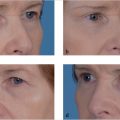
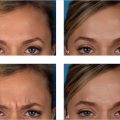
Abstract
Lower eyelid blepharoplasty is one of the most complex procedures performed by plastic surgeons, and if done improperly may cause significant long-term sequelae. Here we provide a comprehensive and systematic approach to the lower eyelid, which is critical for lower eyelid blepharoplasty success.
31 Eyelids: Lower Blepharoplasty
Key Points
A comprehensive and systematic ophthalmic history and examination are critical in establishing goals and formulating a precise surgical plan for lower blepharoplasty.
Lower eyelid malposition, scleral show, dry eyes, ectropion, and other complications can be prevented with a thorough understanding of periorbital anatomy and precise surgical planning and execution.
31.1 Preoperative Planning
31.1.1 Focused Ophthalmic History
A thorough medical history and focused ophthalmologic history must be obtained. Please refer to Chapter 29.
31.1.2 Focused Ophthalmic Examination
Evaluation should include facial proportions, skin type, skin thickness, skin excess, snapback, palpebral fissure size/shape, fat herniation, tear trough, canthal position, extraocular muscle function, Bell’s phenomenon, levator function, margin reflex distance, brow and eyelid ptosis, and globe position relative to malar prominence.
Greater than 6 mm anterior distraction indicates significant skin laxity.
Lateral canthal tilt is typically 2 mm superior to the medial canthal position (positive canthal tilt).
Posterior displacement of the orbital rim in relation to the anterior portion of the globe is a negative vector and must be identified in the preoperative consultation.
Malar anatomy should be evaluated for tear trough deformities or prominent nasojugal folds, which may guide lower eyelid operative plans.
31.1.3 Standardized Photography and Digital Imaging
Standardized photographs including frontal, lateral, and oblique should be obtained for every patient.
Additional dynamic views are recommended.
31.1.4 Preoperative Markings
Markings are performed in the upright position in neutral gaze.
Areas of volume deflation, fat excess, and the tear trough should be marked.
Periorbital fine lines should be marked as these may guide incision placement.
31.2 Operative Approach
See Video 31.1.
31.2.1 Five-Step Lower Blepharoplasty Technique
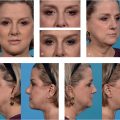
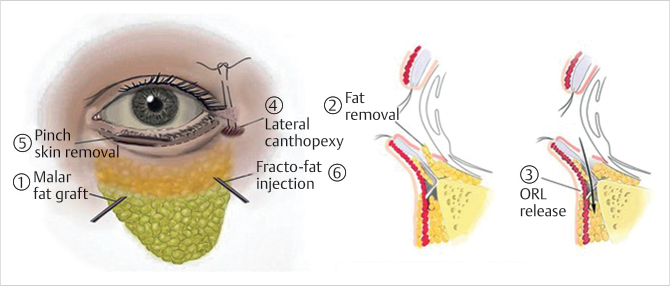
Step 1: Deep malar fat compartment augmentation: Fat is injected into the deep malar space from the alar base as an entry point using a 2-mm blunt single side-hole cannula approximately one fingerbreadth below the orbital rim correcting malar deflation (Fig. 31.1).
Step 2: Transconjunctival removal of lower eyelid fat (if indicated): Only a small amount of fat is removed, proceeding from medial to lateral in most cases. In general, the amount of fat removed decreases as you proceed from lateral to medial. The lateral deep lower eyelid fat tends to be fuller, more robust, and more vascular. The lateral fat pad is also the most likely to be missed, causing persistent lateral fullness postoperatively (Fig. 31.1).
Step 3: Lateral retinacular canthopexy: An absorbable 5–0 Vicryl (Ethicon, Inc., Somerville, NJ) suture should be used for the lateral canthopexy, to prevent scleral show and lower eyelid malposition without affecting long-term lateral canthal shape. A 5–0 Mersilene (Ethicon, Inc., Somerville, NJ) suture may be necessary in men, secondary lax eyelids, cases of dry eyes, and in negative vector patients (Fig. 31.1).
Step 4: Skin pinch removal: After appropriate markings are made, fine-tooth forceps are used to pinch the excess skin, creating a linear partition to be excised. Curved scissors are then used to carefully excise the skin, maintaining the underlying orbicularis muscle intact (Fig. 31.1).
Step 5: Fractionated fat injection and release of the orbicularis retaining ligament: A stab incision is made laterally, right at the orbital rim, followed by fractionated fat (fracto-fat) injected both above the periosteum and also below the muscle with 50% overcorrection. This is performed using a fine 1-mm cannula with a single side hole. Fat is generally harvested from the inner thigh with a small multiport cannula. The harvested fat is centrifuged with the supranatant and infranatant wasted. The remaining fractionated fat is then run through a tulip connector at least 50 times to allow for true fat fractionation. This excludes viable fat cells and therefore prevents uneven fat take in this area. The medial portion of the orbicularis retaining ligament needs to be released from its maxillary attachments to blend this transition zone. Release is performed laterally using the same fine 1-mm cannula and is gently performed in a blunt manner through the supraperiosteal plane (Fig. 31.1).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree