Key Words
mandible fracture, mandibular distraction, jaw tumors, retrognathia, odontogenic tumors
Synopsis
Jaw surgery is a broad topic that encompasses a wide array of pathologies of the maxillofacial skeleton. With regard to global reconstructive surgery and the issues seen most commonly in developing nations, this chapter has been organized into the following three sections:
- 1.
Lower facial fractures
- 2.
Mandibular distraction for severe retrognathia
- 3.
Jaw tumors
Methods of treatment for these three problems vary in both the developed and developing world, and techniques to address these issues that can be applied using basic surgical techniques will be presented.
Lower Facial Fractures
Clinical Problem
Mandible fractures are among the most common fractures of the maxillofacial skeleton, exceeded only by nasal fractures in frequency. In the United States, assault accounts for the highest incidence of mandible trauma for male patients, with motor vehicle trauma accounting for the greatest incidence in the developing world. Individuals with mandible fractures can present with tenderness to palpation of the mandible and mobility of the fracture segments. Malocclusion, trismus, and pain are frequently seen, and can be accompanied by ecchymosis, hematoma, swelling, and paresthesias or frank anesthesia. Associated injuries from trauma are seen in over 40% of patients and must be assessed; cervical spine injuries are seen in 11% of patients and must be ruled out before the initiation of any treatment.
Pre-Operative Management
Physical Examination
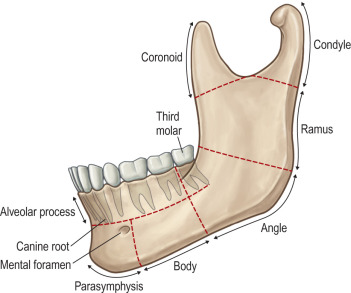
A systematic physical examination is vital in the diagnosis and treatment of mandible fractures. The patient should be asked to point out any areas of pain or tenderness and to run his or her tongue along the teeth to note any dental irregularities, chipped teeth, or crown loss. Patients should be asked to point out any areas of numbness or diminished sensation. Any bruising or swelling should be noted, and any external lacerations should be evaluated; chin lacerations should increase the level of suspicion for a condylar fracture. Intraoral inspection should be performed next, noting any dental irregularities, step-offs in the dental arch, gingival and mucosal lacerations, and any segment instability or mobility. Dentoalveolar injuries should be noted and documented. The patient should be asked to bite his teeth together and asked whether the occlusion feels normal; soft tissue edema can contribute to the sensation of malocclusion, which may not necessarily indicate the presence of a fracture. Lastly, the mandible is palpated externally with the mouth slightly open, assessing the posterior rami, angles, lower border and body, and symphyseal regions; areas of tenderness or pain should be noted. Condylar movements should be assessed by opening and closing the jaw while palpating just anterior to the ear canal ( Fig. 3.10.1 ).
Pre-Operative Testing
Should physical examination suggest a mandible fracture might be present, the radiological examinations of choice are an orthopantomogram (Panorex) and anteroposterior skull view, or a CT examination. The Panorex allows for complete visualization of the maxillary and mandibular dentition, and can be used to evaluate fracture sites. The anteroposterior (AP) skull radiograph allows for better visualization of the symphysis, which can be blurred in a Panorex and is better for evaluating lateral displacement of angle fractures. An axial CT scan with coronal, sagittal, and 3D reconstructions has replaced use of the Panorex and skull films at many institutions. If neither CT scan nor Panorex is available, AP, lateral, and right and left oblique plain film x-rays should be obtained.
Optimal Timing of Surgery
Surgery to repair fractures of the mandible can be performed after establishment of the clinical priorities of other injuries present. Studies have not shown an increased rate of infection, malunion, or nonunion in fractures treated up to 2 weeks post-injury. However, to allow for commencement of healing, surgery should be planned within the first week post-injury if possible, after having addressed any more serious concomitant injuries.
Supplies Needed
Miniplate osteosynthesis and intermaxillary fixation (IMF) have become the mainstays of treatment for mandible fractures. Relatively inexpensive plating systems have been developed locally worldwide, as have arch bar materials and the wires needed to attach them to the teeth and to wire the patient into IMF. In the absence of a plating system, interosseous wiring and IMF can be contemplated, albeit with the possibility of decreased stability across the fracture line.
Recommended supplies include:
Arch bar material
Stainless steel wires (24- or 26-gauge)
Wire cutters
Needle driver
Minnesota retractor
Langenbeck retractor
Sweetheart (Weider) tongue retractor
Wire bending pusher
Electrocautery unit
Electric- or gas-powered drill system
Mandibular plating system with 2.0- and 2.4-mm plates and screws
Plate benders
Gerald forceps with teeth
Suction catheter and tip
Antibiotic irrigation
Anesthesia Concerns
Nasotracheal intubation is required to establish dental occlusion and IMF. If this is not possible due to the presence of concomitant midfacial trauma, either tracheostomy or submento-tracheal intubation will need to be performed.
Surgery
Most fractures can be addressed via an intraoral incision in the gingivobuccal sulcus. Complex fractures and those with overlying soft tissue lacerations can be approached via an external submental or submandibular Risdon incision made along the inferior border of the mandible from the angle forward, taking care to make the incision 1 to 2 cm below the mandibular border to avoid injury to the marginal mandibular nerve and to decrease scar visibility.
Arch bars should be placed first, starting with the maxilla and then the mandible, using 26-gauge wires from the bicuspids through the molars. The arch bar material is bent to follow the contour of the dental arch, one each for the maxilla and mandible, and trimmed to allow for ligation to as many teeth as possible. The lugs of the arch bars should be pointing upward on the maxilla and downward on the mandible. A 26-gauge wire is passed around the premolars on either side of the maxilla or mandible, and the arch bar material is positioned with one end of the wire below the arch bar and the other above. The wire is twisted with a wire twister in a clockwise direction, applying gentle traction to the wire while tightening and taking care not to over twist the wire, which will cause it to break. The twisted end is cut, leaving an approximately 10-mm tail, which is curled in a clockwise direction into a rosette and flattened against the arch bar material, to avoid irritation to the gingiva and to leave the arch bar lugs free of obstruction.
Dental occlusion is next established to apparent pre-injury status, along with gross reduction of the fractures and application of IMF wires. The vestibular or extraoral incision should then be made and the fractures exposed, taking care to avoid injury to the mental nerve (and marginal mandibular nerve should an extraoral approach be used). A cuff of mucosa should be maintained when using the vestibular approach to allow for incision closure.
Anatomical reduction of symphyseal, parasymphyseal, and body fractures is next performed. This can be facilitated with a bone reduction clamp placed perpendicularly into drill holes on either side of the fracture along the inferior border of the mandible. Next, a 2.0-mm miniplate with monocortical screws (5–6 mm) should be placed, spanning the fracture line at the inferior margin of the tooth roots. The bone reduction clamp is then removed, and a 2.0- or 2.4-mm plate placed along the inferior border of the mandible using bicortical screws, measured with a depth gauge. IMF is then removed and the occlusion checked to make certain that the patient opens and closes into his pre-trauma occlusion.
Angle fractures can be addressed with an external oblique ridge (Champy) plate if simple and minimally displaced, or via a vestibular approach with trocar or external approach if complex or widely displaced. Damaged third molars or those interfering with reduction should be removed to allow for reduction and fixation of the fracture. For the intraoral (Champy) approach, after exposure and reduction of the fracture, a 2.0-mm miniplate is bent to follow the contour of the external oblique ridge and is fixated with 6- to 8-mm screws. For the trocar + vestibular incision or external (Risdon) approach, after exposure and reduction of the fracture, a curved 2.4-mm plate is bent to follow the contour of the inferior border of the angle of the mandible, and is fixated using bicortical screws measured with a depth gauge, placed via the trocar or directly using the Risdon approach. As with the symphyseal, parasymphyseal, and body fractures, IMF is removed and pre-trauma occlusion ascertained ( Fig. 3.10.2 ).
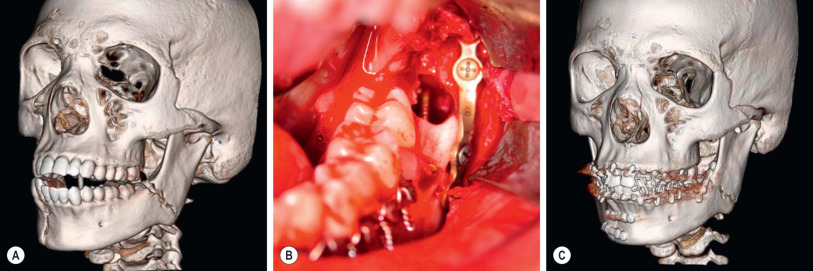
Condylar and subcondylar fractures have seen a recent evolution in their treatment. Condylar head and intracapsular fractures are generally treated with a course of IMF (2 weeks) followed by guiding elastics (2–4 weeks) until resting occlusion is obtained. Neck and low subcondylar fractures with malocclusion, significant displacement (greater than 30 degrees), temporomandibular joint dislocation, and fracture gaps in excess of 5 mm are now seen as best treated with open reduction and internal fixation. A preauricular approach (above the facial nerve), submandibular approach (below the facial nerve), or retromandibular approach (between the buccal and mandibular branches of the facial nerve) can be utilized.
Incisions are closed using either 4-0 polyglactin (Vicryl, Polysorb) or 4-0 chromic sutures, and the patient is placed into IMF with 26-gauge wires ( Fig. 3.10.3 ).
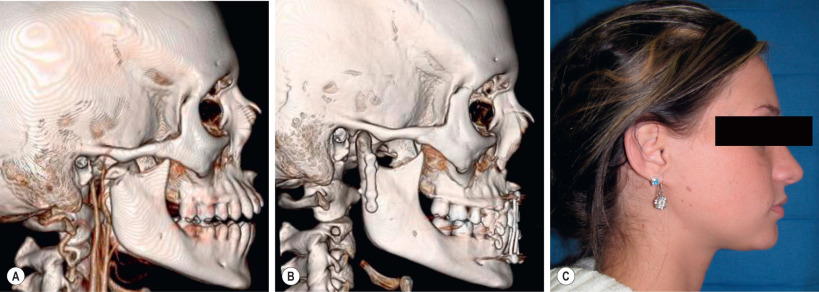
Post-Operative Care
The patient should remain on antibiotics for 5 to 7 days post-operatively, either intravenous or oral liquid routes. Oral rinses with Peridex (chlorhexidine gluconate 0.12%) should be performed three times daily. Post-operative radiography should be obtained to assess reduction and placement of fixation. A liquid (no chewing) diet should be followed for 4 to 6 weeks post-operatively, and arch bars removed after 4 to 6 weeks.
Management of Complications
Malocclusion and Malunion
Abnormalities in occlusion can occur from inadequate or improper reduction, poorly contoured fixation plates that bend the mandible out of reduction, loose plates or IMF, or in multiply comminuted fractures with instability of reduction. Minor bite abnormalities can be addressed with occlusal facet adjustments of the teeth or orthodontics, whereas major abnormalities likely require orthognathic procedures.
Infection and Nonunion
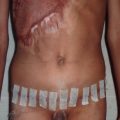
Infection can occur as a result of poor soft tissue coverage, loose hardware, and devitalized bone. Treatment requires removal of hardware, debridement on nonviable tissue, revision of fixation with a larger reconstruction plate, and bone grafting of any fracture gaps. Persistent infection may require the use of external fixation with pins to allow for resolution of infection.
Hardware Failure
Failure can occur by screw loosening and by frank hardware breakage. In both instances it is remedied with removal of the plate and screws, revision of reduction, and refixation with a properly contoured, larger plate with newly drilled screw holes.
- •
There is strong clinical evidence supporting the use of pre-operative antibiotics in mandibular fractures (excluding isolated condylar fractures).
- •
After nasal fractures, mandible fractures are the most common fracture of the maxillofacial skeleton, accounting for 36% to 70% of all facial fractures.
- •
There is clinical evidence demonstrating improved patient outcomes with open reduction for displaced fractures of the mandible condyle as well as for mandibular angle fractures.
- •
Upward of 40% of all mandible fractures have associated injuries elsewhere, with 11% of these patients having an associated cervical spine fracture.
- •
More than 50% of mandible fractures occur in multiple locations on the mandible.
Mandibular Distraction for Severe Retrognathia
Clinical Problem
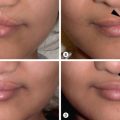
Tongue-based airway obstruction (TBAO) in neonates is a clinical problem that has undergone an evolution over the past 20 years with the advent of mandibular distraction osteogenesis (MDO). Conditions associated with TBAO include Pierre Robin sequence (PRS), Goldenhar, Treacher Collins, and Sticklers, along with rarer or as-yet-unidentified syndromes. Past treatment for micrognathia and TBAO have included tongue-lip adhesion surgery, nasopharyngeal airways, prone positioning, and tracheostomy. None of these treatments, however, addressed the underlying micrognathia responsible for the airway obstruction, and MDO has been demonstrated to be a safe and effective treatment in multiple studies when properly performed ( Fig. 3.10.4 ).
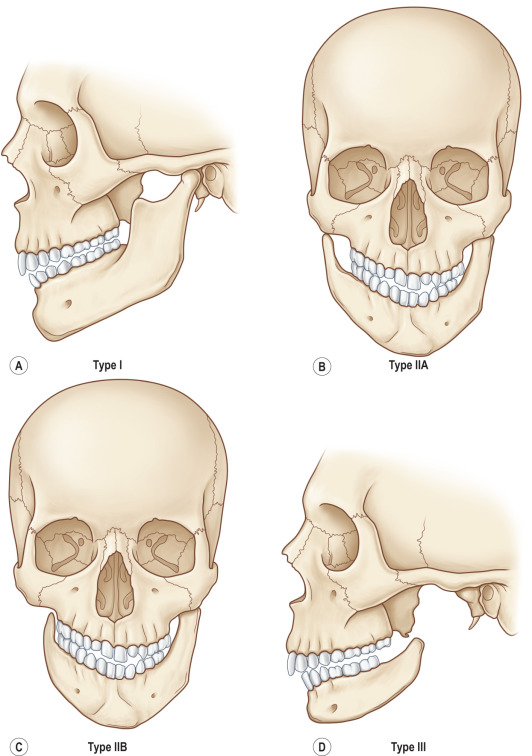
Pre-Operative Management
Physical Examination
Examination of the infant with micrognathia and suspected TBAO should at a minimum include flexible fiber-optic laryngoscopy to ascertain the level of airway obstruction (lengthening of the mandible would not be expected to have any appreciable effect on laryngomalacia alone). Other modalities useful in assessing the severity of TBAO include continuous pulse oximetry with or without jaw thrust and, ideally, inpatient polysomnography to assess the Apnea-Hypopnea Index (AHI). An AHI of 5 or greater requires intervention, and MDO has been advanced as a front-line treatment for TBAO.
Pre-Operative Testing
The most common pre-operative imaging modalities are plain film radiographs and CT scans, with 3D reformatted images having become available with most modern scanners. These 3D images allow for a more accurate assessment of the height and length of the mandible, and are useful in osteotomy planning and distractor placement.
Optimal Timing of Surgery
For those infants intubated immediately after birth with failed attempts at extubation and TBAO as evidenced on nasoendoscopy, distraction can be performed as early as 1 week of age, with the infant remaining intubated until the level of distraction is great enough to overcome the TBAO. For older infants with evidence of recurrent desaturations and TBAO, the surgery can be planned should positioning and nasopharyngeal airways be insufficient to overcome the desaturations.
Supplies Needed
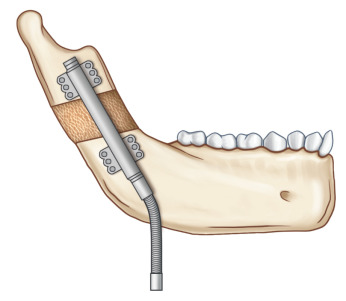
Both internal and external distraction systems have been developed over the years, with internal devices preferred secondary to decreased scarring, more predictable lengthening and vector of distraction, decreased risk of dislodgement, and increased patient comfort. Recommended supplies include:
Distraction system with distractors, screws, screwdrivers, and activation arms ( Fig. 3.10.5 )