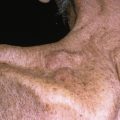
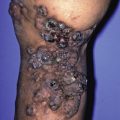
Epidermal Nevus Syndrome
Nevus unius lateralis
Systemized epidermal nevus
Linear and serpiginous presentations of skin disease represent distinctive patterns that are so unique that a diagnosis can often be made without a biopsy or any further testing. In this short chapter, not all linear diseases may be discussed because many rare congenital disorders may present with linear configurations but would be beyond the scope of this practical discourse. It is also important to note that linear and serpiginous patterns should not be confused with sporotrichoid patterns of infection, which appear linear due to lymphatic spread. The sporotrichoid pattern is covered in Chapter 18 .
Important History Questions
Were the lesions present at birth or shortly after birth?
This is an important question because many linear conditions are congenital in nature and were present in the neonatal period (e.g., linear epidermal nevus, incontinentia pigmenti).
Is there a family history of a similar lesion?
In the appropriate clinical circumstances, an affirmative answer would support the diagnosis of incontinentia pigmenti, an X-linked dominant genetic disorder. However, it is important to note that a negative response does not exclude incontinentia pigmenti because spontaneous mutations are common.
How long have the lesions been present?
Some lesions persist for life (e.g., linear epidermal nevus), whereas others have a finite duration (e.g., lichen striatus).
What medications do you take?
This is an important question in patients for whom linear bleomycin-induced erythema or hyperpigmentation is suspected.
Is there a history of recent travel?
This question is designed to include or exclude cutaneous larva migrans. This condition is especially prevalent in the southeast United States and in other subtropical or tropical climates.
Important Physical Findings
What is the distribution of the lesions?
A distribution that follows the lines of Blaschko supports assessment of a linear epidermal nevus or other epithelial hamartoma, whereas cutaneous larva migrans is more common on acral skin.
What color are the lesions?
Linear epidermal nevi are often yellow-brown or brown, flagellate erythema due to bleomycin or cutaneous larva migrans is erythematous, and linear morphea may be white or yellow-white.
Do any lesions demonstrate vesicles or blisters?
Vesiculobullous lesions may be seen in incontinentia pigmenti or cutaneous larva migrans. Although not discussed in this chapter, allergic contact dermatitis may also demonstrate linear vesiculobullous lesions.
Does the lesion demonstrate induration on palpation?
Linear morphea is characterized by marked induration due to thickening of the collagen.
Lichen Striatus
ICD10 code L44.2
INTERNAL DISORDER
There is no easy answer because the lines of Blaschko do not conform to any known anatomic features. Instead, the lines of Blaschko are somewhat circularly defined as lines that congenital linear abnormalities follow. It has been suggested that the lines are due to cutaneous mosaicism of different clones of cells.
Pathogenesis
Lichen striatus is an uncommon, self-limited dermatosis, of unknown cause; it affects mostly children. Some studies have suggested a more frequent personal or familial atopic diathesis in affected patients.
Clinical Features
- •
Some studies have reported a slight female preponderance, whereas others studies have reported that both genders are equally affected.
- •
Most cases occur in preschool children, with a mean age of 3 years, but the condition can also occur in adolescents and young adults as well.
- •
A unilateral (and rarely bilateral) eruption affects the lower limbs (one-third of cases), followed by the upper limbs, trunk and, rarely, the face (~10%).
- •
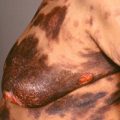
The eruption begins as discrete skin-colored, pink, or red papules ( Fig. 17.1 ), with variable overlying scale. In darker skin types, the condition may appear hyperpigmented ( Fig. 17.2 ) or hypopigmented.
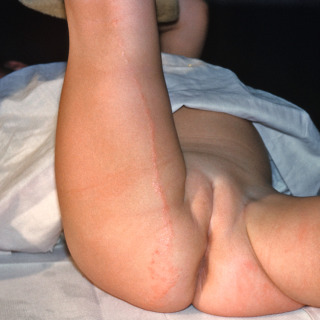
Fig. 17.1
Patient with early lesions of lichen striatus composed of red linear papules.
(From the William Weston Collection, Aurora, CO.)
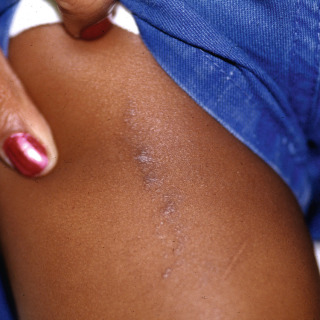
Fig. 17.2
Patient with linear lesions of lichen striatus on the upper thigh demonstrating subtle hyperpigmentation.
- •
Less often, the condition may resemble lichen planus or psoriasis.
- •
Lesion are grouped as continuous or discontinuous lines that generally follow the lines of Blaschko (see box), with some cases manifesting more than one parallel line of involvement ( Fig. 17.3 ).
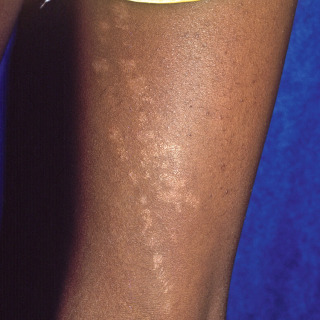
Fig. 17.3
Patient with hypopigmented lichen striatus with two parallel linear lesions following the lines of Blaschko.
- •
Typically, the condition is asymptomatic, but it may be pruritic in about 10% of cases.
- •
Rare patients may demonstrate extension to a contiguous fingernail or toenail, with onychodystrophy manifesting as thinning, splitting, longitudinal ridging, or onycholysis ( Fig. 17.4 ).
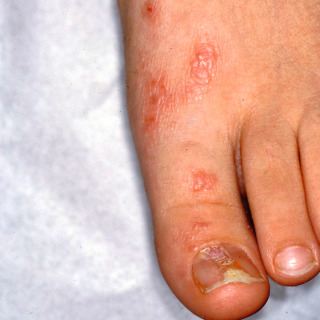
Fig. 17.4
Patient with unusually indurated red linear papules, with associated nail dystrophy.
(From the William Weston Collection, Aurora, CO.)
Diagnosis
- •
The history and clinical appearance are usually diagnostic.
- •
A skin biopsy is not usually required, but, if the presentation is atypical, a biopsy may be performed. The histologic findings will support the diagnosis, but exclusive pathognomonic findings do not exist.
Treatment
- •
Reassurance is usually all that is necessary because the condition is self-limited and typically disappears in weeks or months (rarely years), without permanent sequelae.
- •
Weak to midstrength topical steroids may be used for pruritus.
Clinical Course
The mean duration of disease is 6 to 9 months; however, rare patients may have lesions for up to 3 years. Hypopigmentation may persist for months, even after the lesion resolves. Rare patients may suffer a relapse or even multiple relapses.
Bleomycin-Induced Flagellate Erythema and Hyperpigmentation
ICD10 code Y43.1
DRUG-INDUCED
Pathogenesis
Bleomycin is a chemotherapeutic agent that produces a distinct skin eruption with linear erythema that transitions into linear hyperpigmentation. It is most commonly seen at higher cumulative doses, usually in the range of 90 to 285 mg; however, some patients may develop this reaction with the first dose. There is no clear consensus as to how often this adverse reaction transpires, with a reported range in the literature of 6% to 66% of patients who have received the drug. The mechanism whereby the linear lesions are produced is uncertain, but it has been postulated that it is related to scratching because affected patients report pruritus. Attempts to induce lesions with superficial trauma have not always been successful.
Clinical Features
- •
Lesions usually develop within hours to weeks after taking bleomycin.
- •
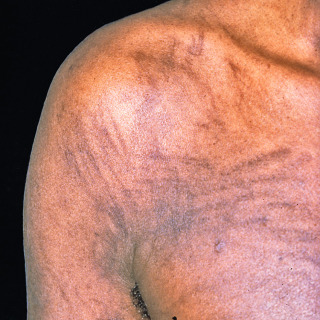
Primary lesions present as linear erythema, with pruritus ( Fig. 17.5 ).
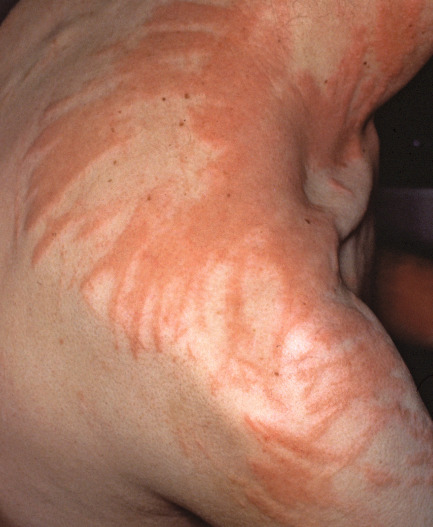
Fig. 17.5
Patient with characteristic flagellate areas of a pruritic erythema produced by bleomycin.
- •
The lesions transition, usually over days or weeks, into linear hyperpigmented lesions, with some patients having transitional lesions that may appear violaceous ( Figs. 17.6 and 17.7 ).