Key Terms
Paronychia
Acute paronychia
Chronic paronychia
Onychomycosis
Leukonychia mycotica
Onychauxis
Thick hyperkeratotic nails
Trachyonychia
Twenty-nail dystrophy
Nail disorders are often encountered as “Oh, by the way…” issues, meaning that the patient brings up the concern during an evaluation for some other medical ailment. Even for dermatologists, the evaluation of nail disorders can be daunting because of the challenging terminology and sheer number of conditions that can affect the nail. Many dermatologists have one or more nail books in their personal reference library for this reason.
- •
Anonychia—absence of the nail
- •
Brachyonychia—short nails
- •
Chromonychia—discolored nails
- •
Koilonychia—spoon nails
- •
Leukonychia—white nails
- •
Micronychia—small nails
- •
Onychauxis—thick nails
- •
Onychocryptosis—ingrown nails
- •
Onycholysis—separation of the nail from the bed
- •
Onychomadesis—nail shedding
- •
Onychorrhexis—longitudinal nail ridging
- •
Onychoschizia—split nails
- •
Paronychia—nail fold inflammation
- •
Trachyonychia—rough nails
Important History Questions
How long have your nails been abnormal?
Nail disorders can be congenital or acquired. Infections are more likely to have an acute onset.
Is there any family history of a similar disorder?
Most nail disorders are acquired, but some conditions, such as pachyonychia congenita and Darier disease, are inherited in an autosomal dominant manner. In psoriasis, which has a strong familial element, this question will elicit a positive response in less than half of cases.
Has there been any trauma, and are the nails continuing to change?
Nail trauma can lead to subungual hemorrhage, but even this should be limited to a point in time—the nail discoloration will grow out distally and, eventually, will be sloughed. Ongoing and persistent change, or even worsening disease, is more concerning and could even be a sign of a malignant process.
Important Physical Findings
How many nails are involved?
Some disorders of the nail suggest a systemic disturbance, particularly when multiple nails, or even all the nails, are involved. Other disorders usually involve just one nail, such as onycholysis caused by Pseudomonas infection.
Which portion(s) of the nail are affected by the disease?
Some disorders affect the entire nail plate, whereas other conditions affect only the lunula (argyria) or the distal nail (most forms of onychomycosis). If the nail is thickened, it is important to determine how much of the nail plate is affected. Onychomycosis usually involves just the subungual area; psoriasis usually involves all layers of the nail plate.
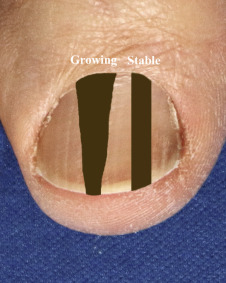
If tan, brown, or black pigment is present in the nail, in a linear fashion, what is the shape of this pigmented area?
Nails are formed in the matrix and move forth as dead keratin. Therefore, the nail provides a 6- to 12-month window into the history of nail health. As shown in Fig. 25.1 , the shape of the pigment deposited provides a clue as to whether the process is growing over time (a widening streak), or if it is a stable process (no widening over time). Longitudinal bands of 4 mm or more in width are more likely to be malignant.
Paronychia
ICD10 code L03.0
BACTERIAL OR FUNGAL INFECTION
Pathogenesis
Acute paronychia is usually caused by bacterial infection, including Pseudomonas spp., Staphylococcus aureus , and β-hemolytic streptococci. Acute paronychia may also be caused by foreign body reactions (ingrown toenails). Chronic paronychia is more often due to infection with Candida albicans . Risk factors for paronychia include frequent gardening, dishwashing, or occupational food handling (one of the authors developed chronic paronychia tending bar). Excessive hand washing (including those in health care) or exposure to solvents and glues may also predispose one to paronychia. Excessive cosmetic removal of the cuticle can result in a space between the nail plate and nail fold that allows for the buildup of irritants (soaps) or for the overgrowth of bacteria (Pseudomonas) and yeast (Candida).
Clinical Features
- •
Acute paronychia is an abrupt inflammatory disorder affecting the proximal nail fold, characterized by pain and erythema. Many cases will drain pus with pressure, or even spontaneously, which may indicate development of an abscess ( Fig. 25.2 ).
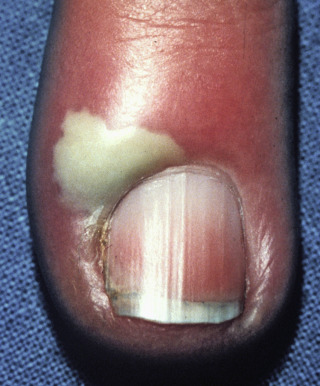
Fig. 25.2
Patient with acute paronychia, with abscess and marked erythema.
(From the Fitzsimons Army Medical Center Collection, Aurora, CO.)
- •
Chronic paronychia is a persistent inflammatory disorder of the proximal nail fold. It affects chiefly women, but both genders and any age group may be affected. It presents as erythema and edema of the proximal nail fold, with loss of the cuticle ( Figs. 25.3 and 25.4 ). The nails may be normal but often demonstrate excessive ridges (Beau lines), variable onycholysis, other nail irregularities, or even a green-blue discoloration due to Pseudomonas infection.
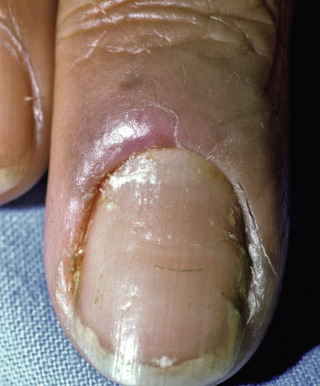
Fig. 25.3
Patient with chronic paronychia, with dystrophic nail.
(From the Fitzsimons Army Medical Center Collection, Aurora, CO.)
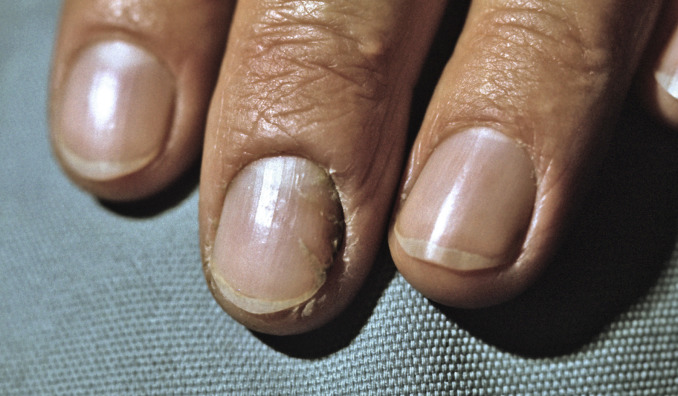
Fig. 25.4
Patient with chronic paronychia, with superficial peeling (onychoschizia) of nails.
(From the Fitzsimons Army Medical Center Collection, Aurora, CO.)
Diagnosis
- •
Acute, chronic, or recurrent erythema and swelling of the proximal nail folds associated with pain suggest the diagnosis; the physical examination is typically diagnostic.
Treatment
Acute Paronychia
- •
Acute paronychia with abscesses, as seen in Fig. 25.3 , should be incised with a no. 11 scalpel blade (usually incised where the skin meets the nail fold or where the nail fold meets the nails). The contents should be cultured.
- •
The most commonly used oral antibiotics are directed against Staphylococcus aureus; options include oral dicloxacillin, cephalexin, and clindamycin if methicillin-resistant S. aureus (MRSA) is a concern.
Chronic Paronychia
- •
Use hand protection (gloves) from potential irritants and water.
- •
Discourage removal of cuticle during a manicure. Explain to the patient that the cuticle is a normal structure necessary to ensure that the nail fold attaches to the nail plate. The absence of this structure results in a space that collects food, soap, bacteria, and yeast.
- •
Discourage the use of antibacterial soaps that result in loss of the normal gram-positive skin flora, resulting in increased gram-negative skin flora (i.e., Pseudomonas ) and yeast overgrowth.
- •
The mainstay of therapy is use of a medium (e.g., triamcinolone) to potent (e.g., clobetasol) topical corticosteroid cream or ointment for 2 to 4 weeks. Approximately 85% of cases will be improved or in complete remission at 4 weeks. However, a high percentage of cases will relapse.
- •
Rare cases may benefit from the addition of a systemic antifungal agent directed against Candida spp. (e.g., itraconazole, 200 mg/day for 4–6 weeks).
Onychocryptosis (Ingrown Toenails)
ICD10 code L60.9
MECHANICAL DISORDER
Pathogenesis
Onychocryptosis is due to an overcurved nail plate that is wider than the nail bed. In many cases, the cause cannot be elucidated, although in some cases it is due tight-fitting shoes, maceration of the lateral nail groove, or cutting the distal nail plate too short. The increased incidence in patients with misalignments of the great toe or wide feet suggests that other mechanical factors are important.
Clinical Features
- •
It may occur in any age group, including neonates, but is most common in adolescents and young adults.
- •
The great toenail is usually affected, but other or multiple toenails may be involved. Less commonly, the nails of the hand can be involved.
- •
Early in the course, erythema, edema, and pain on pressure of the lateral nail groove are present ( Fig. 25.5 ).
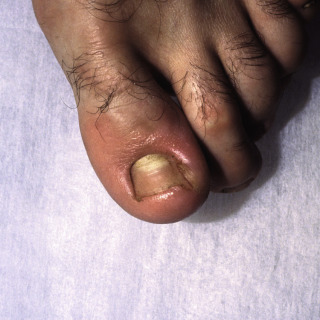
Fig. 25.5
Onychocryptosis of the big toenail in an adult demonstrating marked erythema, induration, and crust of the medial nail fold.
- •
In addition to erythema and edema, developed lesions may demonstrate abscess formation.
- •
Chronic lesions demonstrate granulation tissue and hypertrophy of the lateral nail fold ( Fig. 25.6 ).
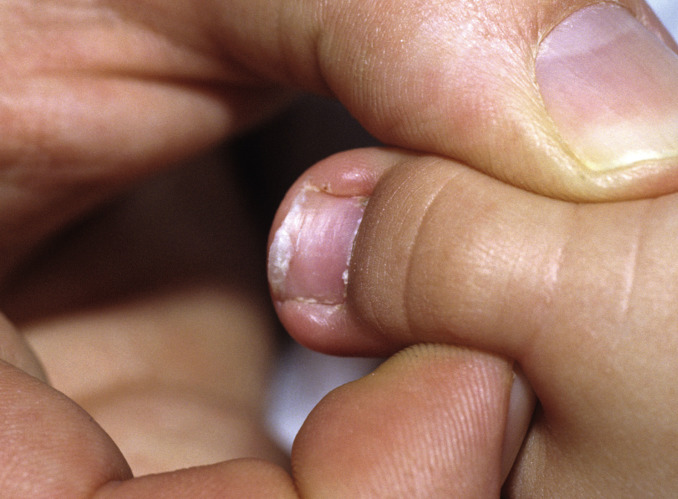
Fig. 25.6
Chronic pediatric bilateral onychocryptosis in a young child. Note that the nail demonstrates more than normal curvature, a frequent clinical finding.
(From the William Weston Collection, Aurora, CO.)
Diagnosis
- •
There is a history of acute or chronic erythema and pain of the lateral nail fold.
- •
The physical appearance demonstrates variable edema and erythema that is most pronounced on the distal lateral nail fold.
- •
Compression of the lateral nail fold toward the nail plate will almost invariably produce pain.
Treatment
Acute Ingrown Toenail
- •
Neonatal ingrown toenails can usually be treated by soaking the nail in warm water, followed by gentle massaging of the distal nail plate and lateral nail fold and then the application of petrolatum.
- •
Adult nails can also be treated with soaking the nail in warm water (with or without Epsom salts).
- •
A wisp of cotton can be gently inserted between the distal lateral nail and lateral nail fold to reduce contact. This can be replaced daily. The cotton can also be impregnated with an antiseptic.
- •
The topical application of a medium (e.g., triamcinolone) to potent (e.g., clobetasol) topical corticosteroid cream or ointment for 1 to 2 weeks is useful for reducing the inflammatory host response.
- •
A strip of adhesive tape may also be attached to the lateral nail fold, pulled beneath the toe, and adhered to the plantar surface to relieve the pressure point between the nail and lateral nail groove. This can be repeated daily, as needed, until the inflammation improves.
Developed Ingrown Toenails With Abscesses
- •
Conservative measures, as outlined for acute ingrown toenails, can be used.
- •
An abscess should be drained for immediate relief.
- •
Surgical treatment options may be considered but require local anesthesia, with a proximal block.
- •
Although many surgical treatments have been described, the most common technique involves using a septum elevator to free the lateral nail fold from the nail bed, matrix, and proximal nail fold, followed by longitudinally splitting the nail (using an English anvil nail splitter) to the matrix and removing a portion of the lateral nail (typically, ≈2 mm wide). This is followed by cauterization of the lateral matrix with 90% phenol for 2 to 3 minutes (some authorities prefer three separate 30-second applications), followed by flushing the area with alcohol to neutralize the phenol.
Chronic Ingrown Toenails With Granulation Tissue and Hypertrophy
- •
Surgical treatment is required in some cases. This should be done by a clinician with experience.
Onychomycosis
ICD10 code B53.1
FUNGAL INFECTION
Pathogenesis
Onychomycosis (tinea unguium) is a fungal infection of the nail that is usually caused by infection with a dermatophyte, with Trichophyton rubrum accounting for the vast majority of cases (>70%). Less commonly, nondermatophytes including Candida spp. (≈10%), Scopulariopsis brevicaulis (≈10%), Fusarium spp., and others may produce disease.
Clinical Features
- •
Although it may occur at any age, the prevalence increases with older age and is most common in the elderly.
- •
Although any nail may be infected, usually toenails are preferentially involved.
- •
The number of infected nails is variable, one to all nails.
- •
The appearance of the nail is dependent on the degree of infection. Typically, the dorsum of the nail plate is normal, and the underlying subungual area is affected with hyperkeratotic crumbly keratin, which may produce a yellow-white discoloration of the nail ( Fig. 25.7 ).
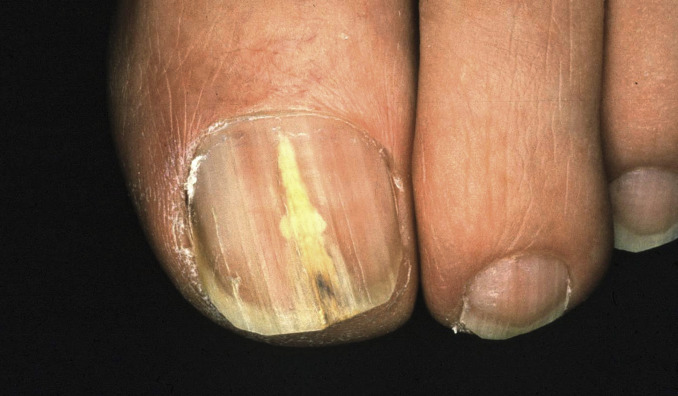
Fig. 25.7
Patient with onychomycosis demonstrating a yellowish-white subungual infection.
(From the Fitzsimons Army Medical Center Collection, Aurora, CO.)
- •
The distal portion of the nail is typically involved, and the proximal area near the skin is spared.
- •
Associated findings consistent with tinea pedis are often present ( Fig. 25.8 ).
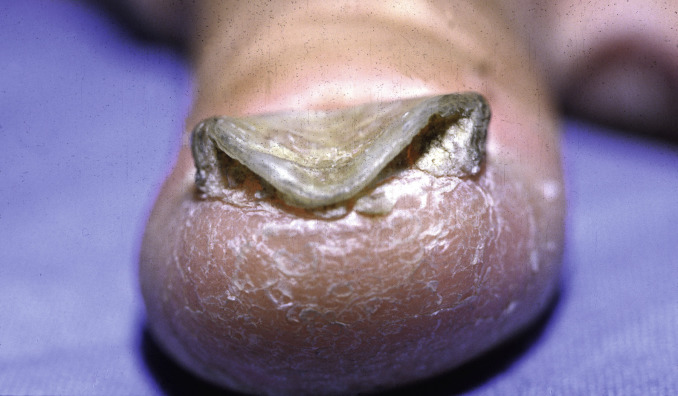
Fig. 25.8
Patient with dry scaly tinea pedis, with development of subungual onychomycosis.
(From the Fitzsimons Army Medical Center Collection, Aurora, CO.)
- •
Less commonly, the nail may demonstrate onycholysis (loss of adhesion).
- •
The nail plate may be normal or dystrophic; very rarely, the nail demonstrate full-thickness infection.
- •
Leukonychia mycotica is a less common variant characterized by a white discoloration on the surface of the nail. This is produced when the dermatophyte has infected the surface of the nail.
Diagnosis
- •
In regard to the clinical presentation, onychomycosis is in the differential diagnosis in any nail disorder demonstrating subungual discoloration or onycholysis.
- •
The diagnosis can be confirmed by sampling the subungual debris with a small curette or scalpel blade (no. 14) and identifying hyphae with a potassium hydroxide preparation (see Chapter 2 ).
- •
Material for culture can be obtained by a small curette or scalpel blade or by clipping or cutting the nail.
- •
For biopsy, the nail plate can be clipped or cut and sent to a pathologist or dermatopathologist for special staining.
Although prospective randomized trials have not been performed, surgical avulsion of nails as a monotherapy has a high recurrence rate in onychomycosis. In those cases in which it needs to be done for mechanical reasons, concomitant antifungal therapy is needed.
Treatment
- •
Onychomycosis is a chronic and often progressive infection that does not spontaneously resolve.
- •
No treatment is an option because the treatment is not always successful; however, patients with diabetes or a history of recurrent cellulitis should be considered for treatment to reduce the chance of developing recurring cellulitis. Patients with painful onychomycoses are also candidates for therapy.
- •
Topical treatments include ciclopirox olamine, 8% lacquer, or efinaconazole, 10% topical solution. Both treatments are applied once daily to the nail for 1 year. The cure rate is around 10%.
- •
Oral terbinafine, which has a cure rate of about 60% to 70%, is the treatment of choice. Fingernails are treated at a dose of 250 mg/day for 6 weeks; toenails are usually treated with 250 mg/day for 12 weeks.
- •
Oral itraconazole and oral fluconazole are alternative options in patients who are not able to take terbinafine; however, the cure rate is lower for both drugs.
- •
Laser ablation followed by topical therapy is an option for select patients who cannot take oral drugs. Approximately 50% of patients demonstrate a complete response with this treatment.
Onycholysis
ICD10 code L60.1
NUMEROUS ETIOLOGIES
Pathogenesis
Onycholysis is not a specific disease but is a term that describes separation of the nail plate from the underlying nail bed. Numerous disease processes may cause onycholysis, including infection (e.g., fungus), medications (e.g., tetracycline-induced photo-onycholysis), trauma (e.g., immersing fingers in scalding water, self-induced), endocrine disorders (e.g., hyperthyroidism), and primary skin disorders (e.g., psoriasis).
Infection
- •
Candida spp.
- •
Dermatophyte
- •
Pseudomonas spp.
- •
Internal disorders
- •
Anemia
- •
Hypothyroidism and hyperthyroidism
- •
Scleroderma
Medications
- •
Chemotherapy
- •
Doxycycline
- •
Oral contraceptives
- •
Fluoroquinolones
- •
Tetracycline
Idiopathic
Neoplasia
- •
Glomus tumor
- •
Squamous cell carcinoma
Skin Disorders
- •
Dermatitis
- •
Psoriasis
Traumatic
Clinical Features
- •
Onycholysis can occur at any age.
- •
Onycholysis may involve one nail or multiple nails.
- •
Onycholysis may be asymptomatic or painful.
- •
Onycholysis usually affects the distal nail, but proximal onycholysis may occur, particularly with chemotherapy.
- •
The lytic (separated) portion of the nail is usually white or yellow-white in color ( Figs. 25.9–25.12 ).
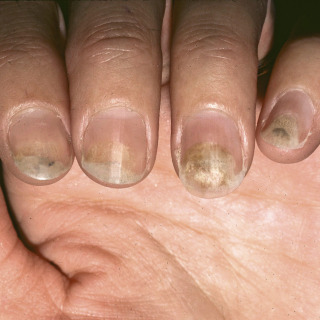
Fig. 25.9
Acute photo-onycholysis due to tetracycline that occurred when the patient was reading a book at the pool.
(From the Fitzsimons Army Medical Center Collection, Aurora, CO.)
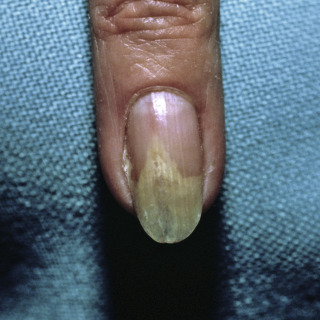
Fig. 25.10
Patient with chronic onycholysis due to repeated trauma of long nails.
(From the Fitzsimons Army Medical Center Collection, Aurora, CO.)
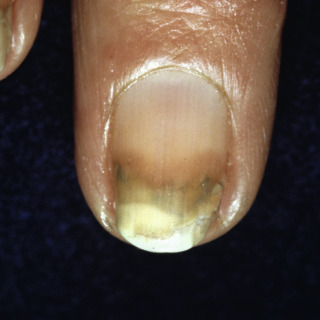
Fig. 25.11
Patient with onycholysis due to excessive use of topical nail hardeners.
(From the Fitzsimons Army Medical Center Collection, Aurora, CO.)
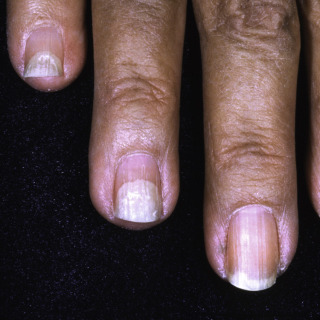
Fig. 25.12
Patient with iatrogenically induced onycholysis due to excessive thyroid supplementation.
(From the Fitzsimons Army Medical Center Collection, Aurora, CO.)
- •
Subungual hemorrhage may be present.
Diagnosis
- •
Onycholysis is usually easily recognized, with observation of a white nail and loss of normal attachment to the underlying nail bed.
- •
Determining the cause of onycholysis is more difficult because multiple disease processes must be considered (see box).
- •
A KOH prep or fungal culture can exclude fungal infection.
- •
Biopsies are usually not performed but may be considered to exclude malignancy, particularly if there is a single onycholytic nail of chronic duration.
- •
In some cases, no cause is ever ascertained (idiopathic).
Treatment
- •
Treatment of the underlying disorder causing onycholysis is the most effective therapy (e.g., decreasing or withdrawing offending medication[s], treatment of infection). It is important to explain to the patient that onycholysis can be permanent.
- •
Unless specific patient behaviors are contributing to the problem, the nails should be trimmed back to reduce the chance of external trauma aggravating the condition.
- •
Repetitive trauma, such as typing or drumming or tapping the nails, should be avoided, where possible.
- •
Prolonged immersion of the nails in water should be avoided, where possible.
- •
Bacterial colonization can be a contributing factor— Pseudomonas produces proteolytic enzymes that aggravate the separation—and yeast can overgrow in the lytic space. Therefore, topical thymol, 3% to 4% in alcohol, applied underneath the nail plate bid for 6 to 12 weeks, is useful. This solution can be formulated by compounding pharmacies or may be purchased via the Internet.
- •
A topical imidazole solution (e.g., clotrimazole) is useful if secondary candidiasis is a concern.
Onychauxis
ICD10 code Q84.5 (or disease-specific code)
NUMEROUS ETIOLOGIES
Pathogenesis
Onychauxis is a descriptive medical term that refers to thick hyperkeratotic nails caused by a buildup of keratin. The most common cause is a dermatophyte (fungal) infection, which is discussed in greater detail in this chapter (see “Onychomycosis”). Psoriasis is another common cause that can be difficult to differentiate from onychomycosis. Other causes are listed in the box.
Common
- •
Onychomycosis
- •
Onychogryphosis
- •
Psoriasis
Uncommon
- •
Darier disease
- •
Norwegian scabies
- •
Pachyonychia congenita
- •
Reactive arthritis (Reiter disease)
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree