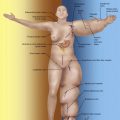
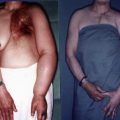
Key Points
- ▪
The vascularized lymph node flap transfer from the groin was first introduced by Clodius in 1982 in two clinical cases.
- ▪
Animal studies described the vascularized lymph node flap as an effective technique for the treatment of lymphedema prior to most clinical studies.
- ▪
The vascularized groin lymph node can be independently transferred to the axilla, elbow, and wrist with promising results.
- ▪
The vascularized groin lymph node can be transferred to the axilla with the low abdominal flap, either the deep inferior epigastric perforator (DIEP) flap or the modified DIEP with nodes, without muscle.
- ▪
The vascularized groin lymph node flap has the advantages of a great number of lymph nodes, rich natural lymphaticovenous connection for drainage of lymph from surrounding interstitial tissue, and a hidden donor site scar. However, it has the disadvantages of potential donor site lymphedema, bulky flap for inset, and poor cosmesis if transferred to distal recipient sites.
Introduction
The tissue containing lymphatic ducts from the arm as a large tubed ‘waltzing’ flap was first introduced by Sir Harold Gillies as a lymphatic wick to treat lower limb lymphedema as early as 1935. In 1979, Shesol et al. successfully restored lymphatic function with the transfer of a pedicled groin lymph node flap to the popliteal area in a rat model. Clodius et al. observed the lymphatic system in the groin flap and clinically reported the first pedicle ‘lymph-bearing’ groin flap transfer and the first vascularized ‘lymph-bearing’ groin flap with partially successful results. They also proposed that the physiologic lymphatic catchment area is essential for the drainage of maximum lymphatic load on the lymphedematous limbs. Later, Becker et al., followed by Chen et al., successfully performed a vascularized lymph node transfer in an animal model. As the radiation treatment for the breast cancer patient significantly increased, the sequelae of postmastectomy-related upper limb lymphedema also proportionately increased up to 40–50%. These landmark studies laid the foundation for study in lymph node transfer and lymphovenous shunting procedures.
Although Clodius shed light onto the treatment of lymphedema in the early nineties, there were few clinical case reports since, until Becker et al. published a series of long-term follow-up vascularized groin lymph node (VGLN) transfer to axilla and elbow in 2006. Becker et al. described that functional vascularized lymph node transplantations can drain lymphatic fluid in patients with postmastectomy upper limb lymphedema. It was later described by Cheng et al. that transferring the VGLN flap with a skin paddle to the dependent, distal site had promising results for providing a new pathway for lymphatic fluid drainage. The outcome of the different recipient sites including axilla, elbow and wrist are currently debated. As a result, more and more clinical series have been reported using the VGLN flap allowing for technical and conceptual refinements in lymphatic microsurgery.
The VGLN can be modified and transferred for the upper limb lymphedema simultaneously with the lower abdominal flap transfer for breast reconstruction with upper limb lymphedema. Although there are some controversies for the patient selection, the VGLN remains the preferred choice in International Society of Lymphology (ISL) stage 2–3 breast cancer-related lymphedema. This chapter will discuss the groin lymph node anatomy, patient selection, various techniques for VGLN flap harvest, and the available recipient sites for flap transfer.
Concepts
Regional Anatomy
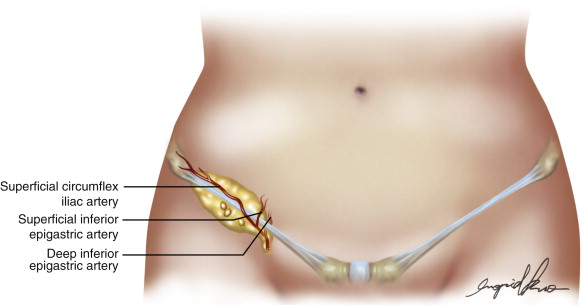
Traditional anatomic descriptions address the most superficial groin (inguinal) lymph nodes located in the femoral triangle of Scarpa—inferior to the inguinal ligament, medial to the sartorius muscle and lateral to the adductor longus. Based on Assouad’s study in 2002, the superficial groin nodes mainly drain the lymph fluid from lower abdomen and it is this group of lymph nodes can be sacrificed and transferred as a vascularized flap to drain the lymphedematous limb. A recent cadaveric dissection for the vascularized groin lymph node flap was reported by Cheng et al., illustrating that there were on average 6.2 sizable superficial groin lymph nodes and were distributed in two groups: a superior row based on the superficial circumflex iliac artery ( Figure 14.1 ), and a medial column based on the medial artery directly originated from the common femoral artery. Dayan et al. further investigated the groin lymph node characteristics and a mean of 8.2 lymph nodes can be found 3 cm below the inguinal ligament and above the groin crease, centered one-third the distance lateral to the pubic tubercle along the inguinal ligament. The study further found that most nodes are found in three locations: the junction of the superficial inferior epigastric vein (SIEV) and superficial circumflex iliac vein (SCIV) (67%), medial to the SCIV (19%), and inferior to the SCIV (14%). Understanding the anatomy of the superficial groin lymph nodes is of extreme importance and is the key to the success of VGLN flap harvest and avoidance of significant donor site morbidity.
Flap Design
The original design described by Clodius was that of the traditional groin flap design with the inclusion of lymphatic tissue. From the understanding the regional anatomy, this flap design may include few or even no lymph nodes, which may be responsible for the original study reporting partial success. The VGLN flap design can be divided into four types according to the published literature. The vascularized groin lymph nodes can be harvest with a skin paddle or without a skin paddle. When the skin paddle is harvested with the vascularized lymph nodes, the composite flap is more appropriately termed a vascularized groin lymph node flap.
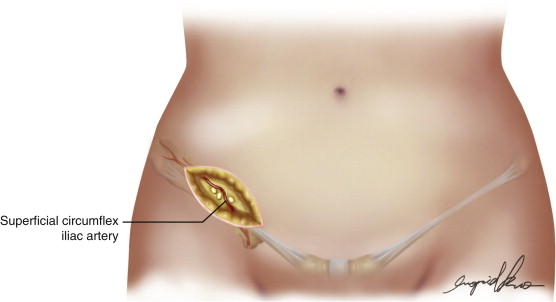
There are four common flap designs to harvest the groin lymph nodes, but only one is favored by the author ( Figure 14.2 ), as follows: The skin incision is made 1.5 cm above the inguinal ligament ( Figure 14.2 ). The superficial circumflex iliac artery (SCIA) and SCIV are identified and looped. The soft tissue around the vein is included and the dissection is continued to the origin of the SCIV, which usually has a common origin with the SIEV. The great saphenous vein is usually preserved since it is not the main drainage of the superficial inguinal lymph nodes.
Patient Selection
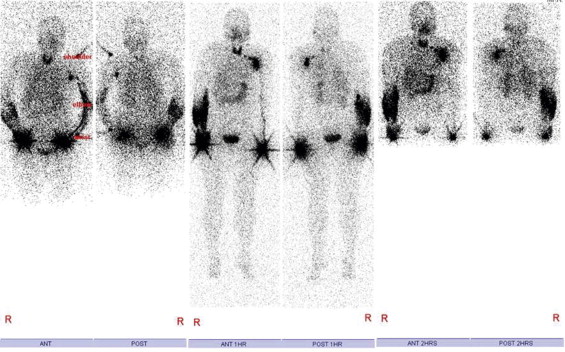
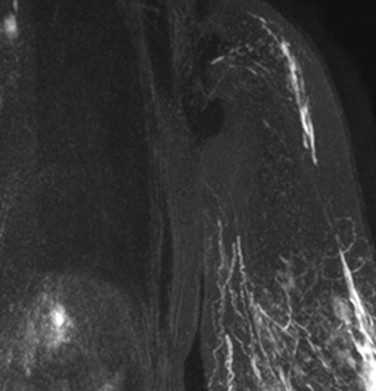
The VGLN flap is suitable for lymphedema stages I–III, even elephantiasis; lymphedema with pain and palsy; lymphedema with chronic infections; lymphedema cases where there is a desire to do the breast at the same time; and lymphedema where there is marked fibrosis in the axilla. Indications of VGLN flap transfer for upper limb lymphedema include total proximal occlusion on lymphoscintigraphy ( Figure 14.3 ) or magnetic resonance lymphangiography ( Figure 14.4 ), failure to complex decongestive treatment and recurrent cellulitis for six months. The contraindications for VGLN flap transfer are local cancer recurrence or distal metastasis. Some patients with brachial plexus neuritis are relative contraindications, but improvements with regional decompression and flap transfer can greatly enhance patients’ quality of life.
Preoperative Considerations
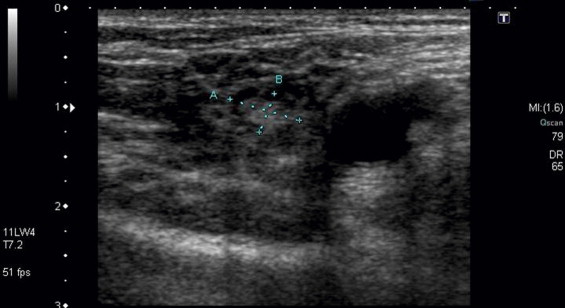
When the VGLN flap is indicated for transfer for the treatment of upper limb lymphedema, the available quantity of lymph nodes in the groin area is one of the most important factors predicting success. Duplex ultrasonography can be used to detect sizable (greater than 0.5 mm in diameter) lymph nodes ( Figure 14.5 ) or an MRI can be used to completely survey the groin lymph nodes in great detail. Duplex ultrasonography is a cheap, easy, and less time consuming (30 minutes) imaging modality. The MRI is more accurate, expensive, and is more time consuming (3–4 hours). Once the quantity and location of available lymph nodes is confirmed, the groin site may be chosen and flap design can be made accordingly.