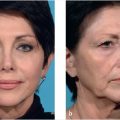
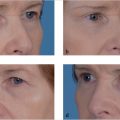
Abstract
Successful forehead lift depends on careful preoperative facial analysis and proper selection of the ideal procedure. Particular attention should be given to the assessment of blepharoptosis, horizontal rhytides indicative of frontalis compensation, corrugator function, hairline, and brow and globe position. Endoscopic and transpalpebral approaches to the forehead provide access for forehead suspension and corrugator resection and isolated corrugator resection, respectively.
33 Brow and Forehead: Forehead Lift
Key Points
Forehead rejuvenation has a significant role in comprehensive facial rejuvenation.
Circumspect facial analysis provides a crucial foundation in selecting the appropriate surgical technique and in optimizing the final aesthetic outcome.
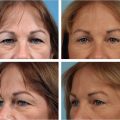
The horizontal lines in the forehead denote frontalis compensation of upper eyelid ptosis or dermatochalasia.
For patients who need a brow lift as well as corrugator muscle resection, an endoscopic procedure would be ideal.
For patients with close to optimal eyebrow position who have deep frown lines, those with a long or very round forehead, and patients with exophthalmos or proptosis, the transpalpebral approach is more appropriate.
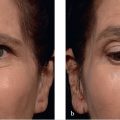
On patients who have eyelid ptosis or proptosis, elevation of the eyebrows may divulge a condition that otherwise may not be so discernable.
33.1 Preoperative Steps
33.1.1 Analysis
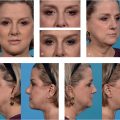
The facial rejuvenation procedure begins with a thorough preoperative analysis including rhytides, forehead length and contour, brow position, shape, and hairline.
Special attention should be given to concomitant eyelid ptosis and overactive frontalis, corrugator supercilii, and/or depressor supercilii muscles with dynamic evaluation.
33.2 Operative Steps
See Video 33.1.
33.2.1 Endoscopic Forehead Lift
Approach to Endoscopic Access
Access is gained using five 1.5-cm incisions hidden in the hairline.
A midline incision is marked vertically at the widow’s peak.
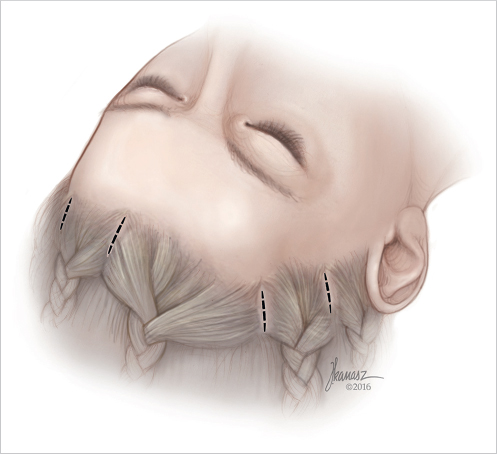
The next two incisions are marked in the temple area, approximately 0.5 to 1 cm behind the hairline; the first about 7 cm from the midline incision and the second about 10 cm from the midline incision (Fig. 33.1).
The entire forehead and scalp area extending about 8 to 10 cm behind the hairline is infiltrated with 1% lidocaine with 1:100,000 units of epinephrine for non-hair-bearing areas and 1:200,000 units in hair-bearing areas.
The patient’s hair may be braided between the marked incisions or put into rubber bands to avoid interference with the procedure.
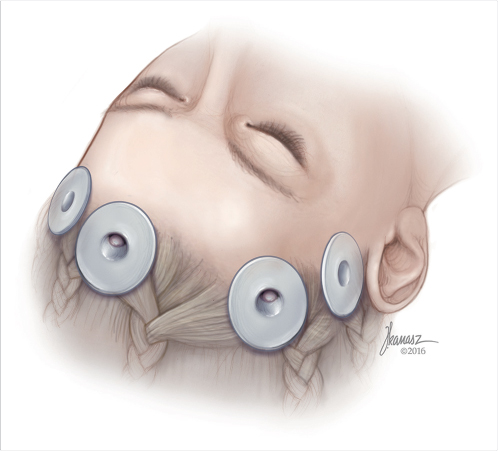
An endoscopic access device (EAD) may be utilized to ease the introduction of instruments during the procedure (Fig. 33.2).
The most lateral incision on one side is carried through the superficial temporalis fascia down to, but not through, the deep temporal fascia.
An elevator, such as an Obwegeser periosteal elevator, is used to dissect the tissue at a plane superficial to the deep temporalis fascia to a minimal extent.
This plane is extended cephalad to a subperiosteal plane, which is located medial to the temporal ridge and therefore overlies only the periosteum, and where the second incision is marked.
Once the second incision is carried down through the periosteum, the dissection is performed medially under the midline incision.
The medial incision is made down through the periosteum and into the target plane.
The procedure is repeated on the contralateral side, developing the plane from lateral to medial.
The two planes are connected using a periosteal elevator and extended cephalad to allow enough tissue laxity for the introduction of the endoscope and related instruments.
The Obwegeser elevator is used laterally to further skeletonize the deep temporal fascia posteriorly to approach ear level. This plane should remain deep to the superficial temporal fascia, but superficial to the deep temporal fascia.
The Obwegeser elevator is then introduced through the midline incision and the area 8 to 10 cm behind the middle incision is released in a subperiosteal plane, providing laxity for the procedure.
Endoscopic Dissection
The endoscope is introduced and dissection of the forehead area is performed under direct visualization in a subperiosteal plane to the supraorbital rim. It is crucial to conduct the dissection immediately superficial to the deep temporal fascia and deep to any piece of fat attached to the superficial temporal fascia to protect the frontal branch of the facial nerve.
The arcus marginalis and periorbita are released from the superior orbital rim and along the lateral orbital wall and dissection carried medially to the glabellar area.
The supraorbital and supratrochlear nerves and vessels are identified immediately above and along the medial third of each orbital rim.
The corrugator muscle lies both deep and superficial to the nerves.
A Daniel endoscopic grasper is utilized to remove the corrugator muscle as radically as possible.
The nerves are preserved and may be retracted utilizing a nerve hook.
Most medially, in the glabellar area, the periosteum is elevated but not transected. Transection is only necessary if there is significant and unusual hyperactivity of the procerus muscle.
A longer periosteal elevator is utilized to reach the midline areas; this subperiosteal plane is also developed laterally along the orbital rim and down to the zygomatic arch.
Dissection is carried laterally and efforts made to avoid and preserve the sentinel vein.
A similar dissection is conducted on the opposite side and the corrugator supercilii muscle is removed.
Hemostasis is maintained utilizing suction electrocautery.
The corrugator muscle is replaced with fat graft harvested through a small rent immediately above the zygomatic arch medially deep to the deep temporal fascia, which is facilitated by pressing on the buccal fat pad, or from another site if other procedures are being performed concurrently.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree