Thalidomide is approved for treating erythema nodosum leprosum and multiple myeloma, but it has also emerged as a useful treatment option for many refractory dermatologic disorders. Some of the innovative but off-label uses of thalidomide include aphthous stomatitis, Behçet’s disease, lupus erythematosus, prurigo nodularis, sarcoidosis, actinic prurigo, graft-versus-host disease, Langerhans cell histiocytosis, erythema multiforme, lichen planus, Kaposi sarcoma, Jessner lymphocytic infiltrate, uremic pruritus, pyoderma gangrenosum, scleroderma, scleromyxedema, and necrobiosis lipoidica. This article reviews the background, pharmacology, and innovative uses of thalidomide in dermatology.
Thalidomide is a synthetic glutamic acid derivative first introduced in 1956 in Germany as an over-the-counter sedative marketed as Countergan. Initially thought a safe medication, thalidomide was marketed to other industrialized nations by 1958 and was also widely used as an antiemetic by pregnant women. Thalidomide was withdrawn from the world market in 1961 due to occurrences of rare congenital abnormalities, such as phocomelia, in infants born to women who ingested thalidomide during pregnancy. It had not been approved in the United States at that time due to concerns of a potential link between thalidomide and peripheral neuropathy. In 1965, Dr Jacob Sheskin, an Isreali dermatologist, made a fortuitous discovery when giving thalidomide to his leprosy patients for its sedative properties. Patients with erythema nodosum leprosum (ENL) had unexpected improvement of skin lesions soon after initiating therapy. This discovery triggered a renewal of interest and research into thalidomide. In 1998, the drug was approved by the Food and Drug Administration for ENL and, in May 2006, it was approved for treating multiple myeloma. Thalidomide’s status as an orphan drug has led to its off-label and innovative use in several dermatologic disorders unresponsive to traditional treatments.
Pharmacology
Thalidomide’s structure has a left-sided pthalimide ring and a right-sided glutarimide ring. Thalidomide is given orally, with peak plasma concentrations occurring approximately 2.9 to 5.7 hours after ingestion. The drug is metabolized mainly through spontaneous, nonenzymatic hydrolysis in blood and tissue, although a minute amount is metabolized via the hepatic cytochrome P450 system. Thalidomide distributes extensively in the body and has been found in semen, making it necessary for male patients taking the medication to wear condoms even if they have had a vasectomy; their female partners are also advised to use an additional form of birth control. Mean elimination time is 5 to 7 hours, and less than 1% of the medication is excreted unchanged in urine. Most dosages of thalidomide used in dermatology have been low (range of 25 to 400 mg daily), although higher doses have been administered in select situations. The mechanism of action for thalidomide is still not completely understood, although it has been shown to have sedative, anti-inflammatory, immunomodulatory, and antiangiogenic activity.
Off-label dermatologic uses
Aphthous Stomatitis
Several studies have shown thalidomide to be effective for recurrent aphthous stomatitis. Mascaro and colleagues reported 6 cases of aphthous stomatitis that completely resolved after 7 to 10 days of therapy with thalidomide (100 mg daily). Jenkins and colleagues reported similar results: 15 patients with aphthous stomatitis were treated with thalidomide (400 mg daily tapered to 200 mg daily). Fourteen of the patients had complete resolution of lesions within 5 to 21 days, and the remaining patient had significant improvement. Unfortunately, most of the treated patients relapsed after therapy was discontinued.
Larger, open-label, noncontrolled studies have also reported successful treatment of severe aphthosis with thalidomide. In a 40-patient trial, severe oral aphthosis was treated with thalidomide at initial dosages of 300 mg daily; mild cases were started on 100 mg daily. In both groups, 75% of patients responded well to therapy. For patients who relapsed after discontinuing therapy, the investigators recommended a dosage of 100 mg daily for 12 days. A controlled, crossover, randomized trial of 73 patients with severe aphthous stomatitis reported 32 patients (44%) with complete remission while on thalidomide (100 mg daily); most other patients in the study experienced dramatic improvement.
A recent open trial of 21 patients compared the efficacy of thalidomide, dapsone, colchicine, and pentoxifylline in treating severe recurrent aphthous stomatitis. Each patient was given 1 of the 4 test drugs for 6 months and switched drugs if toxicity or lack of efficacy occurred. Of the 4 drugs, thalidomide (100 mg daily) was the most effective and well tolerated, resulting in complete remission for 7 of 8 patients. Other studies have shown that thalidomide therapy is also an effective option for recurrent aphthous ulcers in patients with HIV. Aphthous ulcers have a variable natural course and many cases resolve spontaneously, making the interpretation of any therapeutic study somewhat difficult. Thalidomide therapy should be considered only for severe, recurrent, and seemingly recalcitrant cases.
Behçet Disease
Behçet disease (BD) is a systemic disorder with various skin lesions, ocular disease (panuveitis), arthritis, intestinal bleeding, and recurrent aphthous orogenital ulcers. After reports of thalidomide’s efficacy for aphthous stomatitis, a 1982 open trial treated 22 BD patients with thalidomide (400 mg daily for 5 days and 200 mg daily for the next 15–60 days). Although ocular and arthritic symptoms did not improve, orogenital ulcerations healed quickly. Ulcers recurred after withdrawal of thalidomide, but they were milder and less frequent than before treatment. Other studies have shown similar beneficial effects but have also noted recurrence of disease after treatment ended.
A randomized, double-blind trial compared thalidomide dosages (100 mg daily and 300 mg daily) to placebo. The results showed thalidomide dosages of 100 mg daily to be similar in efficacy to 300 mg daily, with both dosages demonstrating better efficacy compared with the placebo control. Withdrawal of either treatment dosage led to prompt recurrence. In a study to find an optimal dosage with minimal toxicity, 50 mg daily of thalidomide was concluded as efficacious, and remission was sustained in more than 60% of patients by a dosage of 50 mg every 2 to 3 days. Recent trials treating BD with thalidomide have used dosages ranging from 25 to 200 mg daily with reported high efficacy. Like aphthous stomatitis, some orogenital ulcerations of BD resolve without treatment, so thalidomide should be reserved for severe, unresponsive BD cases where orogenital ulcerations are prominent features of the disorder.
Lupus Erythematosus
The first reported successful thalidomide treatment of chronic cutaneous lupus erythematosus (CCLE) was in 1977 in a case series of 20 patients. Since that time, there have been at least 200 reported cases demonstrating thalidomide’s efficacy for severe CCLE. One large clinical trial of 60 patients with CCLE reported complete or marked responses in 54 patients (90%), but 71% of patients relapsed after discontinuing treatment. Patients with relapse again responded when therapy was reinitiated.
Subacute cutaneous lupus erythematosus has also shown response to thalidomide therapy. Pelle and Werth reviewed 8 separate case series that reported a total of 171 patients with various forms of cutaneous lupus treated with thalidomide. The overall response rate was 85%, with complete resolution in 59%; the response rates for discoid lupus erythematosus and subacute cutaneous lupus erythematosus were comparable at 90.3% and 82.4%, respectively.
Thalidomide has also been used to effectively treat refractory tumid lupus erythematosus, but the drug has not been as successful in treating lupus panniculitis. Coelho and colleagues reported a complete or partial response in 99% of patients with all types of cutaneous lupus treated with thalidomide (100 mg daily tapered to 50 mg daily or less when clinically feasible). Two-thirds of patients with lupus panniculitis, however, had no response to treatment.
Thalidomide has proved effective for treating cutaneous aspects of systemic lupus erythematosus (SLE) as well. Stevens and colleagues, however, observed that the drug does not significantly suppress systemic disease in SLE. Dosage for treating lupus erythematosus has varied among studies. Published treatment guidelines recommend starting at 100 to 200 mg daily. This dosage can be tapered as the clinical situation warrants. Because relapse of disease occurs in more than 70% of patients after discontinuing thalidomide, low maintenance dosages (50 mg 3–7 times weekly) may be required to sustain remission. Although shown effective in various forms of lupus erythematosus, thalidomide is still considered second-line treatment of cutaneous lupus refractory to other therapies.
Prurigo Nodularis
Prurigo nodularis (PN) is a pruritic type of neurodermatitis with skin-colored, erythematous, or hyperpigmented cutaneous nodules. Patients with PN can be difficult to treat, and standard therapies with corticosteroids and antihistamines may be ineffective. The initial report of thalidomide’s efficacy in treating PN was in 1965 by Sheskin. A more recent retrospective study presented 12 patients with PN who were given thalidomide for at least 1 month at an initial dosage of 100 mg daily. Response was noted in 8 of 12 patients, ranging from mild to moderate improvement, with complete resolution in 1 patient. In another study, 22 patients with PN were given thalidomide (50 to 300 mg daily) for a mean duration of 1 year. In 20 patients, there was immediate, pronounced alleviation of pruritus along with significant reduction in size and number of lesions after 1 to 2 months. Thirteen patients, however, discontinued treatment due to side effects, 5 of them due to neuropathy. Combination therapy of thalidomide treatment followed by narrowband ultraviolet B phototherapy has also been studied and induced excellent therapeutic response. The mechanism of thalidomide’s efficacy for PN is thought to be the drug’s direct toxic effect on proliferative neural tissues. Although thalidomide is efficacious in treating PN at higher doses, the high rate of peripheral neuropathy seen in these studies makes treatment with thalidomide at high doses less than ideal.
Sarcoidosis
There are several case reports and small, open-label, clinical trials using thalidomide to treat cutaneous sarcoidosis. In a review by Doherty and Rosen, it was reported that thalidomide dosing for sarcoidosis has ranged from 50 mg to more than 400 mg daily, and dosages for long-term maintenance have ranged from 50 mg every 15 days to 100 mg every other day. Baughman and colleagues used thalidomide to treat 14 patients with unresponsive chronic cutaneous sarcoidosis for 4 months. All patients experienced subjective improvement, and photographic scoring showed objective improvement in 10 of 12 patients. In another study, 8 patients with cutaneous sarcoidosis were treated with thalidomide for 16 weeks at a dosage of 50 mg daily increased, as needed, to a maximum of 200 mg daily; 6 patients also concomitantly received stable prednisone dosages. After treatment, skin biopsies of all 8 patients showed reductions in granuloma size and epidermal thickness. In a French study of 10 patients given thalidomide for refractory cutaneous sarcoidosis, 3 patients had total regression of skin lesions and 4 had a partial response; 3 patients had no response. The investigators noted relapse of symptoms when the drug was discontinued, but reintroduction of thalidomide was efficacious.
Sarcoidosis involves a Th1-type immune response characterized by increased levels of interferon γ (IFN-γ), interleukin (IL)-2, and IL-12. Also, tumor necrosis factor α (TNF-α) plays a major role by escalating macrophage recruitment into granulomatous lesions. Thalidomide inhibits TNF-α and IFN-γ and has also been shown to induce and enhance IL-4 and IL-5 production, indicating that thalidomide may help modulate a therapeutic switching from disease-inducing predominant Th1 activation—the type principally seen in sarcoidosis—to Th2 activation.
Actinic Prurigo
In the initial 1973 study, 32 of 34 patients with actinic prurigo exhibited clinical improvement after receiving thalidomide (initial dosage of 300 mg daily tapered to 15 mg daily for a mean of 50 days). Patients promptly relapsed, however, on discontinuation of treatment. A 1977 study of 51 patients demonstrated parallel results. In another study of 14 patients with actinic prurigo, 11 patients had lasting improvement with thalidomide (50 to 200 mg daily), but 8 patients required maintenance dosages (50 to 100 mg weekly). As is true of many of the disorders discussed in this article, actinic prurigo also may require ongoing, maintenance drug to prevent relapse of disease.
Graft-versus-host disease
Thalidomide’s efficacy for acute and chronic graft-versus-host disease (GVHD) in humans was first reported in 1988, when a patient was successfully treated with thalidomide for acute cutaneous GVHD after allogeneic bone marrow transplant. More recent studies, however, have shown mixed results. Vogelsang and colleagues used thalidomide (200 mg 4 times daily) as salvage therapy for 23 patients with refractory chronic GVHD and 21 patients with high-risk GVHD; complete response was achieved in 14 patients and partial response in 12 patients. The study concluded thalidomide is a safe and effective treatment option for chronic GVHD.
A randomized, placebo-controlled study of 59 patients concluded thalidomide was not effective as a prophylactic agent for preventing GVHD; the thalidomide group developed a higher incidence of GVHD than did the placebo group. In a 2001 randomized trial, when thalidomide was incorporated as initial therapy for GVHD in a regimen of cyclosporine and prednisone, no significant clinical benefit was found. A 2003 study compared thalidomide’s effect on 21 acute GVHD patients and 59 chronic GVHD patients. Thalidomide was not effective for acute GVHD but did produce clinical benefit in chronic GVHD, and patients responsive to thalidomide had significantly better survival rates. In the study, thalidomide was added to the regimen after patients had already started a variety of other agents, including corticosteroids, cyclosporine, and azathioprine, making the actual benefit of the thalidomide difficult to ascertain.
In summary, although thalidomide has not been shown clinically beneficial as prophylactic or first-line therapy for GVHD, thalidomide can be an effective salvage treatment of chronic GVHD. Common side effects with thalidomide treatment of GVHD include constipation, sleepiness, and neuropathy. In one case report, pancreatitis resulted from thalidomide usage for a patient with chronic GVHD.
Langerhans Cell Histiocytosis
Since the initial report in 1987, several case studies have reported that thalidomide is effective in treating Langerhans cell histiocytosis. In many instances, however, patients relapsed after cessation of treatment and ultimately required maintenance dosages. Broekaert and colleagues recommended an initial dosage of 50 to 200 mg daily and a maintenance dosage as low as 25 mg twice weekly, depending on the course of disease. These investigators also concluded that thalidomide is a safe, well-tolerated, and easy-to-administer treatment choice that is rapidly efficacious on mucocutaneous lesions. Thalidomide has not been reported to have effects on visceral manifestations of the disease, however. A recent article described a phase II trial of 15 patients, in which 7 of 9 patients without organ involvement showed complete or partial response to therapy, but all patients with organ involvement did not respond to therapy. After review of their data and previous reports, the investigators recommended thalidomide for treating patients with refractory skin and bone Langerhans cell histiocytosis but not for treatment of advanced, high-risk disease.
Erythema Multiforme
A 1982 article reported a case of recurrent erythema multiforme (EM) treated with thalidomide (200 mg daily); after a few days, the patient’s lesions on the hands, feet, lips, and glans penis healed, and there was no relapse after tapering dosage to 100 mg daily. A recent report noted an excellent response to thalidomide (200 mg daily) for 2 patients with severe, persistent EM. Neither patient relapsed with a maintenance dosage (50 mg daily), although 1 patient developed neuropathy after 2 years on thalidomide. There are several other case reports treating recurrent EM with thalidomide. In a larger retrospective study, 26 patients with EM were given thalidomide (100 mg daily) after other therapies failed. The 20 patients with recurrent disease had reduction in duration of episodes by an average of 11 days, and 6 patients had lesions disappear within 5 to 8 days, which was maintained with low-dose treatment.
Lichen Planus
Treatment of lichen planus (LP) has often been inadequate, especially for widespread cases of LP. Thalidomide has been reported to treat severe, refractory LP at dosage ranges of 25 to 300 mg daily. In a retrospective study of 6 patients with severe oral LP, thalidomide was initiated at 50 to 100 mg daily and gradually tapered. Four patients had complete healing and 1 patient had partial healing. Oral erosions rapidly recurred when thalidomide was discontinued, however, and 2 patients had side effects of phlebitis and neuropathy.
In a 2009 report, 8 patients with cutaneous LP were treated with thalidomide (100 mg daily) until they had complete resolution of lesions, although 3 patients withdrew due to neuropathy. For patients finishing the study, there was healing of skin lesions at a mean of 4 weeks and complete remission at a mean of 3 months; no recurrences were noted 6 months after treatment.
Torti and colleagues treated 50 oral LP cases through a therapeutic ladder ranging from topical corticosteroids to oral thalidomide. Among treatments, thalidomide resulted in the highest percentage (80%) of patients with substantial or complete healing, but only 5 of 50 patients were given thalidomide, because it was used only for recalcitrant cases unresponsive to other agents. Thalidomide can be a valuable treatment of LP; however, it is reserved only for severe, unresponsive disease. Dosages of 100 mg daily initially have been effective, and clinical response frequently occurs after 3 to 4 months or more of treatment. Patients must be monitored for adverse effects, especially neuropathy.
There have been a few case reports of successful thalidomide treatment of lichen planopilaris, a follicular type of LP. In contrast, a case series of 4 patients of lichen planopilaris showed no clinical improvement from thalidomide treatment.
Kaposi Sarcoma
Thalidomide was first noted to have therapeutic effects for Kaposi sarcoma (KS) in 1996, when a 14-year-old girl with HIV and KS given thalidomide for oral ulcers was noted to have improvement in KS lesions. A phase II study ensued; thalidomide (100 mg daily) was given to 17 HIV patients with KS for 8 weeks. There were 6 (35%) partial responses, but 8 patients withdrew from the study (6 due to toxicity). Another phase II trial treated 20 HIV patients who had KS with thalidomide at an initial dosage of 200 mg daily escalated to a maximum of 1000 mg daily. After a median of 6.3 months of therapy, there were 8 (40%) partial responses, with a median dosage of 500 mg daily at time of response.
Two recent articles analyzed thalidomide therapy for non–AIDS-related KS. One was a retrospective study of 11 patients who received thalidomide at a median dosage of 100 mg daily for a median duration of 16 weeks. There were 3 partial responders and 4 had stable disease, but 3 patients discontinued thalidomide due to neuropathy and vertigo. The second study also used thalidomide (100 mg daily) but treated patients for a longer duration of 12 months. Two of 3 patients had complete remission after 12 months and all 3 had partial response after 4 months. Although effective for some cases of KS—HIV-related and non–HIV-related—thalidomide has not materialized as a first-line treatment of this vascular tumor.
Jessner Lymphocytic Infiltrate
In 2 French case series, thalidomide has shown promise for treating Jessner lymphocytic infiltrate. Moulin and colleagues successfully treated 5 patients with thalidomide (100 mg daily). On stopping thalidomide, skin lesions returned in 4 patients, but continuous dosage of 25 to 50 mg daily for more than 2 years resulted in normal skin for 3 patients. The second study was a controlled, randomized, crossover trial of 28 patients. There was complete resolution in 19 (76%) patients treated with thalidomide (100 mg daily) compared with 4 (16%) patients receiving placebo. Six patients responding to thalidomide relapsed after switching to placebo. For Jessner lymphocytic infiltrate, thalidomide (100 mg daily) seems beneficial. Maintenance dosing may be needed, because withdrawal of treatment has uniformly resulted in clinical relapse.
Uremic Pruritus
For uremic patients receiving hemodialysis, pruritus occurs in 80% to 90% of patients at some point. The cause remains unclear, and no standard treatments have yet been established. In a crossover, randomized, double-blind trial, thalidomide (100 mg daily for 7 days) was compared with placebo for treating refractory uremic pruritus in 29 patients. Of 18 patients finishing the study, approximately 55% showed a response to thalidomide whereas none responded to placebo. In responsive patients, there was an average decrease of 78% to 81% in pruritus scoring. Although promising, additional investigation is needed to evaluate thalidomide’s efficacy for management of uremic pruritus.
Pyoderma Gangrenosum
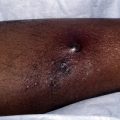
Pyoderma gangrenosum (PG) is a noninfectious skin disorder that begins as painful pustules or papulonodules that enlarge and ulcerate. Several case reports have reported thalidomide’s effectiveness in PG unresponsive to other treatments. One recent case of PG related to myelodysplastic syndrome had dramatic improvement of massive ulcerovegetative lesions after 4 months of combination therapy with IFN-α2a and thalidomide (200 mg daily). In another recent report, a patient with PG and multiple myeloma had complete healing of PG after receiving dexamethasone and thalidomide (200 mg daily for 5 weeks). Another patient with PG unresponsive to several courses of methylprednisolone had complete response to thalidomide (ranging from 100 mg to 200 mg daily over 10 weeks). In one case, thalidomide (100 mg daily) led to complete healing of PG, but withdrawal of treatment after 2 years due to neuropathy led to prompt relapse. Effective dosages of thalidomide in case reports have ranged from 100 to 400 mg daily, with treatment durations ranging from 5 days to 6 months or more. Ehling and colleagues designated thalidomide a third-choice treatment of PG, reserving thalidomide for severe, progressive disease. Controlled clinical trials are needed to further assess thalidomide’s efficacy in PG.
Scleromyxedema
Thalidomide has also been used to treat scleromyxedema. Since a report in 2004 of a scleromyxedema case responding well to thalidomide, a handful of new case reports have described remarkable improvement in skin lesions and monoclonal gammopathy after using thalidomide for scleromyxedema. In one case series, 200 mg daily given in divided doses was effective. Dosages of 100 mg daily have also been successful. Additional studies are required to assess the true efficacy of thalidomide in this setting.
Necrobiosis Lipoidica
A case of necrobiosis lipoidica that was unresponsive to therapy was treated with thalidomide (150 mg daily). Four months after initiation of therapy, there was clinical improvement in all lesions, and thalidomide was tapered to 50 mg daily. After complete resolution at 1 year of therapy, the dosage was further lowered to 50 mg twice weekly with no adverse effects or recurrence after 2 years of therapy. Further studies are needed to confirm thalidomide’s efficacy for necrobiosis lipoidica.
Off-label dermatologic uses
Aphthous Stomatitis
Several studies have shown thalidomide to be effective for recurrent aphthous stomatitis. Mascaro and colleagues reported 6 cases of aphthous stomatitis that completely resolved after 7 to 10 days of therapy with thalidomide (100 mg daily). Jenkins and colleagues reported similar results: 15 patients with aphthous stomatitis were treated with thalidomide (400 mg daily tapered to 200 mg daily). Fourteen of the patients had complete resolution of lesions within 5 to 21 days, and the remaining patient had significant improvement. Unfortunately, most of the treated patients relapsed after therapy was discontinued.
Larger, open-label, noncontrolled studies have also reported successful treatment of severe aphthosis with thalidomide. In a 40-patient trial, severe oral aphthosis was treated with thalidomide at initial dosages of 300 mg daily; mild cases were started on 100 mg daily. In both groups, 75% of patients responded well to therapy. For patients who relapsed after discontinuing therapy, the investigators recommended a dosage of 100 mg daily for 12 days. A controlled, crossover, randomized trial of 73 patients with severe aphthous stomatitis reported 32 patients (44%) with complete remission while on thalidomide (100 mg daily); most other patients in the study experienced dramatic improvement.
A recent open trial of 21 patients compared the efficacy of thalidomide, dapsone, colchicine, and pentoxifylline in treating severe recurrent aphthous stomatitis. Each patient was given 1 of the 4 test drugs for 6 months and switched drugs if toxicity or lack of efficacy occurred. Of the 4 drugs, thalidomide (100 mg daily) was the most effective and well tolerated, resulting in complete remission for 7 of 8 patients. Other studies have shown that thalidomide therapy is also an effective option for recurrent aphthous ulcers in patients with HIV. Aphthous ulcers have a variable natural course and many cases resolve spontaneously, making the interpretation of any therapeutic study somewhat difficult. Thalidomide therapy should be considered only for severe, recurrent, and seemingly recalcitrant cases.
Behçet Disease
Behçet disease (BD) is a systemic disorder with various skin lesions, ocular disease (panuveitis), arthritis, intestinal bleeding, and recurrent aphthous orogenital ulcers. After reports of thalidomide’s efficacy for aphthous stomatitis, a 1982 open trial treated 22 BD patients with thalidomide (400 mg daily for 5 days and 200 mg daily for the next 15–60 days). Although ocular and arthritic symptoms did not improve, orogenital ulcerations healed quickly. Ulcers recurred after withdrawal of thalidomide, but they were milder and less frequent than before treatment. Other studies have shown similar beneficial effects but have also noted recurrence of disease after treatment ended.
A randomized, double-blind trial compared thalidomide dosages (100 mg daily and 300 mg daily) to placebo. The results showed thalidomide dosages of 100 mg daily to be similar in efficacy to 300 mg daily, with both dosages demonstrating better efficacy compared with the placebo control. Withdrawal of either treatment dosage led to prompt recurrence. In a study to find an optimal dosage with minimal toxicity, 50 mg daily of thalidomide was concluded as efficacious, and remission was sustained in more than 60% of patients by a dosage of 50 mg every 2 to 3 days. Recent trials treating BD with thalidomide have used dosages ranging from 25 to 200 mg daily with reported high efficacy. Like aphthous stomatitis, some orogenital ulcerations of BD resolve without treatment, so thalidomide should be reserved for severe, unresponsive BD cases where orogenital ulcerations are prominent features of the disorder.
Lupus Erythematosus
The first reported successful thalidomide treatment of chronic cutaneous lupus erythematosus (CCLE) was in 1977 in a case series of 20 patients. Since that time, there have been at least 200 reported cases demonstrating thalidomide’s efficacy for severe CCLE. One large clinical trial of 60 patients with CCLE reported complete or marked responses in 54 patients (90%), but 71% of patients relapsed after discontinuing treatment. Patients with relapse again responded when therapy was reinitiated.
Subacute cutaneous lupus erythematosus has also shown response to thalidomide therapy. Pelle and Werth reviewed 8 separate case series that reported a total of 171 patients with various forms of cutaneous lupus treated with thalidomide. The overall response rate was 85%, with complete resolution in 59%; the response rates for discoid lupus erythematosus and subacute cutaneous lupus erythematosus were comparable at 90.3% and 82.4%, respectively.
Thalidomide has also been used to effectively treat refractory tumid lupus erythematosus, but the drug has not been as successful in treating lupus panniculitis. Coelho and colleagues reported a complete or partial response in 99% of patients with all types of cutaneous lupus treated with thalidomide (100 mg daily tapered to 50 mg daily or less when clinically feasible). Two-thirds of patients with lupus panniculitis, however, had no response to treatment.
Thalidomide has proved effective for treating cutaneous aspects of systemic lupus erythematosus (SLE) as well. Stevens and colleagues, however, observed that the drug does not significantly suppress systemic disease in SLE. Dosage for treating lupus erythematosus has varied among studies. Published treatment guidelines recommend starting at 100 to 200 mg daily. This dosage can be tapered as the clinical situation warrants. Because relapse of disease occurs in more than 70% of patients after discontinuing thalidomide, low maintenance dosages (50 mg 3–7 times weekly) may be required to sustain remission. Although shown effective in various forms of lupus erythematosus, thalidomide is still considered second-line treatment of cutaneous lupus refractory to other therapies.
Prurigo Nodularis
Prurigo nodularis (PN) is a pruritic type of neurodermatitis with skin-colored, erythematous, or hyperpigmented cutaneous nodules. Patients with PN can be difficult to treat, and standard therapies with corticosteroids and antihistamines may be ineffective. The initial report of thalidomide’s efficacy in treating PN was in 1965 by Sheskin. A more recent retrospective study presented 12 patients with PN who were given thalidomide for at least 1 month at an initial dosage of 100 mg daily. Response was noted in 8 of 12 patients, ranging from mild to moderate improvement, with complete resolution in 1 patient. In another study, 22 patients with PN were given thalidomide (50 to 300 mg daily) for a mean duration of 1 year. In 20 patients, there was immediate, pronounced alleviation of pruritus along with significant reduction in size and number of lesions after 1 to 2 months. Thirteen patients, however, discontinued treatment due to side effects, 5 of them due to neuropathy. Combination therapy of thalidomide treatment followed by narrowband ultraviolet B phototherapy has also been studied and induced excellent therapeutic response. The mechanism of thalidomide’s efficacy for PN is thought to be the drug’s direct toxic effect on proliferative neural tissues. Although thalidomide is efficacious in treating PN at higher doses, the high rate of peripheral neuropathy seen in these studies makes treatment with thalidomide at high doses less than ideal.
Sarcoidosis
There are several case reports and small, open-label, clinical trials using thalidomide to treat cutaneous sarcoidosis. In a review by Doherty and Rosen, it was reported that thalidomide dosing for sarcoidosis has ranged from 50 mg to more than 400 mg daily, and dosages for long-term maintenance have ranged from 50 mg every 15 days to 100 mg every other day. Baughman and colleagues used thalidomide to treat 14 patients with unresponsive chronic cutaneous sarcoidosis for 4 months. All patients experienced subjective improvement, and photographic scoring showed objective improvement in 10 of 12 patients. In another study, 8 patients with cutaneous sarcoidosis were treated with thalidomide for 16 weeks at a dosage of 50 mg daily increased, as needed, to a maximum of 200 mg daily; 6 patients also concomitantly received stable prednisone dosages. After treatment, skin biopsies of all 8 patients showed reductions in granuloma size and epidermal thickness. In a French study of 10 patients given thalidomide for refractory cutaneous sarcoidosis, 3 patients had total regression of skin lesions and 4 had a partial response; 3 patients had no response. The investigators noted relapse of symptoms when the drug was discontinued, but reintroduction of thalidomide was efficacious.
Sarcoidosis involves a Th1-type immune response characterized by increased levels of interferon γ (IFN-γ), interleukin (IL)-2, and IL-12. Also, tumor necrosis factor α (TNF-α) plays a major role by escalating macrophage recruitment into granulomatous lesions. Thalidomide inhibits TNF-α and IFN-γ and has also been shown to induce and enhance IL-4 and IL-5 production, indicating that thalidomide may help modulate a therapeutic switching from disease-inducing predominant Th1 activation—the type principally seen in sarcoidosis—to Th2 activation.
Actinic Prurigo
In the initial 1973 study, 32 of 34 patients with actinic prurigo exhibited clinical improvement after receiving thalidomide (initial dosage of 300 mg daily tapered to 15 mg daily for a mean of 50 days). Patients promptly relapsed, however, on discontinuation of treatment. A 1977 study of 51 patients demonstrated parallel results. In another study of 14 patients with actinic prurigo, 11 patients had lasting improvement with thalidomide (50 to 200 mg daily), but 8 patients required maintenance dosages (50 to 100 mg weekly). As is true of many of the disorders discussed in this article, actinic prurigo also may require ongoing, maintenance drug to prevent relapse of disease.
Graft-versus-host disease
Thalidomide’s efficacy for acute and chronic graft-versus-host disease (GVHD) in humans was first reported in 1988, when a patient was successfully treated with thalidomide for acute cutaneous GVHD after allogeneic bone marrow transplant. More recent studies, however, have shown mixed results. Vogelsang and colleagues used thalidomide (200 mg 4 times daily) as salvage therapy for 23 patients with refractory chronic GVHD and 21 patients with high-risk GVHD; complete response was achieved in 14 patients and partial response in 12 patients. The study concluded thalidomide is a safe and effective treatment option for chronic GVHD.
A randomized, placebo-controlled study of 59 patients concluded thalidomide was not effective as a prophylactic agent for preventing GVHD; the thalidomide group developed a higher incidence of GVHD than did the placebo group. In a 2001 randomized trial, when thalidomide was incorporated as initial therapy for GVHD in a regimen of cyclosporine and prednisone, no significant clinical benefit was found. A 2003 study compared thalidomide’s effect on 21 acute GVHD patients and 59 chronic GVHD patients. Thalidomide was not effective for acute GVHD but did produce clinical benefit in chronic GVHD, and patients responsive to thalidomide had significantly better survival rates. In the study, thalidomide was added to the regimen after patients had already started a variety of other agents, including corticosteroids, cyclosporine, and azathioprine, making the actual benefit of the thalidomide difficult to ascertain.
In summary, although thalidomide has not been shown clinically beneficial as prophylactic or first-line therapy for GVHD, thalidomide can be an effective salvage treatment of chronic GVHD. Common side effects with thalidomide treatment of GVHD include constipation, sleepiness, and neuropathy. In one case report, pancreatitis resulted from thalidomide usage for a patient with chronic GVHD.
Langerhans Cell Histiocytosis
Since the initial report in 1987, several case studies have reported that thalidomide is effective in treating Langerhans cell histiocytosis. In many instances, however, patients relapsed after cessation of treatment and ultimately required maintenance dosages. Broekaert and colleagues recommended an initial dosage of 50 to 200 mg daily and a maintenance dosage as low as 25 mg twice weekly, depending on the course of disease. These investigators also concluded that thalidomide is a safe, well-tolerated, and easy-to-administer treatment choice that is rapidly efficacious on mucocutaneous lesions. Thalidomide has not been reported to have effects on visceral manifestations of the disease, however. A recent article described a phase II trial of 15 patients, in which 7 of 9 patients without organ involvement showed complete or partial response to therapy, but all patients with organ involvement did not respond to therapy. After review of their data and previous reports, the investigators recommended thalidomide for treating patients with refractory skin and bone Langerhans cell histiocytosis but not for treatment of advanced, high-risk disease.
Erythema Multiforme
A 1982 article reported a case of recurrent erythema multiforme (EM) treated with thalidomide (200 mg daily); after a few days, the patient’s lesions on the hands, feet, lips, and glans penis healed, and there was no relapse after tapering dosage to 100 mg daily. A recent report noted an excellent response to thalidomide (200 mg daily) for 2 patients with severe, persistent EM. Neither patient relapsed with a maintenance dosage (50 mg daily), although 1 patient developed neuropathy after 2 years on thalidomide. There are several other case reports treating recurrent EM with thalidomide. In a larger retrospective study, 26 patients with EM were given thalidomide (100 mg daily) after other therapies failed. The 20 patients with recurrent disease had reduction in duration of episodes by an average of 11 days, and 6 patients had lesions disappear within 5 to 8 days, which was maintained with low-dose treatment.
Lichen Planus
Treatment of lichen planus (LP) has often been inadequate, especially for widespread cases of LP. Thalidomide has been reported to treat severe, refractory LP at dosage ranges of 25 to 300 mg daily. In a retrospective study of 6 patients with severe oral LP, thalidomide was initiated at 50 to 100 mg daily and gradually tapered. Four patients had complete healing and 1 patient had partial healing. Oral erosions rapidly recurred when thalidomide was discontinued, however, and 2 patients had side effects of phlebitis and neuropathy.
In a 2009 report, 8 patients with cutaneous LP were treated with thalidomide (100 mg daily) until they had complete resolution of lesions, although 3 patients withdrew due to neuropathy. For patients finishing the study, there was healing of skin lesions at a mean of 4 weeks and complete remission at a mean of 3 months; no recurrences were noted 6 months after treatment.
Torti and colleagues treated 50 oral LP cases through a therapeutic ladder ranging from topical corticosteroids to oral thalidomide. Among treatments, thalidomide resulted in the highest percentage (80%) of patients with substantial or complete healing, but only 5 of 50 patients were given thalidomide, because it was used only for recalcitrant cases unresponsive to other agents. Thalidomide can be a valuable treatment of LP; however, it is reserved only for severe, unresponsive disease. Dosages of 100 mg daily initially have been effective, and clinical response frequently occurs after 3 to 4 months or more of treatment. Patients must be monitored for adverse effects, especially neuropathy.
There have been a few case reports of successful thalidomide treatment of lichen planopilaris, a follicular type of LP. In contrast, a case series of 4 patients of lichen planopilaris showed no clinical improvement from thalidomide treatment.
Kaposi Sarcoma
Thalidomide was first noted to have therapeutic effects for Kaposi sarcoma (KS) in 1996, when a 14-year-old girl with HIV and KS given thalidomide for oral ulcers was noted to have improvement in KS lesions. A phase II study ensued; thalidomide (100 mg daily) was given to 17 HIV patients with KS for 8 weeks. There were 6 (35%) partial responses, but 8 patients withdrew from the study (6 due to toxicity). Another phase II trial treated 20 HIV patients who had KS with thalidomide at an initial dosage of 200 mg daily escalated to a maximum of 1000 mg daily. After a median of 6.3 months of therapy, there were 8 (40%) partial responses, with a median dosage of 500 mg daily at time of response.
Two recent articles analyzed thalidomide therapy for non–AIDS-related KS. One was a retrospective study of 11 patients who received thalidomide at a median dosage of 100 mg daily for a median duration of 16 weeks. There were 3 partial responders and 4 had stable disease, but 3 patients discontinued thalidomide due to neuropathy and vertigo. The second study also used thalidomide (100 mg daily) but treated patients for a longer duration of 12 months. Two of 3 patients had complete remission after 12 months and all 3 had partial response after 4 months. Although effective for some cases of KS—HIV-related and non–HIV-related—thalidomide has not materialized as a first-line treatment of this vascular tumor.
Jessner Lymphocytic Infiltrate
In 2 French case series, thalidomide has shown promise for treating Jessner lymphocytic infiltrate. Moulin and colleagues successfully treated 5 patients with thalidomide (100 mg daily). On stopping thalidomide, skin lesions returned in 4 patients, but continuous dosage of 25 to 50 mg daily for more than 2 years resulted in normal skin for 3 patients. The second study was a controlled, randomized, crossover trial of 28 patients. There was complete resolution in 19 (76%) patients treated with thalidomide (100 mg daily) compared with 4 (16%) patients receiving placebo. Six patients responding to thalidomide relapsed after switching to placebo. For Jessner lymphocytic infiltrate, thalidomide (100 mg daily) seems beneficial. Maintenance dosing may be needed, because withdrawal of treatment has uniformly resulted in clinical relapse.
Uremic Pruritus
For uremic patients receiving hemodialysis, pruritus occurs in 80% to 90% of patients at some point. The cause remains unclear, and no standard treatments have yet been established. In a crossover, randomized, double-blind trial, thalidomide (100 mg daily for 7 days) was compared with placebo for treating refractory uremic pruritus in 29 patients. Of 18 patients finishing the study, approximately 55% showed a response to thalidomide whereas none responded to placebo. In responsive patients, there was an average decrease of 78% to 81% in pruritus scoring. Although promising, additional investigation is needed to evaluate thalidomide’s efficacy for management of uremic pruritus.
Pyoderma Gangrenosum
Pyoderma gangrenosum (PG) is a noninfectious skin disorder that begins as painful pustules or papulonodules that enlarge and ulcerate. Several case reports have reported thalidomide’s effectiveness in PG unresponsive to other treatments. One recent case of PG related to myelodysplastic syndrome had dramatic improvement of massive ulcerovegetative lesions after 4 months of combination therapy with IFN-α2a and thalidomide (200 mg daily). In another recent report, a patient with PG and multiple myeloma had complete healing of PG after receiving dexamethasone and thalidomide (200 mg daily for 5 weeks). Another patient with PG unresponsive to several courses of methylprednisolone had complete response to thalidomide (ranging from 100 mg to 200 mg daily over 10 weeks). In one case, thalidomide (100 mg daily) led to complete healing of PG, but withdrawal of treatment after 2 years due to neuropathy led to prompt relapse. Effective dosages of thalidomide in case reports have ranged from 100 to 400 mg daily, with treatment durations ranging from 5 days to 6 months or more. Ehling and colleagues designated thalidomide a third-choice treatment of PG, reserving thalidomide for severe, progressive disease. Controlled clinical trials are needed to further assess thalidomide’s efficacy in PG.
Scleromyxedema
Thalidomide has also been used to treat scleromyxedema. Since a report in 2004 of a scleromyxedema case responding well to thalidomide, a handful of new case reports have described remarkable improvement in skin lesions and monoclonal gammopathy after using thalidomide for scleromyxedema. In one case series, 200 mg daily given in divided doses was effective. Dosages of 100 mg daily have also been successful. Additional studies are required to assess the true efficacy of thalidomide in this setting.
Necrobiosis Lipoidica
A case of necrobiosis lipoidica that was unresponsive to therapy was treated with thalidomide (150 mg daily). Four months after initiation of therapy, there was clinical improvement in all lesions, and thalidomide was tapered to 50 mg daily. After complete resolution at 1 year of therapy, the dosage was further lowered to 50 mg twice weekly with no adverse effects or recurrence after 2 years of therapy. Further studies are needed to confirm thalidomide’s efficacy for necrobiosis lipoidica.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree