Chapter 4
Incisional Hernias
4.3Laparoscopic Repair of Incisional Hernias
4 Incisional Hernias
4.1 General Principles
4.1.1 Definition
Incisional hernias arise at the site of a previous laparotomy incision. They consist of a hernial orifice and peritoneal sac.
4.1.2 Diagnosis
Clinical examination to palpate the hernia usually suffices. In obese patients and/or when the defect is small, ultrasound of the abdominal wall is the standard method of detection. The width of the defect is the most important aspect. CT or MRI is indicated only with large loss-of-domain hernias.
Preoperative lung function tests may be appropriate depending on defect size and/or respiratory impairment.
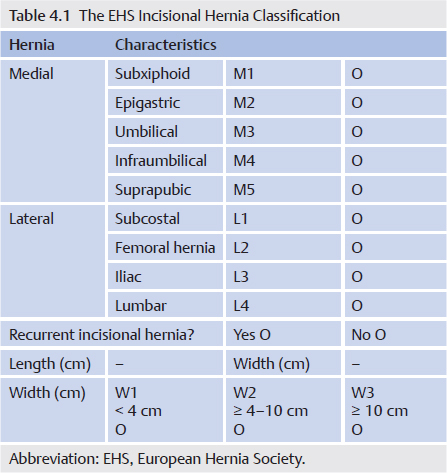
4.1.3 Classification
The European Hernia Society (EHS) classification is shown in  Table 4.1.
Table 4.1.
4.1.4 Indications
 Absolute indications. Incarceration, intestinal strangulation, or perforation of the bowel in the sac.
Absolute indications. Incarceration, intestinal strangulation, or perforation of the bowel in the sac.
 Relative indications. Persistent symptoms, sustained incapacity for work, social deprivation, increase in size. The interval since the last operation should be more than 6 months to allow adequate fascial strength to be regained.
Relative indications. Persistent symptoms, sustained incapacity for work, social deprivation, increase in size. The interval since the last operation should be more than 6 months to allow adequate fascial strength to be regained.
 Contraindications. Peritoneal carcinomatosis, general inoperability, especially respiratory impairment, absent consent.
Contraindications. Peritoneal carcinomatosis, general inoperability, especially respiratory impairment, absent consent.
4.1.5 Preoperative Preparation and Informed Consent
Uninfected skin is desirable for elective surgery and pressure ulcers should be treated conservatively in the first instance.
An enema is given the night before the operation. Orthograde bowel washout is not indicated.
The patient should be given a careful explanation of possible risks and complications.90 These include:
• Wound seroma.
• Wound infection (5–15%).
• Foreign body sensation.
• Bowel injury (~ 2%).
• Chronic pain (~5–15%).
• Recurrence (2–10%).
4.1.6 Anesthesia
General anesthesia.
4.1.7 Position
The patients’s position depends on the location, slightly hyperextended during dissection and neutral position during repair.
4.1.8 Operation Tactics
Numerous repair procedures are available to the surgeon. They differ basically as follows:
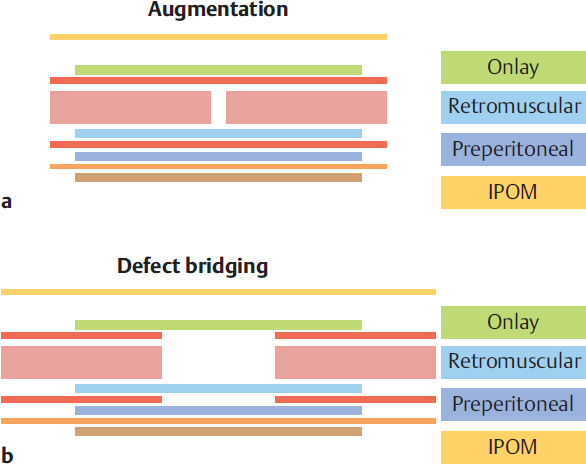
• With mesh augmentation, the abdominal wall is reinforced ( Fig. 4.2).
Fig. 4.2).
• With mesh bridging, the abdominal wall is partially replaced ( Fig. 4.66).
Fig. 4.66).
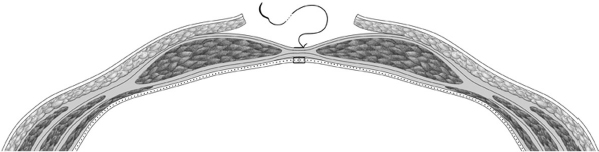
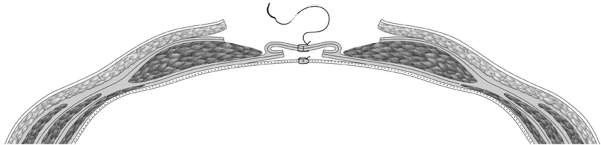
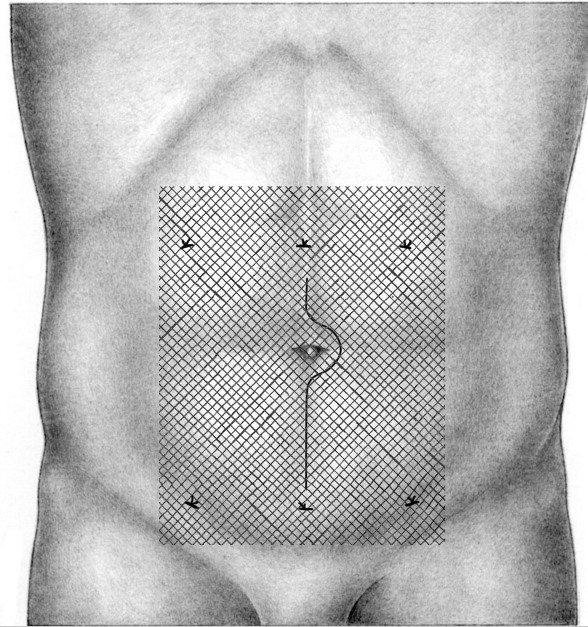
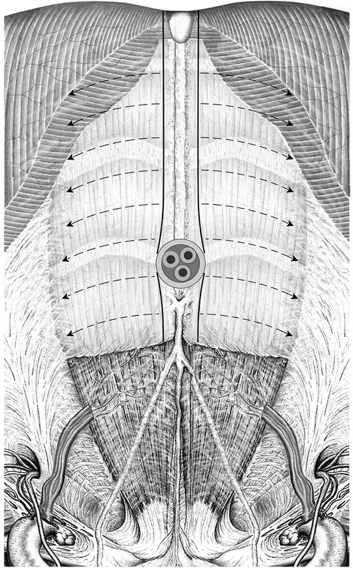
Access can be open or laparoscopic. In an open repair, the mesh can be inserted as an onlay on the fascia, as a sublay (retromuscular) on the posterior layer of the rectus sheath, in preperitoneal position between fascia and peritoneum, or as an intraperitoneal onlay mesh (IPOM,  Fig. 4.1).
Fig. 4.1).
4.1.9 Perioperative Management
Time out.
Perioperative antibiotics, e.g., 1.5 g cefuroxime, and 0.5 g metronidazole, if appropriate, 30 minutes before skin incision; the old incision may be marked and an adhesive drape can be applied.
4.2 Open Technique
4.2.1 Open Sublay (Retromuscular Augmentation)
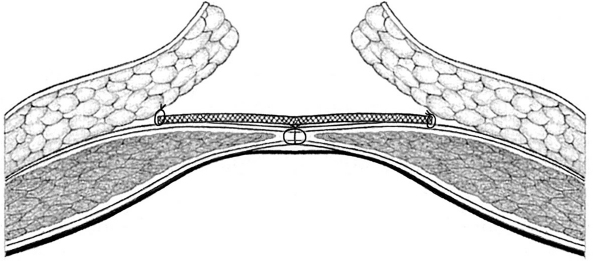
In a sublay repair, the anterior abdominal wall is reinforced with mesh behind the rectus muscle medially or between the external and internal oblique muscles. The aim should always be augmentation of the abdominal wall, i.e., fascial closure should be achieved ( Fig. 4.2). If it is not possible to approximate the fascial edges without tension after dissection of the retromuscular mesh site, separation of the abdominal wall components should be attempted (section
Fig. 4.2). If it is not possible to approximate the fascial edges without tension after dissection of the retromuscular mesh site, separation of the abdominal wall components should be attempted (section  4.3.8). If fascial closure is still not possible, mesh bridging should be considered.
4.3.8). If fascial closure is still not possible, mesh bridging should be considered.
Operation Techniques
See also Conze et al, 2010.22
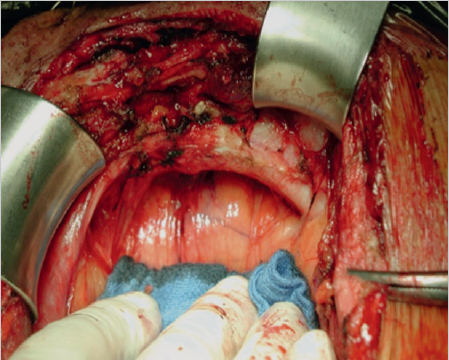
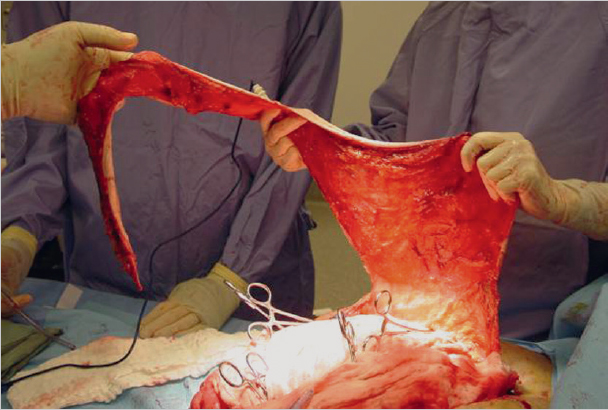
Excision of the Entire Skin Scar, Dissection of the Hernial Sac, and Exposure of the Fascial Defect
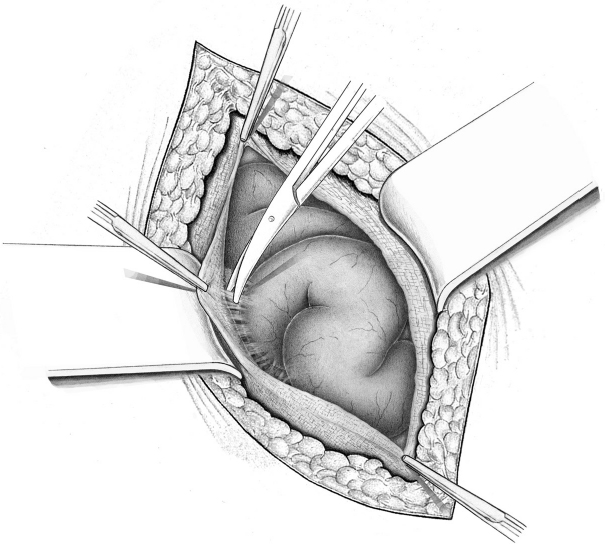
The entire length of the existing skin scar is excised. The hernial sac is dissected gradually from the subcutaneous tissue as far as the edge of the fascial defect. This is then exposed circumferentially and the sac is opened. This provides better vision, prevents further fascial defects from being missed, and avoids iatrogenic bowel injury during dissection of the mesh site. The entire fascial scar is incised under vision (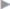 Fig. 4.3).
Fig. 4.3).
Opening of the Hernial Sac, Local Adhesiolysis, and Exploration of the Abdomen
After dissecting the sac from the subcutaneous tissue, it is incised and the abdomen is opened, preserving the sac. This can be resected later. This ensures that enough tissue is available to close the posterior abdominal wall incision. Local adhesions to the anterior abdominal wall are then divided (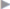 Fig. 4.4). Adhesions between loops of intestine should be divided only if they give rise to clinical symptoms. The abdominal contents are then covered with a moist towel.
Fig. 4.4). Adhesions between loops of intestine should be divided only if they give rise to clinical symptoms. The abdominal contents are then covered with a moist towel.
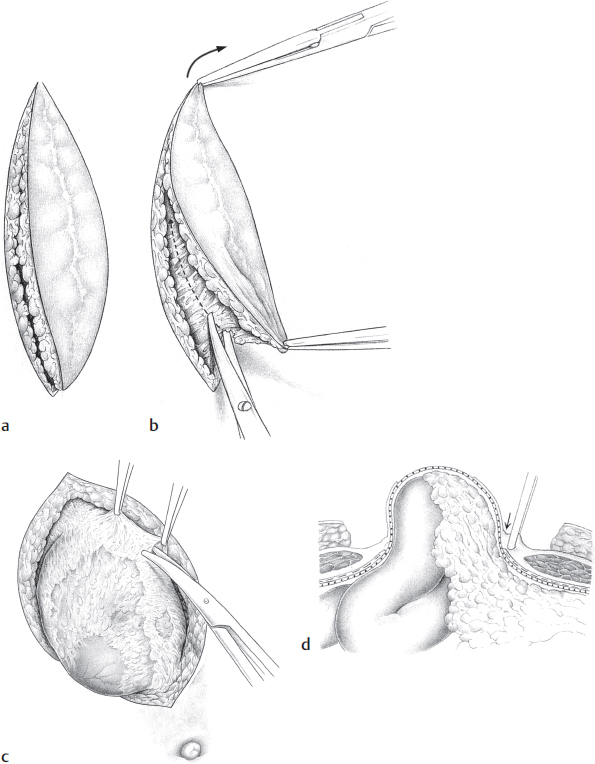
Fig. 4.3 a–d
a Excision of the skin and subcutaneous tissue.
b Dissection down to fascia.
c Circumferential exposure of the fascial edges.
d Dissection of the sac and fascial edges. They are divided from the subcutaneous tissue by sharp dissection (cross-section).
Dissection of the Anterior Fascia
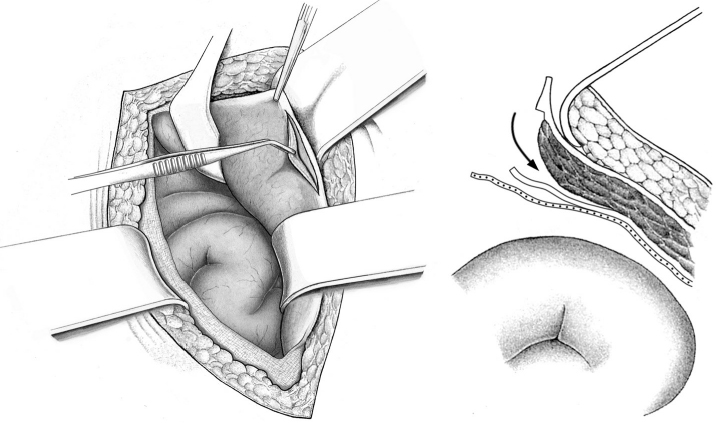
Epifascial dissection of the anterior fascia should be sparing and not exceed 5 mm (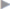 Fig. 4.5). This facilitates subsequent dissection of the mesh site and later fascial closure.
Fig. 4.5). This facilitates subsequent dissection of the mesh site and later fascial closure.
Incision of the Rectus Sheath
The rectus sheath is incised and entered from the medial side (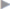 Fig. 4.6).
Fig. 4.6).
Tip
Ensure that as much as possible of the anterior rectus sheath is preserved to provide adequate tissue for subsequent suture placement for closing the fascia.
A vertical incision provides access to the vertical fibers of the rectus muscle. This muscle serves as a guide for further incision.
Dissection of the Retromuscular Mesh Site
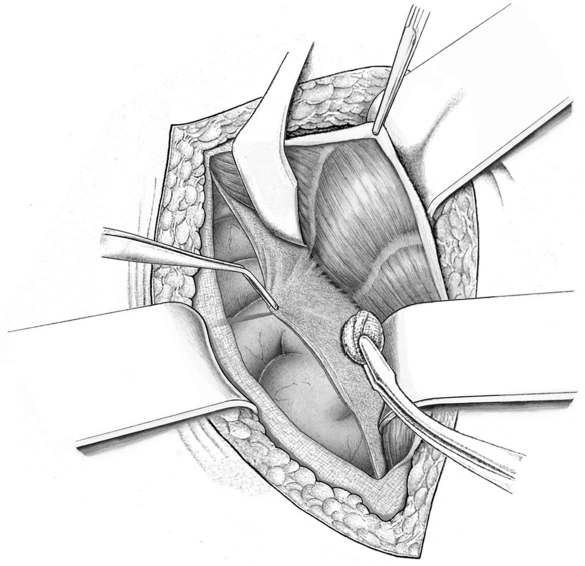
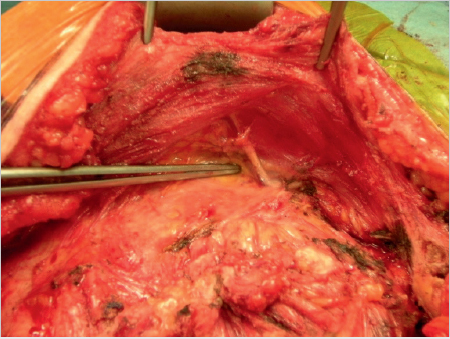
Leaving the belly of the muscle on the anterior fascia, the posterior layer of the rectus sheath can now be dissected largely bluntly as far as its lateral border. The epigastric vessels and segmental perforating vessels should be preserved when possible (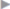 Fig. 4.7). Below the arcuate line, the posterior layer of the rectus sheath merges with the anterior layer so dissection here is preperitoneal. In the case of medial lower abdominal defects, this allows seamless dissection into the retrosymphyseal space (
Fig. 4.7). Below the arcuate line, the posterior layer of the rectus sheath merges with the anterior layer so dissection here is preperitoneal. In the case of medial lower abdominal defects, this allows seamless dissection into the retrosymphyseal space (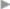 Fig. 4.8).
Fig. 4.8).
Depending on the extent of the fascial defect, this can necessitate detachment of the posterior layer of the rectus sheath from the xiphoid process cranially. The retroxiphoid space is reached to allow adequate mesh overlapping (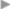 Fig. 4.9).
Fig. 4.9).
Fig. 4.8 Dissection plane at the symphysis; dissection is continued in the preperitoneal space between the bladder and symphysis (space of Retzius).
Fig. 4.9 Dissection plane at the xiphoid; the retroxiphoid space is reached by detaching the posterior layer of the rectus sheath from the xiphoid.
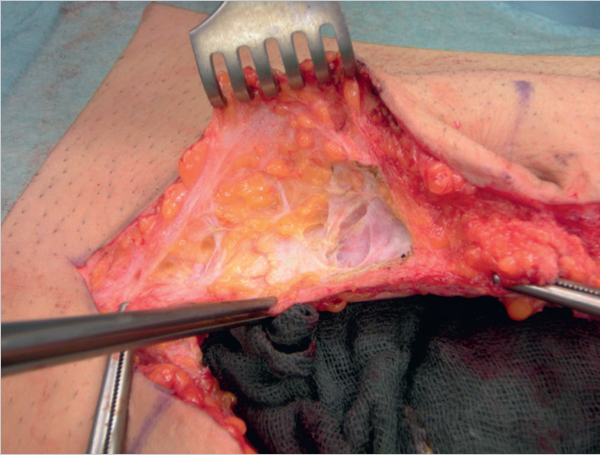
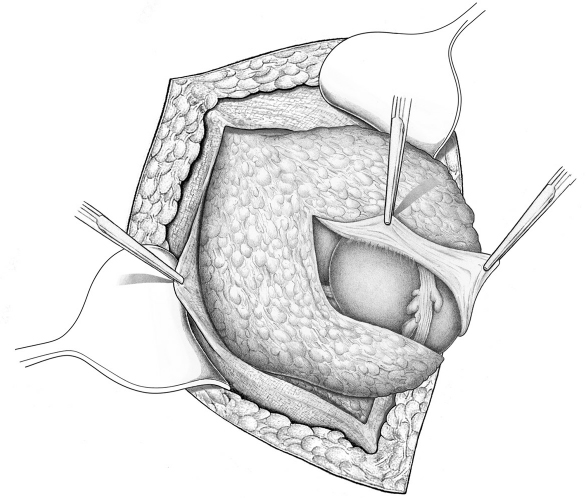
Fig. 4.10 Exposure of the fatty triangle by incision of the posterior layer of the rectus sheath on both sides of the linea alba.
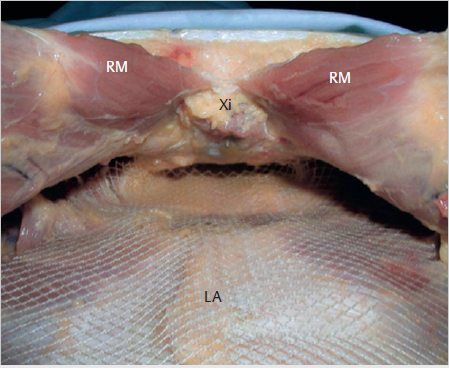
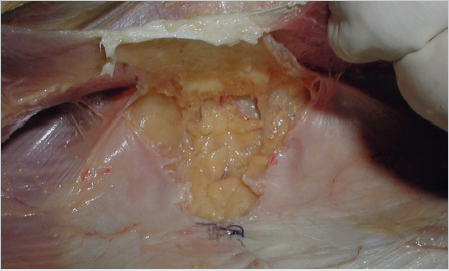
Incision of the Posterior Layer of the Rectus Sheath on Both Sides of the Linea Alba to Expose the Fatty Triangle
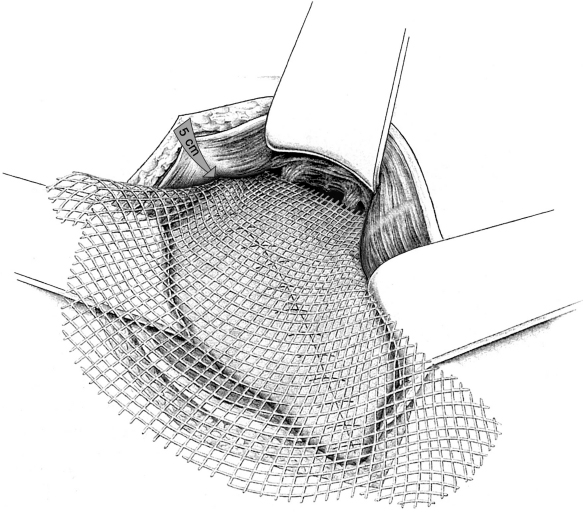
To enable sufficient mesh to be placed in the midline behind the linea alba, a vertical incision is made in the posterior layer of the rectus sheath on both sides of the linea alba. This exposes the yellowish preperitoneal fatty triangle. The incision should be at least 5 cm long (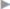 Fig. 4.10).
Fig. 4.10).
When the fascial defect is proximal to the arcuate line, this dissection must also be continued caudally to ensure adequate mesh overlapping (inferior fatty triangle).
Closure of the Abdomen/Suture of the Posterior Wall (Peritoneum)
When dissection is concluded, the abdomen is closed by a continuous suture of the posterior layer of the rectus sheath with absorbable material (e.g., polydioxanone [PDS] 2). The peritoneum is approximated below the arcuate line (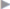 Fig. 4.11).
Fig. 4.11).
Tip
If low-tension approximation is not possible because of the width of the defect, parts of the hernial sac can be used for this. Protruding parts of the sac are only resected thereafter.
The aim of this suture is creation of a natural tissue barrier to avoid direct contact between the mesh and the abdominal viscera.
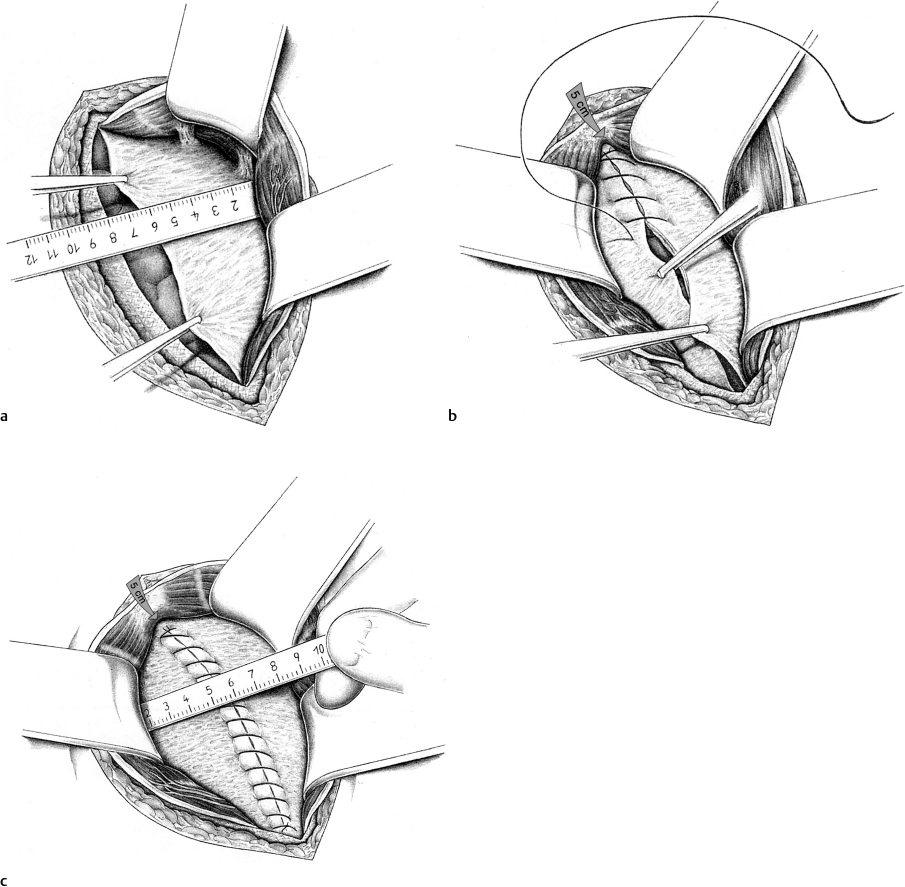
Measurement of the Mesh Site and Mesh Placement
After meticulous hemostasis, the mesh site is measured and a mesh graft is cut to size.
When placing the mesh, it must lie flat without creases and overlap the closed defect by at least 5 to 6 cm in all directions (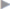 Fig. 4.12). Depending on which mesh type is used, the greatest elasticity should be in the direction of the muscle fibers.
Fig. 4.12). Depending on which mesh type is used, the greatest elasticity should be in the direction of the muscle fibers.
In retromuscular mesh augmentation, the mesh reinforces the abdominal wall and does not replace it. Nonabsorbable, large-pored mesh with a reduced surface is used for augmentation.
Mesh Fixation Only with Bridging Techniques using Transfascial Interrupted Sutures
Mesh fixation is not required for retromuscular mesh augmentation. The anterior fascial closure acts as an abutment for the intra-abdominal pressure which holds the mesh in position. To facilitate crease-free mesh placement, the proximal edge of the mesh can be fixed to the linea alba with an absorbable interrupted suture. This can make it easier to spread out a larger mesh.
Fig. 4.11 Continuous suture of the posterior rectus sheath, if necessary using parts of the hernial sac.
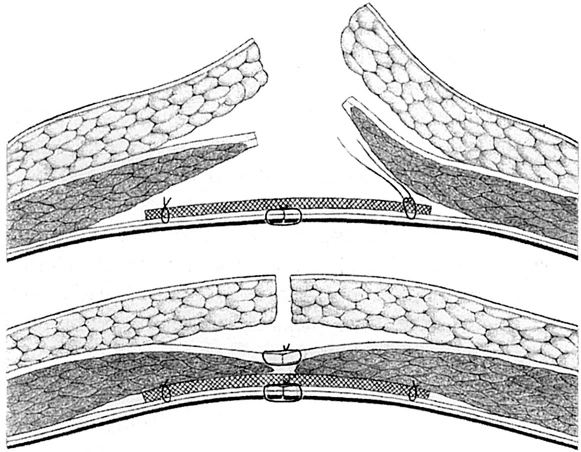
If it is impossible to create an appropriate thrust bearing because of the width of the defect and a bridging repair must be performed, the mesh must be fixed to the anterior fascia with transfascial sutures. These are placed in a circle at intervals of 3 to 4 cm. To avoid further retraction of the fascial edge, it is stitched to the mesh with a continuous nonabsorbable suture (e.g., Prolene 2/0); this is the bridging technique (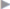 Fig. 4.13).
Fig. 4.13).
Fig. 4.13 Mesh placement with transfascial mesh fixation in the bridging technique for large fascial defects.
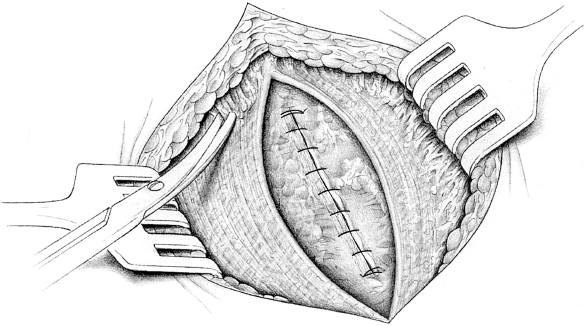
Continuous Fascial Closure of the Anterior Rectus Sheath
The anterior rectus sheath is closed with a continuous nonabsorbable suture to reconstruct the linea alba (e.g., 2/0 Prolene; 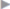 Fig. 4.14). It must be carefully ensured that only the fascial edge is included in the suture. The stitches are placed 5 to 8 mm from the edge of the fascia and at intervals of 3 to 5 mm (“small stitch–small bite”). The ratio between the suture length and wound length should be 4:1.58 Tension-free approximation of the fascial edges is essential so the sutures do not tear out.
Fig. 4.14). It must be carefully ensured that only the fascial edge is included in the suture. The stitches are placed 5 to 8 mm from the edge of the fascia and at intervals of 3 to 5 mm (“small stitch–small bite”). The ratio between the suture length and wound length should be 4:1.58 Tension-free approximation of the fascial edges is essential so the sutures do not tear out.
Subcutaneous Suture, Reattachment of the Umbilicus if Necessary, and Skin Closure
The subcutaneous wound area is irrigated with warm saline. The detached umbilical column is fixed to the midline of the fascia with an absorbable suture (e.g., PDS 2/0). Wound drains are placed only after more extensive epifascial dissection. The subcutaneous tissue and skin are closed with staples or a continuous intracutaneous suture (e.g., Monocryl 4/0;  Fig. 4.15).
Fig. 4.15).
The operation concludes with a sterile wound dressing.
Relevant Anatomy, Dangers, and Tricks
• The epigastric vessels and their perforating branches always run within the rectus sheath at the lateral border. These should be protected during dissection of the mesh site ( Fig. 4.16).
Fig. 4.16).
• If extension of the retromuscular layer into the lateral compartment of the abdominal wall lateral to the rectus sheath is necessary for mesh insertion, this can be achieved by a vertical incision at the lateral border of the rectus sheath.
• Since the neurovascular structures run mainly between the internal oblique and transversus muscles, the lateral mesh position should be between the internal oblique and external oblique muscle.
Management of Special Complications
• Injury of the epigastric artery: ligature.
• Transmural bowel injury: bowel suture and generous irrigation.
• Postoperative hematoma: surgical evacuation of the hematoma.
• Mesh infection: antibiotic therapy, interventional drain insertion or VAC therapy, mesh explantation if necessary.
Postoperative Care
 Medical care. The vacuum drains are removed when the amount is < 10-20 mL/d. The patient should be provided with an information leaflet on gradual resumption of physical effort.
Medical care. The vacuum drains are removed when the amount is < 10-20 mL/d. The patient should be provided with an information leaflet on gradual resumption of physical effort.
 Diet. This depends on the extent of adhesiolysis and postoperative resumption of bowel activity. Liquid diet is usually well tolerated on the first postoperative day.
Diet. This depends on the extent of adhesiolysis and postoperative resumption of bowel activity. Liquid diet is usually well tolerated on the first postoperative day.
 Bowels. If resumption of bowel evacuation is sluggish, an enema should be given from postoperative day 3.
Bowels. If resumption of bowel evacuation is sluggish, an enema should be given from postoperative day 3.
 Mobilization. Mobilization is possible immediately on arrival on the ward with nursing support.
Mobilization. Mobilization is possible immediately on arrival on the ward with nursing support.
 Physical therapy. Physical therapy depends on the extent of the repair and pre-existing comorbidity, especially respiratory therapy.
Physical therapy. Physical therapy depends on the extent of the repair and pre-existing comorbidity, especially respiratory therapy.
 Incapacity for work. Two to three weeks.
Incapacity for work. Two to three weeks.
4.2.2 Open Onlay (Epifascial Mesh Augmentation)
Operation Technique
The operation technique is shown schematically in 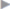 Fig. 4.17.
Fig. 4.17.
Excision of the Entire Skin Scar, Dissection of the Hernial Sac, and Exposure of the Fascial Defect
The entire length of the existing skin scar is excised sparingly. The hernial sac is dissected gradually from the subcutaneous tissue as far as the edge of the fascial defect.
Opening of the Abdominal Cavity If Necessary and Local Adhesiolysis
The sac is opened only if it is irreducible or compromised hernia contents are suspected (ischemia, necrosis, etc.). After managing the contents, the sac is closed again with a continuous suture (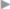 Fig. 4.18).
Fig. 4.18).
Dissection of the Anterior Fascia
Starting from the medial fascial border, the layer between the subcutaneous tissue and anterior fascia is dissected for 5 cm in all directions around the fascial edge (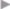 Fig. 4.19). Careful hemostasis must be ensured.
Fig. 4.19). Careful hemostasis must be ensured.
Continuous Fascial Closure with Relaxing Swing Door Incision If Required
The medial fascial edges are approximated with a continuous nonabsorbable monofilament suture (e.g., Prolene 2/0; 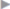 Fig. 4.20).
Fig. 4.20).
If direct fascial approximation is not possible, a “swing door” incision can be made: the anterior layer of the rectus sheath is incised over its entire length 1 to 2 cm lateral to the fascial defect, and the medial part is turned inward to achieve tension-free fascial closure (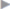 Fig. 4.21).
Fig. 4.21).
Fig. 4.18 Opening the sac and dissecting its contents. After reducing the contents, the sac is excised.
Fig. 4.19 The peritoneum/sac is then closed with a continuous absorbable suture. An epifascial suture line of 5 cm is dissected in all directions.
Measurement of the Mesh Site and Mesh Placement and Fixation
The mesh should overlap the fascial suture by 5 cm in all directions. After measuring, an appropriate mesh is cut to size and placed over the fascial suture. Since a corresponding mesh thrust bearing is lacking, mesh fixation is highly important. This can be done with nonabsorbable interrupted or continuous sutures (e.g., with Premilene/Prolene 2/0). The stitches should be less than 1 cm apart (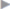 Fig. 4.22).
Fig. 4.22).
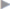 Fig. 4.23 shows the epifascial mesh position after swing door incision.
Fig. 4.23 shows the epifascial mesh position after swing door incision.
Drainage, Reattachment of the Umbilicus if Necessary, Skin Closure
The extended epifascial dissection produces a large wound cavity, which often leads to wound seromas. Subcutaneous vacuum drains are placed on the mesh.
The umbilicus should be reattached to the fascia through the mesh. This can be achieved with an absorbable suture (e.g., PDS 2/0). The operation concludes with approximating subcutaneous sutures and skin closure.
Relevant Anatomy, Dangers, and Tricks
• The blood supply of the subcutaneous tissue and skin can be injured during dissection of the epifascial mesh site, leading to necrosis of the wound edges. Especially after previous pararectal incisions, the blood supply of the skin bridge between the two incisions may be impaired.
• Mesh fixation is more difficult when the fascial defects extend to adjacent bony structures. Fixation that includes periosteum should be avoided because of the possibility of postoperative pain.
• Adequate soft tissue cover of the mesh must always be ensured to avoid possible mesh infection. Early VAC therapy may be necessary with concomitant conditioning of the overlying soft tissues.
Management of Special Complications
• Transmural bowel injury: bowel suture and generous irrigation.
• Postoperative hematoma: surgical evacuation of the hematoma.
• Mesh infection: antibiotic therapy, early VAC therapy, mesh explantation if necessary.
• Wound seroma: observation, sterile aspiration if extensive. Surgical management, possibly with VAC therapy, of persistent loculated seromas with corresponding symptoms is reasonable after 3 to 6 months.
Postoperative Care
 Medical care. The vacuum drains are removed when the discharge is less than 10 to 20 mL/d. The patient should be provided with an information leaflet on gradual resumption of physical efforts.
Medical care. The vacuum drains are removed when the discharge is less than 10 to 20 mL/d. The patient should be provided with an information leaflet on gradual resumption of physical efforts.
 Diet. This depends on the extent of adhesiolysis and postoperative resumption of bowel activity. Liquid diet is usually well tolerated on the first postoperative day.
Diet. This depends on the extent of adhesiolysis and postoperative resumption of bowel activity. Liquid diet is usually well tolerated on the first postoperative day.
 Bowels. If resumption of bowel evacuation is delayed an enema should be given from postoperative day 3.
Bowels. If resumption of bowel evacuation is delayed an enema should be given from postoperative day 3.
 Mobilization. Mobilization is possible immediately on arrival in the ward with nursing support.
Mobilization. Mobilization is possible immediately on arrival in the ward with nursing support.
 Physical therapy. Physical therapy depends on the extent of the repair and pre-existing comorbidity, especially respiratory therapy.
Physical therapy. Physical therapy depends on the extent of the repair and pre-existing comorbidity, especially respiratory therapy.
 Incapacity for work. Two to three weeks.
Incapacity for work. Two to three weeks.
4.2.3 Open Intraperitoneal Onlay Mesh Technique
Introduction
In the open intraperitoneal onlay mesh (IPOM) repair, the mesh is placed intra-abdominally on the peritoneum, allowing technically simple and tension-free repair of the fascial defect. As in the open onlay and retromuscular mesh repair procedures, an intra-operative decision can be made regarding augmentation or defect bridging depending on fascial tension.
While the fascia is closed over the mesh in the case of augmentation, bridging is used to repair an abdominal wall defect of variable size. The IPOM procedure can be performed both laparoscopically and via open surgery. The procedure shown here is the open method.
Especially in patients with a high-risk profile, open IPOM repair to correct an incisional hernia is a simple and safe operation for the multimorbid patient. Postoperative transfer to the intensive care unit, sometimes with a need for prolonged ventilation, can often be avoided as this technique offers a tension-free procedure with a short operating time.41
The most serious complications after ventral hernia repair with intraperitoneal mesh are fistulas and adhesions with their sequelae.56 These complications have been observed especially when heavyweight and small-pored mesh has been used, and they have also been described with extraperitoneal mesh implantation.25,102
In the past few years, further modifications of mesh for intraperitoneal placement for incisional hernia repair have been introduced, which appear to have significant advantages compared with expanded polytetrafluoroethylene (e-PTFE) mesh. These new types of meshes prevent intestinal adhesions because of specially altered surface properties or because they use new antiadhesive polymers.
Apart from their increased antiadhesive properties, the new-generation meshes for IPOM meet all the criteria of modern lightweight and large-pored mesh types. The flexibility of the “newer” IPOM meshes compared with e-PTFE mesh is of great importance when repairing large incisional hernia defects. It must be stressed, however, that the ideal mesh for intraperitoneal placement has not yet been found, and many authors reject intraperitoneal mesh placement. In addition, this type of mesh is much more expensive than the mesh used for extraperitoneal augmentation.
Open IPOM repair developed from the inlay technique. The latter had a high recurrence rate of over 40% and is no longer used nowadays to treat incisional hernia.1 A sufficiently wide contact area between mesh and tissue is important to enable broad fibrocollagenous healing.
Operation Techniques
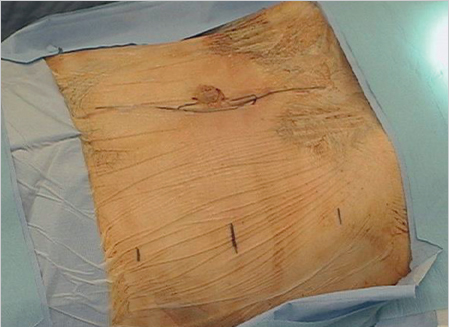
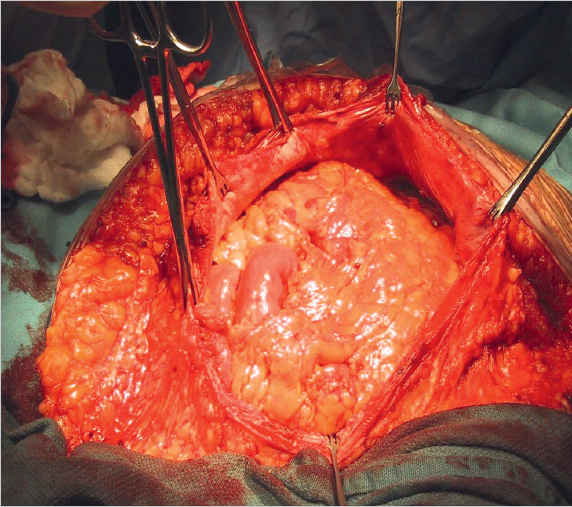
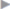 Fig. 4.24 shows a large incisional hernia.
Fig. 4.24 shows a large incisional hernia.
Preparation and Access
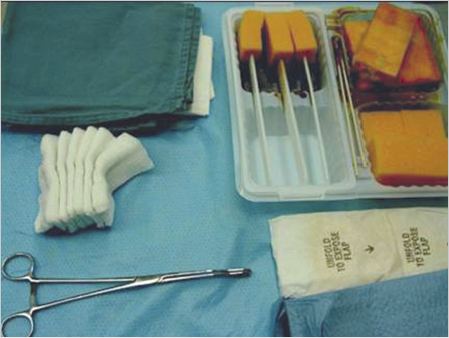
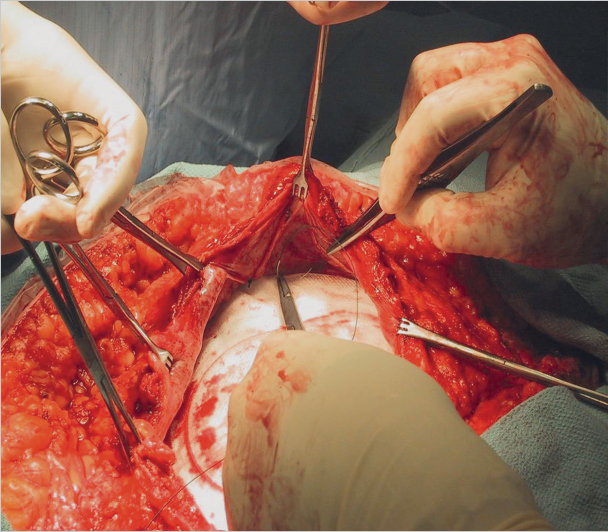
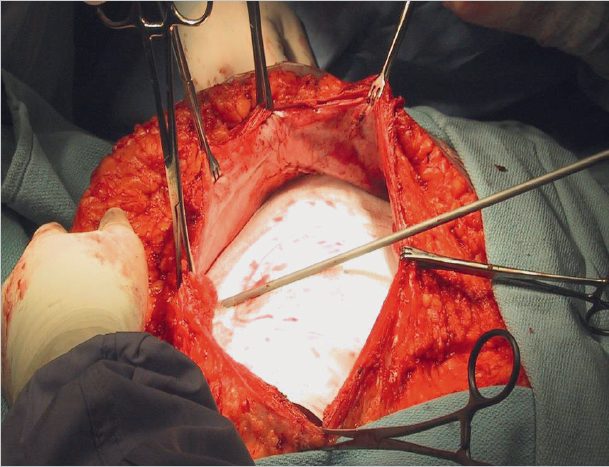
The operation area is prepared extensively and calculated antibiotic prophylaxis is given.28 Good skin disinfection, if necessary using adhesive drapes, is important to avoid later mesh infection (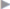 Fig. 4.25 and
Fig. 4.25 and 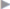 Fig. 4.26). During implantation, the mesh should not come in contact with the skin to avoid contamination.
Fig. 4.26). During implantation, the mesh should not come in contact with the skin to avoid contamination.
Operation Steps
The entire skin scar is excised and dissection continues through the subcutaneous tissue as far as the hernial sac. The fascial edges are exposed ( Fig. 4.3). The sac is opened and its contents are reduced. Complete adhesiolysis of the small and large intestine is performed only when the adhesions are extensive and there is a history of chronic abdominal pain or symptoms of bowel obstruction. The sac is resected.
Fig. 4.3). The sac is opened and its contents are reduced. Complete adhesiolysis of the small and large intestine is performed only when the adhesions are extensive and there is a history of chronic abdominal pain or symptoms of bowel obstruction. The sac is resected.
Dissection of the Mesh Site
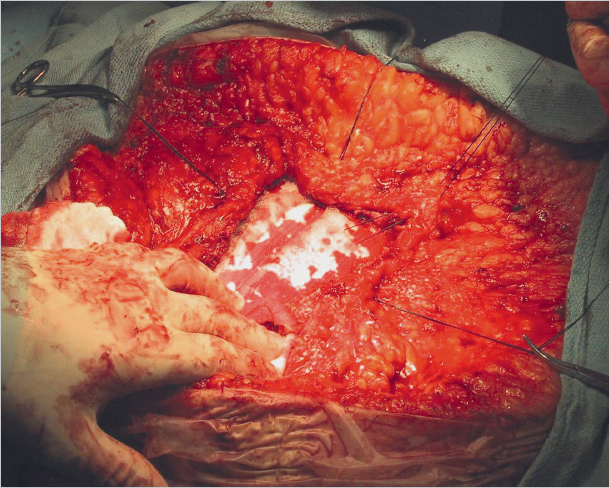
With incisional hernias in the upper abdomen, the falciform ligament and round ligament of the liver are divided at the level of the fascia. When the hernia is in the lower abdomen, the prevesical space is exposed after division of the medial folds to allow mesh placement behind the symphysis. The required mesh overlap of at least 3 to 5 cm69 in craniocaudal direction is possible only in this way ( Fig. 4.27,
Fig. 4.27,  Fig. 4.28, and
Fig. 4.28, and  Fig. 4.29).
Fig. 4.29).
Mobilization of the left or right colon may be necessary to achieve an adequate overlap laterally.
Fig. 4.25 Intraoperative use of adhesive drapes to reduce the rate of impaired wound healing and mesh infection.
Fig. 4.26 Careful skin disinfection to reduce the rate of impaired wound healing and mesh infection.
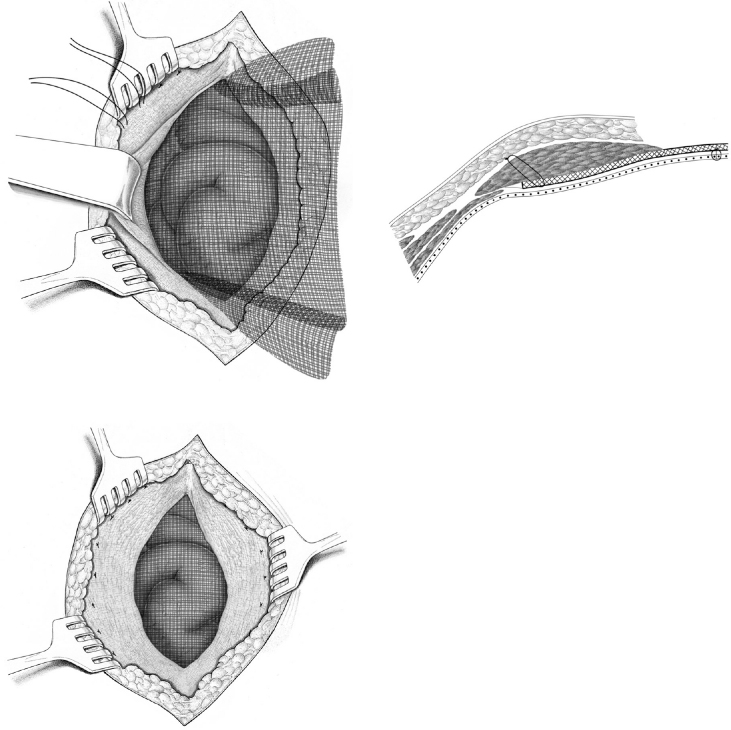
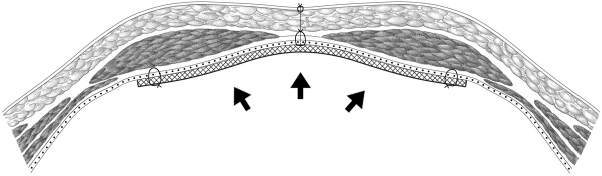
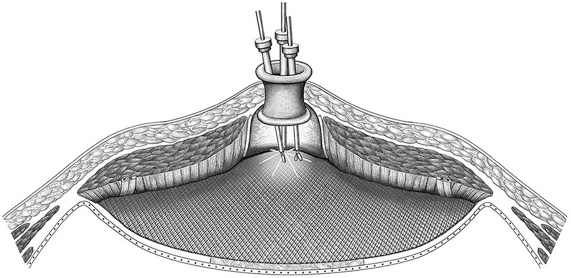
Fig. 4.27 Open intraperitoneal onlay mesh technique with fascial closure (augmentation). The mesh overlaps by at least 3 to 5 cm in all directions. The mesh is pressed against the abdominal wall by intra-abdominal pressure. This promotes ingrowth of the mesh into the peritoneum/abdominal wall.
Mesh Selection
Following preparation, the mesh size is determined by measuring the hernial orifice in two places with a flexible tape measure. The size of the defect is estimated roughly beforehand to have suitable mesh sizes available (see 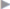 Fig. 4.24). The mesh must project beyond the hernial orifice by at least 3 cm in all directions (see
Fig. 4.24). The mesh must project beyond the hernial orifice by at least 3 cm in all directions (see 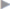 Fig. 4.27 and
Fig. 4.27 and  Fig. 4.28). Suitable meshes range from ePTFE (expanded polytetrafluoroethylene), coated meshes, combined meshes (e.g., polypropylene and ePTFE) to inert materials such as polyvinylidene fluoride and biological meshes.
Fig. 4.28). Suitable meshes range from ePTFE (expanded polytetrafluoroethylene), coated meshes, combined meshes (e.g., polypropylene and ePTFE) to inert materials such as polyvinylidene fluoride and biological meshes.
It is important for all mesh used intraperitoneally to minimize adhesions to the bowel as far as possible and, on the other hand, to ensure good incorporation in the abdominal wall. In abdominal wall bridging, the mesh must be stable enough to prevent a bump or pseudohernia.
Mesh Placement and Fixation
The mesh is placed intraperitoneally without tension and with the required overlap in all directions (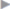 Fig. 4.30). The mesh should be separated from the bowel by the greater omentum to diminish the development of adhesions to the bowel. Compared with all other procedures, mesh placement is very easy in a relaxed patient.
Fig. 4.30). The mesh should be separated from the bowel by the greater omentum to diminish the development of adhesions to the bowel. Compared with all other procedures, mesh placement is very easy in a relaxed patient.
Fig. 4.29 Preparation of the abdominal cavity with resection of the sac, adhesiolysis, and adequate mobilization of the abdominal wall in all directions, if necessary with division of the round ligament of the liver and division of the median and medial umbilical folds when dissecting the prevesical space.
Fig. 4.30 Intraperitoneal mesh placement and fixation with interrupted sutures to the peritoneum and posterior rectus fascia at intervals of at least 3 cm.
The fixing sutures should include not only the peritoneum but also the posterior rectus fascia. This is the only way to ensure adequate mesh fixation until fibrocollagenous incorporation of the mesh takes place (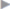 Fig. 4.30). To facilitate this, the sutures can be prepared in the mesh at intervals of roughly 3 cm before intraperitoneal placement.
Fig. 4.30). To facilitate this, the sutures can be prepared in the mesh at intervals of roughly 3 cm before intraperitoneal placement.
Use of absorbable or nonabsorbable tacks can shorten the operation time for open mesh fixation (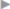 Fig. 4.31). As in the laparoscopic procedure, mesh fixation uses the “double-crown technique,” i.e., at least two fixing sutures are required (
Fig. 4.31). As in the laparoscopic procedure, mesh fixation uses the “double-crown technique,” i.e., at least two fixing sutures are required (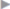 Fig. 4.32).16
Fig. 4.32).16
Augmentation or Bridging
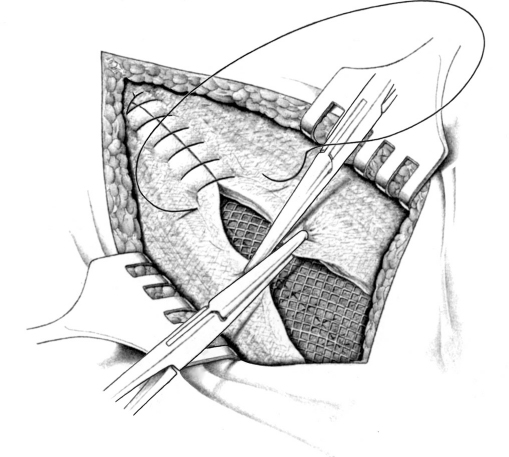
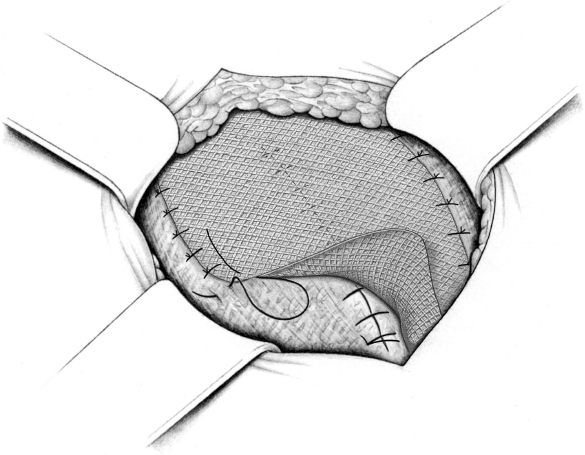
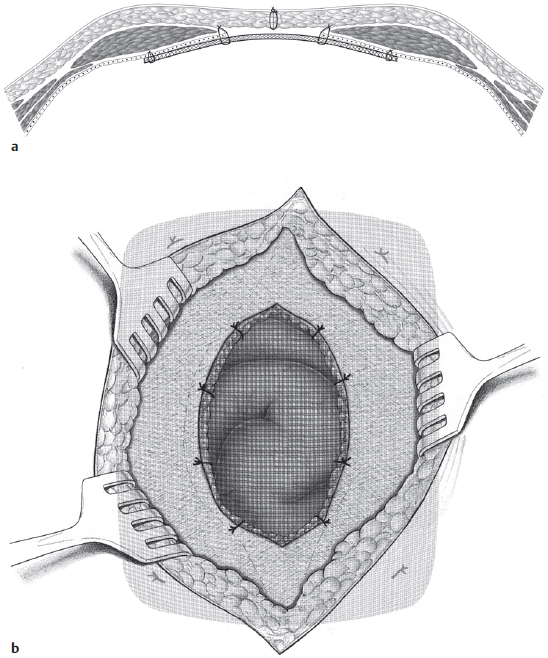
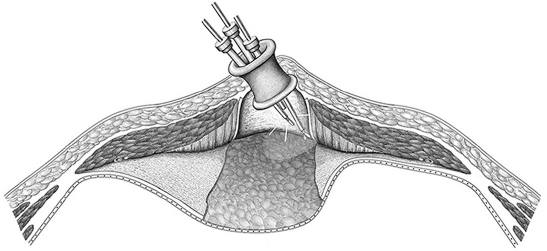
Fascial closure over the mesh may be omitted to reduce tension and the risk of an abdominal compartment syndrome. In this case, the edge of the fascia or hernial sac should then be fixed to the mesh with continuous or interrupted nonabsorbable sutures (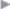 Fig. 4.32). This “topstitched seam” prevents further retraction of the fascial border and reduces the exposed mesh surface.
Fig. 4.32). This “topstitched seam” prevents further retraction of the fascial border and reduces the exposed mesh surface.
According to the literature, laparoscopic incisional hernia repair requires closure of the orifice.18 This can also be achieved in the open IPOM repair, e.g., by combining intraoperative mesh positioning with swing-door incisions105 or component separation.76 However, this requires more extensive dissection. The advantages have not yet been demonstrated in the literature.
Abdominal Wall Closure
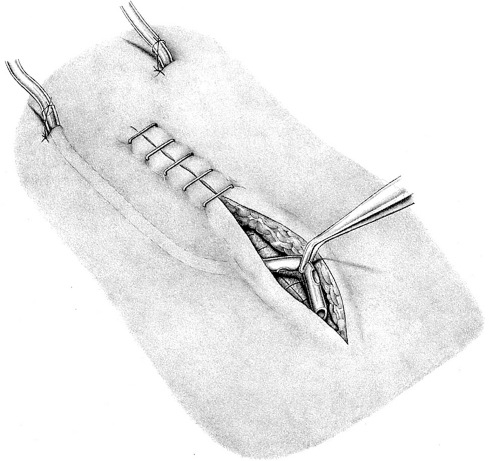
Finally, the skin and subcutaneous tissue are closed over the mesh. At the same time, the scar can be revised and overstretched, followed by the excision of the excess skin, if necessary (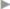 Fig. 4.33).
Fig. 4.33).
Fig. 4.32 In abdominal wall replacement, the hernia edges are fixed to the mesh with interrupted sutures. A nonabsorbable suture is generally used. Mesh fixation therefore uses the “double-crown technique.”
Placement of drains is controversial.22 In over 60% of cases of open incisional hernia repair, drains are inserted with the aim of diverting wound secretions to reduce complications such as seroma, hematoma, or infection. A recent Cochrane database analysis showed that drains did not significantly reduce the complication rate after open incisional hernia repair and there was no difference whether or not a drain was used.34 The author tries to avoid use of drains as these are a potential source of infection.
Postoperative Care
An abdominal bandage is routinely worn for at least10 days. Adequate analgesia is required.
Advantages and Disadvantages
The advantages of open IPOM repair are obvious: there is no learning curve, as with laparoscopic procedures. “See one, do one, teach one” applies to open IPOM incisional hernia repair more than to any other technique. This also explains the short operation times.5 Intraperitoneal mesh placement is simple and shows good results in the literature41 (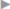 Fig. 4.34).
Fig. 4.34).
The time-consuming division of adhesions during laparoscopic hernia repair, with the serious complications reported in the literature, such as thermal bowel injury and unrecognized iatrogenic enterotomy, is not mentioned in the literature in association with the open technique.14,55 Enterotomy is an important complication of laparoscopic incisional hernia repair with mortality of up to 7.3%.54
The possibility of revising the old scar and excising excess skin and subcutaneous tissue is a particular advantage of the open methods (see 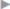 Fig. 4.33). The postoperative cosmetic result from the patient’s point of view is a clear advantage compared with laparoscopic IPOM repair.
Fig. 4.33). The postoperative cosmetic result from the patient’s point of view is a clear advantage compared with laparoscopic IPOM repair.
The disadvantage of open IPOM repair is the supposedly higher wound infection rate compared with the laparoscopic technique.21,31,32,87 Compared with other open methods such as the sublay technique or the Ramirez repair, access trauma is much less with the open IPOM technique. The infection risk therefore falls; retrospective studies have shown a low infection rate to date with the open IPOM method (between 2 and 8% after follow-up of up to 52 months). There are still no randomized studies.2,9,21,41
Chronic pain after open incisional hernia operations is described 10–20% of cases.64,69 The suggested etiology includes:
• Fixation.
• Foreign material.
• Mesh infections.
• Adhesions between the bowel and the mesh.
• Mesh positioning.
Summary
Open IPOM repair is an important addition to the range of surgical options for incisional hernia treatment. It should be a part of the hernia surgeon’s armory. The classical indication is repair of laparostomy and large incisional hernias in which the abdominal muscles have retracted so far that approximation of the midline is no longer possible even using component separation techniques.9
Fig. 4.33 With the intraperitoneal onlay mesh technique, plastic reconstruction of the scar and excess soft tissue can be carried out. This provides a postoperative result that is very satisfactory for the patient.
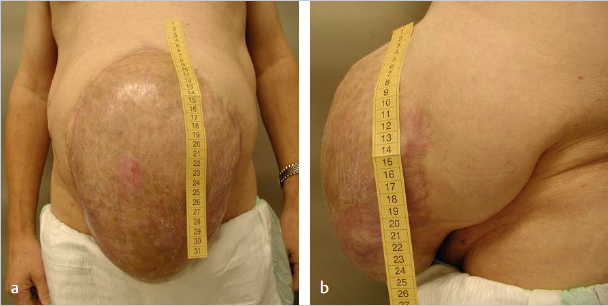
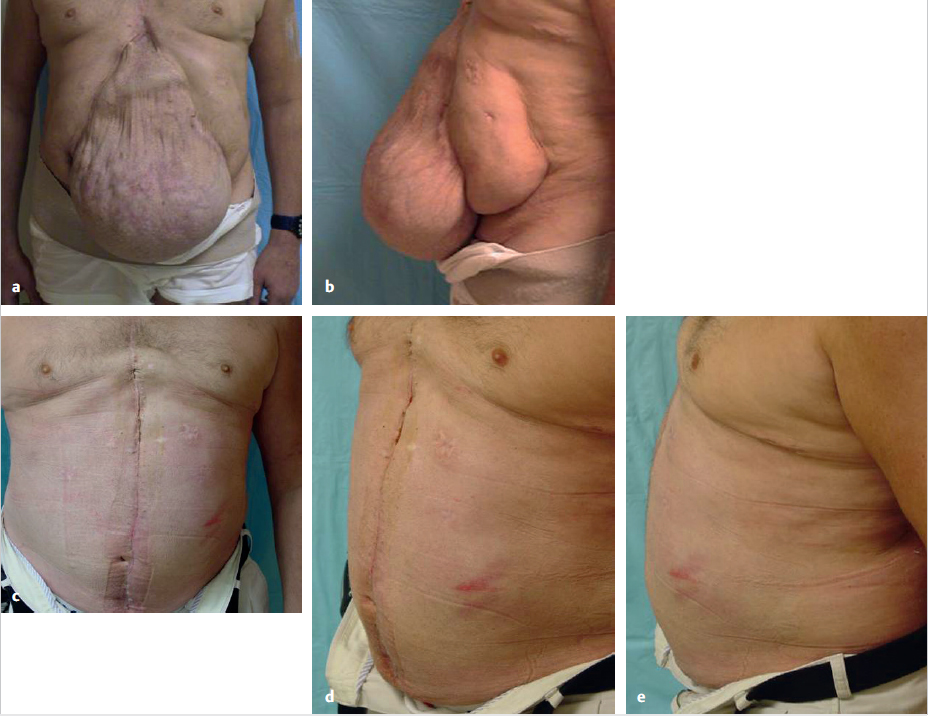
Fig. 4.34 Reconstruction of a giant incisional hernia.
a Preoperative anterior view, previous laparostomy with split skin graft.
b Preoperative lateral view.
c Postoperative anterior view after reconstruction with the open intraperitoneal onlay mesh technique.
d Postoperative oblique view.
e Postoperative lateral view.
4.3 Laparoscopic Repair of Incisional Hernias
4.3.1 General Principles
Repair of incisional hernia basically consists of implantation of a nonabsorbable mesh to augment the abdominal wall. In the open procedures, mesh can be placed on the external oblique aponeurosis (onlay), behind the rectus muscles (sublay), and intraperitoneally (IPOM). Intraperitoneal onlay mesh repair can be performed laparoscopically and was first described in 1993.53
In essence, following complete division of adhesions to the anterior abdominal wall, the hernial orifice is not closed but is covered with a broadly overlapping nonabsorbable mesh licensed for intraperitoneal use. The crucial differences from the conventional technique are as follows:
• The original laparotomy scar is not touched.
• The layers of the abdominal wall are not separated.
• There is no additional tension, as the hernial orifice is not closed.
• Wide overlapping is possible in nearly every hernia location.
A reduced rate of wound complications can be expected after laparoscopic procedures because there is less trauma to the abdominal wall. This has been confirmed in many studies and meta-analyses.7,14,72 Open surgery of incisional hernias after transverse laparotomy by means of sublay augmentation holds the danger of denervation of the rectus muscles in the affected segments, as dissection must proceed beyond the lateral rectus sheath. Intraperitoneal mesh repair can always avoid this “ground disturbance.”
Indications
Clear indications for a laparoscopic procedure are apparent from a comparison of the conventional and laparoscopic approaches:
• Patients with a high risk of infection,12 for instance, after deep wound infections following the index operation, obesity, or comorbidity or comedication that causes an additional risk of infection.
• Incisional hernia after transverse laparotomy.
• Subxiphoid and suprapubic hernias, which are often poorly accessible for anatomical reconstruction because of their proximity to the bony attachments of the abdominal wall.
• Recurrent hernias after conventional and especially retromuscular mesh augmentation.
Contraindications
Several previous conventional operations are not a contraindication to a laparoscopic procedure, as it is not possible to predict the extent of the adhesions.
Clear contraindications are as follows:
• Impossibility of achieving an adequate overlap of at least 5 cm.
• Portal hypertension presents a particular problem for laparoscopic division of adhesions and must be regarded as a contraindication.
• Abdominal wall paresis, specifically after flank access, cannot be permanently stabilized laparoscopically.62
• When access to the abdominal cavity is not possible even at minilaparotomy, this requires immediate conversion.
• In very rare cases, laparoscopic adhesiolysis is not possible. However, this situation also presents a particular challenge in open surgery.
Operation Techniques
Both open and laparoscopic incisional hernia repairs are usually performed with single-shot antibiotic prophylaxis. A transurethral catheter should be placed when dissection in the prevesical space is necessary, that is, for lower abdominal hernias and after primary access that extends far below the umbilicus. Orthograde bowel preparation is not necessary and an enema on the morning of the operation is sufficient.
Patient, Surgeon, and Video Tower Positioning
Patients with hernias after midline or transverse operations should be in supine position on a vacuum mattress with both arms by their sides. The mattress can be elevated for transverse approaches extending far into the flank. The arm on the elevated side can then be moved outward.
The skin should be disinfected and draped as far laterally as possible. Abducting the patient’s legs so the surgeon can stand between them has never proved necessary or even advantageous in our experience. The video tower is naturally opposite the cameraman and surgeon. The scrub nurse can stand either beside the video tower or beside the surgeon.
Access
Minilaparotomy generally provides the safest access to the abdominal cavity. The abdominal quadrant in which the least adhesions are suspected should always be chosen. This is the right upper abdomen after left-sided colon resection (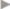 Fig. 4.35) and the left upper quadrant after right-sided colon resection (
Fig. 4.35) and the left upper quadrant after right-sided colon resection (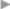 Fig. 4.36).
Fig. 4.36).
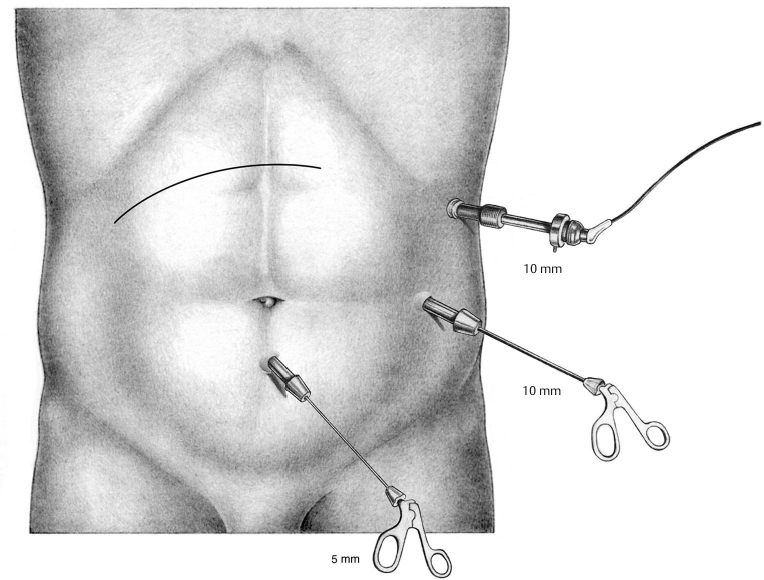
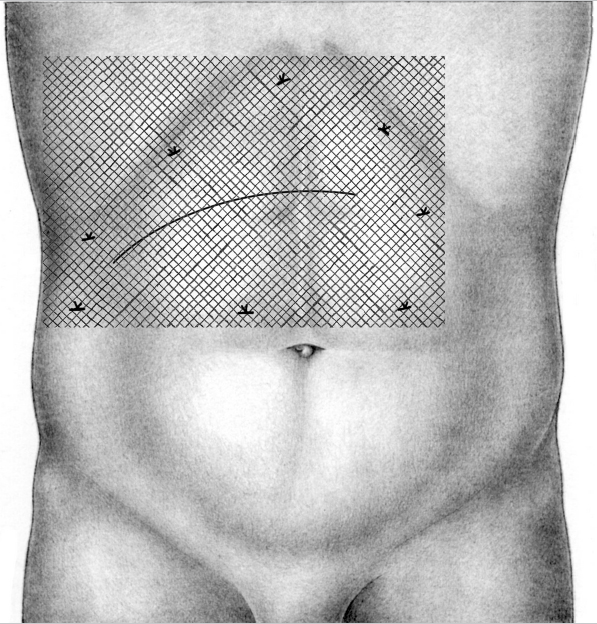
After upper abdominal operations through a transverse incision, few adhesions are to be expected in the right or left lower abdomen. Trocar placement is shown in 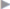 Fig. 4.37. After aortic replacement through both a transverse and midline approach, there are always fewer adhesions in the right half of the abdomen, so this should be used for access.
Fig. 4.37. After aortic replacement through both a transverse and midline approach, there are always fewer adhesions in the right half of the abdomen, so this should be used for access.
It is very helpful to mark the hernia and the planned mesh position before creating the pneumoperitoneum, bearing in mind that the entire original scar must remain visible. This allows the appropriate mesh size to be established at the start of the operation.
Trocar Placement
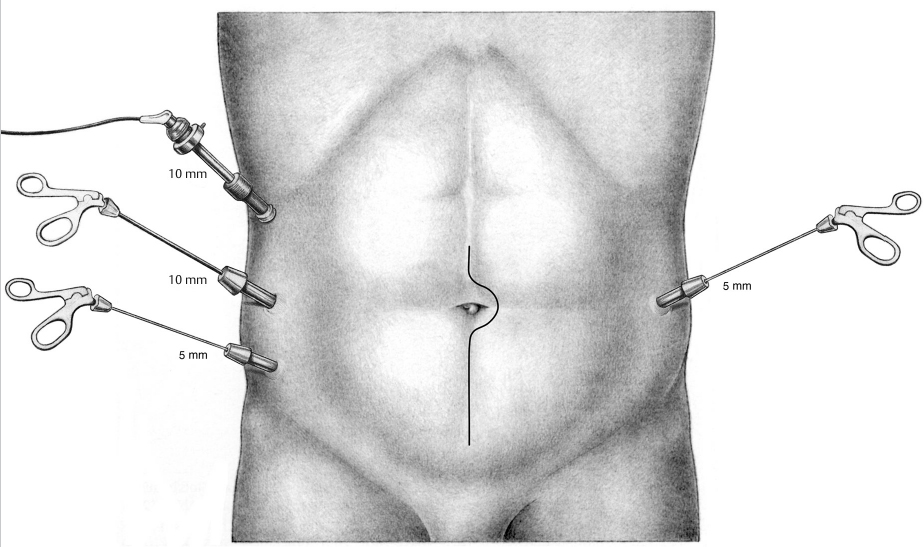
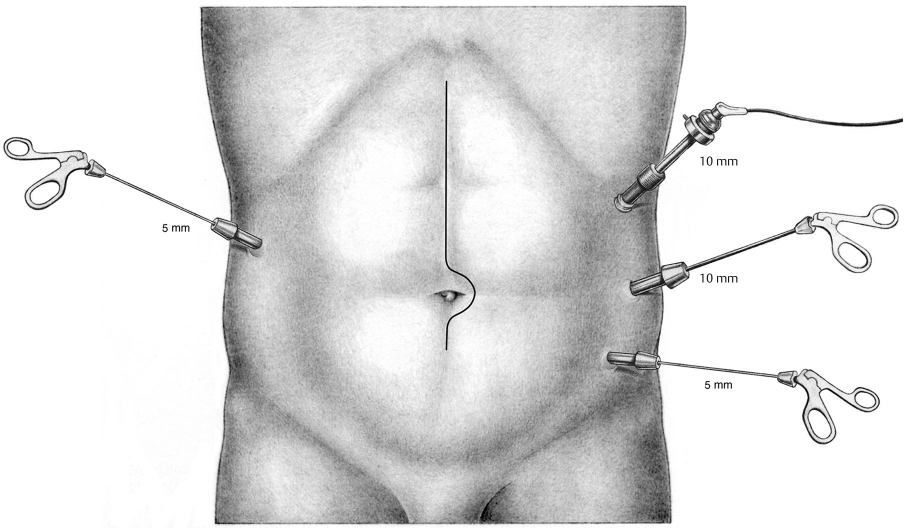
An angled optic, e.g., 30°, naturally provides an ideal viewing angle for the abdominal wall. For incisional hernias after midline incisions three trocars are placed along the anterior axillary line: subcostally, at the level of the umbilicus and in the lower abdomen. An additional trocar is inserted on the contralateral anterior axillary line at umbilical level. For incisional hernias after transverse incisions, the trocars are placed in a half-moon arrangement. Meshes up to 20 × 30 cm in size can usually be placed through a 10-mm trocar. A 12- or 13-mm trocar is recommended for larger meshes.
For a right-handed surgeon, dissection of the lower abdomen in the space of Retzius is easier from the right. Conversely, dissection from the left side is recommended in the upper abdomen.
Fig. 4.37 The right or left lower abdomen can usually be chosen for access after upper abdominal operations through a transverse incision.
Adhesiolysis
Adhesiolysis is the riskiest step in laparoscopic incisional hernia repair. Under pneumoperitoneum conditions, leakage of bowel content must not occur immediately following enterotomy; so, such an injury can easily be overlooked.
Caution
Superficial or transmural injuries of the bowel wall must be avoided. This is best achieved by exclusively sharp adhesiolysis. Energy sources such as monopolar or bipolar scissors or ultrasonic scalpels must be avoided. The same applies for instrumental traction on the bowel.
Dissection can be facilitated by external pressure on the abdominal wall with the nondominant hand. The entire anterior abdominal wall must be exposed. The round ligament of the liver and the falciform ligament must always be divided to ensure an adequate overlap. Dissection can continue as far as the left triangular ligament without endangering the hepatic veins.
After lower abdominal incisions, the prevesical space must be opened to ensure stable mesh fixation in the extraperitoneal space. Purely intraperitoneal mesh placement will always result in suprapubic recurrence.
Additional medial inguinal or femoral hernias can be covered with the mesh used for incisional hernia repair. Formal transabdominal preperitoneal mesh repair (TAPP) should be performed for additional lateral hernias. If there are very dense adhesions between the intestine and anterior abdominal wall, parts of the posterior rectus sheath can be left on the intestine. In the case of recurrent hernias after intraperitoneal mesh repair, separation of bowel loops from the mesh may not be possible in individual cases, depending on the material used. The mesh can then be mobilized from the abdominal wall and left on the bowel. Segments of bowel adherent in the hernial sac often become visible only on manual pressure from without. In these cases, instrumental traction should always be avoided.
Mesh Placement and Fixation
Because of the contact between foreign material and the intestines, simple polypropylene or polyester mesh must not be used. In these cases, massive adhesions and fistula formation would be likely.52 Alternatives approved for intraperitoneal use include ePTFE and coated polypropylene or polyester mesh. Polyvinylidene fluoride (PVDF) is currently the most modern material.
The ePTFE-based structures have the greatest tendency to shrinkage24 and must always be removed if infection occurs. Coated or pretreated polypropylene and polyester structures are inelastic and this limits their handling characteristics considerably. In addition, they sometimes induce substantial adhesions experimentally. Moreover, superimposing two or more meshes has not been studied to date.
Polyvinylidene difluoride (PVDF) structures are elastic and transparent, they can be overlapped without difficulty, and are highly resistant to infection due to low microbial adherence. There is hardly any tendency to shrinkage.46,49 A clinical study in 344 patients showed excellent tolerability in this respect also.7
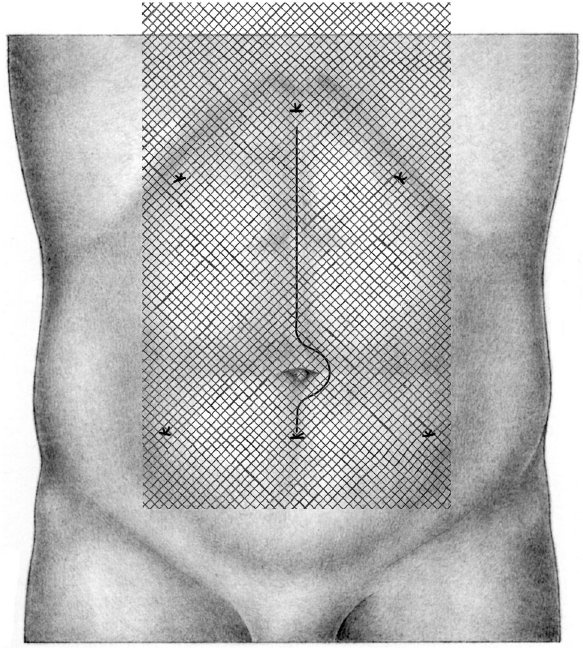
The entire original incision must be covered with an overlap of at least 5 cm in all directions. As mentioned above, the correct mesh size can be established prior to insufflation of the pneumoperitoneum. Four corner sutures are used. Additional cranial and caudal retaining sutures in the midline after midline incisions have been shown to be helpful. When overlapping toward the costal margin (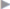 Fig. 4.38) or behind the symphysis (
Fig. 4.38) or behind the symphysis (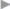 Fig. 4.39), the midline sutures should be placed 5 to 6 cm from the edge of the mesh to enable overlapping toward the diaphragm or behind the symphysis. In these cases, the placement of the corner sutures must be altered as required by the anatomy.
Fig. 4.39), the midline sutures should be placed 5 to 6 cm from the edge of the mesh to enable overlapping toward the diaphragm or behind the symphysis. In these cases, the placement of the corner sutures must be altered as required by the anatomy.
Because of the greater transverse curvature of the abdominal wall, eight marking sutures are recommended, as shown in 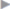 Fig. 4.40. The suture material is not critical; absorbable or nonabsorbable sutures can be used, as the surgeon prefers. After introducing the mesh, which should be folded and not rolled, the midline sutures are passed transfascially first, followed by the corner sutures. The mesh is thus optimally positioned.
Fig. 4.40. The suture material is not critical; absorbable or nonabsorbable sutures can be used, as the surgeon prefers. After introducing the mesh, which should be folded and not rolled, the midline sutures are passed transfascially first, followed by the corner sutures. The mesh is thus optimally positioned.
Final fixation is achieved with tacks that again can be absorbable or nonabsorbable. We place tacks every 4 to 5 cm but the sutures are always tied. The literature recommends the use of nonabsorbable material for sutures and tacks15 in conjunction with ePTFE-based structures but there are no definitive experimental or clinical results to substantiate this recommendation.
The bladder does not have to be fixed to the anterior abdominal wall with suture or tacks as it resumes its position readily after release of the pneumoperitoneum.
Postoperative Care
Drains are not required. Unrestricted diet is resumed depending on bowel function. However, stubborn postoperative ileus can occur. Administration of a mild osmotic laxative is recommended, starting on the evening of the operation.
Postoperative pain in the initial days is a major problem and is much greater than expected after a laparoscopic procedure. Intensive and consistent analgesia is therefore required, which may even include use of an epidural catheter.
Unanswered Questions
Two questions, in particular, remain unanswered today. Firstly, it is not clear whether the mesh should be fixed with tacks and sutures or with only one of these two methods. The idea that corner sutures lead to more pain has not been confirmed in recent studies. Recurrences also do not appear to be influenced by the mode of fixation.
Another point of contention is whether the results of laparoscopic repair can be improved by closure of the fascial defect. Various studies have shown that the hernia can be closed laparoscopically and that the recurrence rate is low and sometimes extremely low.70 However, primary and secondary ventral hernias were analyzed jointly, which is no longer permissible today.50,95 A recent study that retrospectively compared the standard procedure with repair with fascial suture showed better results with regard to recurrence rate and patient satisfaction after the gap in the fascia was closed.20 This group, however, did not distinguish between primary and secondary ventral hernias. In addition, the results of the standard procedure are unusually poor as regards both aspects. Thus, the literature is still unable to answer this question.
There are theoretical considerations, however, that render fascial closure doubtful. Compared with retromuscular mesh placement, intraperitoneal mesh placement is very much weaker. Usually, these meshes can be separated bluntly from the anterior abdominal wall. In addition, there is considerable tension on the fascial suture, which can hardly be absorbed by an intraperitoneal mesh compared with retromuscular placement. There is also a danger that smaller meshes are used so that a hernia will recur with the further fascial dehiscence that can be expected in the short term. Until the permanence of anatomical reconstruction by laparoscopic fascial suture is confirmed, surgeons should refrain from this procedure.
Anatomical reconstruction certainly makes sense for very large defects, such as following a subcutaneous burst abdomen. In our hands, however, this can best be achieved with component separation and subfascial mesh repair. To date, no studies have investigated the size of fascial defect above which such reconstruction is useful because of the improvement in function.
Summary
The laparoscopic approach represents an important enhancement of incisional hernia repair options. Accurate knowledge of the anatomical and pathophysiological basis of the hernia and of conventional treatment methods, including component separation is essential as laparoscopic management is not possible in every case. Moreover, laparoscopic incisional hernia repair makes particular demands on the surgeon’s laparoscopic experience, and low case numbers may make it impossible to train surgeons adequately; it may even be necessary to forego use of the technique when the case numbers are too low. In these cases, knowledge of the method and its advantages and disadvantages is particularly important to provide the patient nevertheless with the chance of optimal treatment.
4.3.2 Endoscopic Totally Extraperitoneal Transhernial Sublay Ventral Hernia Repair using the Single-Port Technique
The Rives and Stoppa sublay mesh herniorrhaphy80 is currently the most frequently used procedure in ventral hernia surgery, apart from laparoscopic intraperitoneal mesh repair (lap. IPOM). The advantages of the Rives-Stoppa operation are as follows:
• Extraperitoneal mesh position without the need for extensive mesh fixation with tacks, staples, or transmural sutures.
• Hernia closure over the mesh is often possible.
• Standard plastic mesh and self-adhesive mesh can be used.
• Abdominal cavity remains intact in an ideal case.
The disadvantages are higher infection rates described in the literature and greater access trauma. To date, there have been only three studies in the literature of endoscopic totally extraperitoneal sublay mesh implantation for ventral hernias.48,60,100 The use of single ports has not yet been reported. In the endoscopic totally extraperitoneal sublay ventral hernia repair using the single-port technique developed by our working group, transhernial extraperitoneal mesh implantation is performed minimally invasively. The procedure combines the advantages of the Rives-Stoppa operation and the laparoscopic IPOM technique
We have so far used the transhernial single-port ventral TEP procedure in 24 patients with small and medium-sized ventral and incisional hernias: the average defect size was 17 cm2, the average mesh size 292 cm2, and minimum mesh sublay 5 cm. In 12 cases, the abdominal cavity was not opened. No complications occurred apart from two retromuscular hematomas, which were treated conservatively. With a follow-up of 8 months (2–15 months), no recurrences and no chronic pain have occurred to date.
The high cost is a disadvantage, approximately 300 Euros for the single port. We have not yet treated lateral incisional hernias with this technique.
Indications
Small- and medium-sized ventral and incisional hernias (EHS classification W1 and W2).
Relative Contraindications
Lateral incisional hernia. Incisional hernia after transverse laparotomy (no experience to date).
Contraindications
Absolute general inoperability or absence of consent.
Alternative Procedures
• Endoscopic totally extraperitoneal transhernial sublay mesh repair of the abdominal wall with gasless endoscopy.
• Endoscopic totally extraperitoneal transhernial sublay mesh repair of the abdominal wall with standard endoscopy using the three-trocar technique.
• Rives-Stoppa open sublay mesh hernia repair.
• Laparoscopic IPOM repair.
Operation Preparation
• Preoperative diagnostics: standard preparation, ultrasound of the abdomen and abdominal wall.
• Antibiotic prophylaxis, e.g., cefazolin 2 g i.v. 30 minutes preoperatively.
• Medical thrombosis prophylaxis always given, preferably with low-molecular-weight heparin.
Special Risks, Informed Consent
• Bowel and bladder injury (< 1%).
• Nerve injury (< 1%).
• Bleeding (< 5%).
• Hernia recurrence (< 5%).
• Infection (< 1%).
• Chronic pain (0–10%).
Anesthesia
General anesthesia.
Position
Supine.
Access
Two skin incisions over the hernia up to 4 cm long. The exact skin incision can be determined preoperatively by ultrasound.
Relevant Anatomy, Dangers, and Tricks
Precise knowledge of the anatomy of the anterior abdominal wall is essential. Protect the nerves supplying the rectus muscle; these are readily visible endoscopically.
Check the peritoneum carefully for tears that must be repaired. If impaired gastrointestinal transit due to adhesions and/or bands is suspected clinically or on ultrasound, laparoscopy and laparoscopic adhesiolysis should be performed, with “mini-open” adhesiolysis if appropriate.
If gas-tight placement of the single port is not possible, gasless endoscopy should be performed with long narrow retractors.
When reusable metal single ports are used, monopolar electrocauterization should be employed with particular caution.
Very careful hemostasis is required.
The skin incision should be somewhat larger, especially during the first operations and in very obese patients; so, the hernial sac and orifice can be identified with certainty and to enable gas-tight introduction of the single port.
One to two additional 5-mm trocars may be introduced if necessary for insertion of very large meshes.
Management of Special Complications
Extensive hematoma: endoscopic hematoma evacuation.
Infection: endoscopic debridement, irrigation, and drainage initially; open procedure if necessary; mesh removal if necessary.
Postoperative Care
Brief hospitalization for treatment is usually possible, with clinical and ultrasound monitoring and monitoring of inflammatory parameters. Patients with cardiopulmonary comorbidity may require respiratory therapy.
We recommend an elastic abdominal bandage for 3 to 6 weeks depending on the hernia size. The evidence level for this measure is grade D.
Operation Techniques
Dissection of the Hernial Sac and Orifice
A 2- to 4-cm skin incision is made over the hernia. The sac is dissected and excised as necessary. The peritoneum is closed if it was opened.
Insertion of the Single Port
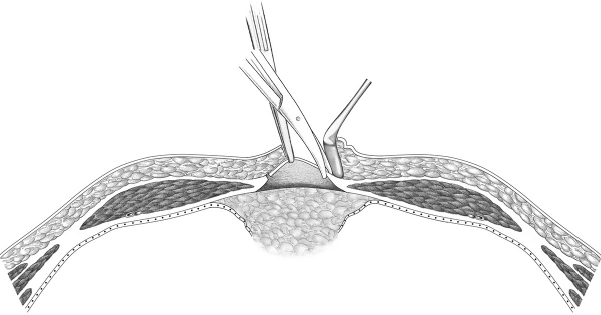
A small preperitoneal space with a radius of 1 to 2 cm is prepared by “mini-open” dissection. The single port is introduced into the hernial orifice. If necessary, this is tightened to allow gas-tight insertion of the single port with three 5-mm ports (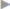 Fig. 4.41).
Fig. 4.41).
Endoscopic Dissection of the Preperitoneal Space
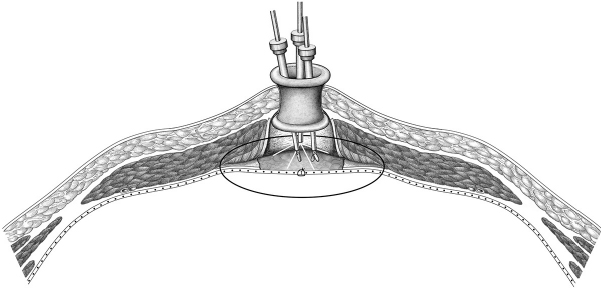
We use a long 5-mm, 30° optic. The procedure is performed with conventional straight 5-mm instruments. Preperitoneal dissection is initially in cranial and caudal direction posterior to the linea alba (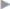 Fig. 4.42). A vertical incision is made in the posterior layer of the rectus sheath bilaterally 1 to 1.5 cm lateral to the medial border of the rectus muscle (
Fig. 4.42). A vertical incision is made in the posterior layer of the rectus sheath bilaterally 1 to 1.5 cm lateral to the medial border of the rectus muscle (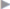 Fig. 4.43). Dissection then continues bilaterally anterior to the posterior layer of the rectus sheath, if necessary as far as the lateral border of the rectus compartment (
Fig. 4.43). Dissection then continues bilaterally anterior to the posterior layer of the rectus sheath, if necessary as far as the lateral border of the rectus compartment (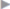 Fig. 4.44). The entire rectus compartment can thus be dissected endoscopically. The posterior layer of the rectus sheath remains open. The mesh is in preperitoneal position medially in the region of the linea alba and in front of the posterior layer of the rectus sheath laterally on both sides. The largest mesh we have implanted using this technique was 35 × 25 cm. Dissection is performed through 360° around the hernia defect. The laparoscopy tower is initially at the patient’s feet and is moved to the patient’s left and right side as needed. An alternative is to use several monitors.
Fig. 4.44). The entire rectus compartment can thus be dissected endoscopically. The posterior layer of the rectus sheath remains open. The mesh is in preperitoneal position medially in the region of the linea alba and in front of the posterior layer of the rectus sheath laterally on both sides. The largest mesh we have implanted using this technique was 35 × 25 cm. Dissection is performed through 360° around the hernia defect. The laparoscopy tower is initially at the patient’s feet and is moved to the patient’s left and right side as needed. An alternative is to use several monitors.
Mesh Insertion
After repeated skin disinfection and removal of the single port, the mesh is inserted transhernially using the double-roll technique, as far as possible without skin contact. It is first opened and spread out under digital control. The single port is reinserted and the mesh is placed in its final position endoscopically (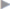 Fig. 4.45). The edge of the mesh can be fixed endoscopically with sutures or staples but this can be omitted if the mesh overlaps the hernia defect by at least 5 cm and the hernia is then closed with anatomical reconstruction of the linea alba. Alternatively, self-adhesive mesh can be used.
Fig. 4.45). The edge of the mesh can be fixed endoscopically with sutures or staples but this can be omitted if the mesh overlaps the hernia defect by at least 5 cm and the hernia is then closed with anatomical reconstruction of the linea alba. Alternatively, self-adhesive mesh can be used.
Fig. 4.42 Single port insertion and a 360° dissection of the preperitoneal space, initially in cranial and caudal direction posterior to the linea alba.
Fig. 4.43 Endoscopic vertical incision of the posterior layer of the rectus sheath bilaterally through the single port.
Fig. 4.44 The 360° dissection of the preperitoneal space laterally in front of the posterior layer of the rectus sheath bilaterally.
4.3.3 Laparoscopic Repair of Parastomal Hernias
Parastomal hernia is a very frequent complication after construction of a terminal colostomy or ileostomy. It was recently shown that the majority of patients with parastomal hernias have clinical symptoms that have a considerable impact on their daily life.63
It is generally accepted that nonabsorbable mesh is necessary to repair a parastomal hernia, which is regarded as a special form of incisional hernia. Nevertheless, the results of clinical studies are not exactly promising as there are significant wound complication rates as well as recurrence rates between 10 and 50%. However, the validity of most studies is diminished by the limited number of patients.37
Laparoscopic repair is increasingly promoted in the literature. There are three procedures:
• The keyhole technique.
• The Sugarbaker technique.
• The sandwich technique.
Keyhole Technique
The principle of this technique is based on a keyhole-shaped incision in a mesh, which is then passed around the stoma loop. Recent studies, however, have shown that recurrence rates between 30 and nearly 50% can be expected. Only one series of 72 patients showed a recurrence rate of only 3%. However, this patient population had extreme operation-related morbidity; so, this procedure should generally be avoided as the revision rate is 13% with mesh complications in 7%.104
In summary, the keyhole technique is today regarded in the literature as unpromising.37
Sugarbaker Technique
This technique was first described in 1985 as a conventional procedure.96 It is based on intraperitoneal mesh placement, placing the stoma loop between the mesh and the abdominal wall and lateralizing it by at least 5 cm. If necessary, the midline can be covered by a suitably larger mesh. This technique is ideal for a laparoscopic approach and ultimately corresponds to a simple incisional hernia repair.
The results in the literature are conflicting, with recurrence rates between 0 and 33%. A recent meta-analysis of nonrandomized studies favors this technique, however, as it is compared exclusively with the keyhole technique.37
A study conducted by us in 41 patients,6 who were treated laparoscopically by the Sugarbaker technique, yielded a recurrence rate of nearly 20%. All these patients had a lateral hernia, from which the recurrence ultimately arose. The Sugarbaker technique therefore is reserved for parastomal hernias where the fascial defect is located medially. This is often difficult to assess laparoscopically.
Tip
It must be pointed out that in the case of an additional simultanuous incisional hernia, the entire original access must always be covered with a wide overlap.
Sandwich Technique
After the Sugarbaker technique proved unsuccessful in our experience for laterally located hernias, a combination of keyhole and Sugarbaker technique was introduced, known as the sandwich technique. The background to this is the need to stabilize the lateral abdominal wall by the keyhole cut in the first mesh. Medial stabilization and broad lateral overlapping6,7 are achieved by a second mesh as in the Sugarbaker method.
Operation Techniques
As described for incisional hernia, the operation can be divided into individual steps.
Patient, Surgeon, and Video Tower Positioning
Patients are placed supine on a vacuum mattress with both arms by their sides if possible. If necessary, especially in the case of very obese patients, the arm on the side of the stoma can be abducted. Antibiotic prophylaxis is given routinely. A transurethral bladder catheter should be placed to facilitate later dissection of the prevesical space.
The video tower is on the side of the stoma, and the surgeon and cameraman stand on the opposite side. The scrub nurse can stand beside or opposite the surgeon.
After skin disinfection and sterile draping, the stoma is covered with a round sponge that is fixed with an adhesive film. The mesh with keyhole incision is then marked and the second Sugarbaker mesh is also marked on the abdominal wall. In this way, the mesh size can be established at the start of the operation.
Access and Trocar Placement
A minilaparotomy is performed in the anterior axillary line, usually subcostally, on the side opposite the stoma, and a trocar and the 30° optic are placed under vision. More trocars are introduced in the anterior axillary line at umbilical level and in the lower abdomen. A further subcostal trocar on the stoma side is usually helpful subsequently.
In patients who have had a colectomy with access not extending to the xiphoid, the primary minilaparotomy can also be subxiphoid. Naturally, if there is an intact quadrant in the upper abdomen, the Veress needle puncture is also possible. However, it is possibly always safer to perform minilaparotomy.
Adhesiolysis
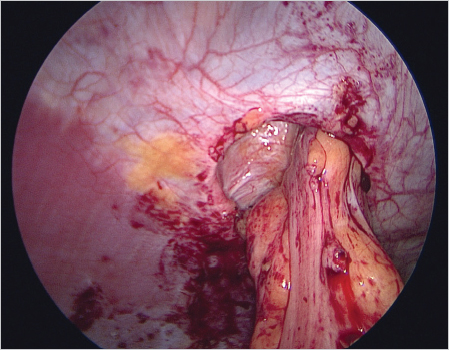
As with all secondary ventral hernias, adhesiolysis represents the most difficult and hazardous step of the operation. Energy sources should not be used during adhesiolysis. as their use drastically increases the rate of secondary enterotomy. As shown in 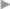 Fig. 4.46, the opening of a parastomal hernia is often not very large; so, mobilization of adherent loops of bowel in the hernial sac can be very difficult. Manual pressure from the exterior can facilitate dissection and reduction of prolapsed loops of bowel. Mobilization of the stoma loop without endangering the bowel is possible only in isolated cases. Overall, dissection of the stoma loop and mesocolic or mesenteric segment is the most difficult operation step. Direct traction on bowel loops must always be avoided.
Fig. 4.46, the opening of a parastomal hernia is often not very large; so, mobilization of adherent loops of bowel in the hernial sac can be very difficult. Manual pressure from the exterior can facilitate dissection and reduction of prolapsed loops of bowel. Mobilization of the stoma loop without endangering the bowel is possible only in isolated cases. Overall, dissection of the stoma loop and mesocolic or mesenteric segment is the most difficult operation step. Direct traction on bowel loops must always be avoided.
After complete adhesiolysis of the anterior abdominal wall and identification of the stoma loop, the round ligament of the liver (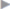 Fig. 4.47) must usually and the falciform ligament sometimes be dissected. The fat pad between the medial folds, including the latter, is also divided just below the umbilicus and dissected from the anterior abdominal wall to open the space of Retzius widely (
Fig. 4.47) must usually and the falciform ligament sometimes be dissected. The fat pad between the medial folds, including the latter, is also divided just below the umbilicus and dissected from the anterior abdominal wall to open the space of Retzius widely (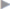 Fig. 4.48). These steps are essential to adequately stabilize the midline, which is usually dehiscent also.
Fig. 4.48). These steps are essential to adequately stabilize the midline, which is usually dehiscent also.
Mesh Placement and Fixation
Depending on the size of the parastomal fascial defect, a keyhole incision is made in the mesh; this mesh usually measures 15 × 15 cm. The central opening is roughly 1 cm. The mesh is passed around the stoma loop so that both leaves of the mesh lie medially (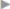 Fig. 4.49). These are joined with two nonabsorbable transfascial sutures and spiral tacks (
Fig. 4.49). These are joined with two nonabsorbable transfascial sutures and spiral tacks (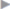 Fig. 4.50).
Fig. 4.50).
It is essential to close it with nonabsorbable material. As mentioned before, this mesh is indispensable for stabilizing the lateral abdominal wall. In exceptional cases, it is further fixed in two rows, an outer one at the edge of the mesh and an inner one around the stoma. The distance between the tacks can be 3 or 4 cm so that the inner row consists finally of four fixing points. Another mesh is placed in the Sugarbaker technique to cover the midline and lateralize the stoma loop by at least 5 cm between the two meshes (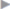 Fig. 4.51).
Fig. 4.51).