16 Management of Thyroid-Related Eyelid Retraction
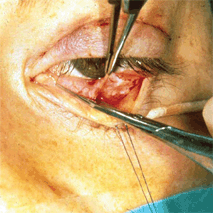
Retraction of the eyelids is one of the most common ophthalmic manifestations of Graves’ disease. This malposition may occur with or without exophthalmos and is responsible for functional and cosmetic problems in many patients with thyroid-related eye disease. The etiology of eyelid retraction in Graves’ disease is not clearly understood, but several factors seem to be contributory. In the upper lid, these factors include (a) Müller’s muscle overaction from sympathetic stimulation, (b) levator contraction from degeneration and thickening of the levator muscle or the aponeurosis, (c) levator adhesions to the orbicularis muscle and orbital septum, and (d) overaction of the levator–superior rectus complex in response to a hypophoria produced by fibrosis and retraction of the inferior rectus.
In the lower eyelid, adrenergic stimulation of the Müller’s muscle plays a smaller role, but fibrosis of the inferior rectus exerting a retraction action on the lower eyelid through its capsulopalpebral head appears to be more influential.
SURGICAL INDICATIONS
Surgical treatment of eyelid retraction is usually reserved for patients whose endocrine status and eyelid height have been stable for at least 6 months to 1 year, and in whom retraction causes significant exposure keratopathy, lagophthalmos, chronic conjunctival injection, and cosmetic imperfection.
Several surgical procedures have been described to bring the retracted upper eyelid downward. These included levator tenotomy or recession, Müller’s muscle resection or myectomy, and combined levator tenotomy and mullerectomy. However, the aponeurotic approach described by Harvey and Anderson (1981) is preferred because it is anatomically, surgically, and physiologically sound. In this technique, the Müller’s muscle is completely extirpated, the lateral horn of the levator severed, and the aponeurosis recessed. Additionally, this anatomic approach is similar to that used in aponeurotic ptosis surgery.
Upper eyelid
Local anesthesia is preferable whenever feasible. This permits lid height, contour, and symmetry to be adjusted intraoperatively. A full-face preparation is given, and the head is draped with 3-M 1,000 surgical drape. The use of an open-face adhesive drape allows the patient to sit up in the middle of the surgery for lid height adjustment, without having to constantly adjust any loose head drape during this maneuver.
The normal skin crease is marked with a fine-tipped marking pen. For unilateral retraction cases, the skin crease is marked to correspond with the natural crease contour of the contralateral upper eyelid. Topical tetracaine may be instilled into the upper cul-de-sac intermittently throughout the procedure. Subcutaneous infiltration of lidocaine 2% with 1:100,000 epinephrine is given along the preplaced marking with a 30-gauge needle. The anesthetic solution should be delivered slowly to minimize patient discomfort, and no more than 1.5 ml is needed. A swollen lid will render fine lid height and contour adjustments suboptimal later on in the procedure.
A 4–0 double-armed silk traction suture is placed in the central margin of the upper lid and anchored to the surgical drape inferiorly with a hemostat. The needle is passed through the tarsal plate in a lamellar fashion, avoiding the marginal arcade and preventing unnecessary bleeding. When secured inferiorly, this traction suture puts all lid structures posterior to the orbicularis on stretch, while allowing the overlying skin and orbicularis to be mobilized. The skin is incised along the preplaced lid crease marking with a scalpel. All bleeding points are cauterized with a bipolar cautery.
The skin and orbicularis are grasped with a forceps on both sides of the incision centrally.
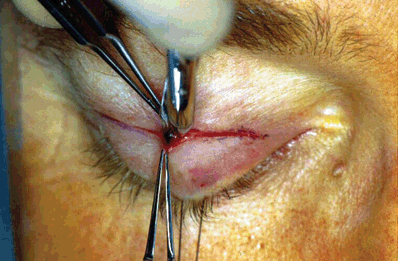
Figure 16-1. The orbicularis is tented anteriorly as far as possible from the posterior structures, and a full-thickness vertical incision of the muscle is made with a Westcott scissors.
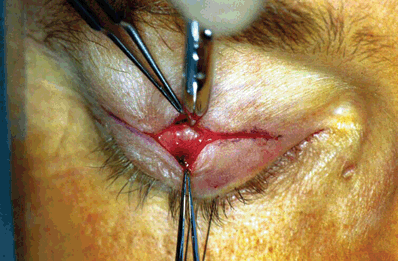
Figure 16-2. A full-thickness incision through the orbicularis muscle places one at the avascular postorbicular fascial plane, where the shiny surface of the orbital septum can be seen. Bleeding from the muscle layer should be cauterized immediately so that this important tissue plane is not obscured.
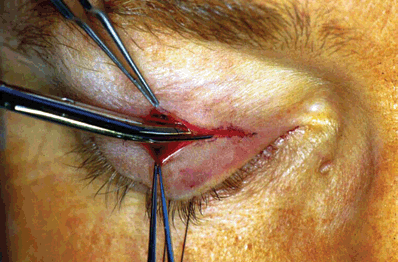
Figure 16-3. One blade of a scissors is passed bluntly in this plane medially and laterally to open the full length of the incision.
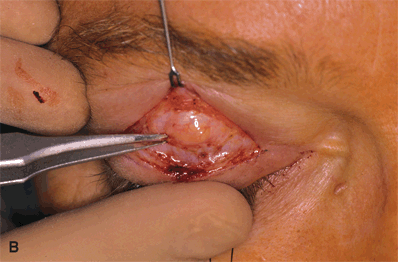
Figure 16-4A and B. The lid margin suture is then released and gentle retrograde digital pressure is applied onto the globe to prolapse the preaponeurotic fat pad. The yellowish fat pad can be seen bulging forward and distending the overlying thin, translucent orbital septum. The tip of the instrument is pointing at an intact orbital septum, with its attachment to the aponeurosis. A horizontal snip with scissors directed perpendicularly is used to buttonhole the orbital septum above its fusion with the aponeurosis.
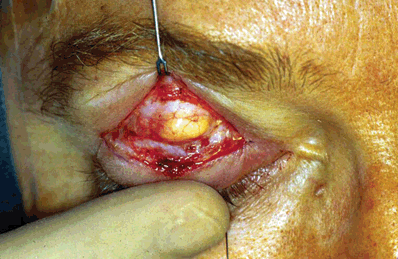
Figure 16-5. This allows the yellow preaponeurotic fat with its intact capsule to herniate through the buttonhole. The preaponeurotic fat pad is a key anatomic landmark to identify in this procedure. The entire orbital septum is opened by placing one blade of a Westcott scissors behind the septum and extending the incision medially and laterally. Incision of the septum should always be made over a bulging fat pad, using it to insulate the scissors from making iatrogenic defects in the aponeurosis.
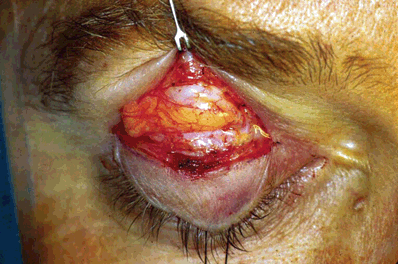
Figure 16-6. With the skin edge retracted superiorly, the full expanse of the preaponeurotic fat is displayed.
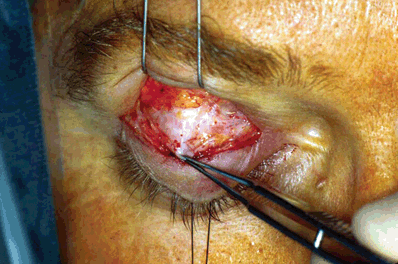
Figure 16-7. The preaponeurotic fat is gently teased away from the underlying white glistening structure with a cotton-tipped applicator. This structure, located immediately beneath the fat pad, is the levator aponeurosis. The forceps is grasping this structure. Grasping the glistening tissue with a forceps and asking the patient to look down and up can easily confirm the structure of the mobile, force-generating levator aponeurosis. The Whitnall’s ligament can be identified at the superior limit of the aponeurosis. Once the entire fat pad has been dissected free from the aponeurosis, it is retracted superiorly with a self-retaining Jaffe retractor to expose the shiny anterior surface of the levator aponeurosis.
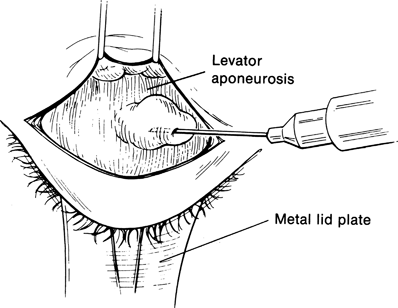
Figure 16-8. A metal lid plate is inserted into the superior fornix to protect the globe, while local anesthetic is injected under the levator aponeurosis with a 30-gauge needle to hydraulically separate the aponeurosis from Müller’s muscle. One should avoid infiltrating the anesthetic too close to Whitnall’s ligament or into the levator muscle, as paresis of the levator will affect the outcome of lid height adjustment later on.
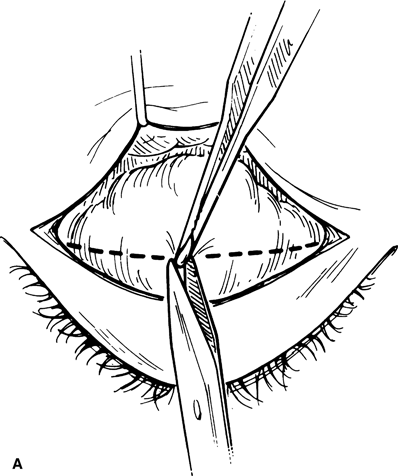
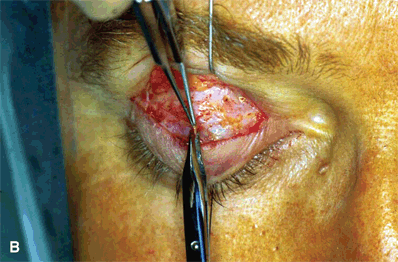
Figure 16-9A and B. A snip incision of the aponeurosis is made at the superior margin of the tarsal plate to expose a distinct tissue plane between the aponeurosis and the anterior surface of Müller’s muscle. One blade of a Westcott scissors is passed bluntly in this plane medially and laterally to sever the attachment of the aponeurosis from the tarsal plate. Sharp dissection is used to fully detach the undersurface of the aponeurosis from Müller’s muscle. Care is taken not to buttonhole the aponeurosis. Blunt dissection within this tissue plane is discouraged, since it may cause dehiscence of the aponeurosis.
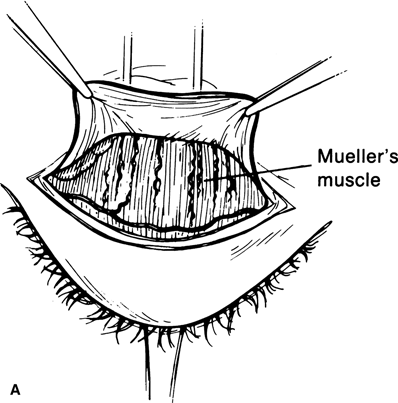
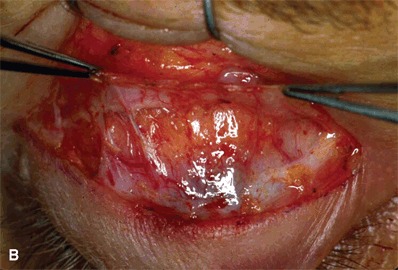
Figure 16-10A and B. With forceps lifting up the aponeurosis, the peripheral arcade of vessels is seen in Müller’s muscle just above the tarsal border. Müller’s muscle can be seen as a thin vascular structure with vertically oriented muscle fibers inserting onto the superior border of the tarsal plate. Frequently, fatty infiltration and fibrosis of the muscle are seen in patients with Graves’ disease. Bleeding from Müller’s muscle is usually moderate because of the highly vascular nature of the tissue. It should be stopped immediately, with pinpoint cautery, before proceeding with further dissection. Meticulous hemostasis is critical at this juncture of the procedure, as uncontrolled bleeding will obscure this tissue plane and make further dissection more difficult. To avoid thermal damage to the cornea, one must lift the tissue off the globe with the bipolar tip, before cauterizing.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree