Self-Declared Sensitive Skin Overall
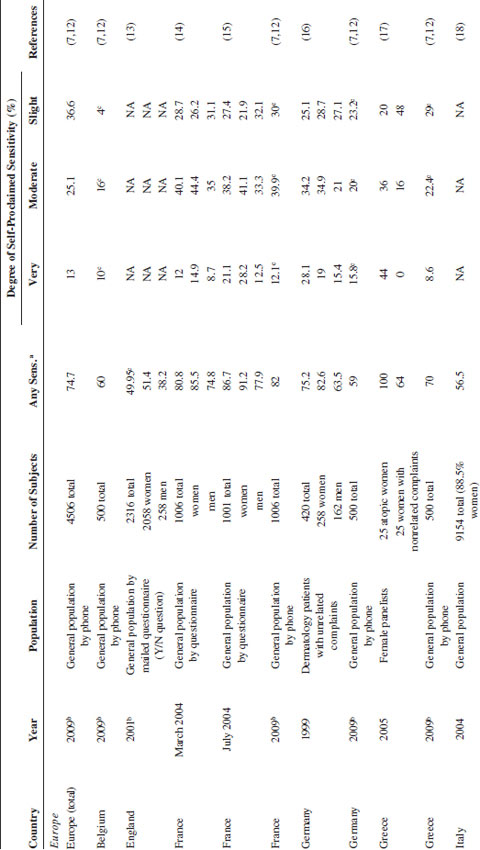
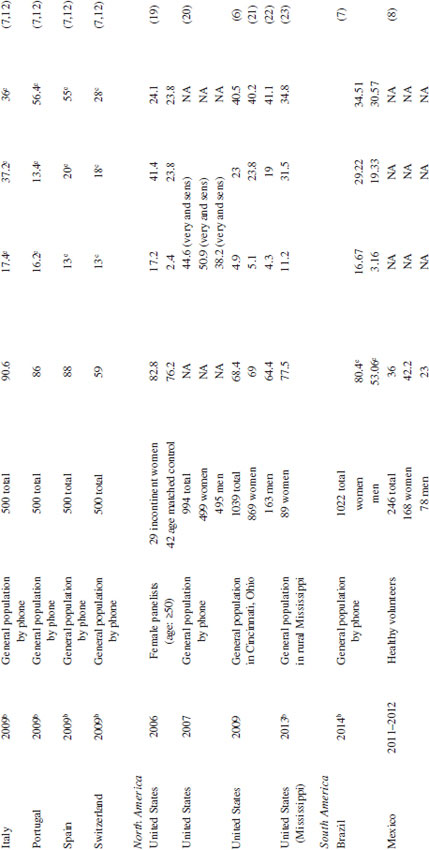

Note: NA: not available.
a Any sensitivity, for example, very, moderate, or slight.
b If year of study is not given, the date corresponds to the year of publication.
c Percentages are not reported but interpreted from other data in publication.
Differing cultural practices may produce widely different exposures to potential irritants and, therefore, to perceptions of sensitive skin. Women are more likely to use cosmetic products on the face and, therefore, more likely to experience unpleasant sensory effects as a result. Similarly, in most countries women are more frequently exposed to household cleaners and products compared to men and, as a result, have more opportunities to experience reactions to these products. Hygiene practices and the use of feminine products, such as douches, perfumes, medications, antifungal medications, and contraceptives, are a common cause of vulvar irritation in women (24). These practices can vary between different countries or between socioeconomic groups within countries (25). Based on the differing uses of these products, older women are more likely to report irritation due to incontinence products, whereas younger women are more likely to report irritation due to tampons (26). These findings are almost certainly based on culturally driven levels of exposure rather than on actual physiological differences.
There is no consensus on a classification for sensitive skin; however, several have been proposed (27). A number of these include consideration of objective signs of irritation, such as inflammation, or visible dermatological disorders. Since the etiology of sensitive skin and its association with frank skin inflammation or underlying dermatological disease is still not well understood, Misery (27) has proposed classifying sensitive skin according to severity, that is, very sensitive, sensitive, slightly sensitive, and nonsensitive.
Physiological and External Factors That Contribute to Sensitive Skin
The etiology of sensitive skin is unknown, but the disorder is believed to be related to a number of intrinsic physiological characteristics and other causes (Table 17.2), including alterations in skin barrier function, neurosensory function, and other host and external factors (3,28–30).
TABLE 17.2
Possible Contributing Factors to Sensitive Skin
Factor | References |
Alterations in Barrier Function | |
Thin SC | |
Decreased hydration of SC | |
Disruption of SC | (38) |
Increased sweat glands | (32) |
Increase neutral lipids and decreased sphingolipids | (39) |
Decreased lipids | |
High-baseline TEWL | (45) |
Neurosensory Function | |
Increased epidermal innervations | |
Other Host Factors | |
Fair skin | (13) |
Susceptibility to blushing and/or flushing | (13) |
Atopy and other skin conditions | |
Female sex | |
Hormonal status | (48) |
External Factors | |
Cultural expectations in technologically advanced countries | (16) |
Barrier Function
Poor barrier function can result in abnormal penetration of potentially irritating substances and a decrease in the skin tolerance threshold (35). A number of early studies have suggested a link between sensitive skin and alterations in barrier function (49). Berardesca et al. (50) studied hyperreactors to nicotinate and concluded that they may have a thinner SC with a reduced corneocyte area resulting in a higher transcutaneous penetration of water-soluble chemicals. Seidenari et al. (40) concluded that alterations of baseline capacitance values indicates a tendency to barrier impairment and supported the view that skin hyperreactivity to water-soluble irritants is induced by the absorption of greater amounts of irritants. Corneosurfametry data were used by Goffin et al. (51) to demonstrate significant differences in SC reactivity between individuals with sensitive or nonsensitive skin. However, increased absorption is not the only explanation for sensitive skin. Cho et al. (52) evaluated individuals classified into sensitive skin and nonsensitive skin based on a LAST performed on the face. These investigators demonstrated no differences in TEWL as a measure of barrier function, but a significant difference in the mean quantity of SC ceramides, which were significantly lower in the sensitive skin group compared to the nonsensitive group. In a series of studies on individuals with sensitive skin, Roussaki-Schulze et al. (53) concluded that patients with sensitive skin had significantly lower levels of sebum and hydration than nonsensitive individuals. In addition, individuals with sensitive skin were more likely to develop alkali resistance and had significantly higher hyperreactivity of blood vessels in response to the application of methyl nicotinate.
Barrier function requires a well-organized, multilayered lipid structure between corneocytes (29). Further, the barrier properties of the SC are dependent on the precise lipid composition. Regions with higher neutral lipids and lower sphingolipids are associated with superior barrier properties (39,54). A weak barrier would not only facilitate the penetration of potentially irritating substances, but may also inadequately protect nerve endings resulting in hyperreactivity.
Neurosensory Function
The pain and other unpleasant sensations that are the hallmark of sensitive skin imply a likely relationship to neurosensory dysfunction, probably involving several neuromediators and sensory receptors. Possible mechanisms for neural system hyperreactivity include nerve fibers; endothelin receptors; burn, itch, and heat receptors; cold receptors; and neutrophins (55). Dermal nerve fibers extend throughout viable epidermis as free nerve endings, but the epidermal component of this network is still poorly characterized (46).
Besne et al. (56) evaluated epidermal innervation of biopsy samples from different anatomical sites; two facial sites (upper eyelid and preauricular area), the abdomen, and the mammary area. The innervation of the facial areas was significantly higher than the other anatomical sites. With increasing age, the dermal innervation of the facial sites decreased, while it increased in the mammary skin and was unchanged on the abdominal skin. These authors proposed that epidermal nerve density variation could explain the different sensitivity thresholds in various anatomical sites.
Skin sensations such as itching, pain, and warmth are mediated by unmyelinated C fibers (29,57). Kim et al. (58) evaluated C fiber measurements at 5 Hz electric current stimulation in a study on a small number of young adult male volunteers. The individuals prone to sensitive skin showed a tendency toward a decreased sensory perception threshold compared with the individuals who were not prone to sensitive skin.
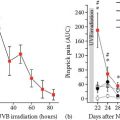
Querleux et al. (59) used lactic acid to induce slight painful stimulation and a feeling of discomfort while monitoring brain activity using fMRI. The test was performed on nine subjects with self-declared sensitive skin and nine subjects with nonsensitive skin. During the study, the individuals with sensitive skin had a higher level of declared discomfort as a result of lactic acid application compared to the individuals with nonsensitive skin. Brain activity recording using the fMRI showed striking differences between the two groups. In the nonsensitive individuals, activity was concentrated in the left primary sensorimotor area, contralateral to the side of application of the lactic acid. By contrast, in the sensitive skin group, the discomfort-related activity was found in the sensorimotor cortex in both hemispheres. In addition, in the sensitive group only, specific discomfort-related activity was observed in the bilateral peri-insular regions classically considered as secondary the somatosensory area. This study indicated that subjects with sensitive skin have a specific CNS response during a LAST and suggests that the excitability of sensitive nerves in the facial epidermis lead to brain activation very similar to those observed in the pain process.
Other Contributing Causes
Individuals with fair skin are more likely to have skin sensitivity. Willis et al. (13) found that individuals susceptible to blushing were more likely to have sensitive skin, as were individuals with atopy or other skin conditions such as rosacea and acne. A similar observation was reported by Kamide et al. (9) based on a survey conducted among 1500 individuals in Japan. Sensitive skin was more likely to be declared by individuals who flush easily and are susceptible to sunburn. In contrast, Jourdain et al. (60) conducted a survey among 811 women in the San Francisco area in 1998 and found no significant differences between the incidence of sensitive skin among ethnic groups (i.e., African Americans, Asians, Euro-Americans, and Hispanics).
There appears to be an association between perceived sensitive skin and AD. In a study conducted in 2005 in a dermatology clinic in Greece, Farage et al. (17) surveyed 25 women diagnosed with AD and 25 women with unrelated complaints. All patients in the group with AD described their skin as sensitive to some degree, with 80% claiming their skin was either very or moderately sensitive (44% and 36%, respectively). The remaining 20% described their skin as slightly sensitive. By contrast, 64% of the individuals in the control group described their skin as sensitive to some degree, with none of the patients claiming to have very sensitive skin, and only 16% of the subjects claim that their skin was moderately sensitive. The association between the clinical diagnosis of AD and self-declared sensitive skin was statistically significant (P < .0001). Misery et al. (12) conducted a study in eight European countries and reported that a history of childhood AD was more frequent among individuals with sensitive or very sensitive skin compared to individuals with slight or nonsensitive skin. In contrast, in a 2001 publication, Willis et al. (13) found no association between the incidence of self-perceived sensitive skin when atopic subjects were compared to nonatopics (49% and 51%, respectively).
Gender plays a role in the perception of sensitive skin. Generally, the proportion of women who claim sensitive skin is cited as 50–70%; and the proportion of men, 30–60% (21). In a study conducted among 420 volunteer subjects (162 men and 258 women), Loffler et al. (16) reported a higher proportion of women claiming some degree of skin sensitivity (moderate, strong, or severe) compared to men (82.6% and 63.6%, respectively). In a study conducted in the United Kingdom among 3300 women and 500 men, Willis et al. (13) reported an incidence of perceived sensitive skin of 51.4% among women and 38.2% among men.
Misery et al. (15) conducted a study to compare perceptions of sensitive skin in summer versus winter. A higher percentage of women claimed to have very sensitive skin in both seasons, and a higher percentage of men declared that their skin was slightly or nonsensitive. In a study conducted in eight countries in Europe, investigators reported that a higher proportion of women declared sensitive skin compared to men (49.4% and 37%, respectively; P < .05) (16). In studies reported by Farage (21), there was no significant difference between genders when all degrees of general skin sensitivity were considered. However, women consistently reported a higher proportion of very and moderately sensitive skin. Men reported a higher proportion of slightly sensitive skin.
The gender difference in the perception of sensitive skin may be due to a variety of factors. Men’s and women’s skin differs in a number of physiological parameters, including skin thickness, hormone metabolism, hair growth, sweat rate, sebum production, surface pH, fat, and collagen content (28). Women tend to be exposed to a wider variety of cosmetics and household products, creating more opportunities to experience the sensations associated with sensitive skin. Further, perhaps it has been more culturally acceptable for women to claim sensitivity compared to men, although with the growth in the popularity of men’s products formulated for sensitive skin, this may cease to be the case in the modern consumer world.
Interestingly, skin barrier function and reactivity to some irritants exhibit a cyclical variability in women that demonstrates hormonal influences in sensitive skin (61). Harvell et al. (62) investigated water barrier function on the back and forearm and found that the TEWL value was significantly higher on the day of minimal estrogen/progesterone secretion compared to the day of maximal estrogen secretion. This suggests that the skin barrier function is less complete on the days just prior to the onset of the menses compared to the days just prior to ovulation. In women, the forearm skin exhibited stronger reactions to SLS on day 1 than during days 9–11 of the menstrual cycle, while no difference was detected in a male control group evaluated during the same time period (63).
A number of test methods have been developed to objectively identify individuals with sensitive skin. A few examples are listed in Table 17.3. Some of these methods evaluate sensory responses such as stinging in response to the application of lactic acid (64) or capsaicin (55) or irritant reactions to materials such as SLS (65). However, there is a great deal of interpersonal variability in individual responses to specific irritants (3,54,66), even among chemicals with similar modes of action (67). Reactivity to one chemical is not necessarily predictive of reactivity to other materials (68). Biometric measures of possible underlying physical effects show promise, such as TEWL to assess barrier function, cross-polarized light and/or temperature differences to evaluate underlying blood flow, or measurement of cytokines. However, to date, no single objective test exists to identify individuals with hyperreactive or sensitive skin.
Triggering Factors of Sensitive Skin
Questionnaire-based surveys have identified a variety of external stimuli as triggers of sensitive skin. Reactions to weather, climate, and environmental conditions are commonly associated with sensitive skin. In a 2008 publication by Saint-Martory et al. (69), environmental triggering factors for sensitive skin at various body sites included cold (66% of sensitive skin group), sun exposure (51%), wind (42%), heat (28%), and pollution (18%). In a study of 994 individuals in the United States, Misery et al. (16) reported that the percentage of subjects experiencing cutaneous reactivity to all climatic and environmental factors, such as dry air, cold, wind, heat, and pollution, was significantly higher in the sensitive skin group compared to that in the nonsensitive skin group. In our studies conducted in the United States, we found a similar result (6,22,23). Perceived irritation to each of the weather conditions listed in the survey (i.e., cold, hot, dry, and humid) was associated with sensitive skin to a significant degree. Similar data were reported by Kamide et al. (9) in a study conducted in Japan. In individuals with sensitive skin, weather and climate conditions were identified as potential triggers by large portions of the sensitive skin group (dry air, 70.5%; cold climate, 53.2%; temperature shifts, 46.9%; air-conditioning, 40.0%; and pollution, 39.3%).
Weather and climate triggers for sensitive skin are dependent on the local conditions. In a recent survey among the general populations of Brazil and Russia, Taïeb et al. (7) found a difference in the most frequently identified environmental triggering factors for sensitive skin. In Russia, the most frequently named factors among the very or rather sensitive individuals were wind (59%), cold (56%), water (54%), temperature shifts (51%), and pollution (47%). In Brazil, where climatic conditions are more homogeneous, sensitivity to cold was less pronounced. The most frequently cited triggers were warm climate (37%), temperature shifts (30%), and pollution (28%), with cold cited by a smaller proportion of subjects (26%).
Misery et al. (14,15) conducted a study during two seasonal periods in France. These investigators reported a higher percentage of the general population claiming sensitive skin in July (86.7% reporting some degree of sensitivity) compared to March (80.8%), leading the authors to conclude that sensitive skin appears more frequently in summer than in winter. In addition, the severity of sensitive skin was worse, as reflected by the number of individuals claiming their skin was very sensitive (21.1% versus 12%, respectively). Cold is a very common triggering factor for sensitive skin. In addition, cooler, dryer weather has been demonstrated to result in higher TEWL values in facial skin which would reflect poorer skin barrier function (70). In light of these observations, it is a bit unexpected that the prevalence of sensitive skin would be higher in the summer (14,15). However, other triggering factors in the summer months, such as sun exposure, air-conditioning, frequent temperature changes, and greater air pollution, may play a role in increasing the perception of sensitive skin (15).
Another commonly cited trigger for sensitive skin is stress or emotions. In our investigation among 1039 individuals in the United States (22), stress was identified as a cause of skin irritation by 63% of the sensitive skin group and 24% of the nonsensitive group. In a study conducted in Italy among 2101 individuals (18), emotions were cited as one of the main triggers for irritation by a large proportion of the sensitive skin group (52% of women and 27.9% of men). In a study in France conducted to evaluate the prevalence of sensitive skin at specific body sites, Saint-Martory et al. (69) reported that 61% of sensitive skin subjects identified stress as a triggering factor, a frequency second only to cold (66%). Animal models have demonstrated that stress can activate dermal mast cells and skin nerves (1). Further, individuals with reactive skin (as determined by electric current perception) have been demonstrated to have a higher density of mast cells (74).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree