Key Words
burn contracture release, lower extremity, local tissue rearrangement, skin graft, burn reconstruction
Synopsis
Over 200,000 patients are treated yearly in the United States for burns, and yearly millions suffer from burns overseas. Due to the large surface area and dependent position of the lower extremities, burns are very common and can range from small, superficial burns to extensive, deep burns resulting in amputation. Burn scar contracture release is the most commonly performed lower-extremity burn reconstructive procedure in our practice. The key to successful lower-extremity burn contracture release is an understanding of the advantages and limitations of the available techniques for contracture release. This chapter is divided into pre-operative management of the burned and contracted lower extremity, surgical techniques, post-operative care, and management of the complications. The purpose of this review is to display the treatment strategies in leg burn reconstruction in the global surgery setting.
Clinical Problem
Leg burn reconstruction encompasses a wide range of clinical problems and solutions. These include everything from debriding a small burn to managing a catastrophic injury resulting in amputation. Of all the lower-extremity problems we see in our burn surgery practice, burn scar contractures are by far the most common.
Burn scar contractures can present anywhere from the groin to the toes. Their severity varies from mild discomfort due to loss of elasticity in the scarred area to severe deformity, loss of function, pain, and disability. The flexor surfaces are more commonly affected, because the flexion creases under the joints tend to have thinner skin than the extensor counterparts, so burns tend to result in deeper injuries and more scars. The strong muscle mass of the lower extremities can sometimes overwhelm the strength of the scar bands, resulting in auto-releases leading to recurrent areas of ulceration in the scar.
Burn contractures can present in patients of any age, but recurrences are more common in children, because they are still growing and often outpace the growth of their scars. Intervention of burn contractures in a timely fashion can prevent joint stiffness and potentially irreversible functional deficits. Regular follow-up for patients who have undergone lower-extremity contracture releases can help detect recurrences early, especially in children.
Pre-Operative Management
To establish the most appropriate management plan, one has to individualize the care for each patient and start by deciding the best timing for surgery.
In the first year or two after the injury, burn scars continue to mature and remodel. Immature scars are often thick, dark, and hyperemic and can cause severe pruritus. At this stage, contracture releases often result in prompt recurrence of the contracture. Immature scars causing minimal symptoms can therefore be managed by trying one or more of the nonoperative therapy options: compression garments, silicone sheets, scar massage, or possibly even consideration of steroid injections or laser therapy for scar management. Once scar maturation has occurred, surgical intervention tends to result in better outcomes. Not every scar contracture requires immediate surgery. In children who are still growing, we sometimes delay surgery if a contracture is mild and wait until it becomes more symptomatic to minimize the total number of interventions. This has to be done with caution, though, because unnecessary delay of contractures can result in additional problems. These can include joint damage and shortening of tendons and neurovascular bundles, which may prevent a complete release and ultimately may lead to worse outcomes.
Lower-extremity burn scar contractures can affect all joints from the hip/groin area to the distal joints in the toes. Some areas have thin skin: the popliteal fossa at the level of the knee, the dorsum of the ankle, and the dorsum of the toes. As a result, deep burns and burn contractures often occur in these areas, causing flexion of the knee or hyperextension of the ankle and toes.
Release of contractures by dividing the scars, followed by skin grafting, remains the primary means of burned lower-extremity contracture release. When evaluating an area with contracture for potential release, it is imperative to perform a complete examination including assessment of joint mobility, strength, sensation, and perfusion. Tendons and other vital structures that may be exposed and difficult to cover with skin grafts should be identified. The blood supply and nerve branches of a contracted limb could be abnormal, especially in long-term or recurrent contractures. A pre-operative neurovascular examination can help establish any preexisting injuries and can help with discussion of the risks associated with surgery. As the joint contracts, the respective neurovascular bundles shorten, and upon release, tension on the bundle can stretch and even tear blood vessels or nerves. Intraoperative examination of the neurovascular structures allows the surgeon to determine the extent of release that is safe to perform. It is sometimes necessary to stage a contracture release and perform only a partial release at each step.
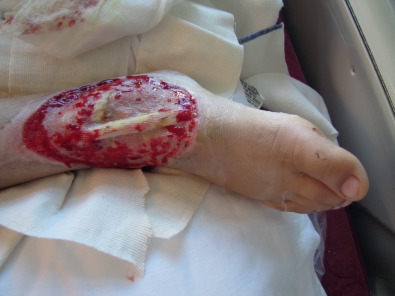
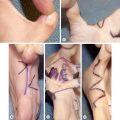
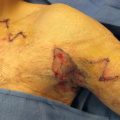
Defects in the burned lower extremity are seen in the acute setting and after contracture releases. They can be reconstructed using skin grafts or flaps. Small defects can be easily covered with a full-thickness skin graft harvested from the groin or lower abdomen. Large defects almost always require a split-thickness skin graft; the resulting donor site can be painful and may require wound care for a week or two. We therefore try, whenever possible, to reconstruct leg burn defects with either full-thickness grafts or local flaps to minimize morbidity. Z-plasties are simple flaps that can add length to an area of tight scar. They can be used only if the surrounding areas are not tight. Many times, unfortunately, the areas surrounding the scar band are also badly scarred. Larger flaps, including pedicled fasciocutaneous and muscle flaps as well as free flaps, are sometimes used to cover defects that cannot be grafted. In our experience, these are needed only rarely in the global surgery setting. Two examples of flaps used with ease in global settings are presented in the figures: A patient with an exposed tendon ( Fig. 4.9.1 ) is treated with simple local rotation flaps ( Fig. 4.9.2 ) and skin grafts. By combining small flaps with grafts, the defect is completely covered ( Fig. 4.9.3 ). Another patient, a 3-year-old with deep burns leading to exposed bone, was successfully treated with a cross-leg flap ( Fig. 4.9.4 ).