Lateral Orbitotomy
The surgical procedure utilized for the excision of an orbital lesion will depend on the lesion’s location, size, and suspected pathology. In addition, the biological behavior of the suspected lesion may influence the approach. Thus, a lacrimal gland lesion may be approached through a transseptal anterior orbitotomy if biopsy of a suspected inflammatory or malignant process is anticipated. However, if a benign mixed tumor of the lacrimal gland is the working diagnosis, a lateral orbitotomy is necessary for total removal. Some disease processes that involve only the subperiosteal space, such as subperiosteal hematoma or abscess, floor fracture, and mucocele, are best approached through a transperiosteal route that does not violate the periorbita. The lateral approach provides the best access to the retrobulbar compartments inside and outside the muscle cone. It is especially useful for lesions in the lacrimal gland fossa, but may be inadequate for some lesions at the orbital apex. The key for any successful and atraumatic surgical exploration is adequate exposure. This is especially true in the orbit because of the many important structures confined within this tight space. To minimize operative morbidity, the surgeon must have a thorough understanding of the orbital anatomy as well as a complete familiarity with the chosen surgical technique.
PREOPERATIVE MANAGEMENT
It is usually unnecessary to type and crossmatch blood in preparation for orbital surgery. However, it should be considered in patients with low hemoglobin or hematocrit values, or in whom significant intraoperative bleeding is anticipated, such as in resecting an arteriovenous malformation. Patients taking anticoagulants, such as warfarin sodium (Coumadin), or inhibitors of platelet aggregation, such as aspirin, should have these drugs discontinued at least 2 weeks before surgery, if possible. The surgeon should also inquire about the intake of any over-the-counter drugs containing aspirin, such as Alka-Seltzer, Sine-Off, and Midol. Fish oil, a product sold for prevention of heart disease, is frequently not regarded as medication by patients; hence, their use is often not disclosed to the surgeon. Fish oil, when taken in large quantity, can interfere with platelet function and prolong bleeding time.
General endotracheal anesthesia is preferred when the retrobulbar area is explored. Induced intraoperative hypotensive anesthesia, although usually not required, may be considered, to improve hemostasis and to facilitate tissue dissection in some cases. This technique should be employed only in patients in good physical health and in conjunction with an anesthesiologist who is acquainted with its application.
MAGNIFICATION AND ILLUMINATION
A fiberoptic headlight and magnifying loupes are essential to provide illumination and magnification of fine orbital structures during lateral orbitotomy. A binocular operating microscope with coaxial illumination is particularly useful when surgery, such as sheath fenestration, is performed on the optic nerve. By choosing an objective lens between 200 and 250 mm, adequate room can be obtained between the surgical field and the microscope for instrument manipulation. An improvement in visualization, combined with proper microsurgical techniques and working knowledge of the deep orbital anatomy, adds a new dimension to the safety of orbital surgery.
OPERATIVE PROCEDURE
The patient is placed in a slight reverse Trendelenburg’s position to reduce orbital venous pressure. The face is turned slightly away from the operative site. The primary surgeon is seated on the side of the orbit on which surgery is to be performed, and the assistant is seated at the head of the table. The cornea may be protected by a small piece of moistened Gelfoam during surgery, particularly for eyes that are proptotic. One should refrain from placing a suture tarsorrhaphy on the lids, as it will prevent forward displacement of the globe and preclude monitoring pupillary reactions during orbital manipulation.
An S-shaped Stallard skin incision is preferred because it gives excellent exposure and eliminates the necessity to reconstruct the lateral canthal angle at the end of the procedure.
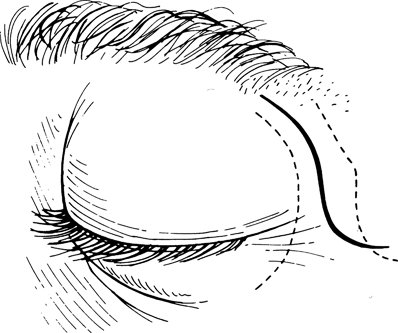
Figure 32-1. After the surgical site has been prepared, the S-shaped skin outline is marked with a marking pen. The marking begins beneath the inferior cilia of the lateral one third of the eyebrow, extending inferolaterally along the superior and lateral bony orbital rim, past the level of the lateral commissure to terminate over the zygomatic arch. The tail end of the marking may be camouflaged within a laugh line. The lateral canthal region and the temporalis muscle are infiltrated with lidocaine 2% with 1:100,000 dilution of epinephrine before draping and scrubbing of hands. This allows the vasoconstrictive effect of epinephrine to work before an incision is made.The initial incision is carried down to, but not through the periosteum.
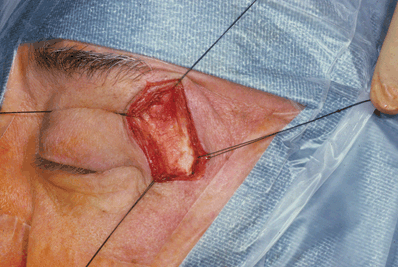
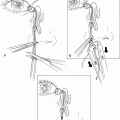
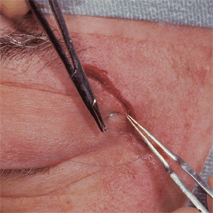
Figure 32-2. Subcutaneous tissues and orbicularis oculi muscle are bluntly dissected away with a Freer periosteal elevator to expose the periosteum and fascia of the temporalis muscle. Bleeding from orbicularis muscle is controlled by bipolar cautery. Traction sutures of 4–0 black silk are positioned in both sides of the skin-muscle flaps and secured to the surgical drapes with hemostats.
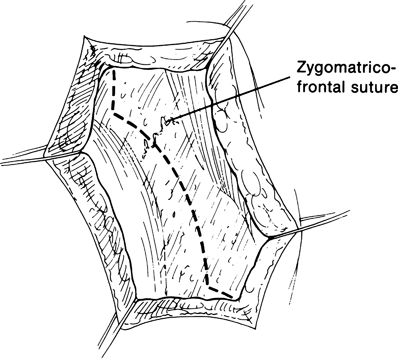
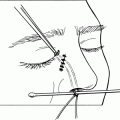
Figure 32-3.The periosteum is then incised with a size 15 Bard-Parker blade parallel to and approximately 2 mm lateral to the orbital rim. The periosteal incision is carried superiorly above the zygomaticofrontal suture line and inferiorly past the superior aspect of the zygomatic arch. Periosteal relaxing incisions are made at the superior and inferior ends of the incision.
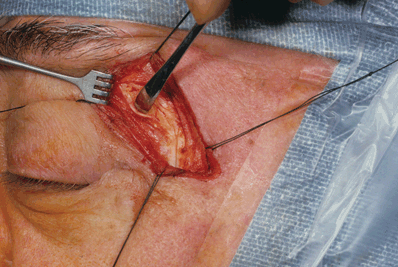
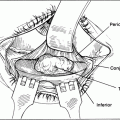
Figure 32-4. The periosteum and temporalis muscle are reflected from the zygomatic process of the frontal bone and the frontal processes of the zygomatic bone. This maneuver is accomplished by using either a Woodson or Freer periosteal elevator.
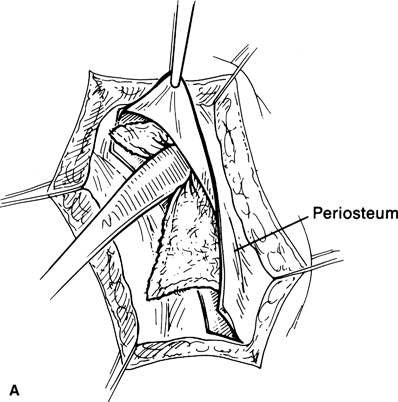
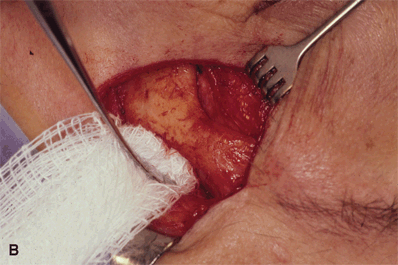
Figure 32-5A and B. Once the dissection is carried into the temporalis fossa, the separation of the periosteum and temporalis muscle is facilitated by forcing an opened 4 × 4 gauze into the dissection plane, with a Freer elevator, to just behind the sphenozygomatic suture line. By bluntly dissecting the temporalis muscle off its bony attachment with a gauze, shredding of the muscle by the sharp tip of the periosteal elevator can be avoided. Brisk bleeding may be encountered in the bed of the temporalis muscle or from avulsion of the zygomaticotemporal artery. This can be controlled either by pressure or with bipolar cautery. Oozing from the bony surface can be stopped with bone wax.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree