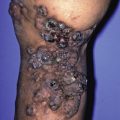
Follicular disorders represent pathologic processes that alter or otherwise inflame the pilosebaceous (follicular) unit. Alopecias are also follicular disorders but are considered elsewhere in this text. Numerous disorders can affect the follicle, including infections, disorders of keratinization, some neoplasms (e.g., follicular mycosis fungoides), genodermatoses, and other inflammatory disorders. The following questions are important to ask during the evaluation of follicular disorders.
Common
- •
Acne vulgaris
- •
Dermatophytic folliculitis
- •
Drug-induced acneiform disorders
- •
Keratosis pilaris
- •
Neonatal acne
- •
Pityrosporum folliculitis
- •
Rosacea
- •
Staphylococcal folliculitis
Uncommon
- •
Eosinophilic folliculitis
- •
Follicular atopic dermatitis
- •
Follicular mycosis fungoides
- •
Lichen spinulosus
- •
Perioral dermatitis
- •
Pseudomonal folliculitis
- •
Viral folliculitis
Important History Questions
How long has the follicular alteration been present?
It is helpful to determine if the condition is acute or chronic. For example, acne vulgaris, keratosis pilaris, and follicular atopic dermatitis are typically chronic disorders, whereas drug-induced acneiform eruptions and pseudomonal folliculitis are acute events.
Have you started any new medications in the past month?
This question is most relevant to drug-induced acneiform eruptions. Oral corticosteroids, androgens, isoniazid, lithium, and some birth control medications can cause medication-induced acne.
Are you putting anything on the skin of the affected area?
Many patients use home remedies, over-the-counter remedies, or even prescription remedies, which can worsen follicular disorders. For example, some patients with acne use comedogenic cosmetic products that aggravate the condition. Mistaken or misguided use of topical corticosteroids can also aggravate acne vulgaris and rosacea, cause perioral dermatitis, or complicate dermatophyte infections.
Have you recently used a hot tub or hot springs pool or had some other immersive water exposure?
This question is pertinent when the clinical differential diagnosis includes Pseudomonas folliculitis.
Important Physical Findings
What is the distribution of the follicular disorder?
Some follicular disorders have characteristic distributions. Acne vulgaris usually involves the face and upper trunk, whereas rosacea is typically confined only to the face. Pseudomonas folliculitis is almost always truncal and is most prevalent beneath areas that were covered by a bathing suit.
Is there a distinct pattern to the dermatitis?
Some follicular disorders are grouped (e.g., lichen spinulosus) or dermatomal. Grouped erythematous follicle-situated papules or vesicles, in a dermatomal pattern, lead to consideration of herpes zoster.
Are other mucocutaneous findings present?
Some follicular disorders have other cutaneous findings that suggest the diagnosis. For example, rosacea often has background erythema, telangiectasias, or ocular findings, whereas pseudomonal folliculitis may be associated with mastitis, conjunctivitis, otitis externa, or pharyngitis.
Is a pustular component present?
Some follicular disorders, such as lichen spinulosus or follicular eczema, are almost never pustular, whereas staphylococcal folliculitis or pseudomonal folliculitis often demonstrate follicle-centered pustules.
Acute Vulgaris
ICD10 code L70.0
INTERNAL DISEASE
Pathogenesis
Acne is a multifactorial disorder. Abnormal follicular maturation, in response to an altered hormonal milieu, leads to follicular plugging and retained sebum. This results in the overgrowth of a commensal bacteria called Propionibacterium acnes. The bacterium elaborates proinflammatory mediators, and follicular rupture leads to the liberation of proinflammatory free fatty acids into the dermis. The result is a classic “zit.” Follicular plugging alone causes comedones (blackheads, whiteheads). This concept of acne as a multifactorial disorder is important because treatment may be directed against any of these contributing factors. Ergot, agents that prevent comedone formation, reduce sebum production, decrease bacterial growth, or blunt the proinflammatory response, may improve the condition.
Clinical Features
- •
Acne typically begins during puberty (after andrenarche).
- •
Acne is usually distributed on the face (most common site), neck, and upper chest or back.
- •
Acne typically causes the following:
- •
Comedones (blocked pores), which may be open (blackheads; Fig. 23.1 ) or closed (whiteheads)
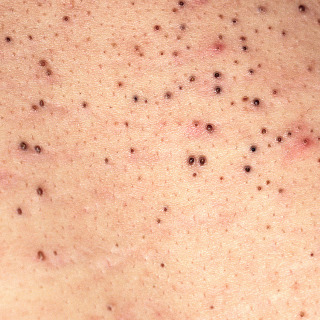
Fig. 23.1
Open comedones (blackheads) on the back of an adolescent male with acne.
- •
Erythematous follicle-based papules
- •
Follicle-based pustules and nodules
- •
Acneiform epidermoid cysts (see Fig. 34.2 )
- •
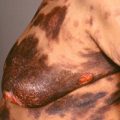
Scarring may develop at sites of marked follicular inflammation or follicular rupture; this may result in substantial residual pigmentary changes, particularly in persons with darker skin.
- •
Diagnosis
- •
Acne is almost always a clinical diagnosis; often it has already been diagnosed by the patient.
- •
Women with male pattern hair growth on the face or genitals, early-onset alopecia, cliteromegaly, severe acne, and other signs of hirsutism warrant an endocrine evaluation.
Treatment
- •
Mild acne (primarily comedonal acne)
- •
Mild comedonal acne can be treated with a topical retinoid or azelaic or salicylic acid.
- •
Mild inflammatory acne with papular and/or pustular elements can be treated with a topical retinoid and topical benzoyl peroxide.
- •
- •
Moderate acne (substantial comedones and/or a papular or pustular component)
- •
This can be treated with topical retinoid plus benzoyl peroxide and/or a topical antibiotic (including combination agents with benzoyl peroxide and erythromycin or clindamycin).
- •
This can be treated with a topical retinoid plus topical benzoyl peroxide plus an oral antibiotic. Topical or oral antibiotic monotherapy is not recommended for more than 12 weeks to prevent the development of bacterial resistance.
- •
- •
Severe acne (nodulocystic, with scarring or the potential to scar; see Fig. 23.2 )
- •
Systemic isotretinoin
- •
Hormonal therapy in women
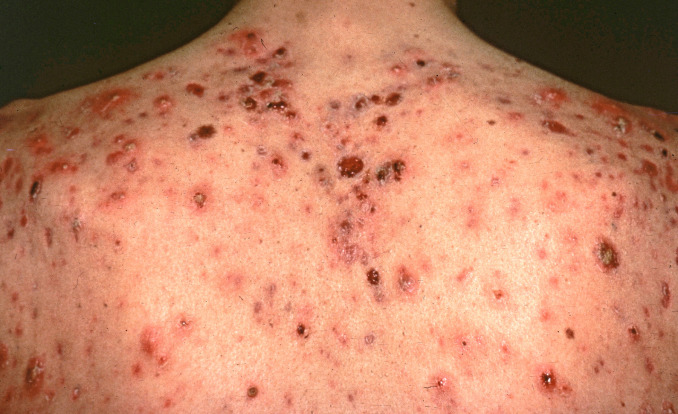
Fig. 23.2
Patient with severe acne with follicular papules, follicular pustules, and acneiform cysts. This will produce permanent scarring, and the patient is a strong candidate for systemic isotretinoin.
(From the Fitzsimons Army Medical Center Collection, Aurora, CO.)
- •
- •
Antibiotic selection depends on a number of variables, including cost. Although most dermatologists consider minocycline to be superior to doxycycline due to better penetration into the sebaceous unit, it is generally more expensive and sometimes associated with drug-induced lupus. Minocycline and doxycycline are both considered superior to simple tetracycline.
Clinical Course
The clinical course of acne is capricious. Some adolescents have mild disease that resolves quickly, whereas others progress to severe acne with scarring. Acne may persist for years or decades, especially in women. Acne is generally not a problem of late middle or older age, and occurrence in this age group should prompt investigation for an instigating agent (e.g., endocrine abnormality, drug effect).
A single-blinded, randomized, controlled clinical trial of 27 men was carried out for 6 weeks using a foaming facial cleanser that had no active antiacne properties. They were randomized to groups that washed once, twice, or four times daily. At the end of the study, no statistically significant differences among the three groups were realized, although the group that washed twice daily subjectively demonstrated slight improvement. The authors concluded that there is some evidence for washing the face twice daily.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree