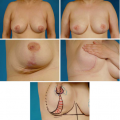
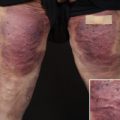
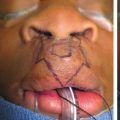
Randomized Controlled Trial Comparing Health-Related Quality of Life in Patients Undergoing Vertical Scar versus Inverted T–Shaped Reduction Mammaplasty
Achilleas Thoma M.D., M.Sc.
Teegan A. Ignacy B.Sc.
Eric K. Duku Ph.D.
Robert S. Patterson M.D.
Arianna Dal Cin M.D.
Carolyn M. Levis M.D., M.Sc.
Charles H. Goldsmith Ph.D.
Hamilton, Ontario; and Burnaby, British Columbia, Canada
From the Division of Plastic Surgery, Department of Surgery, the Department of Clinical Epidemiology and Biostatistics, the Surgical Outcomes Research Center, and the Department of Psychiatry and Behavioral Neurosciences, McMaster University; and the Faculty of Health Sciences, Simon Fraser University.
Received for publication September 14, 2012; accepted January 17, 2013.
This trial is registered under the name “Vertical Scar Versus Inferior Pedicle Reduction Mammoplasty,” Clinical Trials.gov identification number NCT00149344 (http://clinicaltrials.gov/show/NCT00149344).
Presented at the 16th World Congress of the International Confederation for Plastic, Reconstructive and Aesthetic Surgery, in Vancouver, British Columbia, Canada, May 21 through 27, 2011; the 91st Annual Meeting of the American Association of Plastic Surgeons, in San Francisco, California, April 14 through 17, 2012; and the 66th Annual Meeting of the Canadian Society of Plastic Surgeons, in Toronto, Ontario, Canada, June 5 through 9, 2012.
Copyright © 2013 by the American Society of Plastic Surgeons
DOI: 10.1097/PRS.0b013e3182910cb0
Disclosure: The authors have no financial disclosures or conflicts of interest with the content presented.
Background: There is controversy regarding the superiority of the vertical scar reduction technique versus the inverted T–shaped reduction technique for breast reduction surgery.
Methods: Two hundred fifty-five patients were randomized to either the vertical scar reduction or inverted T–shaped reduction technique immediately before surgery over a 5-year period. Patients completed the Health Utilities Index Mark 3, Short Form-36, Breast-Related Symptoms Questionnaire, and Multidimensional Body-Self Relations Questionnaire at 1 week preoperatively and 1, 6, and 12 months postoperatively. Data were treated according to intention-to-treat principles. The primary outcome was the difference in the change in Health Utilities Index Mark 3 score from baseline to 12 months postoperatively between the two techniques.
Results: Patients undergoing either technique gained a statistically significant and clinically important improvement from baseline to 1 year postoperatively in the Health Utilities Index Mark 3 (vertical scar reduction, 0.81, 0.16 to 0.87, 0.19; inverted T–shaped reduction, 0.79, 0.20 to 0.89, 0.15) and the Breast-Related Symptoms Questionnaire (vertical scar reduction, 50.26, 12.98 to 95.59, 9.36; inverted T–shaped reduction, 50.06, 12.50 to 94.09, 9.86). No difference in mean change in scores from baseline to 12 months postoperatively was seen in any of the quality of life questionnaires between the techniques.
Conclusions: There was a clinically important improvement between baseline and 1 year postoperatively in both groups in the Health Utilities Index Mark 3 and the Breast-Related Symptoms Questionnaire. The authors conclude that the techniques are similar when quality of life is the outcome of interest. (Plast. Reconstr. Surg. 132: 48e, 2013.)
CLINICAL QUESTION/LEVEL OF EVIDENCE: Therapeutic, I.
There is cumulative evidence from several observational studies that breast hypertrophy is associated with clinically important morbidity and reduced health-related quality of life and that breast reduction has a beneficial effect.1–9 A randomized controlled trial comparing reduction mammaplasty to no surgery in patients with breast hypertrophy using quality-of-life scales confirmed the clinical benefit of surgery.10 The improvement in quality of life after breast reduction using the inverted T–shaped reduction technique was recently quantified to be 5.32 Quality Adjusted Life Years, which is equivalent to each patient gaining on average an additional 5.32 years of life in perfect health.11
On reviewing the breast reduction literature, there are two main techniques, with their characteristic scars, used in North America currently. The inverted T–shaped reduction technique was popularized by many authors in the 1970s.12–15 Vertical scar reduction was promoted over the years by others.16–20
In 2002, a survey of board-certified plastic surgeons demonstrated that inverted T–shaped reduction remained by far the most commonly used technique for breast reduction in the United States, preferred by 75.5 percent of survey respondents.21 A more recent survey among Canadian plastic surgeons showed that the inverted T–shaped reduction was preferred by 66 percent of surgeons.22 The pendulum may be shifting toward the vertical scar reduction technique because of the smaller scars and management of the learning curve.19
There is ongoing controversy concerning the superiority of one technique over the other in terms of patient satisfaction, complications, scar acceptance, and health care resource use.23–26 We found one randomized controlled trial that compared the vertical scar reduction and inverted T–shaped reduction techniques.23 The authors concluded that although complications rates were similar, there was a higher rate of dog-ears using the vertical scar reduction technique. Using a Likert-type satisfaction scale, the patients rated the procedures similarly in terms of overall satisfaction. Cruz-Korchin and Korchin23 found a statistically significant difference in terms of scar acceptance and the aesthetic results in favor of the vertical scar reduction technique. In appraising the Cruz-Korchin and Korchin23 randomized controlled trial, we found a number of methodologic weaknesses, including the use of even and odd chart numbers to allocate patients, no reporting of a sample size justification, no mention of the learning curve, and no use of validated health-related quality of life scales. We therefore remain uncertain about the superiority of vertical scar reduction over inverted T–shaped reduction mammaplasty in a number of outcomes, including health-related quality of life. In the past three decades, evidence-based medicine and clinical outcomes research movements have promoted measuring surgical outcomes from the patient’s perspective.27–30
The evidence from observational studies and the single randomized controlled trial suggests that there are no scientific or ethical concerns about one technique being better than the other, thus satisfying equipoise, the main precondition for performing a randomized controlled trial.31,32 The purpose of this study was to evaluate the superiority of vertical scar reduction mammaplasty to the inverted T–shaped reduction mammaplasty in terms of patient health-related quality of life.
Patients and Methods
This is a parallel randomized controlled trial comparing vertical scar reduction and inverted T–shaped reduction mammaplasty in terms of patient health-related quality of life. This study was approved by St. Joseph’s Healthcare Hamilton and Hamilton Health Sciences research ethics boards. The objectives of the trial were explained to the patients. All patients gave written consent to participate before study initiation.
All women older than 18 years with breast hypertrophy who were candidates for both procedures (women requiring <1000 g resected from each breast) and received approval from the Ontario Health Insurance Plan were asked to participate. If there was uncertainty as to whether the resection would exceed 1000 g, patients were asked to measure the volume of their breasts using the Archimedes displacement principle. If neither breast exceeded 1000 g, the patient was considered eligible for the study. The 1000-g threshold was used, as a number of authors have expressed caution about using the vertical scar reduction technique in very large breasts.20,23,33–36 Despite this restriction of cases involving less than 1000 g/breast, recent surveys of American and Canadian plastic surgeons revealed that the majority (80 percent and 87 percent, respectively) of reductions required the removal of less than 1000 g.21,22 Full inclusion/exclusion criteria are listed in Table 1. Baseline demographic information was collected before surgery.
Participating Surgeons and the Learning Curve
Four experienced plastic surgeons recruited participants from their private practices. The operations were performed at two McMaster University–affiliated hospitals in Hamilton, Ontario, Canada. All four surgeons
participated in standardizing the operative protocol. Before trial initiation, each surgeon watched a video describing the vertical scar reduction technique, which we considered the novel technique, and performed at least 10 vertical scar reduction procedures without complication before commencing patient recruitment.
participated in standardizing the operative protocol. Before trial initiation, each surgeon watched a video describing the vertical scar reduction technique, which we considered the novel technique, and performed at least 10 vertical scar reduction procedures without complication before commencing patient recruitment.
Table 1. Patient Eligibility Criteria | ||
|---|---|---|
|
Randomization
Patients were recruited at their preoperative appointment approximately 1 week before surgery. Patients were randomized 1 hour before the actual surgery using a remote site 24-hour telephone system that randomized patients using a computer-generated sequence. The surgeon marked the patient with markings according to the technique. A note was made on the case report form if there was deviation from technique execution. Patients were equally likely to be randomized to either group. Sequences were stratified by surgeon. Block sizes of 2 and 4 were used and group allocation balance was achieved at allocations of multiples of eight.
Blinding
Because of the distinct scar patterns of each technique, patients and investigators could not be blinded to the technique. A blinded statistician however analyzed the data, using data coded as treatment 1 and treatment 2.
Surgical Techniques
Vertical Scar Reduction
The vertical scar reduction technique used was similar to the technique described by Hall-Findlay.19 The nipple-areola complex was based on a superomedial pedicle.
Inverted T–Shaped Reduction
The inverted T–shaped reduction technique was based on the Robbins technique, with the nipple-areola complex based on an inferior deepithelialized breast pedicle.14 No liposuction was performed on the breast, as such cointervention would have confounded the study. This was a pragmatic study37 and, as such, the staff surgeon performed the breast reduction on one breast and the assistant senior plastic resident performed the breast reduction on the second breast under direct supervision. Different plastic surgery residents rotated through the services of each of the four participating surgeons over the 5-year period of the trial. The weight of the tissue excised from each breast was recorded and sent to the pathology laboratory for tissue examination.
Outcomes
Health-related quality of life was measured using four self-administered validated scales: the Health Utilities Index 338,39 and the Breast Reduction Assessment of Value and Outcomes instruments, consisting of the Short Form-36,40 the Breast-Related Symptoms Questionnaire,5,41 and the Appearance Evaluation domain of the Multidimensional Body-Self Relations Questionnaire.42 The health-related quality of life scales are further described in Table 2. No evaluation of aesthetic outcome was performed in the study. Each of the questionnaires was administered to patients 1 week preoperatively and 1, 6, and 12 months postoperatively. The questionnaires were administered to patients at their regular follow-up appointments. Questionnaires were administered in the same order for each visit. Patients were asked to complete the questionnaires based on how they are feeling in general during the current week. Patients who were unable to attend their 6- or 12-month follow-up appointments were mailed the questionnaires, which were to be completed at home and returned by mail.
Generic Utility Instruments: Health Utilities Index Mark 3
The Health Utilities Index is an instrument that assesses health-related quality of life.38,39,43 The Health Utilities Index Mark 3 has been demonstrated to be a reliable, responsive, and valid instrument38,39,43 that provides a score for each of eight individual attribute levels and a comprehensive overall score. The Health Utilities Index Mark 3 defines a person’s health on a scale from 0.00 (dead) to 1.00 (perfect health).
Generic Health Profile: Short Form-36
The Short Form-36 is a multipurpose health survey that measures eight domains of health. The scale provides two summary scores: a Physical Component Summary score and a Mental Component Summary score. The eight domains can vary between 0 and 100 and the summary scores are standardized to have a
mean of 50 and a standard deviation of 10.40 The scores were standardized according to the mean score of the general population.44
mean of 50 and a standard deviation of 10.40 The scores were standardized according to the mean score of the general population.44
Table 2. Instruments Used to Assess Patient-Reported Health-Related Quality of Life | ||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| ||||||||||||||||||
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree