Hyperhidrosis
George Kontochristopoulos
Andreas Katsambas
Dimitrios Rigopoulos
BACKGROUND
Hyperhidrosis is a dermatologic condition characterized by excessive and uncontrolled sweating, more than required for regulation of body temperature.1,2 Prevalence estimates of hyperhidrosis in different studies range from 0.6% to 17%.3,4 A large epidemiological survey in the United States that included 150 000 households reported a prevalence of 2.8%.5 The disease most commonly occurs among people aged 25 to 64 years. Of these, approximately 1.4% present with axillary hyperhidrosis. Men and women are equally affected. In a recent study, using epidemiological data from UK and US health care databases, the lifetime prevalence of hyperhidrosis was calculated to be between 1% and 1.6%.6
PRESENTATION
Patients with hyperhidrosis present with a chief complaint of excessive sweating. The excessive perspiration is most often reported to occur in the underarms, palms, or soles and less commonly other anatomic sites. In some cases, patients may report that it occurs following certain triggers, such as eating, or postsurgically in circumstances involving nerve damage.
DIAGNOSIS
Clinical Diagnosis
The first step before the start of any treatment is to determine whether hyperhidrosis is primary or secondary and
to evaluate the severity of the disease and the impact on the quality of life. A thorough history and clinical examination are sufficient to differentiate primary from secondary hyperhidrosis. Diagnostic criteria of primary hyperhidrosis include no less than 6 months of excessive sweating, with 4 or more of the following features: primarily involving eccrine-dense (axillae/palms/soles/craniofacial) sites, bilateral and symmetric, absent nocturnally, episodes at least weekly, onset at age of 25 years or younger, positive family history, and impairment of daily activities.7
to evaluate the severity of the disease and the impact on the quality of life. A thorough history and clinical examination are sufficient to differentiate primary from secondary hyperhidrosis. Diagnostic criteria of primary hyperhidrosis include no less than 6 months of excessive sweating, with 4 or more of the following features: primarily involving eccrine-dense (axillae/palms/soles/craniofacial) sites, bilateral and symmetric, absent nocturnally, episodes at least weekly, onset at age of 25 years or younger, positive family history, and impairment of daily activities.7
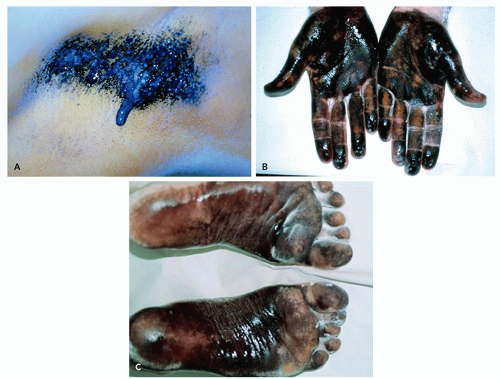
The Minor iodine-starch test is a very useful method for mapping the areas of excessive sweating before treatment (Figure 9.3.1), whereas gravimetric measurement is used only for research methods.
The Hyperhidrosis Disease Severity Scale is a quick and reliable diagnostic tool for measuring disease severity and impact on daily activities before and after treatment8 (Table 9.3.1). The quality of life can also be assessed by the Hyperhidrosis Impact Questionnaire and the Dermatology Life Quality Index.
Specific laboratory tests will assist in ruling out a range of diseases responsible for secondary hyperhidrosis.
Histopathology
On histology, eccrine glands appear morphologically and functionally normal. Biopsies of localized hyperhidrosis may reveal an abnormal number and/or distribution of normal eccrine glands. Examples of such conditions include eccrine nevus and eccrine angiomatous hamartoma.
Subtypes
According to etiology, hyperhidrosis is classified as primary or secondary and, according to its extent, as focal or generalized.7
Primary
Primary hyperhidrosis is typically focal and affects anatomic areas rich in eccrine sweat glands, most often the axillae, palms, soles, face, and scalp (Figure 9.3.2).
Secondary
Conversely, secondary hyperhidrosis is typically generalized, affecting the entire body, although it may affect select areas in cases of neurologic hyperhidrosis.
Causes of Secondary Hyperhidrosis
Paraneoplastic.
B-cell lymphoma
Pheochromocytoma
POEMS syndrome (polyneuropathy, organomegaly, endocrinopathy, monoclonal gammopathy, skin changes)
Glomus tumor
Carcinoid tumor
TABLE 9.3.1 Hyperhidrosis Disease Severity Scale | ||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| ||||||||||||||
Vascular Hamartomas.
Blue rubber bleb nevus syndrome
Eccrine angiomatous hamartoma
Eccrine nevus
Differential Diagnosis
Neurologic
Burning feet syndrome
Reflex sympathetic dystrophy
Riley-Day syndrome (familial dysautonomia)
Frey syndrome (auriculotemporal)
Syringomyelia
Harlequin syndrome
Parkinson disease
Acrodynia
Hines and Bannick syndrome
Endocrinologic
Medication Related
Antidepressants (eg, tricyclics, selective serotonin reuptake inhibitors)
β-Blockers (eg, propranolol)
Cholinergics (eg, physostigmine, donepezil, malathion, pilocarpine)
Opioid withdrawal
Nonsteroidal anti-inflammatory drugs
Glucose regulators (eg, glyburide, insulin)
Infectious
Febrile infections
Encephalitis
Parotidis
Herpes zoster virus
Pitted keratolysis
Tuberculosis
Miscellaneous
Alcoholism
Primary hypertrophic osteoarthropathy
PATHOGENESIS
The etiology of primary hyperhidrosis is not well understood. Positive family history has been reported in 34.1% to 65% of patients, suggesting a genetic predisposition.9,10,11,12
There is evidence that primary hyperhidrosis is inherited in an autosomal dominant mode of transmission with incomplete disease penetrance.13 The loci 14q11.2-q13 and 2q31.1, identified in Japanese and Chinese populations, respectively, have been associated with primary hyperhidrosis.14,15,16 Moreover, several genetic disorders are associated with hyperhidrosis, such as pachydermoperiostosis, pachyonychia congenita, ectodermal dysplasia, Book syndrome, Meleda disease, nail patella syndrome, and inflam-matory familiar palmoplantar keratoderma, among others.
Primary hyperhidrosis has been speculated to result from hyperactivity of the sympathetic nervous system due to emotional or thermal stimuli leading to overstimulation of the eccrine sweat glands. In addition, anatomical/histological changes, as well as metabolic, enzymatic, and neurological dysfunctions, have been observed in patients with primary hyperhidrosis, thus indicating a complex etiopathogenesis.17,18,19,20,21 Other trigger factors include spicy foods, drinks, alcohol, caffeine, and smells.
Secondary hyperhidrosis can be related to any number of underlying conditions, such as infections; endocrine, metabolic, neurologic, cardiovascular, and respiratory disorders; spinal cord injury; tumors; drugs; anxiety; and stress.1,2 It can commence at any point of life, and there is no gender predilection.
TREATMENT
Hyperhidrosis can be a disabling condition causing social and psychological problems with a negative impact on the patient’s quality of life.22 Hence, it is important to recommend the right treatment for the right patient to improve the unpleasant symptoms of the disease. Algorithm 9.3.1 presents the treatment algorithm for approaching hyperhidrosis.
Detection and treatment of the underlying condition is essential for the improvement of secondary hyperhidrosis. Patient education, general measures, and systemic drugs may be helpful in reducing sweat secretion.
Primary hyperhidrosis is a difficult-to-manage condition. Although many treatments are now available, there is no uniform treatment for all patients and all forms with good efficacy, with permanent duration, and without adverse reactions. Current treatment of primary hyperhidrosis includes general measures and lifestyle changes, topical products, systemic drugs, iontophoresis, botulinum toxin A injections, lasers or other energy devices, and various surgical interventions.23,24 All therapeutic aspects of the treatment of hyperhidrosis are included in Algorithm 9.3.1.
Medical
General Measures and Lifestyle Changes
These include weight loss, light dressing, cool environment, good hygiene, avoiding aggravating factors, and replacement of lost fluids and minerals.
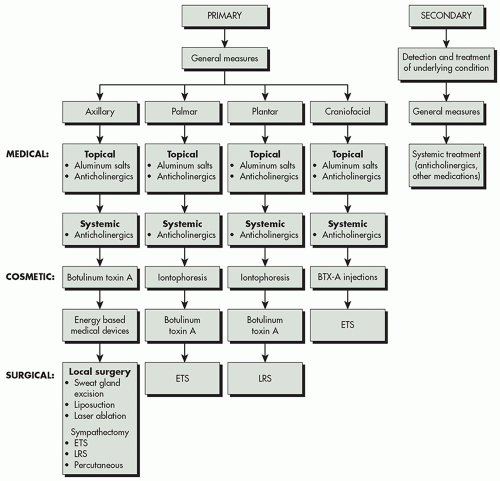 ALGORITHM 9.3.1 Treatment algorithm for hyperhidrosis. ELS, endoscopic lumbar sympathectomy; ETS, endoscopic thoracic sympathectomy. (Courtesy of Macrene Alexiades, MD, PhD.) |
Metallic Salts
Aluminum salts constitute a first-line therapy for mild to moderate focal hyperhidrosis.25 The majority of commercially available antiperspirant products contain 1% to 2% concentration of aluminum salts, whereas medical products contain 12.5% to 35% concentration. The most commonly used salts are aluminum chloride hexahydrate and aluminum chlorohydrate. The addition of zirconium salts increases the effectiveness of the above-mentioned formulations. Aluminum salts cause an obstruction of the sweat duct at the acrosyringium level, leading to functional and structural degeneration of eccrine glands with loss of secretory function.26 Metallic salts also have antimicrobial properties and are recommended to control body odor. They are diluted in ethanol or salicylic acid gel 2% to 4%. Salicylic acid has a keratolytic ability, which enables the hyperkeratotic skin to absorb the salts but without dehydrating the skin as ethanol does.27
The most frequent side effect is irritating dermatitis due to the formation of weak hydrochloric acid resulting from the reaction of aluminum chloride hexahydrate with water.28 The need for safer products prompted the search for alternative metallic salts.29 Carboxylic and hydrocarboxylic titanium salts decrease axillary hyperhidrosis in the same manner as aluminum salts and with a lower risk of irritating dermatitis. Moreover, a 10% concentration of ammonium titanium lactate was found to be more effective in the decrease of perspiration in vitro. Other topical agents, rarely used today because of side effects (irritation, allergic sensitization, skin staining, and central nervous system toxicity), include formaldehyde, glutaraldehyde, and tannic acid.
The most frequent side effect is irritating dermatitis due to the formation of weak hydrochloric acid resulting from the reaction of aluminum chloride hexahydrate with water.28 The need for safer products prompted the search for alternative metallic salts.29 Carboxylic and hydrocarboxylic titanium salts decrease axillary hyperhidrosis in the same manner as aluminum salts and with a lower risk of irritating dermatitis. Moreover, a 10% concentration of ammonium titanium lactate was found to be more effective in the decrease of perspiration in vitro. Other topical agents, rarely used today because of side effects (irritation, allergic sensitization, skin staining, and central nervous system toxicity), include formaldehyde, glutaraldehyde, and tannic acid.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree