Although disorders of pigmentation are not life-threatening, their impact can be profound. Lack of pigment or excessive pigment is quickly noticed by others and can create psychological stress for affected individuals. This is even more important during the sensitive years of adolescence, when many of these disorders begin. Depression, anxiety, embarrassment, seclusion, low self-esteem, fear of rejection, and perception of discrimination may occur in these patients. Additionally, the stigma associated with pigmentary disorders in certain cultures can cause an even greater psychological impact. Clinicians should be aware of these issues as well as the diagnosis and treatment of pigmentary disorders when treating affected patients.
Vitiligo, one of the most common pigmentary disorders, affects 0.5% to 1% of the world’s population without discrimination based on gender, age, location, or race. Women and those with darker skin may be more likely to present to medical attention. Most affected individuals develop lesions before 20 years of age and experience a progressive increase in depigmentation over time. The disease is multifactorial but ultimately results in loss of melanocytes, causing disfigurement, sun sensitivity, and severe psychosocial distress.1 For these reasons, it should be thought of as more than a purely cosmetic disorder and recognized for its real effects on patient health.
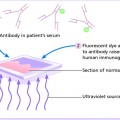
Research into the pathogenesis of vitiligo is an active field, but has not yet resulted in a clear answer. Several mechanisms have been proposed, such as genetic abnormalities, autoimmunity, and dysregulation of redox (reduction–oxidation), biochemical, and neural pathways, all of which culminate in the common endpoint of melanocyte destruction.2 Vitiligo is considered an autoimmune disease for several reasons.3 First, it is associated with other autoimmune disorders (particularly autoimmune hypothyroidism, pernicious anemia, Addison’s disease, and systemic lupus erythematosus). Second, elevated levels of autoantibodies not only directed at melanocytes, but also at other end organs (thyroid, gastric mucosa, adrenal gland, etc.) are often found in affected individuals. Additionally, cytotoxic T cells infiltrate active lesions, clearly implicating the immune response in disease activity. Interestingly, vitiligo sometimes develops in patients who successfully mount an immune response to malignant melanoma, and has even been observed following bone marrow transplantation from an affected donor.4
Controversy exists as to whether autoantibodies and immune system activation are the precipitating event or a response to melanocyte death from other causes in patients with vitiligo.5 For example, impaired handling of oxidative stress is observed in affected patients, leading to cell death. Affected skin may be more susceptible to cell loss through apoptosis and via melanocytorrhagy, which is the upward migration and loss of melanocytes through the stratum corneum due to inadequate cell adhesion.
The distribution of segmental vitiligo is in a quasi-dermatomal pattern, leading to the hypothesis that neural factors are important in the development of this form of vitiligo, a theory that is further supported by an association between vitiligo and certain neurological disorders. Genetically mediated disease susceptibility underlies each of the above mechanisms of melanocyte cell loss. Perhaps not coincidentally, the genes known to play a role in disease expression (PTPN22, NALP1, and certain HLA genes) are also functional components of the immune system, linking the genetic and autoimmune theories of pathogenesis. As with many disorders, it is likely that no single pathway is solely responsible but that multiple pathogenic mechanisms overlap to manifest disease in patients with vitiligo.6
Initial onset may be sudden, but the patient will usually report slow, progressive expansion of white spots on the skin without associated symptoms. A personal history of autoimmune disease or family history of vitiligo may be present. Sun exposure or trauma may draw attention to the lesions, causing the patient to seek medical attention. Subjectively, the patient may express emotional distress over the conspicuous and disfiguring lesions.
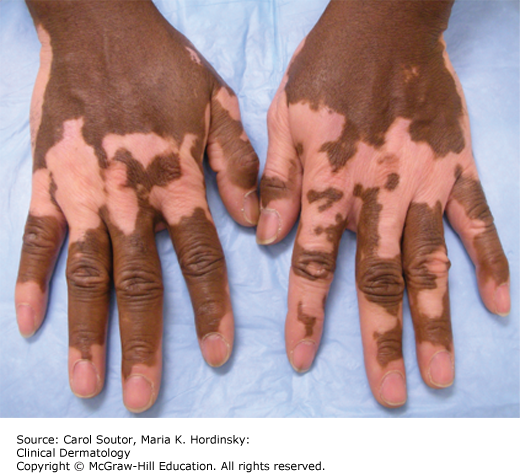
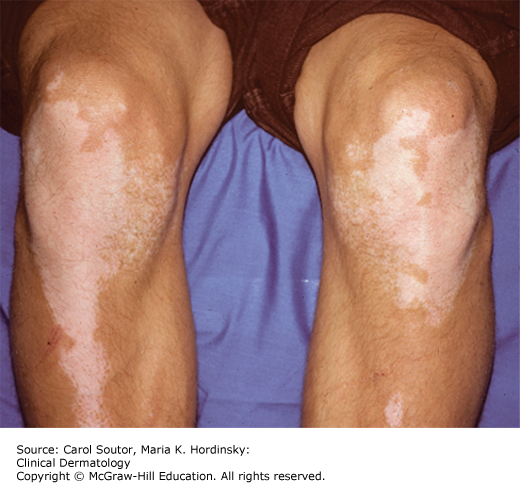
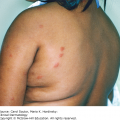
Stark white, well-demarcated macules of varying sizes are noted in five possible patterns.
Generalized-bilaterally symmetrical macules on face, trunk, and extremities (Figures 21-1 and 21-2).
Segmental pattern: Affecting one site or one side of the body.
Acrofacial: Affecting the lips, perioral areas, hands, and feet.
Universal: Involving over 50% of the body surface area over a wide distribution.
Mixed pattern: A combination of generalized, segmental, or acrofacial patterns.
The macules are nonscaling and accentuate with Wood’s lamp examination. Lesions are often symmetric but may occur anywhere with a peculiar predilection for circumferential involvement of orifices, face and upper chest, and sites of pressure. Hair and mucous membranes may also be affected. Only rarely are borders erythematous or hyperpigmented.
No abnormalities are seen in routine laboratory studies; however, patients may have evidence of thyroid abnormalities or other autoimmune diseases. Histologically, vitiligo is characterized by the absence of melanocytes in affected skin, although degenerating melanocytes may be seen in lesional borders. Conversely, normal melanocytes are seen in clinically nonaffected skin, but keratinocytes may appear abnormal, with extracellular granular material and vacuolated cytoplasm in the basal layer.
Diagnosis is clinical, based on the appearance and distribution of the lesions, chronic and progressive involvement, lack of associated symptoms, and exclusion of vitiligo mimics.
✓ Tinea versicolor: May be differentiated by the presence of fine scale, positive potassium hydroxide (KOH) preparation, and distribution primarily on the trunk and neck.
✓ Pityriasis alba: A relatively common condition in children with atopy; also may have fine scale, but lesions retain some pigment and are less sharply demarcated.
✓ Postinflammatory hypopigmentation: A history of trauma or inflammation of the affected area will precede the loss of pigment.
✓ Guttate hypomelanosis: Presents with hypopigmented macules in a photodistribution on a background of actinic damage primarily on the arms and legs; unlike vitiligo, the macules are usually 5 mm in diameter or less.
✓ Chemical leukoderma: Certain chemicals, particularly aromatic derivatives of phenols and catechols, can destroy melanocytes, resulting in chemical leukoderma that may be differentiated from vitiligo by the history of toxin exposure, lesions with bizarre borders and scale, a “confetti-like” distribution, and symptomatic pruritus.
✓ Ash leaf spots of tuberous sclerosis: Accompanied by angiofibromas, periungual fibromas, connective tissue nevi, and possibly neurological sequelae.
✓ Other: Sarcoidosis, Hansen’s disease, and mycosis fungoides (cutaneous T-cell lymphoma) may present with white macules and should be considered in the appropriate clinical setting, requiring a skin biopsy to make the correct diagnosis.
The rate of spontaneous repigmentation is as high as 20%,1 but is usually incomplete. Treatment is almost always undertaken due to the often progressive course and significant psychosocial burden of disease.7 The most important aspect of treatment is establishing realistic expectations with the patient in terms of the aesthetic outcome anticipated and the need for prolonged treatment.
A multifaceted approach is used based on the varied mechanisms contributing to vitiligo. Immunosuppression quiets the autoimmune contribution and stimulation of melanin production counteracts the progressive loss of melanocytes. Both of these ends are accomplished with psoralen plus ultraviolet (UV) A photochemotherapy and UV B phototherapy. Topical corticosteroids, calcineurin inhibitors (pimecrolimus cream, tacrolimus ointment), and vitamin D3 supplementation may improve vitiligo by affecting the immune system locally. Light therapy commonly causes itching, dry skin, and sometimes perilesional hyperpigmentation. There is also a low, albeit concerning, risk of iatrogenic skin cancer in patients with excessive UV doses. Topical or systemic steroids are sometimes used in combination with phototherapy. Caution must be exercised to avoid the many side effects of chronic steroid use. Oral antioxidants such as vitamins C and E may be useful adjuncts to minimize oxidative damage from free radicals present in lesional skin. The excimer laser is a new form of narrow band UVB treatment with the ability to treat localized areas without affecting normal skin. Finally, several surgical techniques for autologous transplantation (such as punch-grafting, split-thickness grafting, and epidermal blister grafts) have been employed with good to excellent success in patients resistant to other medical therapies. Donor site cells may even be cultured to allow treatment of more extensively affected regions. Again, a combination of medical and surgical therapy is often used to maximize repigmentation.
Aside from influencing disease activity, specialized makeup may be surprisingly effective in evening skin tone. Cosmetic tattooing is usually limited to specific areas, such as the lips. The opposite approach is sometimes taken for extensive disease involving more than 50% of the body surface area by depigmenting normal skin to attain the goal of homogenous skin coloration. In addition to vigilant sunscreen use, meticulous search for skin cancers is required, as the depigmented skin is prone to the deleterious effects of sun damage. Concomitant autoimmune disorders should be sought with thyroid studies, screening for antinuclear and other organ-specific antibodies, and hematologic evaluation.
Information on support groups should be offered to patients with vitiligo due to the potential for significant psychosocial effects and negative impact on quality of life associated with this condition.7 A patient’s perceived quality of life impacts treatment response, regardless of modality used, and must be addressed in order to achieve treatment success. In addition, vitiligo patients suffer an increased rate of psychiatric comorbidity, and when necessary, appropriate psychiatric referral should be given.
When patients are not responding to topical therapy, they should be referred to a center experienced in phototherapy or even to a specialty center skilled at surgical therapy for vitiligo.
The National Vitiligo Foundation offers educational materials, reports clinical trials and research updates, and support groups on the website: www.nvfi.org
Vitiligo Support International provides disease information, discussion forums, and public advocacy accessible at: www.vitiligosupport.org
The American Vitiligo Research Foundation strives to increased public awareness by focusing on affected children and supporting humane research initiatives: www.avrf.org