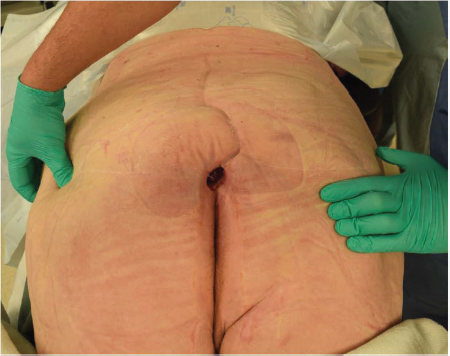
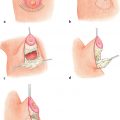
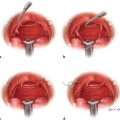
16 Pressure Ulcers Abstract This chapter will review pressure ulcers and the preoperative optimization of flap candidates in pressure ulcer reconstruction. Readers will be able to diagnose pressure ulcers and plan the preoperative optimization and surgical intervention of pressure ulcers, as well as formulate postoperative protocols. Keywords: pressure ulcer, osteomyelitis, flap surgery Six Key Points • First-line treatment for pressure ulcers is conservative management with pressure offloading and nutritional optimization. • Presence of sensation, ambulatory status, and level of spinal cord injury are considerations. • Evaluation should include assessment for previous surgery. • Presence of palpable bone is an indication of osteomyelitis. • Ischial debridement may lead to other pressure ulcers. • Recurrence rates are high; surgery does not treat underlying problem. A T11 paraplegic presents with a pressure ulcer (Fig. 16.1). 1. What do you do? The first step is to identify the location, the anatomic location of the pressure ulcer (in this case sacral), assess for previous surgery, either from known history or from visible scars, and then stage the pressure ulcer. After the pressure ulcer is staged, it is important to ascertain the circumstances surrounding the development of the pressure ulcer, and the patient involvement in a turning or moving protocol. Initial conservative steps should be taken to pack the wound with wet to moist dressing changes, turn the patient or move every 2 hours, improve nutrition, and optimize the patient’s overall medical condition with tobacco cessation, strict blood glucose control, weight loss, a bowel regimen, and spasm control. 2. What are the indications to use a negative pressure wound dressing? Negative pressure wound therapy can have the advantages of reducing the total number of weekly dressing changes and stimulating the development of granulation tissue. Contraindications include malignancy, presence of eschar or fibrinous material, exposed blood vessels or viscera, or fistulas with unknown distal drainage. 3. The patient has soilage of the pressure ulcer despite a strict bowel regimen. What do you recommend? If there is persistent soilage despite a bowel regimen, the pressure ulcer will not heal. A diverting colostomy is indicated in those instances. 4. There is exposed bone. What do you do? Exposed bone, or the ability to probe to bone, indicates the presence of osteomyelitis. The wound can still be treated conservatively until the patient is optimized for surgery. Bone biopsies can be performed to guide antibiotic therapy.
Questions
Case 1
Plastic Surgery Key
Fastest Plastic Surgery & Dermatology Insight Engine