22 Reconstructive burn surgery
Synopsis
 Improvements in burn survival have shifted the focus of burn care and research towards long-term outcomes. Accordingly, reconstructive burn surgery has become an increasingly relevant topic in the care of the burn patient.
Improvements in burn survival have shifted the focus of burn care and research towards long-term outcomes. Accordingly, reconstructive burn surgery has become an increasingly relevant topic in the care of the burn patient.
 Burn reconstructive surgery seeks to restore both form and function lost to burn injury and relies on many of the basic principles of plastic surgery.
Burn reconstructive surgery seeks to restore both form and function lost to burn injury and relies on many of the basic principles of plastic surgery.
 Timing of reconstructive procedures is contingent not only on the readiness and impact of a particular scar or wound but also on the psychological preparedness of the patient.
Timing of reconstructive procedures is contingent not only on the readiness and impact of a particular scar or wound but also on the psychological preparedness of the patient.
 The majority of secondary burn defects are due to scarring and contracture. To correct deformities, scar release is necessary and then appropriate coverage is obtained from skin grafts or flaps – either local or distant.
The majority of secondary burn defects are due to scarring and contracture. To correct deformities, scar release is necessary and then appropriate coverage is obtained from skin grafts or flaps – either local or distant.
 A postoperative plan that incorporates critical aspects of splinting and range of motion is needed to optimize outcome.
A postoperative plan that incorporates critical aspects of splinting and range of motion is needed to optimize outcome.
Introduction
Advances in critical care and surgical management have significantly improved survival following burn injury. In fact, survival following even severe burn injury has become the rule rather than the exception. Accordingly, there is increasing emphasis being placed on long-term outcomes following burn injury and reconstructive surgery for burn survivors has become an increasingly relevant topic in burn care.1 Burn reconstruction refers to the numerous and varied procedures performed on healed wounds or skin grafts. The overall goal of burn reconstruction is to improve both the appearance and function of the person who sustained a burn injury. These procedures should never be considered “cosmetic” – they are reconstructive as they seek to restore that which has been lost to injury.
Hypertrophic scars and contractures
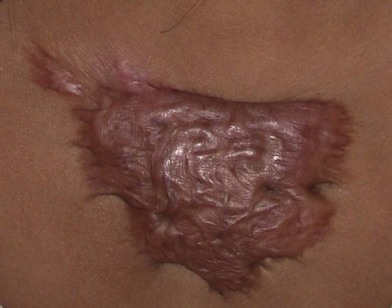
Hypertrophic scarring remains the most significant source of pain, discomfort, and misery for burn survivors and constitutes the chief complaint of the majority of patients seeking burn reconstruction (Fig. 22.1). Despite the frequent occurrence of these scars – estimated to be as high as over 50% – still little is known about the causative factors and, therefore, a cure or effective prevention strategy remains elusive. Risk factors for hypertrophic scarring include delay in wound closure, infection and race (i.e., patients with pigmented skin are believed to be at higher risk of forming hypertrophic scar).2 There have been several proposed prevention and treatment strategies for hypertrophic scars, including steroids, oral anti-inflammatory agents, pressure garments and silicon, and all have been reported to have varying levels of effectiveness. Steroid injection into scars and topical silicon sheeting can be used during the period of scar maturation to alleviate symptoms of pain and itch and potentially improve scar appearance. However, scar injection may be difficult to perform in children and is seldom useful for broad areas of hypertrophic scar.
Overview of techniques for reconstructive surgery
Scar release
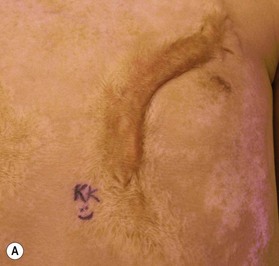
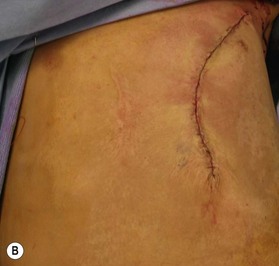
In some cases, total scar excision is necessary and practical. This is particularly true for smaller or discrete areas of scar. There are two general approaches to scar excision: intralesional and extralesional. When performing intralesional excision, a rim of scar is left in the wound and subsequently closed. The purported benefit of intralesional excision is that there will be no new tissue injury – the incision is made through previously scarred tissue only and therefore the process of scar formation has already occurred in this tissue and is unlikely to recur (Fig. 22.2). This is in contradistinction to extralesional excision, in which the incision is made in the healthy tissue surrounding the scar so the entire scar can be removed. The relative risks and benefits of each approach should be discussed with the patient prior to surgery. Many scars are too large to be removed in one setting and often require several “serial” excisions. We typically wait 8–12 months between serial excisions in order that the tissue can sufficiently heal and soften so that it can be optimally mobilized again to achieve closure.
Wound closure
Local flaps
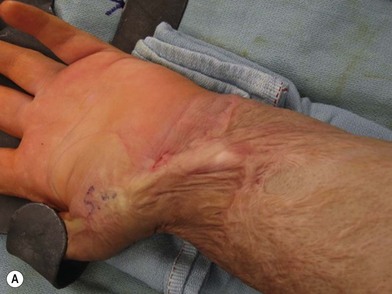
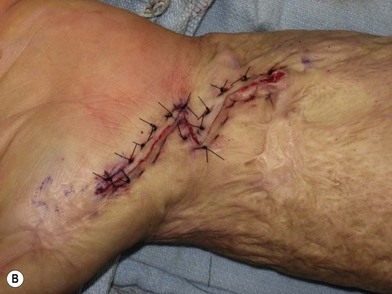
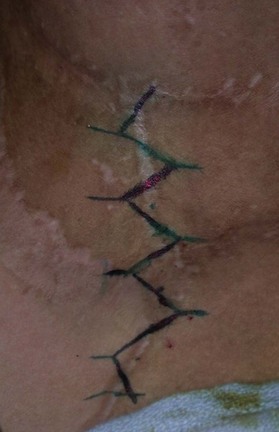
There exists a veritable alphabet soup of local tissue rearrangement flap options that have been described, including Z-plasty, Y-V-plasty, V-Y-plasty and W-plasty. Each has its distinctive geometric properties, as well as relative benefits. We most commonly use Z-plasties (Fig. 22.3) and Y-V-plasties to address scar bands (Fig. 22.4). It is critical to understand that these procedures are most appropriate for scar lengthening and are not the solution to all reconstructive problems. Areas with even moderate degrees of missing tissue will be inadequately addressed by a Z-plasty and require the addition of soft tissue either in the form of a skin graft or a flap. The principal drawback to Z-plasty use is that transposition and advancement of the Z-limbs requires extensive undermining and this often means undermining scar that can result in partial flap ischemia. For this reason, in many cases we prefer to use Y-V plasties because they require minimal flap undermining in order to achieve the desired advancement.