Introduction
The upper aerodigestive (UAD) tract is an intricate maze of alleyways, muscular tubes, and cords that allows humans to have a common functional pathway for oral intake and breathing, as well as harmonizing vibrations into speech. Articulation of speech is dependent on the symphony of functions of these passages, influenced by the larynx, epiglottis, pharyngeal walls, soft and hard palate, the tongue musculature, salivation, lip seal or oral competence and dentition as a tightly ordered orchestra. Many of these functional elements involve the pharynx. The posterior reaches and ramifications of the UAD tract coalesce into a continuous 15 cm-long muscular collecting tube, the pharynx, which begins in continuity with the nasopharynx superiorly and connects to the esophagus inferiorly. It extends from the skull base to the esophagus and comprises three parts: upper or nasopharynx behind the nose, middle or oropharynx behind the mouth, and lower or hypo- or laryngopharynx behind the epiglottis and larynx.
Pathology
Pharyngeal cancers are predominately squamous cell carcinoma (SCC) and are of two types: HPV+ related to human papilloma virus (better prognosis) and HPV− usually linked to alcohol and tobacco. Risk factors include alcohol and tobacco, exposure to Epstein–Barr virus, and Chinese ethnicity, especially for nasopharyngeal carcinoma. Organ preservation has become the main aim in the management of UAD tract malignancy. Fortunately, early stage disease can be effectively treated conservatively with radiotherapy or chemoradiation combination so that function can largely be preserved. Given the morbidity of surgery in this most sophisticated functional zone, its place is increasingly reserved for advanced stage disease or in salvage treatment after failure of nonsurgical protocols. Sadly, most patients present at advanced stages and are associated with poor overall survival. Between 70% and 85% have stage 3 or stage 4 disease at presentation and 5-year survivals are reported around 15%–35%. The reality is that most surgery is palliative and although the prime focus here is inevitably on removal of the cancer and reduction in the risk of local recurrence, the overall focus must be on the quality of survival. By contrast, nasopharyngeal cancers have a better prognosis as they are mostly responsive to radiotherapy and rarely require surgical resection or reconstruction.
Anatomy
The nasopharynx is open to the nasal cavities anteriorly and extends from the base of the skull superiorly to the upper surface of the soft pallet where it becomes the oropharynx. The oropharynx communicates with the mouth anteriorly and includes the soft palate, the tonsils, and the tongue base posterior to the circumvallate papillae. The oropharyngeal tube extends from the soft palate above to the hyoid below. The hypopharynx is continuous below the oropharynx, extending from the level of the hyoid bone to the esophageal inlet. The larynx lies in close anterior proximity. The thyrohyoid membrane through which the internal branch of the superior laryngeal nerve gains access to the larynx is located superolaterally. The detailed anatomy of the UAD tract can be found in specialized texts. Anatomically, the area has a rich lymphatic drainage to the jugular chains as well as the retropharyngeal nodes and the node of Rouvière, with frequent crossing of the midline. The pharyngeal muscular tube, which spans from the base of the skull to the C6 vertebra, comprises circular fibers that form constrictions to propel contents into the esophagus and longitudinal fibers that lift the walls of the pharynx during swallowing.
Indications for Surgery and Reconstruction
Most commonly, major UAD tract defects result from surgical ablation of malignancies. It is accepted that radiotherapy is just as effective as surgery for eradication of early disease, and because radiotherapy is less destructive to function, it is the preferred modality of treatment. Surgery is therefore reserved for advanced stage or recurrent cancers and will be inevitably destructive. The principles of wide oncological resection, the proximity of the vital structures and the protection of the upper airway patency, speech, and deglutition dictate the indications for reconstruction of any significant UAD tract defects. Many pharyngectomies for advanced disease are associated with combined laryngectomy. Thus most advanced neoplasms involving the oropharynx, hypopharynx or cervical esophagus will result in a pharyngeal defect requiring reconstruction.
Classification of Pharyngeal Defects
A useful classification of pharyngeal defects was previously devised by Disa et al, however, this classification did not specify whether the defect involved the larynx or the base of the tongue. More recently, Urken et al, proposed a new classification scheme that addresses this issue:
- •
Type 0: minimal defects of the pharyngoesophageal segment that are amenable to primary closure
- •
Type I: non-circumferential defect with a presence of a viable strip of mucosa, measuring a minimum of 2 cm in width
- •
Type II: circumferential defect extended no further cephalad than the level of the vallecula
- •
Type III: circumferential or noncircumferential defect extended cephalad to the level of the vallecula
- •
Type IV: any resection that extends caudal to the level of the clavicles.
Historical Perspectives
The first attempts at pharyngoesophageal reconstruction date back to the nineteenth century. These proved notoriously unreliable, with chronic aspiration, hemorrhage, and early death in the postoperative course, followed by stricture formation in those who survived the immediate aftermath of the surgery. This led to a loss of enthusiasm for reconstruction until Wookey rekindled interest in 1948 with a random pattern anterior neck skin flap to reestablish the UAD tract. His two-stage reconstruction included using the cervical skin raised as a random flap sutured to the upper and lower ends of the defect, but left open anteriorly thereby exteriorizing the pharynx and esophagus. The sulcus thus created was closed 5 weeks later at a second-stage operation. The next surgical leap came when Bakamjian described the more reliable axial deltopectoral flap, based medially on what has subsequently been shown to be the upper second and third internal thoracic artery perforating branches. It was, however, still a two- or three-stage treatment and was not uniformly reliable.
In 1979, Ariyan’s description of a tubed myocutaneous pectoralis major flap finally made possible a single‐stage ablative reconstruction with a more predictable outcome. Subsequently, both the trapezius and latissimus dorsi myocutaneous flaps were described as alternatives for a single‐stage reconstruction, but not surprisingly did not achieve significant popularity.
Parallel with these skin tube developments, more reliable pedicled interposition gastrointestinal reconstructions were being attempted as far back as the 1930s; their primary role, however, was in total esophagectomies. Adaptation of the Ivor–Lewis gastric pull-up to the cervical esophagus and pharynx was one such procedure, which has survived as a mostly reliable option into the modern era. In addition to the gastric pull-up, the spectrum of these pedicled flap reconstructions included the left colon and the seldom used pedicled jejunum.
In 1959, Seidenberg reported the first successful harvesting and transferring of a jejunal free flap using microsurgical techniques, reportedly with threaded 6‐0 silk sutures under loupes magnification. His patient died 5 days postoperatively from a massive cerebrovascular accident, but the first successful human free flap was found to be viable at the time. The following year Hiebert and Cummings Jr performed an uneventful gastro-antral free graft joining 2 mm-diameter gastroepiploic vessels to the superior thyroid artery end to side and facial vein end-to-end. They noted the report of Jacobson and Suarez, the acknowledged founders of microvascular technique that occurred subsequent to their procedure, recommending using a microscope. These feats were performed at least a decade before the tidal wave of microsurgery began, with the works of Buncke et al, Daniel and Taylor, and O’Brien et al, and others who used other tissues, including omentum and skin. Soon, microsurgical free tissue transfer was to become a first-line mainstream reconstructive option.
Microvascular technique brought with it the promise of a reconstruction not bound by restraints of pedicle length or random proportions. The reliability of an axial flap transfer into the defect revolutionized the approach to major reconstructive challenges. Gastro-omental, gastric antral, ileocolic as well as colon free flaps have been described; however by far the most common visceral reconstruction is a free jejunal reconstruction. The earliest significant clinical series of microsurgical jejunal reconstructions were those reported by Jurkiewicz. But his daring and technical skill were not widely adopted for almost a further 20 years. The free jejunal flap, whether as a tube or patch, has since become one of the two most reliable reconstructive tools for laryngopharyngectomy and/or cervical esophagus reconstruction.
Tubed or patch fasciocutaneous flaps are the other main alternative reconstructive options for pharyngeal defects. The most common flaps used are the anterolateral thigh and radial forearm flaps.
Assessment and Planning
As with any operative surgery, planning remains the most important step in execution of the technique. This is best considered as part of a regular multidisciplinary (MDT) meeting, which includes, in addition to head and neck, oral maxillofacial and plastic surgeons, radiation oncologists, medical oncologists, pathologists, speech therapists, dieticians, physiotherapists, and social workers, as well as a radiologist specializing in head and neck malignancies. An estimation of the extent of the defect and the need for reconstruction is discussed at these meetings. The reconstructive team, in conjunction with the ablative team, can decide on the best reconstructive option and begin planning for surgery after assessment of all possible donor sites. Previous history of laparotomy and upper GI surgery is noted and the patient’s forearms and thighs are assessed.
A decision is also made at these multidisciplinary meetings in relation to the need for perioperative radiotherapy and preoperative dental surgery, as well as nutritional needs. Most, if not all, patients requiring major reconstruction have either advanced disease or chemoradiation failure for relatively advanced disease and suffer from malnutrition. The need for nutritional supplementation is almost universal, including during the radiation therapy period. This may require percutaneous endoscopic gastric (PEG) tube insertion, depending on the surgical unit. Nutritional status will influence wound healing and reduce fistula formation. Uncomplicated healing streamlines the programming of radiation therapy in the shortest time window possible for the best therapeutic outcome.
Reconstruction
The broad principles of pharyngeal reconstruction are:
- •
maintaining or recreating a patent airway and protection from aspiration;
- •
reestablishing the integrity of the pharyngeal pathway to allow swallowing and adequate caloric intake; and
- •
voice and speech rehabilitation.
All of these endeavors have in common the creation of a patent tube. Salvage of all these functions is possible to various extents. The advent of microsurgery has made possible transfer of large amounts of tissue sculpted to more or less reconstruct the created defect. In addition, introduction of tissues with a new vascular supply into settings of advanced disease requiring major resections and radiotherapy or following chemoradiation failure, promotes better wound healing and discourages fistula formation.
The two key determinants that influence the nature of the reconstruction are the surgery (i.e., the defect created as well as donor availabilities) and the patient’s general status. Many of these patients have life-long history of heavy smoking and drinking, with the attendant risk of cardiac or respiratory disease and malnourishment. These are all factors to be considered in the light of the length of surgery and the added morbidity from choice of donor sites. The added burden of a laparotomy or a chest flap on the respiratory reserves, the speed of skin flaps versus bowel in patients with poor cardiac reserve or malnourishment, and the benefits of donor sites that allow simultaneous access during the primary resection for two-team surgery are issues to ponder. Preoperative anesthetic, respiratory, and cardiac assessment is mandatory. Any reasonable optimization of the patient’s status should be undertaken prior to surgery.
All patients require confirmation of continuity and integrity of the UAD tract at 7–10 days postoperatively, with a contrast study before removal of nasogastric tubes and resumption of oral intake.
Reconstructive Options
Local Flaps
In practical terms, these include surrounding cervical skin and soft tissue and they rarely provide a practical reconstructive option for major defects. Not only is the neck skin vasculature unreliable, especially after flap elevation and block dissection, but it is generally sacrosanct to ensure cover of vital structures such as the carotid vessels. Frequently, the neck skin has been or will be irradiated. The generalized devascularization associated with the treatment modalities greatly favors the importation of new, independently vascularized tissue, either from a regional source or more commonly now as a free flap transfer. Recently, the supraclavicular flap based on the transverse cervical vessels including a deltoid skin extension has been successfully used in lower level pharyngeal reconstructions.
Regional Flaps
Aside from the pectoralis major flap, other pedicled flaps described include gastric pull-up flap, the myocutaneous latissimus dorsi and trapezius flaps, as well as the traditional fasciocutaneous deltopectoral or its modification the internal mammary artery perforator (IMAP) flap. This is essentially a paramedian vertically oriented propeller flap based on the second or second and third internal mammary perforators. It can be rotated 180° and employed for some hypopharyngeal reconstructions.
Pectoralis Major
This type V Mathes and Nahai myocutaneous flap remains one of the most reliable reconstructive options for the head and neck. With the advent of microsurgical reconstructions it has been increasingly relegated to a second choice or salvage reconstructive option. Some of the current indications for its use include:
- •
situations where general patient state and systemic disease dictate reduced operative time
- •
in combination with another flap or alone, where an external skin defect is present or has evolved after primary surgery
- •
in coverage and protection of major neck vessels
- •
in closure of pharyngostome
- •
wound dehiscence.
This flap is based on the pectoral branch of the acromiothoracic axis. It is most commonly raised as a myocutaneous flap with its skin island placed medially in women to reduce breast tissue inclusion. The skin component is rolled to form a tube to reconstruct circumferential defects. In order to avoid traction on the vascular pedicle a 3-cm cuff of muscle should be retained at the clavicular origin where possible. A so-called defensive incision for accessing the muscle without violating the potential deltopectoral salvage flap is made and the flap is raised and, where possible, tunneled through the neck into the defect. For partial defects the skin island can be designed as a patch and sutured into the remnant pharyngeal mucosa. Anchoring the remnant pharynx and cervical esophagus to the prevertebral fascia, interdigitating the lower flap inset with the esophagus, and de-epithelialization of the leading skin edge have also been described as means of reducing stricture and fistula formation. Others have advocated removal of the skin island and using only the myofascial component of the flap for repair to reduce bulk and to discard the least vascularized tissue component. Table 26.1 lists published outcome studies specific to pharyngeal reconstructions. Increased flap complication rates are reported with hypopharyngeal reconstructions, female patients, previous radiation therapy, obesity, patients >70 years old, and preoperative malnutrition (albumin <4.0 g/dL).
| Defect | No. of Patients | Successful Swallowing | Stricture (%) | Fistula Leak (%) | Flap Failure (%) | Medical Complication (%) | Immediate Mortality (%) | Patient Received Voice Prosthesis (%) | Functional Outcome (%) | ||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Pectoralis Major | |||||||||||
| Chan et al | Pharyngeal (circumferential) | 92 | 100 | 27.2 | 23.9 | 35.8 | |||||
| Clark et al | Hypopharyngeal | 68 | 81 | 12 | 35 | 15 | 3 | 44 | 100 | ||
| Chan et al | Hypopharyngeal | 30 | 100 | 26.7 | 0 | ||||||
| Espitalier et al | Hypopharyngeal | 41 | 39 | 22 | 2.5 | 0 | 2 | 100 | |||
| Cervical | |||||||||||
| Esophageal | |||||||||||
| Spriano et al | Hypopharyngeal | 37 | 0 | 13 | 0 | 10 | 3 | 24 | 100 | ||
| Saussez et al | Hypopharyngeal | 12 | 17 | 33 | 0 | 0 | 0 | 50 | 83 | ||
| Leite et al | Oropharyngeal and hypopharyngeal | 84 | 31 | 2 | |||||||
| Pectoralis Major + Trapezius + Sternocleidomastoid | |||||||||||
| Carlson et al | Cervical | 45 | 27 | 78 | 2 | 0 | 0 | ||||
| Esophageal | |||||||||||
| Hypopharyngeal | |||||||||||
| Range | 0–39 | 0–78 | 0–2.5 | 0–15 | 0–3 | 24–50 | 35.8–100 | ||||
Flap bulk often precludes meaningful voice rehabilitation using a tracheoesophageal puncture (TEP). In addition, recurrent descent and obstruction of the stoma may require surgical revisions.
Free Flaps
The most common arterial recipient vessel is the superior thyroid or facial and the most common veins are the internal and external jugular or facial veins. Free flap reconstructions are broadly divided into two groups: the visceral free flaps , the commonest being the jejunal transfer, and fasciocutaneous free flaps , from the radial forearm and anterolateral thigh.
Free Jejunum
For obvious reasons, jejunum is an ideal reconstructive option for pharyngeal and upper esophageal reconstructions. Previous laparotomy, although not absolute, is a relative contraindication to its use. Patients with minimal respiratory reserve should be considered with caution, given the additional morbidity of a laparotomy. A segment of proximal jejunum up to 25 cm length can be transferred as a free flap. The luminal diameter of the jejunal flap ranges between 3 and 5 cm. Despite its advantages, this flap has several technical shortcomings.
- •
It is exquisitely sensitive to hypoxia; any hypoxia beyond 3 hours will almost always result in flap death and subsequent potentially catastrophic fistula formations.
- •
The vein is particularly thin and will not tolerate traction.
- •
The pedicle remains relatively short in comparison to its fasciocutaneous counterparts; the average length is described as 4–6 cm, with a maximum length of 10 cm based on superior mesenteric vascular axis.
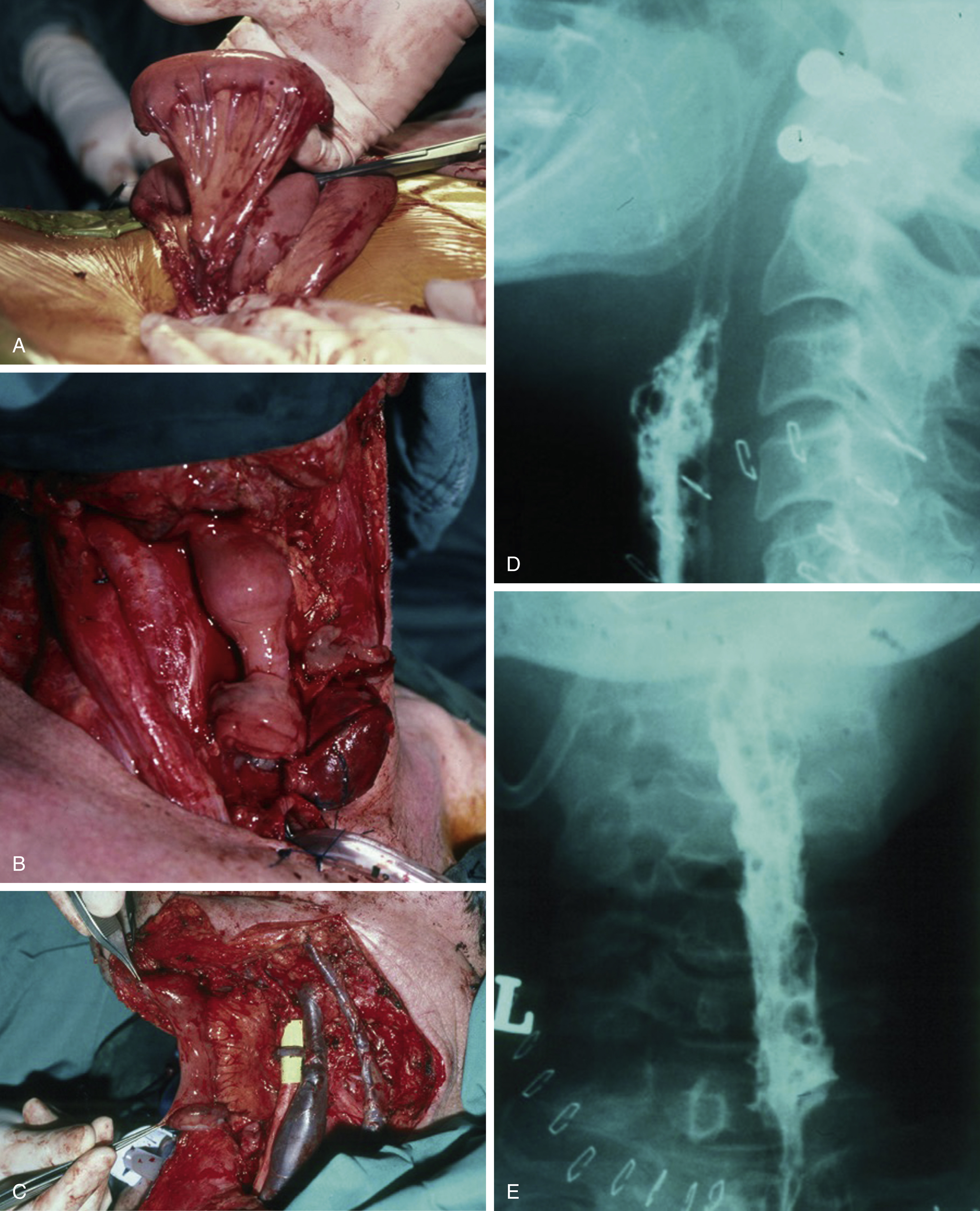
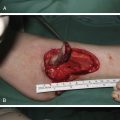
An isolated segment of jejunum is measured under mild stretch to the length of the defect and is transferred in an isoperistaltic orientation. The loop is chosen as proximal to the duodenum as is feasible because here the mesenteric vessels are longest. The oropharyngeal inset can be technically difficult, not least due to usual size discrepancies. Either a slit in the antimesenteric border or closing suture of the oropharyngeal remnant may be used to readjust for size mismatches. Island jejunal patches based on the same vascular arcade can be reoriented and inset into a split in the upper end of the tube to accommodate wide oropharyngeal discrepancies. A nasogastric tube is passed through the jejunal segment, and the tube length is adjusted and anchored at either end, such that the pedicle trails without tension into the recipient vessel site field. Definitive repair of each end awaits microvascular anastomosis so as to reduce ischemic time. The lower inset is performed last. All bowel anastomoses are done using interrupted sutures rather than staples or continuous sutures. Any significant redundancy in bowel length will increase the postoperative swallowing difficulties and a common error is to design the segment too long. A survey of the reported outcomes in the literature, outlined in the next section, supports its reliability and low complication rate ( Fig. 26.1 ).