Key Words
nine nasal subunits: dorsum, tip, columella, and paired sidewalls, soft triangles, and ala, subunit principle, local transposition flaps, paramedian forehead flap, cartilage grafts, restoration of nasal lining
Synopsis
Nasal defects pose a unique set of challenges for the reconstructive surgeon given the significance, both functionally and esthetically, and nuanced anatomy of the nasal framework. The character of the defect, including the size, location, depth (layers of tissue lost), subunits involved, and comorbid patient factors, will dictate the most appropriate method of reconstruction. All components of the nasal defect must be restored, including lining, support, and skin. Options for soft tissue cover include healing by secondary intention, full-thickness skin grafts (FTSGs), bilobed flaps, melolabial flaps, paramedian forehead flaps, and microvascular flaps. Bony and cartilaginous framework may be reconstructed with split calvarial, conchal, septal, or rib grafts, respectively. Lining restoration is critical to prevent contracture and distortion of the external nasal shape and airway, and may be achieved with septal flaps, prelaminated forehead flaps, or microvascular free tissue transfer for extensive or complex defects. A combination of these aforementioned key techniques may be used to reconstruct nearly any nasal defect.
Clinical Problem
Nasal defects demonstrate a wide spectrum of presentations that vary by location, size, depth (nasal lining, support, and skin), and wound condition. Given the central position of the nose on the face, such defects are commonly secondary to resections of cutaneous malignancies. Other etiologies include congenital malformations, trauma, burns, infection, and immune disease. In the developing world, infections and late-presenting tumors resulting in significant nasal defects may be more common.
Pre-Operative Management
Key Anatomy
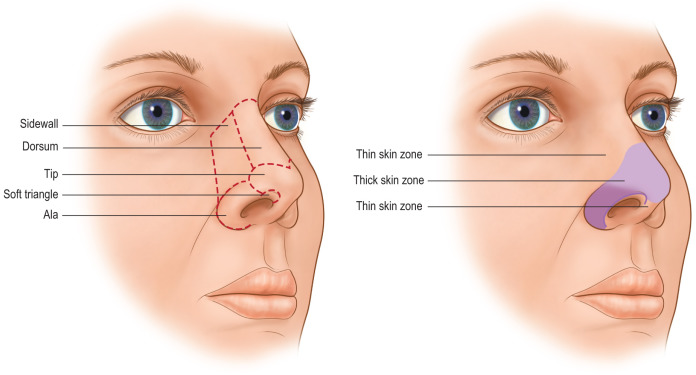
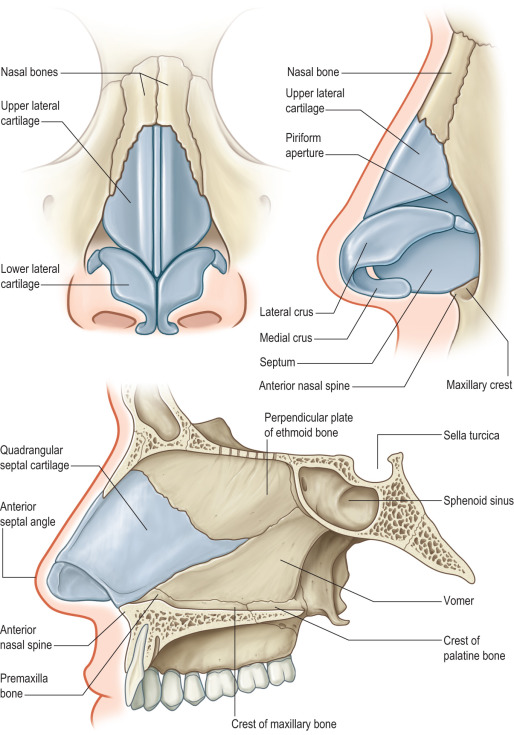
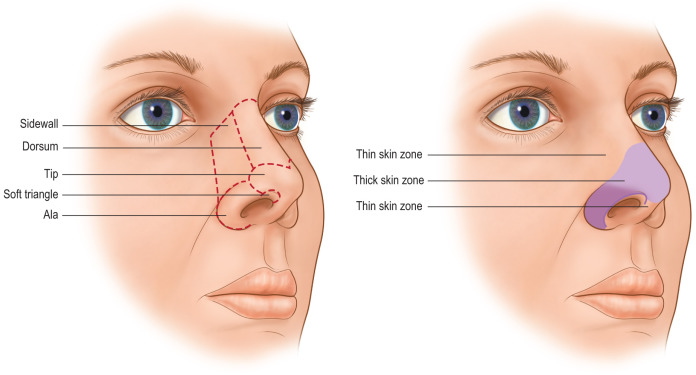
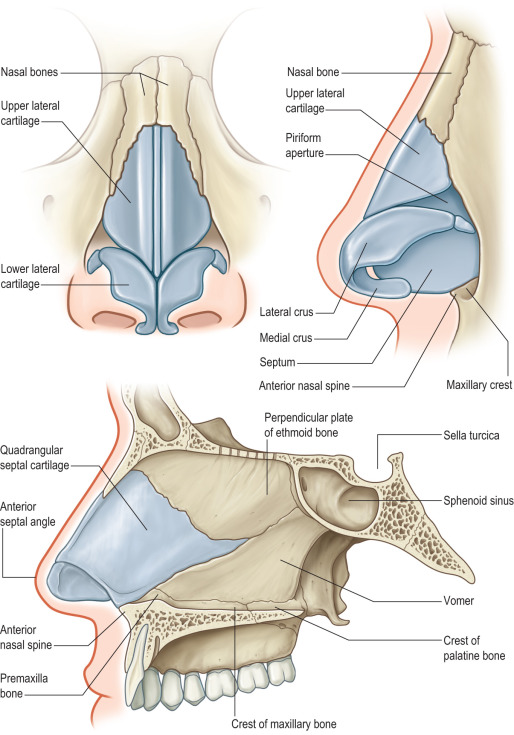
The nose is a complex three-dimensional structure composed of nine subunits based on skin quality and contour: dorsum, tip, columella, and paired sidewalls, soft triangles, and ala ( Fig. 3.8.1 ). The superior two-thirds of the nose and columella have thin, mobile skin. The skin of the inferior one-third of the nose tends to be thicker with adherent sebaceous glands. The nose is internally lined by skin caudally, which then transitions to mucosa at the pyriform aperture. The bony and cartilaginous skeleton provides nasal contour and is divided into three vaults ( Fig. 3.8.2 ). The upper vault is formed by the nasal bones and frontal process of the maxilla, whereas the middle and lower vaults are composed of the upper lateral cartilages (ULCs) and lower lateral cartilages (LLCs), respectively. Each LLC has three crura: medial, middle, and lateral. The keystone area is the site of overlap between the nasal bones and the ULCs, and is typically the widest area of the nasal dorsum. The scroll area is the connection of the lateral crura to the ULCs. The nasal septum, which is the main source of nasal support, consists of both a quadrangular septal cartilage and bone of the ethmoid and vomer.
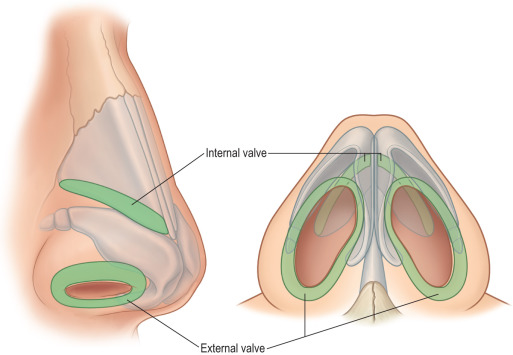
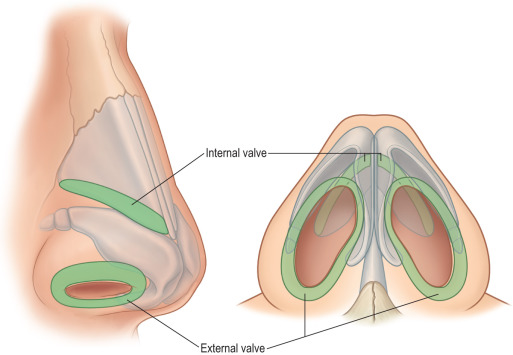
The nasal valves are often involved in airway obstruction ( Fig. 3.8.3 ). The internal nasal valve is created by the junction of the septum and ULC and measures 10 to 15 degrees, with more acute angles associated with obstruction. The external nasal valve is formed by the septum and LLC, and insufficiency may manifest as collapse of the sidewall or ala upon inspiration.
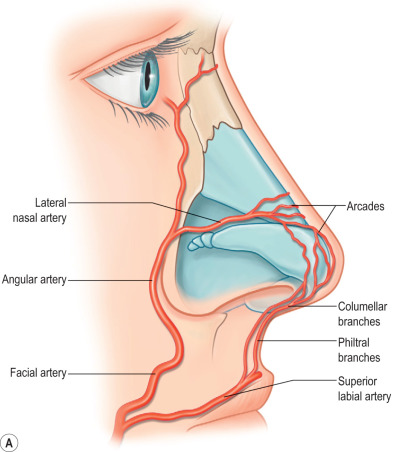
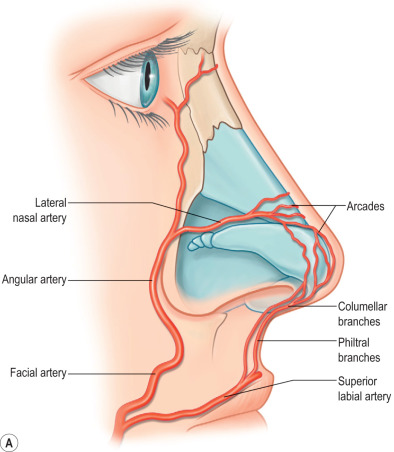
Blood supply to the nose is from branches of the internal and external carotid arteries with interconnections via extensive collateralization ( Fig. 3.8.4A ). The ophthalmic artery arises from the internal carotid to supply the superior nasal envelope, with branches including the anterior ethmoidal, dorsal nasal, and external nasal arteries. The maxillary artery from the external carotid supplies the dorsum and lateral sidewalls via the infraorbital branch. The facial artery also arises from the external carotid to provide the majority of the blood supply to the nasal envelope and tip via the superior labial and angular branches. The superior labial artery supplies the nasal sill, septum, and columellar base, and branches to form the columellar artery. The angular artery gives rise to the lateral nasal artery that supplies the lateral aspects of the caudal nasal envelope. Arteries course in the subdermal plane. Venous drainage mirrors arterial supply, with most vessels draining to the facial vein.
Sensory and motor innervation is provided by branches of the trigeminal and facial nerves, respectively. The supratrochlear and infratrochlear nerves, which originate from the ophthalmic division of the trigeminal nerve, innervate the radix, rhinion, and cephalic nasal sidewalls. The external nasal branch of the anterior ethmoid nerve from the ophthalmic division travels between the nasal bone and ULC to innervate skin over the dorsum to the tip. The infraorbital branch of the maxillary division emerges from the infraorbital foramen to supply the caudal sidewalls and columella. Branches of the facial nerve innervate nasal musculature including the nasalis, procerus, depressor septi nasi, and levator labii superioris alaeque nasi.
Physical Examination
The most critical aspect of the pre-operative physical examination is definition of the anatomical defect, including the size, depth, location, subunits involved, health of the wound, and surrounding skin quality. The defect should be examined for involvement of the skin, lining, and cartilaginous and bony framework. The patient interview should include questions about any prior history of nasal surgeries, and prior facial scars should be noted, particularly scars of the nose, cheek, forehead, and ears if donor auricular cartilage is anticipated. It is also important to assess for comorbid factors that may impair vascularity or affect the timing of reconstruction, including smoking, radiation, diabetes, and peripheral vascular disease.
Operative Planning
Several considerations influence surgical timing. In cases of malignancy where the goal is a curative resection, negative margins must be ensured before reconstruction. The wound should also be clean and free of infection. If the defect involves bone and/or cartilage, it is advisable to reconstruct these components at the time of soft tissue reconstruction or in a delayed primary manner, because reconstruction becomes more challenging after the formation of scar tissue and contracture.
Most skin grafts and local or regional flaps can be performed under local anesthesia or monitored anesthesia care. General endotracheal intubation is often necessary for larger reconstructions. For procedures involving internal dissection, application of a topical lidocaine 4% and oxymetazoline hydrochloride mixture and septal injection of local anesthetic are useful techniques to augment vasoconstriction and analgesia. Nerve blocks with local anesthetic may also be performed. The infraorbital nerve is blocked by injection at its site of emergence from the infraorbital foramen, approximately 1 cm below the inferior orbital rim. The infratrochlear nerve is targeted by injection of the cephalic sidewall near the medial canthus. Lastly, the external nasal branch of the anterior ethmoidal nerve is blocked by injection 1 cm lateral to the midline where it emerges between the nasal bones and ULCs.
Pre-Operative Management
Key Anatomy
The nose is a complex three-dimensional structure composed of nine subunits based on skin quality and contour: dorsum, tip, columella, and paired sidewalls, soft triangles, and ala ( Fig. 3.8.1 ). The superior two-thirds of the nose and columella have thin, mobile skin. The skin of the inferior one-third of the nose tends to be thicker with adherent sebaceous glands. The nose is internally lined by skin caudally, which then transitions to mucosa at the pyriform aperture. The bony and cartilaginous skeleton provides nasal contour and is divided into three vaults ( Fig. 3.8.2 ). The upper vault is formed by the nasal bones and frontal process of the maxilla, whereas the middle and lower vaults are composed of the upper lateral cartilages (ULCs) and lower lateral cartilages (LLCs), respectively. Each LLC has three crura: medial, middle, and lateral. The keystone area is the site of overlap between the nasal bones and the ULCs, and is typically the widest area of the nasal dorsum. The scroll area is the connection of the lateral crura to the ULCs. The nasal septum, which is the main source of nasal support, consists of both a quadrangular septal cartilage and bone of the ethmoid and vomer.
The nasal valves are often involved in airway obstruction ( Fig. 3.8.3 ). The internal nasal valve is created by the junction of the septum and ULC and measures 10 to 15 degrees, with more acute angles associated with obstruction. The external nasal valve is formed by the septum and LLC, and insufficiency may manifest as collapse of the sidewall or ala upon inspiration.
Blood supply to the nose is from branches of the internal and external carotid arteries with interconnections via extensive collateralization ( Fig. 3.8.4A ). The ophthalmic artery arises from the internal carotid to supply the superior nasal envelope, with branches including the anterior ethmoidal, dorsal nasal, and external nasal arteries. The maxillary artery from the external carotid supplies the dorsum and lateral sidewalls via the infraorbital branch. The facial artery also arises from the external carotid to provide the majority of the blood supply to the nasal envelope and tip via the superior labial and angular branches. The superior labial artery supplies the nasal sill, septum, and columellar base, and branches to form the columellar artery. The angular artery gives rise to the lateral nasal artery that supplies the lateral aspects of the caudal nasal envelope. Arteries course in the subdermal plane. Venous drainage mirrors arterial supply, with most vessels draining to the facial vein.

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree