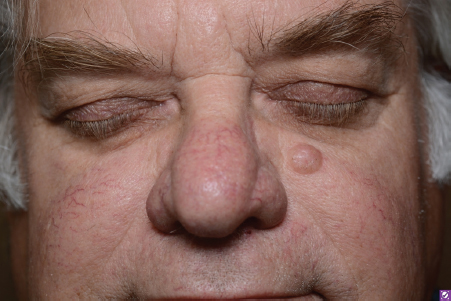
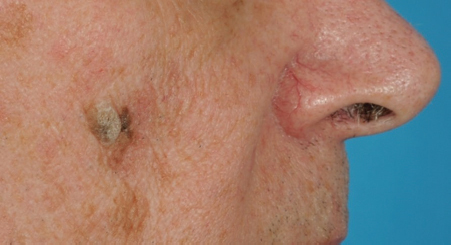
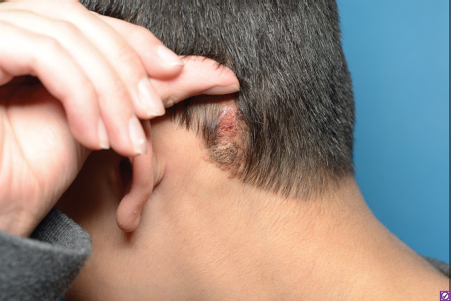
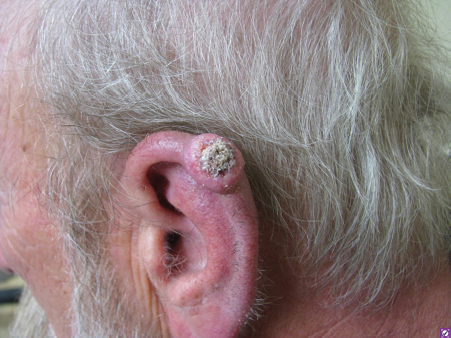
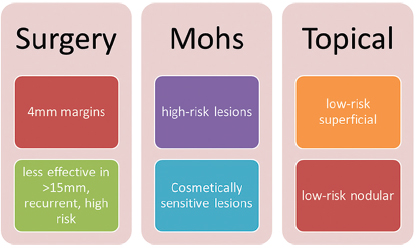
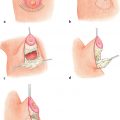
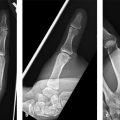
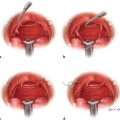
8 Skin Cancer Abstract This chapter will review the workup and management of skin cancer, including basal cell carcinoma, squamous cell carcinoma, and melanoma. The reader will develop preoperative workup plans for these cancers, describe cancer staging, and generate surgical plans for their resection, including oncologic margin control. Keywords: skin cancer, nonmelanoma skin cancer, squamous cell carcinoma, basal cell carcinoma, keratoacanthoma Six Key Points • Skin lesions need a tissue diagnosis. • Treatment of basal cell carcinoma is dependent on whether the lesion is high risk or low risk. • Skin malignancies need oncologic margins. • Complete circumferential peripheral and deep margin assessment can be used when Mohs is not available. • Melanoma must be staged. • Treatment of melanoma depends on stage. A patient has a lesion of his left cheek (Fig. 8.1). 1. What is your differential diagnosis? Skin lesions are described using the ABCDE scheme. Asymmetry, borders, color, diameter, and elevation. This provides aunified description pattern. While the differential diagnosis of all skin lesions is quite large, lesions are either benign or malignant. The most common benign lesions includeseborrheic keratosis, nevus sebaceous, epidermal nevus, and actinic keratosis. 2. How do you distinguish between the different benign skin lesions clinically? • Seborrheic keratoses: Seborrheic keratoses have a waxy, “stuck-on” appearance and have well-demarcated borders. Over time, they can develop darker brown pigment. They typically occur on the face, neck, and trunk. • Actinic keratosis: Actinic keratosis (also known as solar keratosis) has a sandpaper feel and is usually several millimeters, but can be larger (Fig. 8.2). • Nevus sebaceous: Nevus sebaceous is a hairless verrucous plaque, and occurs most commonly on the scalp and face. While malignant transformation is rare, it can occur and surgical excision of these lesions is recommended insuspicious cases (Fig. 8.3). • Epidermal Nevus: An epidermal nevus typically appears in the first year of life as a well-circumscribed plaque, most commonly on the trunk or extremities. • Melanocytic Nevi: Melanocytic nevi are pigmented and can be congenital, acquired, or atypical. They can occur anywhere on the body. 3. How should a keratoacanthoma be treated? A keratoacanthoma has a distinctive course and appearance. It is a fast-growing lesion that has an ulcerated center (Fig. 8.4). A traditional shave or punch biopsy is not recommended for a keratoacanthoma because of the difficulty in distinguishing it from squamous cell carcinoma. 4. What are the malignant skin lesions? The malignant skin lesions are subdivided into melanoma and nonmelanoma skin cancer and nonmelanoma skin cancer include basal cell carcinomas and squamous cell carcinomas. Fig. 8.4 Example of a lesion consistent with keratoacanthoma. The patient reported a history of fast growth, over the course of 2 months. Final pathology on excisional biopsy demonstrated invasive squamous cell carcinoma. 5. How do you biopsy it? While basal cell carcinomas (BCCs) and squamous cell carcinomas can have accurate diagnoses by shave biopsy, melanoma requires a punch biopsy to determine depth. An incisional biopsy allows diagnoses of BCC and squamous cell carcinoma, with the exception of a keratoacanthoma as above. 6. The diagnosis is a BCC. What do you do? Treatment for BCC is determined by the specific characteristics of a given BCC, including size, location, and histological features. Treatment options include electrodessication and curettage, topical and (less commonly) intralesional agents, photodynamic therapy, radiation therapy, Mohs surgery, and surgical excision (Fig. 8.5). 7. Describe each of these therapies. Electrodessication and curettage is used for low-risk tumors because histology is not performed and margins cannot be assessed. There are no randomized controlled trials of this technique, and recurrence rates vary from 6 to 19%1 (Fig. 8.6). Topical agents include imiquimod 5% cream, approved for treatment of low-risk superficial and nodular BCC. Topical 5-fluorouracil (5-FU; 5%) does not have randomized controlled trials proving its efficacy but is often used in low-risk, superficial BCCs. Intralesional agents including interferons, 5-FU, and bleomycin can be used. Of these, only interferons have randomized controlled trials.2 Because of lower cure rates and unknown efficacy, these therapies are used for high-risk lesions in nonsurgical candidates. Photodynamic therapy involves placement of a photosensitizing porphyrin on the lesion, followed by the application of visible light in the 40- to 450- or 630- to 635-nm range. It is used on superficial lesions. Radiation therapy is reserved for patients who cannot tolerate surgical intervention. Mohs surgery is used for high-risk lesions or lesions in cosmetically or functionally sensitive areas. It is generally not recommended for low-risk lesions or those on the trunk or extremities, because the time and expense of Mohs is not justified. Surgical excision requires oncologic margins. Because BCCs are contiguous lesions, oncological margins are simply cancer-free margins. Because of the way pathology is read, however, oncological margins require several millimeters. The majority of studies have looked at 2- to 5-mm margins, and recurrence rate for 5-mm margins is 0.4% and that for 4-mm margins is 1.6%. Features that will decrease cure rates include size of primary BCC greater than 15 mm, lesions in high-risk areas, and recurrent tumors (Fig. 8.7).
Questions
Case 1
Plastic Surgery Key
Fastest Plastic Surgery & Dermatology Insight Engine