frequent washing with povidone-iodine solution. |
Acute irritant contact dermatitis is essentially a chemical “burn.” The rapid appearance of erythema, edema, and sometimes blistering is typical (Fig. 6.19). Poorly keratinized skin, such as the modified mucous membranes of the vulva, the glans penis, and the inner aspect of the prepuce, is very fragile, and blister roofs if present are shed quickly, forming erosions or even ulcers (Figs. 6.20 and 6.21). On the more resilient keratinized skin, blisters may remain visible for a day or two before they too become unroofed, leaving erosions or ulcers (Fig. 6.22).
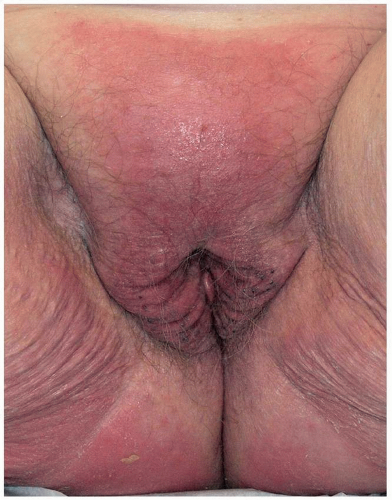 FIG. 6.16. Poorly demarcated, glazed, chapped plaque that spares skin folds is a common finding produced by chronic irritation of urine in this elderly incontinent woman. |
Diagnosis
The diagnosis of chronic irritant contact dermatitis is made on the appearance as described above, together with a history that suggests undue exposure to soap, water, sweat, urine, feces, vaginal discharge, or less frequently encountered irritants such as listed within the
section on “Pathogenesis.” Biopsy is rarely necessary and, if carried out, provides only a nonspecific histologic picture of spongiosis, superficial perivascular lymphocytic inflammation, and sometimes epithelial acanthosis (18). That is, the histology only indicates that the problem is an eczematous process without specifically pointing toward an irritant contact etiology. The differential diagnoses are primarily the other eczematous diseases, especially LSC, as described above. Differentiation from allergic contact dermatitis can be problematic. Patch testing may be helpful in this regard (17), but all too often a positive patch test result does not correlate with documentable exposure to that chemical or product. Uncommon and rare conditions that can mimic chronic irritant contact
dermatitis include candidiasis, extramammary Paget disease, Hailey-Hailey disease, and Darier disease.
section on “Pathogenesis.” Biopsy is rarely necessary and, if carried out, provides only a nonspecific histologic picture of spongiosis, superficial perivascular lymphocytic inflammation, and sometimes epithelial acanthosis (18). That is, the histology only indicates that the problem is an eczematous process without specifically pointing toward an irritant contact etiology. The differential diagnoses are primarily the other eczematous diseases, especially LSC, as described above. Differentiation from allergic contact dermatitis can be problematic. Patch testing may be helpful in this regard (17), but all too often a positive patch test result does not correlate with documentable exposure to that chemical or product. Uncommon and rare conditions that can mimic chronic irritant contact
dermatitis include candidiasis, extramammary Paget disease, Hailey-Hailey disease, and Darier disease.
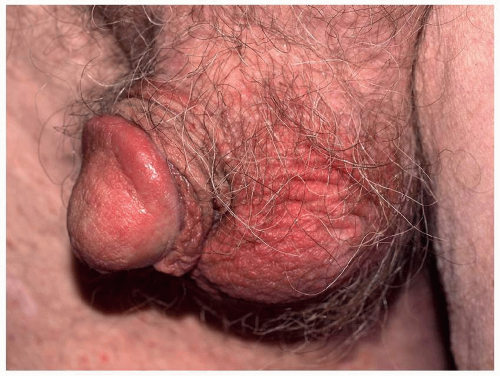 FIG. 6.18. The redness and erosion of the glans penis and scrotum of this patient resulted from frequent soaks in an antibacterial mouthwash. |
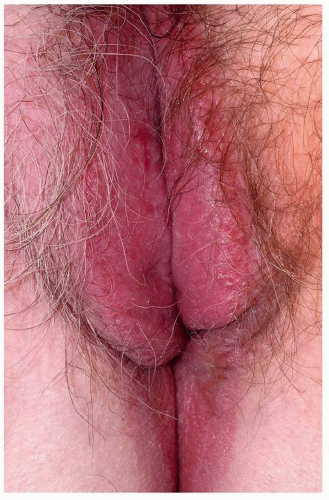 FIG. 6.19. The deep erythema and erosion of the vulva were caused by the application of a compounded topical anesthetic applied before a surgical procedure. |
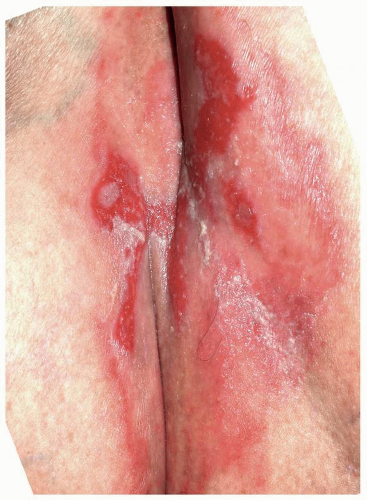 FIG. 6.20. Blisters from diarrhea held under adult diapers and between skin folds evolved quickly into painful erosions. |
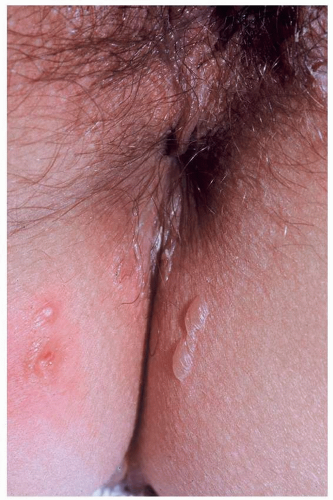 FIG. 6.22. The application of trichloroacetic acid has produced clear vesicles of acute irritant contact dermatitis; essentially, this is a chemical burn. |
The diagnosis of acute contact dermatitis is easier to establish because of the short interval between exposure and development of inflammation. Thus, patients can almost always identify the contactant that caused the problem. Often the products responsible are medications that have been recently been applied by medical personnel (Table 6.1). On the rare occasions where such a history is not forthcoming, one should consider the possibility of obsessive-compulsive disorder or factitial disease caused by the patient or the patients’ caretakers. Biopsy is not useful in acute irritant contact dermatitis as the histology only shows disruption or destruction of the epithelium without pointing to a specific cause.
Pathophysiology
Irritant contact dermatitis can be caused either by repeated exposure to a weak irritant (chronic irritant contact dermatitis) or by one, or only a few, exposures to a very strong irritant (acute irritant contact dermatitis) (Table 6.1). The most common causes of chronic irritant contact dermatitis are overexposure to soap and water and chronic exposure to urine or feces in a diapered infant or an incontinent adult. Other chronic irritants include douches, feminine hygiene products, depilatories, personal lubricants, and spermicides. An often overlooked irritant is the presence of candidiasis where the candidal proteins can cause irritation quite apart from true infection. Because repeated exposure is necessary for the development of irritant contact dermatitis and because the symptoms and signs develop gradually, the patient is frequently unaware that the offending substance is irritating and is thus playing a role as a cause of his or her problem.
TABLE 6.1 Causes of irritant contact dermatitis | ||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| ||||||||||||||||||||||||||||||||||||||||
Because acute irritant contact dermatitis is produced by one or only a few exposures to a very strong irritant, this exposure is often accompanied by a very short duration of time before pain, burning, and stinging are noted. For this reason, the patient usually knows what caused the problem, although he or she frequently misinterprets this as allergy rather than irritation. The most common causes of acute irritant contact dermatitis include various treatments for genital warts, such as trichloroacetic and bichloroacetic acids, podophyllin products, imiquimod, and cantharidin. Some patients with very sensitive skin can experience acute irritant contact dermatitis to the cream, gel, or solution vehicles used in topical medications and lubricants. This is probably the result of chemicals such as alcohol, propylene glycol, and polyethylene glycol. This type of problem is frequently experienced with the “azole” group of anticandidal/antifungal creams (Fig. 6.17). Lastly, keep in mind that patients will sometimes apply very unorthodox products to their genitalia in misguided attempts to clean an area that is perceived to be “dirty” or “odorous.” We have seen reactions to things such as lye, kerosene, and bleach.
Management
The most important aspects of therapy are the identification and elimination of all irritants. Irritant contact dermatitis in the genital area is often multifactorial, so all medications, soaps, antiseptics, douches, powders, and vigorous to hygiene should be discontinued. However, keep in mind that some patients become “addicted” to certain behaviors and as a result there may be very poor compliance with instructions to cease these ritualistic behaviors. After the offending agent(s) are discontinued, chronic irritant contact dermatitis improves quickly and is hastened by the use of a mid-potency topical corticosteroid ointment, such as triamcinolone 0.1% applied twice a day. If the skin is dry and chapped, lubricants (see Chapter 3) may be useful. Infants and diapered adults may require the use of a “barrier” product such as zinc oxide ointment to keep urine and feces away from the skin. In those instances where itching or pain is really troublesome, prednisone, at a dose of 40 mg each morning for a few days, can lead to symptomatic improvement until healing is well under way, at which point a mid- or low-potency topical corticosteroid can be substituted.
The pain and burning of acute irritant contact dermatitis can be minimized through the use of tepid tap
water bathtub soaks several times a day for the first few days. Lubrication with a thin layer of petrolatum should be applied immediately following each soak. Nighttime sedation and oral analgesics may be necessary for several days. Topical analgesics should be avoided as they may cause additional discomfort.
water bathtub soaks several times a day for the first few days. Lubrication with a thin layer of petrolatum should be applied immediately following each soak. Nighttime sedation and oral analgesics may be necessary for several days. Topical analgesics should be avoided as they may cause additional discomfort.
Allergic Contact Dermatitis
As opposed to irritant contact dermatitis wherein all individuals are potentially capable of developing the problem, allergic contact dermatitis requires immunologic processing. This is a more restrictive process, and only certain individuals exposed to a potential allergen will develop allergic contact dermatitis at the time of their next contact with the allergen.
Clinical Presentation
Controversy exists regarding the frequency with which allergic contact dermatitis of the genitalia occurs. Nearly all of the published material on prevalence deals primarily with contact dermatitis of the vulva in women (18). However, excellent articles by Warshaw et al. and Bauer et al. summarize this work and also adds new information regarding contact dermatitis in men (10,17). The information contained in these studies regarding patients with anogenital disease sent for patch testing suggest that one or more clinically relevant positive patch tests will be found in 15% to 40% of women with vulvar dermatoses and that the frequency in men is roughly similar. Two studies found that irritant contact dermatitis was less common than allergic contact dermatitis (10,17), but another study (18) together with our own observations suggests that, at least for women, the opposite is true. This discrepancy probably revolves around two potential problems. First, there is considerable difficulty in determining which positive patch tests are truly clinically relevant. Second, patients with rigorously defined atopic dermatitis have an extraordinarily high frequency of positive patch tests to common environmental allergens and it is not known what role, if any, these allergens play in the pathogenesis of their dermatitis (19).
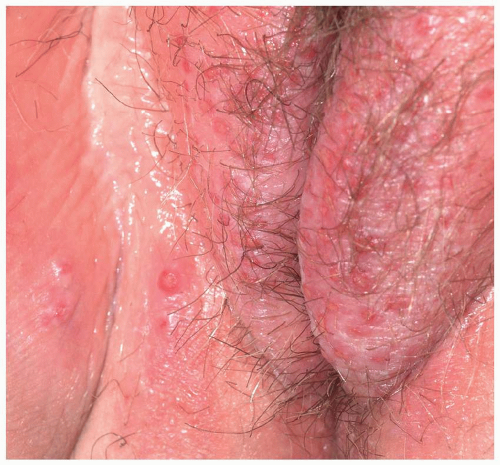
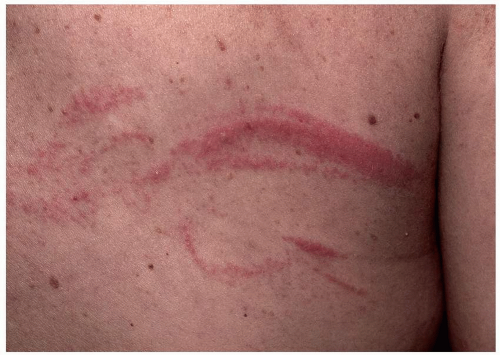
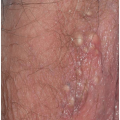
Allergic contact dermatitis is characterized by the presence of poorly marginated, bright red, edematous patches and plaques (Fig. 6.23). Scale is generally less prominent than it is in atopic dermatitis and irritant contact dermatitis. Pruritus is regularly present and in some instances can be quite problematic. Not surprisingly, this frequently results in the development of the itch-scratch cycle and the consequent development of the clinical signs of LSC. Sometimes, vesicles, usually minute in size (representing macroscopic evidence of histologic spongiosis), stud the surface of the erythematous plaques (Fig. 6.24). Occasionally, odd shapes (linear or angular) are found (Fig. 6.25). These generally occur by way of irregular application of medications applied with the finger tips. The labia majora are usually involved in women, and both the penis and the scrotum may be affected in men. Perianal involvement is found in both sexes (10).
Allergic contact urticaria, as opposed to dermatitis, is rarely encountered and is a separate and distinct disorder from allergic contact dermatitis. The appearance can be that of tissue swelling (angioedema) or can develop as
urticarial papules (wheals, “hives”) and plaques that are entirely similar to those that occur with garden-variety urticaria. Unlike the situation with allergic contact dermatitis, there is no clinical evidence of epithelial abnormalities. Such reactions are usually easy to recognize because of the quick development of the urticarial reaction within minutes after contact has taken place.
urticarial papules (wheals, “hives”) and plaques that are entirely similar to those that occur with garden-variety urticaria. Unlike the situation with allergic contact dermatitis, there is no clinical evidence of epithelial abnormalities. Such reactions are usually easy to recognize because of the quick development of the urticarial reaction within minutes after contact has taken place.
Diagnosis
The diagnosis of allergic contact dermatitis is most often made on a clinical basis. The role of patch testing for patients with eczematous disease of the genitalia is controversial. Some clinicians believe that a diagnosis of allergic contact dermatitis is often missed unless all patients presenting with an eczematous morphology are patch tested (10,17). Others, like ourselves, believe, in accordance with the Bayes theorem, that patch testing is best carried out only in highly selected patients so as to reduce the large number of false-positive results that occur when testing is carried out in a relatively unselected population. Moreover, the simple presence of a positive patch test does not prove that the disease in question is due to that allergen. It is necessary first to identify the presence of that allergen in one or another of the products coming in contact with the patient’s tissue and, second, for marked clinical improvement to occur when use of the offending product is discontinued. Absolute proof would require a new episode of contact with the suspected product to see whether the rash redevelops. However, this latter approach is almost uniformly rejected by the patients!
Biopsy is not likely to be helpful because the principle findings of spongiosis and acanthosis are essentially identical to those in all of the other eczematous diseases. In spite of this, some believe that the presence of eosinophils in the inflammatory infiltrate suggests a high likelihood of allergic contact dermatitis.
All of the eczematous disorders, as described in this chapter, need to be considered in one’s list of differential diagnoses. In addition, one should bear in mind the possibility of candidiasis and the dermatophyte fungal infection, tinea cruris.
Pathophysiology
Allergic contact dermatitis represents a cell-mediated, delayed-type (type IV) hypersensitivity reaction. It arises when a chemical, acting as an antigen, is processed by macrophages (Langerhans cells) in the epidermis and is then presented to the T-cell immune system. This results in the development, activation, and proliferation of antigen-specific T cells. These cells return to the skin at the time of the next contact with allergen, resulting in the clinical development of allergic contact dermatitis (18).
The most common causes of allergic contact dermatitis in the anogenital area are either prescription or over-the-counter topical medications (20). The agent we have most often incriminated is benzocaine, which is a component of Vagisil and some other topical analgesics. In addition to these products, clinicians who frequently carry out patch testing identify numerous other substances that are potential offenders (10,17,18). The most common of these substances are listed in Table 6.2. Note specifically that positive patch tests occasionally occur with several topically applied corticosteroids and with vehicles, preservatives, and stabilizers found in almost all cosmetic and medical products. In spite of the positive
patch tests, our experience suggests that these substances infrequently cause problems. However, in instances of recalcitrant anogenital dermatitis, discontinuation of all topically applied agents including corticosteroids and all lubricants other than petrolatum is warranted. If this is followed by improvement, agents can be added back one at a time in an attempt to identify the culprit.
patch tests, our experience suggests that these substances infrequently cause problems. However, in instances of recalcitrant anogenital dermatitis, discontinuation of all topically applied agents including corticosteroids and all lubricants other than petrolatum is warranted. If this is followed by improvement, agents can be added back one at a time in an attempt to identify the culprit.
TABLE 6.2 Causes of allergic contact dermatitis | ||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| ||||||||||||||||||||||||||||||||
A special situation occurs in patients who are allergic to seminal fluid and latex (21). These represent a type I, IgE-mediated, immediate reaction in which angioedema and urticarial papules and plaques arise within minutes of contact. These occur very infrequently but are mentioned because of the potential for development of anaphylaxis.
A number of commonly used products are not listed here because of controversy about their ability to cause either allergic or irritant reactions. These include soaps, laundry detergents, fabric softeners, antistatic sheets, medicated wipes, toilet paper (scented or unscented), menstrual pads, and other feminine hygiene agents. In our opinion, normal use of these products rarely leads to anogenital dermatitis.
Management
The first step in therapy is the identification and elimination of the most likely offending contactant. If the responsible substance can be identified either clinically or through patch testing, the patient needs to be instructed regarding avoidance. This can be difficult because some allergens can be found in multiple and often apparently innocuous and unsuspected sources. Information regarding these potential sources can be found in standard dermatologic textbooks. In instances of suspected allergic contact dermatitis where a specific contactant cannot be identified, it may be necessary to counsel the patient to avoid all topical agents other than clear water and petrolatum.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree