FIGURE 13.1 Split-face application of lactic acid and its vehicle (control) before measuring cerebral activation by fMRI. (From Querleux, B., Dauchot, K., Jourdain, R. et al., Skin Res Technol, 14, 454–461, 2008. With permission.)
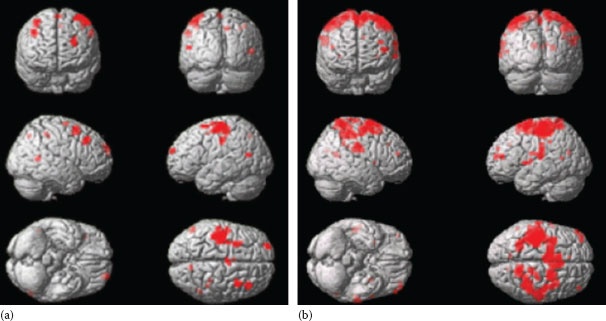
As the LAST is based upon the reported sensations by the subject in terms of nature and intensity, it has raised controversies owing to the use of a subjective individual pain scale hard to tackle by the investigator. Indeed, there is no consensual scale for quantifying the intensity of the sensory response experienced (23). So the experience of pain reported by a subject can never be fully confirmed or invalidated by an external observer. Nevertheless, the relevance of the stinging sensations reported by the subjects has been shown by measuring cerebral responses to the LAST with fMRI (24). According to their answers to a self-assessment questionnaire, 18 subjects were divided into two balanced groups: severe sensitive skin and completely nonsensitive skin. Inclusion criteria involved the absence of any dermatological, neurological, or vascular condition affecting the face. Event-related fMRI was used to measure cerebral activation induced by split-face application of lactic acid and its vehicle (control) (Figure 13.1). In both groups, skin discomfort due to lactic acid increased activity in the primary sensorimotor cortex contralateral to the application site and in a bilateral frontoparietal network including the parietal cortex, the prefrontal areas around the superior frontal sulcus, and the supplementary motor area. However, activity was significantly larger in the sensitive skin group. Most remarkably, in the sensitive skin group only, activity spread into the ipsilateral primary sensorimotor cortex and the bilateral peri-insular secondary somatosensory area (Figure 13.2). These results demonstrated that compared with control subjects, self-perceived sensitive skin subjects had a specific cerebral activation during LAST, which allowed the authors to hypothesize that self-perceived sensitive skin was intrinsically linked to a specific neurophysiologic pattern for these subjects. This study highly contributed to give evidence of the clinical reality of this syndrome and of the pertinence of the psychophysical approach.
FIGURE 13.2 Evidence of SSS. Cerebral activity induced by lactic acid application is larger in sensitive skin subjects (a) than in nonsensitive skin subjects (b). (From Querleux, B., Dauchot, K., Jourdain, R. et al., Skin Res Technol, 14, 454–461, 2008. With permission.)
Although very useful for assessing the product safety, the LAST does not fully render the complexity of self-assessed sensitive skin, as illustrated by the discrepancy between lactic acid response and self-perception of sensitive skin (25). In 2000, this difference was taken into account for the recommendation to include stingers with a concomitant self-declared sensitive skin as panelists for safety testing (26).
The Capsaicin Test
Owing to the great similarity of symptoms induced by topically applied capsaicin with those associated with sensitive skin (27), a new elicitation test using a 0.075% emulsion of this pungent compound extracted from chili peppers was proposed in the 1990s to identify people with sensitive skin (28). By activating TRPV1, the cutaneous application of capsaicin causes the appearance of uncomfortable sensations such as itching, burning, or stinging associated or not with redness at the application side (27,29). These unpleasant reactions are more frequent and more intense in self-declared sensitive skin subjects (28). Whether it is linked to difference in nerve ending density and/or TRPV1 functionality remains an open question. This initial capsaicin test was very promising as it presented a stronger link with self-declared sensitive skin than the LAST (30). But similar to the LAST, it could have been controversial since involving the use of a subjective individual pain scale as well and it induced too painful sensations in very sensitive skin subjects.
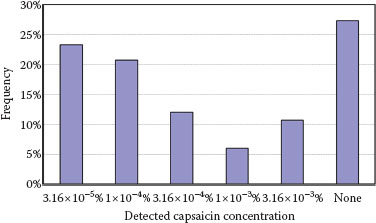
To overcome these issues, a second-generation test with capsaicin has been proposed. This test, called capsaicin detection threshold (CDT) test, combines the specific reactivity of sensitive skin to capsaicin confirmed by other studies (31), the application simplicity of the LAST, and a method of detection threshold. It does not rely anymore on the quantification of the intensity of the response but on the determination of detection thresholds of topically applied capsaicin. Five capsaicin concentrations are used in 10% ethanol aqueous solution (3.16 × 10−5%, 1 × 10−4%, 3.16 × 10−4%, 1 × 10−3%, 3.16 × 10−3%). The method used to attain the detection threshold consists of applying increasing concentrations of capsaicin onto the nasolabial folds (3-minute interval between each application). The vehicle is simultaneously applied following a split-face, single-blind plan. The test is stopped as soon as the subject reports a specific sensation on the capsaicin side. Its accuracy/reliability and its safety were first assessed in a random population of 150 healthy adult women (32). The CDT test allowed the test population to be classified according to six threshold levels corresponding to the sensitive reaction to one of the five capsaicin concentrations and to the absence of reaction to the highest concentration (Figure 13.3). The lowest capsaicin concentration was detected by 23.3% of the panelists, whereas almost the same proportion (27.3%) did not perceive even the highest concentration that is a hundred times more concentrated. This large distribution of the test population illustrated the very important interindividual differences concerning activity and/or density of cutaneous nerve endings, which is probably the major physiological feature explaining the phenomenon of sensitive skin. In addition, the distribution of the population was surprisingly not unimodal and revealed the existence of two different subgroups: individuals with low CDT and those with high threshold. These two subpopulations strongly differed in their respective self-perception of sensitive skin according to their responses to a sensitive skin questionnaire. The higher the self-declared sensitive skin incidence was, the lower the detection threshold was.
FIGURE 13.3 Distribution of 150 women in six subpopulations according to their CDT. (From Jourdain, R., Bastien, P., de Lacharrière, O., and Rubinstenn G., J Cosmet Sci, 56, 153–166, 2005. With permission.)
This difference is certainly due to an overactivation of TRPV1 receptor, which can be reduced by the selective antagonist trans-4-tert-butylcyclohexanol developed as a novel bioactive for the treatment of sensitive skin (33). In addition, the safety of the CDT test was judged as excellent by the panelists since all the reported sensations were considered as slightly or moderately perceptible, even in volunteers with the most sensitive skin. The total absence of pain is highly advantageous for testing routine in the cosmetic domain. The bilateral procedure with the simultaneous presentation of the vehicle on the contralateral side as control helps volunteers to differentiate background cutaneous sensations from those specifically caused by capsaicin (27), thus avoiding false-positive results (34
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree