Management of Diabetic Foot Ulcers
Rahim Nazerali
DEFINITION
Foot ulcers are the most common complication affecting patients with diabetes mellitus.1
A result of lower extremity neuropathic disease, trauma, and deformity.
May be compounded by ischemia, callus formation, and edema.
ANATOMY
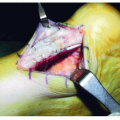
Resembles laceration, puncture, or blister with round or oblong shape.
May be necrotic, pink, or pale with well-defined smooth edges.
Periwound often presents with callus.
PATHOGENESIS
Origin and development have several components.
Thirty-two unique casual pathways for developing foot ulcers.2
Peripheral neuropathy, structural foot problems, and minor trauma are present in the majority (63%).
Other less prevalent causes include edema, callus, and peripheral ischemia.
Major common pathways involve pressure/trauma, ischemia/hypoxia, infection, cellular failure, and chronic inflammation.
PATIENT HISTORY AND PHYSICAL FINDINGS
Basic history, including state of health, record of diabetic complications, shoe problems, pain in extremity, medications, glycated hemoglobin level.
Risk factor assessment involving absence of protective sensation due to peripheral neuropathy, vascular insufficiency, structural deformities/callus formation, autonomic neuropathy, limited joint mobility, long duration of diabetes, long history of smoking, poor glucose control, obesity, impaired vision, past history, increased age, male gender, poor footwear.
The Wagner scale for foot wound classification based on depth and presence of osteomyelitis and gangrene is the most widely accepted classification scheme4 (FIG 1) but does not address the critically important parameters of ischemia and infection.
Grade 0: intact skin
Grade 1: superficial without penetration of deep layers
Grade 2: deeper reaching tendon, bone, or joint capsule
Grade 3: deeper with abscess, osteomyelitis, or tendonitis extending to those structures
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree