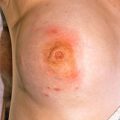
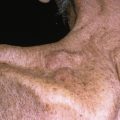
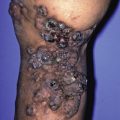
Morbilliform eruptions are eruptions that resemble measles. The term is derived from the Latin word for measles, morbilli. Morbilliform reactions are never due to external factors and always indicate an internal problem; the most important are viral and drug reactions, and connective tissue disorders are a distant third.
Important History Questions
How long have your spots been present?
Most morbilliform eruptions present acutely (e.g., morbilliform drug eruptions, morbilliform viral eruptions, rickettsial infections), whereas some disorders, such as lupus erythematosus, are more likely to be chronic or recurrent.
Have you started any new medications in the last 10 days?
This is a very important question, because a morbilliform drug eruption is a common cause of this pattern. Oral antibiotics are the most common cause of morbilliform reactions.
Have you had any fever?
This question is directed toward determining a potential infectious cause, such as a viral or rickettsial infection.
Do you have any other medical problems?
This question can produce an abundance of important clinical information, including a history of a connective tissue disorder or mononucleosis. Mononucleosis is notorious for producing morbilliform reactions when the patient has been given ampicillin.
Important Physical Findings
What is the distribution of the lesions?
Most morbilliform eruptions do not have a characteristic distribution; however, some, such as Rocky Mountain spotted fever, tend to start acrally, whereas unilateral thoracic exanthem, as the name implies, typically is predominantly unilateral at its initial presentation.
Presence or absence of lesions in the oral mucosa
Oral lesions are more frequently seen in some but not all morbilliform viral eruptions and are usually absent in morbilliform drug eruptions and rickettsial infections.
Are any blisters present?
Morbilliform eruptions, by definition, do not have blisters; however, it is important to remember that some eruptions may initially appear to be morbilliform (e.g., very early erythema multiforme) before they blister. Obviously, if blisters are present, the differential diagnosis and thought process change.
Do any of the lesions demonstrate hemorrhage?
Focal hemorrhage, especially minute areas of hemorrhage on the lower extremities, can occur in morbilliform viral and drug eruptions. The presence of hemorrhage obviously raises the possibility of Rocky Mountain spotted fever or even a very early leukocytoclastic vasculitis.
Do any of the lesions demonstrate a reticulated (netlike) appearance?
A morbilliform eruption with a reticulated appearance should raise the possibility of erythema infectiosum; however, reticulated patterns are not specific and may occasionally be seen in other morbilliform eruptions.
Morbilliform Drug Eruptions
ICD10 code L27.0
DRUG ERUPTION
Pathogenesis
The pathogenesis of a morbilliform drug eruption is not understood, and very little research has been directed toward resolving the mechanism(s) involved. The frequent development of morbilliform drug eruptions precipitated by ampicillin in a patient with Epstein-Barr virus infection and by sulfonamides in a patient with HIV infection suggests that an altered immune system may be important in some cases. This might explain why not all patients develop a morbilliform reaction when rechallenged later. An older study has demonstrated antipenicillin antibodies, an interesting finding, but one that has not been verified by other studies.
- •
Ampicillin
- •
Allopurinol
- •
Penicillin
- •
Phenytoin (Dilantin)
- •
Sulfonamides
Clinical Features
- •
Morbilliform drug eruptions typically begin 3 to 10 days after administering the offending drug.
- •
In most cases, lesions are primarily located on the trunk.
- •
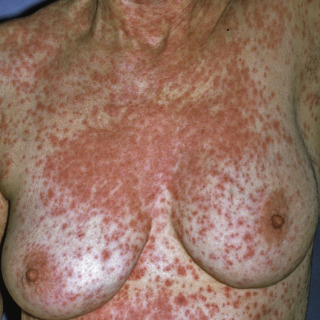
The primary lesion is a 1- to 10-mm blanchable macule that can demonstrate coalescence into large patches of erythema ( Figs. 3.1–3.3 ).
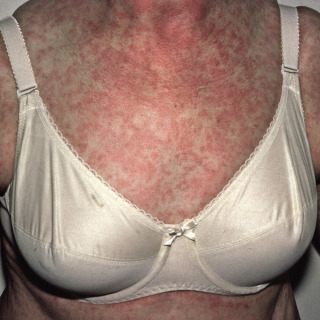
Fig. 3.1
Morbilliform drug eruption due to a sulfonamide antibiotic.
(From the Fitzsimons Army Medical Center Collection, Aurora, CO.)
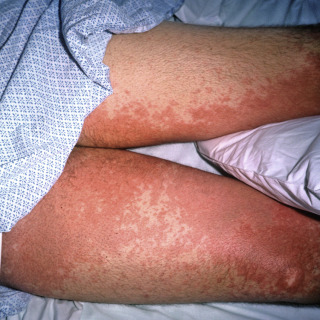
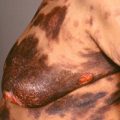
Fig. 3.2
Morbilliform drug eruption secondary to penicillin.
(From the William Weston Collection, Aurora, CO.)
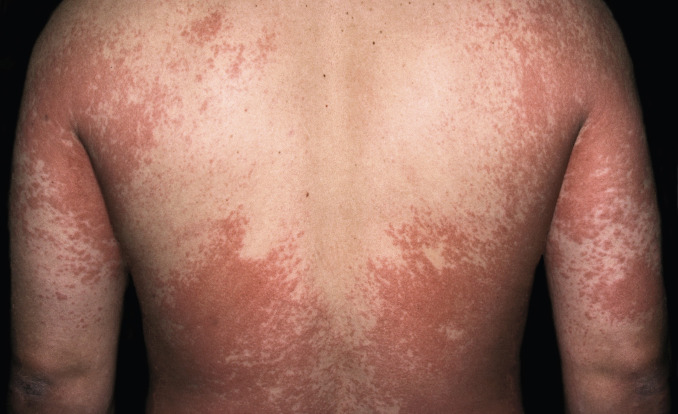
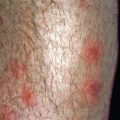
Fig. 3.3
Morbilliform drug eruption due to oral penicillin. Note the focal confluence of macules into the patches of erythema.
(From the Fitzsimons Army Medical Center Collection, Aurora, CO.)
- •
Symptoms range from absent to significant pruritus.
- •
Lower extremity lesions may demonstrate focal hemorrhage.
Serum Sickness
Morbilliform reactions may also be a component of serum sickness. Serum sickness is characterized by a cutaneous eruption (urticaria, morbilliform dermatitis, and purpura or erythema multiforme), fever, joint involvement (arthritis or arthralgias), edema, and lymphadenopathy.
Diagnosis
- •
Drug exposure history is critical. The exposure period of interest is usually 3 to 10 days, but occasional cases may fall outside of this range.
- •
Skin biopsies typically demonstrate a superficial perivascular lymphocytic dermatitis. This pattern is not diagnostic and can be seen in other morbilliform reactions, including viral morbilliform exanthems, which can be clinically identical. Most cases do not require a biopsy. If a biopsy is needed, always do a 3- or 4-mm punch biopsy, never a shave biopsy.
- •
Check a complete blood count (CBC). An elevated eosinophil count favors a drug eruption, and a very high eosinophil count may suggest a severe drug hypersensitivity reaction, a drug reaction with eosinophilia and systemic symptoms (DRESS).
- •
Liver function tests (LFTs) should be ordered when DRESS is a clinical consideration.
Treatment
- •
Discontinue the offending medication. Although cases may resolve with continuation of the drug, occasional cases demonstrate continued progression to full body erythema.
- •
Use symptomatic treatment measures, such as sedating antihistamines (e.g., diphenhydramine), in patients who are markedly pruritic. There is no evidence to suggest that the clinical course is altered or shortened by antihistamines.
- •
Rare cases may require topical corticosteroids or a brief course of oral corticosteroids.
Clinical Course
In most cases, the reaction will start to subside within 1 to 3 days and be completely resolved in 7 to 10 days.
 Drug Eruption With Eosinophilia and Systemic Symptoms
Drug Eruption With Eosinophilia and Systemic Symptoms
ICD10 code L27.0
DRUG ERUPTION
Pathogenesis
The pathogenesis of DRESS is not understood, but it is clearly an immunologically mediated hypersensitivity syndrome. The eosinophils are thought to be related to interleukin-5 released by stimulated T cells. This constellation of findings has also been referred to as drug hypersensitivity syndrome .
- •
Allopurinol
- •
Carbamazepine (Tegretol)
- •
Lamotrigine
- •
Minocycline
- •
Phenobarbital
- •
Phenytoin (Dilantin)
- •
Piperacillin-tazobactam
- •
Salazopyrin
- •
Sulfasalazine
- •
Trimethoprim
- •
Valproic acid
Clinical Features
- •
Clinical features typically begin 1 to 8 weeks after starting the drug.
- •
Lesions are located on the face, trunk, and extremities, primarily on the trunk in many cases.
- •
Early primary lesions are 1- to 10-mm blanchable macules that quickly coalesce into large patches of erythema ( Figs. 3.4–3.6 ).
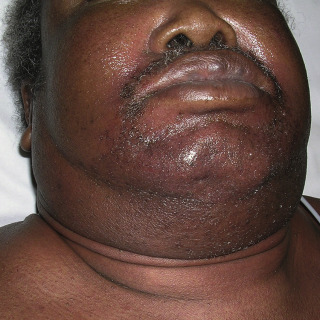
Fig. 3.4
Patient with DRESS demonstrating characteristic facial erythema and edema.
(Courtesy Dr. Tim Chang.)
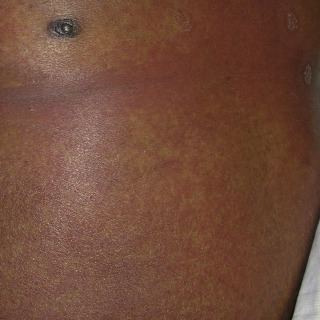
Fig. 3.5
Patient with DRESS demonstrating macular erythema of the trunk.
(Courtesy Dr. Tim Chang.)
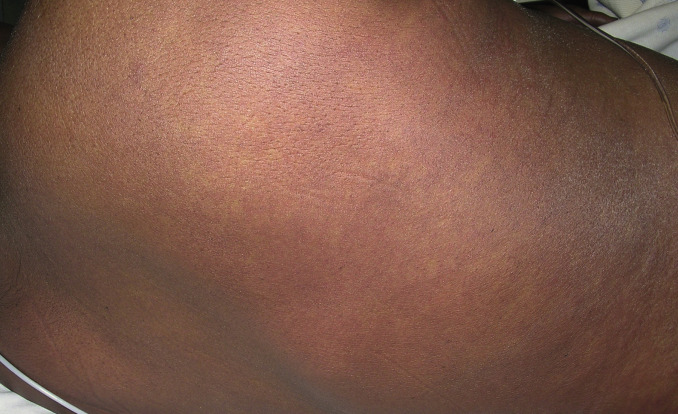
Fig. 3.6
Patient with DRESS with confluent truncal macular erythema.
(Courtesy Dr. Tim Chang.)
- •
Facial (hallmark of the disease) and limb edema are frequently present (see Fig. 3.4 ).
- •
Symptoms range from being absent to significant pruritus.
- •
Clinical variations include primary lesions that are pustular, bullous, or purpuric.
- •
Lymphadenopathy is frequently present.
- •
On the CBC, eosinophilia may be profound, with variable numbers of atypical lymphocytes.
- •
Hepatitis may be mild to severe and potentially fatal.
- •
Other organ systems that may be involved include the brain, lungs, heart, and kidneys.
Diagnosis
- •
A drug exposure history is critical. The exposure period of interest is usually 2 to 6 weeks before the onset of the eruption, but occasional cases may fall outside of this range.
- •
A 3 or 4 mm punch biopsy (never a shave biopsy) will demonstrate nonspecific findings. It typically demonstrates a superficial perivascular lymphocytic dermatitis, with variable numbers of eosinophils. A biopsy may help exclude other diseases.
- •
A minimal initial laboratory evaluation would include LFTs and a CBC, with a differential diagnosis.
Treatment
- •
The offending or suspected offending medications should be discontinued immediately. Although cases may resolve with continuation of the drug, occasional cases demonstrate continued progression to full body erythema and a fatal outcome.
- •
Oral corticosteroids, at a dose of 40 to 60 mg/day, is the treatment of choice. Therapy may need to be maintained for weeks or even 1 month or longer.
Clinical Course
The mortality rate has been reported to be as high as 10% in untreated patients.
Morbilliform Viral Eruptions
ICD10 code B09
VIRAL INFECTION
Pathogenesis
There are many different viruses that produce morbilliform (measles-like) viral exanthems. Most are not clinically distinct, although some are distinct enough that they can be discussed separately (e.g., roseola, erythema infectiosum). Morbilliform reactions may be produced by viral infections of the host cells or may be due to the host response.
- •
Adenovirus
- •
Coxsackie virus
- •
Erythema infectiosum
- •
Measles
- •
Respiratory syncytial virus
- •
Roseola
- •
Rubella virus
- •
West Nile virus (morbilliform eruption in 50%)
Clinical Features
- •
Viral exanthems most commonly affect infants and children but can affect those at any age, including geriatric patients.
- •
Viral exanthems are frequently but not always associated with other findings of a viral syndrome, such as a prodrome of malaise and fever or active oral mucosal infection (sore throat, rhinorrhea) or gastrointestinal infection (abdominal pain, diarrhea). Measles is typically associated with coryza, conjunctivitis, and cough.
- •
The primary lesion—pink to red macules or subtle papules—may vary in size from 1 mm to more than 1 cm.
- •
Variations include petechial or vesicular lesions.
- •
Rubella lesions are often rose pink rather than erythematous.
- •
The distribution is typically generalized and often spares the palms and soles ( Figs. 3.7–3.10 ).
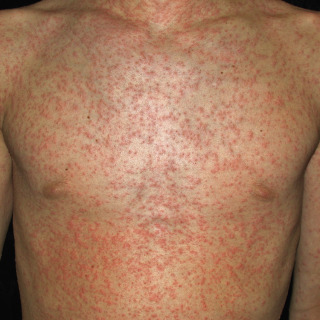
Fig. 3.7
Patient with papular viral exanthema of an unknown viral type affecting the trunk and extremities.