Acknowledgment
This chapter was originally written by E. Burke Evans, MD. He passed away in May 2012. We are indebted to his knowledge of burn care. Care was taken to preserve as much of his original material while adding new information.
Introduction
Burn injuries have a tendency, even as they heal, to create musculoskeletal deformity. In addition, the protracted burn illness that accompanies severe burns may result in other skeletal changes. Box 41.1 presents a classification of musculoskeletal changes secondary to burns; from this, the most commonly occurring and clinically significant alterations have been selected for discussion.
Box 41.1
Classification of Musculoskeletal Changes Secondary to Burns
Alterations limited to bone
-
■
Osteoporosis
-
■
Periosteal new bone formation
-
■
Irregular ossification
-
■
Diaphyseal exostosis
-
■
Acromutilation of fingers
-
■
Pathologic fracture
-
■
Osteomyelitis
-
■
Necrosis and tangential sequestration
-
■
Alterations involving pericapsular structures
-
■
Pericapsular calcification
-
■
Heterotopic paraarticular ossification
-
■
Osteophyte formation
-
■
Alterations involving the joint proper
-
■
Dislocation
-
■
Chondrolysis
-
■
Septic arthritis
-
■
Spontaneous dissolution
-
■
Ankylosis
-
■
Alterations involving muscles and tendons
-
■
Desiccation of tendons
-
■
Fibrosis of muscles
-
■
Alterations secondary to soft tissue
-
■
Muscle and joint contractures
-
■
Malposition of joints
-
■
Scoliosis
-
■
Soft tissue injury
-
■
Compartment syndrome
-
■
Nerve injury
-
■
Abnormalities of growth
-
■
Acceleration and retardation
-
■
Destruction of growth plates
Changes confined to bone
Osteoporosis
Osteoporosis is the most frequently occurring postburn change involving bone. Ongoing studies by Klein et al. suggest that, among persons with serious burns, reduction of bone mass density is pervasive. Stated causes of osteoporosis in thermal burns are bed confinement, immobilization, hyperemia, reflex vasomotor phenomena, and adrenocortical hyperactivity. Klein reviews the effects of burn injury on bone metabolism. , Klein et al. noted very limited bone formation after a severe burn. Other endocrine changes that lead to loss of bone after burns have been described by Dolecek et al. This, coupled with the relatively high resorption, leads to osteopenia postburn. Endogenous corticosteroid production is likely responsible for the decreased bone formation, and inflammatory cytokines are responsible for the bone resorption. In this section, only what is clinically apparent is discussed.
The more extensive the burn and the greater the number of complications, the longer the patient may be confined to bed and relatively immobile. The onset of osteoporosis is accelerated, and its intensity is more marked in the burn illness that features a hypermetabolic state. Klein et al. found that osteoblasts and probably osteocytes underwent apoptosis in response to the glucocorticoid stress hormones. The overall effect of burn is catabolic, and muscle wasting is also noted. If a single extremity of an otherwise normal person is immobilized for a long time because of local trauma, as with a fracture, loss of bone density can be easily seen on plain radiographs. So, with burns isolated to the extremities, the bones of affected extremities become osteoporotic, and in persons with generalized burns, the bones of deeply burned extremities may show more profound mineral loss than is observed in nonburned extremities or in the axial skeleton ( Fig. 41.1 ). This tendency for more osteoporosis in severe burns was also noted by Pandit et al., who found that 56% of postburn patients had radiographic evidence of osteopenia. Van der Wiel et al. found in an x-ray absorptiometry study of 16 adults with fractures of one tibia that there was eventual loss of bone mineral density in the contralateral femur and in the lumbar spine but to a lesser degree than in the ipsilateral femur. These findings, although not strictly analogous to those observed in burns, nevertheless point to the occurrence of generalized osteoporosis in other trauma states and the difference in loss of bone density relative to local factors. In fractures or in burns, impaired mobility and local hyperemia could account for this difference.
(A) At 6 months after injury, the coarsened trabeculation of marked osteoporosis of bones is evident on the left hand and forearm of a 4-year-old boy whose 70% full-thickness burn involved the head, chest, and both upper extremities. (B) A radiograph of the left tibia and fibula obtained on the same date as that of the hand shows minimal atrophy.
Another characteristic of the osteoporosis of burns that seems to set it apart is its persistence, not just until restoration of the anabolic state but also for months and years after the burn has healed ( Fig. 41.2 ). This phenomenon may be most clearly observed in patients who have survived 90% burns, but Klein et al. record less than normal bone among even moderately burned children as long as 17 months after injury. Some studies suggest that prolonged dysfunction in the sympathetic nervous system may negatively affect bone metabolism even after acute burn phase, up to 2 years or longer. To further investigate, Roshanzamir et al. measured sympathetic skin response (SSR) in patients after electric burn (>6 months before study) and compared them to a control group. They found that SSR latency is prolonged and amplitude reduced in burn patients; hence, bone metabolism is impeded for a longer time in this subset. In a later study, the same authors proposed using SSR as a predictor for long-term decreased bone mineral density in burn patients and to plan preventive measures for patients at risk. , Muscle atrophy or the failure or inability of the person to return to the preburn level of physical activity may account in part for this protracted state of reduced bone mineralization.
(A) Advanced osteoporosis in the hands of a 14-year-old boy 9 months after a 100% total body surface area burn. All growth plates are open. (B) At 24 months after injury, osteoporosis persists, and there is irregular closure of the metacarpal and phalangeal growth plates. (C) At 8 months after injury, the growth plates of the distal tibiae and fibulae remain open. (D) At 24 months after injury, the distal growth plates of the tibiae and fibulae are closed. Other major growth plates remain open. Osteoporosis is unchanged.
There is no way to prevent osteoporosis in a patient whose burn is of such severity as to require an extended period of bed confinement. Methods of medical treatment described by Klein and Rousseau et al. include anabolic hormones, bisphosphonates, and cholecalciferol. Cholecalciferol was noted to have a positive effect on muscle health but little effect on bone. β-blockers such as propranolol are also recommended because they moderate burn-induced hypermetabolism through inhibiting catecholamine binding to β-adrenoreceptors. As a result, they induce protein synthesis and reduce loss of bone mass. ,
The advance of bone atrophy can at least be favorably modified, even among patients with large burns, if mobilization and active exercise are initiated soon after the burn. The bones of the axial skeleton, the pelvis, and the lower extremities are most efficiently stressed by weightbearing. Thus standing is a priority measure, and it is common practice now to walk patients to tolerance before permanent wound cover. Muscle contraction alone may help forestall bone atrophy, and bone is better stressed if the contraction is resisted. Isometric muscle contraction is possible from even extensively burned patients and is important for bone stress and for maintaining muscle tone and muscle. Passive motion has no effect on bone and thus does not figure in the prevention of osteoporosis. Other preventive measures, such as closure of the wound and maintenance of nutrition, are routine in critical burn care. Treatment of established osteoporosis involves the more aggressive use of measures for prevention. There are no long-term comparative studies, however, that persuasively measure the effectiveness of exercise, diet, medication, or modality in the treatment of osteoporosis in any state. Thus osteoporosis can be lessened by active muscle contraction and weightbearing. Medical treatments that show promise include anabolic hormones, bisphosphonates, β-blockers, and possibly cholecalciferol.
Osteomyelitis
In burns, bones can become infected through exposure of bone by the burn, an open fracture accompanying the burn, extension of infection from a septic joint, introduction of organisms along traction pins or internal fracture fixation devices, or bloodborne organisms of bacteremia. Considering the apparent risk for seriously burned patients to develop osteomyelitis, it is surprising that it does not occur more regularly. A retrospective study of 600 children followed for 10 years showed incidence of 2%. Clinically significant osteomyelitis in burn patients is uncommon. Antibiotics given for the general state may prevent seeding of the bone or may repress any small focus of bone infection.
The cortex of long bones is a good barrier to surface organisms. Even exposure of cortex will have little adverse effect if the blood supply of the bone remains intact. Prolonged exposure will kill the outer layer of the cortex, which will in time sequestrate, separating at a well-defined fissure between dead and living bone. With minor or moderate exposure, the bone will usually survive long enough for bordering granulation tissue to cover it. For large defects, it may be useful to drill closely spaced holes through the exposed cortex to encourage buds of granulation tissue to emerge from the still-vascular medullary canal. Another way to encourage granulation tissue formation over exposed bone is with superficial decortication with an osteotome or burr to expose the capillaries of the inner cortex. With these practices, there is little risk of infecting the bone. It may be that there is sufficient centripetal pressure to discourage the invasion of organisms when the holes are fresh and that the holes are rapidly sealed by blood clots and advancing tissue. There are no reports of deep bone infection related to cortex drilling.
With open fractures at the site of a major soft tissue burn wound, bone infection is probably inevitable. These infections can often remain localized to the fracture site and not involve the rest of the bone. Only local debridement and stabilization of the soft tissue wound are required for treatment. Dowling et al. reported osteomyelitis of the tibia related to an open bimalleolar fracture in an extensively burned extremity. English and Carmichael showed three cases of osteomyelitis out of 28 fractures, and all were found in open fractures. Conversely, osteomyelitis developed in neither of the two open fractures reported separately by Choctaw et al. and Wang et al. We treated three patients in whom open fractures of the femur complicated thigh burns. Each case required aggressive and repeated debridement. One fracture was treated in traction, and the other two were treated with external fixators. In one of the patients, who was admitted 8 months after acute burn, there was established osteomyelitis of the femur in relation to the exposed fracture. Osteomyelitis did not develop in either of the other patients; in the end, all three had sound femurs.
When traction pins are directed through burned skin for the treatment of fractures or for suspension of a burned extremity, the factors favoring development of infection along the pin track and the formation of cigarette sequestra are:
-
■
Introduction or migration of organisms from the burn wound
-
■
Thermal necrosis during introduction of the pins
-
■
Linear pressure of the traction pin
-
■
Prolonged traction
-
■
Excessive movement of the extremity leading to loosening of the pin
-
■
Sealing of the skin of the pin sites
For traction or suspension, pins may be inserted through acutely burned skin, through eschar, through granulation tissue, or later through ischemic burn scar, which may be colonized with uncommon and antibiotic-resistant organisms. No amount of local cleaning is likely to sterilize the surface through which the pin must pass, yet it seems that organisms in sufficient numbers to colonize and infect are rarely introduced in this manner.
Local low-grade infections usually resolve when pins are removed if the pin sites are vigorously curetted of granulation tissue. In one case in which a four-pin custom external fixator was used in the treatment of an open infection of the elbow, diffuse osteomyelitis of the humerus and radius resulted. The infection was controlled with antibiotics and without surgery after the pins were removed. This case was included in the Barret et al. report of skeletal pinning in 41 severely burned children. In experience with the Ilizarov system for correction of skeletal deformity in burns, one patient developed a pin-tract infection of such severity as to require removal of the pin, curettage, and intravenous antibiotics for control of methicillin-resistant Staphylococcus spp. Carmichael et al. reported experience of treating nine patients with open joints in external fixation for an average of 7.1 weeks, and none of them developed pin-tract infections or osteomyelitis. The open joints were treated in joint-spanning external fixators. Most patients had multiple failed skin grafting procedures before fixator placement. The fixators were thought to have decreased the need for additional skin grafting.
Hematogenous osteomyelitis and osteomyelitis caused by spread from an infected joint are rare. There is no report of the occurrence of either entity in association with burns. If bone infection of this sort were to be recognized, effective treatment would depend on the identification of the offending organisms for organism-specific antibiotic regimens.
Fractures
Pathologic fractures were at one time common in burn management because of the practice of delayed excision of eschar and of keeping patients in bed until wounds were completely covered. During that time, fractures occurred because of bone collapse when patients first stood or walked or when stiff joints were manipulated ( Fig. 41.3 ). Bones most commonly affected were the femur at its distal metaphysis and the tibia at its proximal metaphysis. The only treatment required was support of the extremity until the fracture consolidated, usually in 4 to 6 weeks. Children were more often affected than adults, and the fractures usually compressed one cortex, producing an angular deformity that rapidly corrected with growth. A study by Klein et al. strongly suggests that fractures occur more frequently in burned children than in a matched normal population, even months after the acute burn. Now, however, in acute burn management, the most frequently seen fractures are those occurring at the time of, or in association with, the burn injury. Falls or violent trauma account for many of the fractures, and the sites are those common to the causes, bearing no relation to the burn itself.
Pathologic fracture of the osteoporotic femur of a 9-year-old girl sustained on the first day she stood after 5 weeks of confinement for a 40% total body surface area burn.
Although fractures complicate burn treatment and occasionally delay mobilization of patients, their management need not be complex. Fractures in extremities not burned can be treated by manipulative reduction and cast immobilization, by open reduction and fixation, with an external fixator, or with skeletal traction ( Fig. 41.4 ). Fractures in extremities with first-degree or superficial second-degree burns can be managed in the same way. Deep second- and third-degree burns present a different problem only with respect to the early bacterial colonization of third-degree burns and the degradation of deep second-degree burns to full-thickness burns that will in turn become colonized. There is a precious window of time when fractures requiring open reduction and internal fixation (ORIF) can be definitively treated without increased risk for infecting the bone; however, fracture reduction and stabilization are so important in the functional management of a severely burned patient that the risk for bone infection should be acknowledged and shouldered at any postburn stage. English and Carmichael showed that if fractures were treated with open reductions within the first 48 hours postburn, the risk of infection is minimal. Therefore early stabilization is encouraged in the first 48 hours before the risk of infection increases. Newer studies, however, suggest that the higher rate of infection and complications correlates more with severity of the injury than the method and time of fixation. Largely, there is still no consensus on treatment choice and timing. ,
(A) This 15-year-old boy sustained closed fractures of the right femur, left tibia, and left humerus at the time of a 46% total body surface area burn involving mainly the trunk and right lower extremity. The femur and humerus fractures were treated in skeletal traction. Suspension of the right lower extremity aided management of circumferential deep burns of that extremity. Lesser burns of the left leg made it possible to treat the minimally displaced fracture of the left tibia in a circular cast. All fractures consolidated in 6 weeks in satisfactory alignment. (B) Fracture of the left humerus as it appeared at the time of admission to the hospital. (C) At 5 weeks after injury, the fracture shows a maturing callus. Traction was discontinued at 6 weeks.
Skeletal traction is used infrequently today. The disadvantages of skeletal traction are the confinement to bed and the imposed relatively fixed position of the affected extremity. External fixators make it possible to align and stabilize fractures in burned extremities without open operation and provide mobility to the patient. Brooker’s extensive favorable experience supports this concept. With both skeletal traction and external fixation, there is an added risk for bone infection because of the path from surface to bone provided by the pins. Pin-tract infections can be minimized by scrupulous pin site care and by removal and replacement of any loosening pins. Frye and Luterman recognized and discussed the specific and continuous difficulties encountered in the management of fractures and burns.
When casts are used for stabilization of fractures in burned extremities, the wound is made inaccessible, and there is an abiding fear that the unattended wound will seriously degrade or at best not improve. Such fear may be well founded; however, Wang et al. showed that a bivalved circular cast could be used effectively for an open comminuted fracture of a proximal tibia with overlying deep burns, and Choctaw et al. reported successful use of a cast for immobilization of an open comminuted fracture after immediate postburn grafting of the affected extremity. Common sense should dictate which fractures can be treated with circular or bivalved casts or with splints. If casts are used over burned skin, they would need to be removable to allow burn care. If a reduced or moderately displaced but aligned fracture is so stable as to require external support only for maintenance of alignment, then cast or splint immobilization should be all that is needed. On the other hand, if a fracture, because of instability, requires maintenance of reduction by three-point pressure or molding of the cast material, it will be better treated by other means.
English and Carmichael had 28 fractures that were treated over a 20-year span. In that study, 22 of 24 fractures available for long-term review healed in appropriate time. There were five infections noted, including two superficial pin-tract infections from external fixation and three cases of osteomyelitis, all of which were open fractures. In contrast, there were no infections in 42 fractures reported by Saffle et al., nine of which were treated by ORIF. With two fractures of the femur, each of which was exposed at the base of a deep, chronic burn, aggressive debridement of the wounds and the fracture ends was followed by treatment with skeletal traction in one and by external fixation with the Ilizarov system in the other. Both fractures healed without further complication. Coverage of exposed bone can be done with skin grafts, local flaps, and free flaps. Burring of the exposed bone to stimulate bleeding and induce granulation tissue can be used alone or with other procedures to help cover exposed bone. Newer techniques using graft substitute have shown promise in coverage of exposed bones in burn patients. ,
Among severe burn patients, nondisplaced or minimally displaced fractures may not be detected until unusual local pain in an affected extremity prompts radiographic examination. A radiograph obtained for other reasons may reveal a fracture as an incidental finding. These fractures are usually of no functional significance. Modest angular deformity near a joint is more of a problem in adults than in children, who still have remodeling potential. Undetected transphyseal fractures in children can be a major functional threat, however.
Changes involving pericapsular structures
Heterotopic ossification
Heterotopic ossification (HO) is a rare but functionally important complication of thermal burns. The incidence in a general burn population is reported to be somewhere between 1% and 3%. , In select populations, the incidence may be higher, as it will be if patients with periarticular calcification are included in the statistics. For example, Tepperman et al. reported a 35.3% incidence among patients referred to a tertiary care center for rehabilitation. Jackson and Mac observed that the incidence of HO could be expected to be less in institutions that admit patients with minor burns. A radiographic survey by Munster et al. of 88 adult and teenaged patients with 160 burned upper extremities yielded a 16% incidence of pericapsular calcification; the 23% incidence reported by Schiele et al. included both HO and heterotopic calcification. In the early routine radiographic study reported by Evans, periarticular calcification that did not progress to HO was excluded from the final calculation of an incidence of 2%. The 3.3% incidence recorded by Kolar and Vrabec included patients with pericapsular calcification. Pandit noted pericapsular, periarticular, and tendon calcifications at around 1.25% each in a radiographic study. Even if HO occurs infrequently in thermal burns, it often compromises joint motion and is difficult to treat after it develops. In addition, its pathogenesis is still incompletely understood, thus protocols for prevention may in fact be unsuccessful.
Pathogenesis of heterotopic ossification
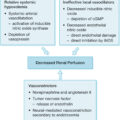
The metabolic changes occurring after thermal burn are increased metabolic rate, protein catabolism, ureagenesis, fat mobilization, glycogenolysis, gluconeogenesis, elevated glucose flow, and eventual total body weight loss. , There is an accompanying suppression of the immune system that favors wound infection but simultaneously favors survival of skin allografts. Infection, failure of skin graft take, or anything that delays closure of a burn wound will extend the altered metabolic state. Although it might be assumed that there occurs, along with the metabolic upheaval, an adverse change in connective tissue milieu, the exact nature of such a change is not known. It is also not clearly understood what the metabolic changes have to do with the development of HO, but it is apparent that the burn disease is necessary to its formation. Current evidence describes endothelial cells, adipose-derived stem cells (ASCs), muscle satellite cells, mesenchymal stem cells (MSCs), fibroblasts, tendon cells, and progenitor cells as potential precursor cells for HO. The combination of osteogenic precursor cells and osteogenic induction factors in the right microenvironment assists in osteogenic differentiation into chondrocytes and eventually ectopic bone. To explain the pathogenesis further, Hu et al. suggested three key pathways involved in the process:
-
1.
Vessel and endothelial cell pathway: Burn-induced edema and hypoxia followed by damage to capillary basement membrane and endothelial cells initiate this pathway. Next, hypoxia-induced factor 1 activates vascular endothelial growth factor (VEGF), which has potent bone regeneration ability and osteogenic differentiation. VEGF acts on ASCs and MSCs and creates preosteoblasts, eventually developing HO. In addition, circulating endothelial cells can transform into potential osteogenic precursor cells via endothelial-to-mesenchymal transition with bone morphogenic proteins (BMP-2, BMP-4) and transforming growth factor β playing a role in this transition.
-
2.
Immune cell-based pathway: Development of HO resulting from hyperinflammatory state and immunosuppression caused by burn injury is driven by circulating inflammatory cells and cytokines, where tumor necrosis factor α, interleukin 6 (IL-6), IL-1β, neutrophils, and monocytes increase while lymphocytes decrease. These changes were evident in a burn/tenotomy-induced HO mouse model. Monocytes and macrophages were noted as the main culprits that drive HO formation in response to inflammation.
-
3.
Muscle satellite cell-based pathway: Satellite cells possess the ability to proliferate and differentiate to repair muscle fibers after thermal injury. In addition, they have the ability to be osteoprogenitor cells through Rho signaling, switching from myogenesis to osteogenesis.
The dysregulation of calcium metabolism through burn-induced resorption was also mentioned as way to facilitate HO formation by depositing the excessive calcium. Other factors to be considered in the genesis of HO are percentage of burn, location of burn, period of confinement, osteoporosis, superimposed trauma, and genetic predisposition.
Percentage of burn effect on heterotopic ossification
Most reported cases of HO have had a 20% or greater total body surface area (TBSA) burn; however, it has been found in patients with as little as 10% third-degree burn. Peterson et al., Munster et al., and Elledge et al. have reported affected patients with TBSA burns of 8%, 14%, and 12%, respectively. Levi et al. analyzed data from nearly 3000 thermal injury patients and showed that patients with greater than 30% TBSA burns had 11 times higher odds of developing HO. Other studies have also implied that HO risk is strongly associated with increased burned TBSA. ,
Location of burn effect on heterotopic ossification
By no means has all of the reported HO occurred in joints with overlying burn. In their initial report, Evans and Smith described HO occurring a distance from any third-degree burn involvement. Johnston noted that in one of his three patients, the skin overlying one affected joint was not even superficially burned. If degradation of connective tissue milieu in burns is a total-body phenomenon, then it follows that heterotopic bone formation need not be burn-site dependent. Thus the location of the burn cannot alone be a determining factor.
Period of confinement effect on heterotopic ossification
Evans and Smith expressed the belief that length of bed confinement was an important factor in the development of HO. At the time of that report, patients with even moderate burns might be kept in bed for several weeks. The consequences of prolonged confinement were loss of active range of joint motion and bone demineralization; it was thought that each of these adverse changes might contribute to the formation of HO. Thus any maloccurrence that necessitated longer confinement could be a factor in pathogenesis. Kolar and Vrabec implicated wound sepsis as an independent factor, along with length of confinement. Other investigators have not addressed the period of confinement as specifically, and there have been no comparative studies of groups of confined and nonconfined patients. Thus it may never be determined whether the current aggressive practice of early mobilization of patients will have an effect on the incidence of heterotopic bone. We believe the incidence of HO is lower at our institution after the advent of early mobilization postoperative protocols.
Osteoporosis and heterotopic ossification
Only Schiele et al. have found a relation between HO and osteoporosis. Among their group of 70 adults with burns confined to the upper extremities, 11 of the 16 who developed HO had radiographically identifiable osteoporosis. In their series of patients, there were 24 with osteoporosis. Thus fewer than half of these developed HO, and there were two in the group who developed HO who did not have osteoporosis. If the findings in that study are not altogether persuasive, the matter is further confused by the knowledge that the survivors of extensive TBSA burns, who may develop profound osteoporosis, seem to have no greater liability to the formation of heterotopic bone than the general burn population.
Superimposed trauma on heterotopic ossification
In one of the patients reported by Evans and Smith, the elbow of the more often used and minimally burned right upper extremity developed HO, but the elbow of the less used, but more seriously burned, left upper extremity did not. In the same patient, the right hip spontaneously dislocated. After reduction, that hip developed extensive HO in the planes of the rectus femoris and iliopsoas. The opposite hip developed only a small, inoffensive spicule of HO anteriorly at the joint line. Experience with this one patient reinforced the authors’ belief that there occurs with burns a general compromise of connective tissue that renders it particularly susceptible to superimposed trauma and that it is this liability to injury that accounts for the appearance of HO at sites of repeated stretching of soft tissue, as at the minimally burned elbow or at sites of recognized abrupt excessive stretching, as with the dislocated hip. According to all reports, the elbow is the most common site of HO in adults and children. , , , Perhaps it is the regular use of this joint that accounts for that orientation. Jackson has pointed out that the elbows are subjected to pressure posteriorly and medially when they are used for leverage or are simply in contact with the bed. He suggests that external pressure is a factor in the orientation of HO to the elbow. There may be other factors that favor the elbow. Commonly, the elbow is splinted in extension to prevent flexion contracture. If flexion range is lost, passive stretching and encouragement of active flexion are part of the rehabilitation effort. The posterior structures most affected by this effort are those attached to the olecranon. HO often develops medially in line with and deep to the medial fibers of the triceps. If a flexion contracture develops, the HO is commonly in the line of brachialis or biceps attachments to coronoid process and biceps tubercle. And if there is loss of pronation and supination range, stretching may cause HO to form in line with the proximal radioulnar ligaments and interosseous membrane. There is an implication here that both the quality and timing of postburn exercise may be important. Gentle passive and active motion should cause less tissue disruption than abrupt passive, active, or even chronically repeated motion, and the effect of any mobilization effort must vary with the relative stiffness of the joint and the intrinsic resistance of soft tissue. The longer a joint is limited in its motion, the stiffer it will become and the greater the soft tissue damage will be with any forced manipulation.
The concept of superimposed trauma as a cause of heterotopic bone is supported by the experimental work of Evans and of Michelsson and Rauschning. Evans found that all burned and nonburned rabbits given a single necrotizing injection in one quadriceps muscle readily healed the lesions, but rabbits burned or nonburned that were given a second same-site injection 7 days after the first uniformly developed well-defined and histologically identifiable HO. In this experiment, it was clear that in susceptible animals, it was not the burn that made the difference, but the chronicity of the wound. Michelsson and Rauschning determined that forceful or regular active remobilization of rabbit knees that had been immobilized for 1 to 5 weeks resulted in the development of heterotopic calcification and ossification in the muscles that were stretched. The response was more consistent in the quadriceps of the knees immobilized in extension than in the hamstrings of those immobilized in flexion. The longer the period of immobilization and the more vigorous the remobilization, the greater the response was. Muscle necrosis was a prominent histologic finding.
Superimposed trauma is implicated in the development of HO in head-injured patients or those with posttraumatic or infectious transverse myelitis. In these patients, it is assumed that tissue media are altered by injury to the central nervous system. The secondary injury, as in burns, is periarticular. In posttraumatic myositis ossificans, the development of HO depends on persistence of the muscle lesion and local necrosis and thus, at least by inference, on repeated insults to the affected muscle.
The development of HO in burns has been associated with the agitation of patients and their resistance to physical therapy. , Two affected adults and one affected child in a 10-year study resisted physical therapy programming. One adult refused to move, and the other was extremely apprehensive. The child was likewise apprehensive and refused to cooperate with the therapist. The development in all three of posterior HO in both elbows could have been ascribed both to the difficulty encountered in mobilizing the elbows and to the continual pressure on the elbows in bed.
Genetic predisposition to heterotopic bone
It is difficult to explain the low incidence of HO among great numbers of patients similarly burned, except on the basis of some currently unidentified, inherited factor. It is known that persons with proliferative noninflammatory arthritis of the hip are more likely to develop HO after total hip replacement than persons who have hips replaced for other reasons. In this instance, the predisposing inherited abnormality is identifiable. Although HO formation may occur more regularly among patients with spinal cord injuries and head injuries than among burn patients, by no means do all persons with head and spinal cord injuries develop HO. The total burn experience at the University of Texas Medical Branch has yielded only two similarly affected siblings. Twin brothers who had 19% and 20% TBSA burns and who were mobile throughout much of their treatment and recovery period developed near-identical HO of both elbows. There is, however, no scientific proof that genetic predisposition has anything to do with the formation of HO in burns. Nor is there any literature to support the idea that a person who develops HO when burned will be liable to develop it if sustaining head or spinal cord injury. Vrbicky, in a comprehensive review of postburn HO formation, suggests that a key for the genetic predisposition may be in the human leukocyte antigen (HLA), reporting that an HLA B27 survey showed a 7% HLA distribution in the normal population compared with 70% in a population with HO.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree