Hair
OVERVIEW
Androgenetic alopecia (AGA) is often perceived as an indication of diminished physical attractiveness, particularly in Western societies. Disorders such as extensive alopecia areata and folliculitis decalvans are causes of hair loss that may lead to profound psychological problems. Other types of alopecia may be due to temporary disease or medication reactions (e.g., cytotoxic drugs, birth control pills, anticoagulants).
AGA in men and women (patterned alopecia), diffuse alopecia, occurring mainly in white women, and traumatic alopecia in women of African descent are the most common causes of hair loss in adults. Alopecia areata and tinea capitis account for most cases of alopecia in children.
For diagnostic purposes, it is helpful to recognize the pattern and distribution of hair loss. Whether patterned, as in male and female AGA; diffuse, as in telogen effluvium; focal, as in occipital alopecia of the newborn and most instances of alopecia areata; or patchy, as in tinea capitis, such findings afford important clues to its etiology.
Scarring alopecia, a permanent loss of hair follicles, also known as cicatricial alopecia, comprises a diverse group of disorders that may be due to infections, trauma (often self-induced), discoid lupus erythematosus, or lichen planopilaris. Scarring alopecia is seen in all ethnic groups and races; however, women and men of African descent are most often affected.
ALOPECIA-NON SCARRING
ADULTS
Androgenetic Alopecia
Androgenetic (AGA), which manifests as male- or female-patterned common baldness, commonly occurs with aging. Seen more frequently in men, AGA tends to be less apparent in women because hair loss in women is generally incomplete and begins at a later age, most notably at the time of menopause.
AGA is genetically influenced (autosomal dominant with variable penetrance) and is more common in whites than in Asians or blacks. It is caused by an androgenic action (dihydrotestosterone) on hair follicles that shortens the anagen (growth) phase of the hair cycle and thus produces thinner, shorter hairs in a process known as miniaturization.
Distinguishing Features
Diagnosis
Clinical pattern and absence of specific disease that may cause hair loss
Blood tests and other laboratory studies only when the diagnosis is in doubt
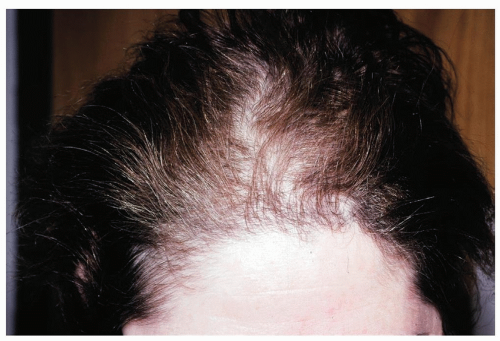
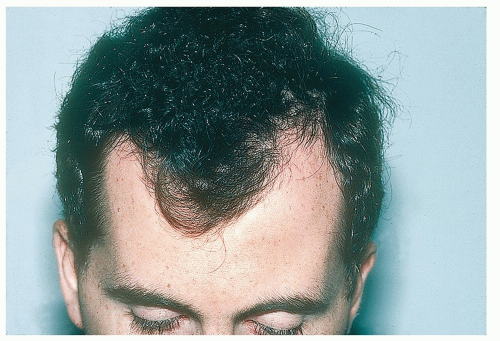 Figure 1-1 Male-pattern alopecia. This is characterized by an M-shaped recession on the frontal and temporal scalp. |
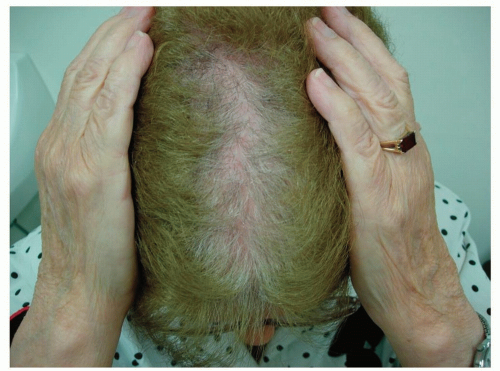 Figure 1-2 Female-pattern alopecia. The “widened part” in a “Christmas tree” pattern is seen in this patient. |
Management
Males
Minoxidil 5% solution (Rogaine)
Finasteride (Propecia)
Females
Minoxidil 2% or 5% foam or solution (Rogaine)
Systemic antiandrogen therapy (e.g., spironolactone or oral contraceptives), is sometimes used off-label for hair loss in women; however, it should not be used by women who may become pregnant because it may feminize a male fetus
Males and females
Hair transplantation
Wigs/hairpieces
Low-level light therapy
Platelet-rich plasma
Diffuse Alopecia
Diffuse alopecia is defined as a nonscarring reduction in hair density over all areas of the scalp. In many cases, the hair loss may not be apparent to the examiner and the cause may be difficult, if not impossible, to determine. Unfortunately, with the exception of acute telogen effluvium, the explanation for diffuse hair loss, most often seen in adult women, frequently presents a confusing and frustrating challenge.
Acute Telogen Effluvium
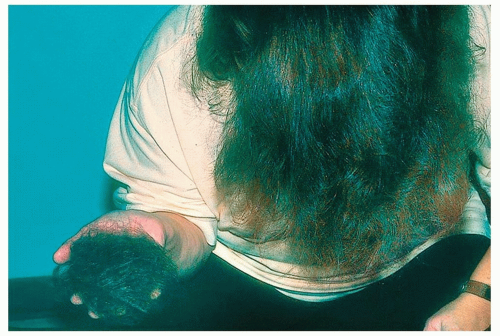
A sudden diffuse hair shedding favors the diagnosis of an acute telogen effluvium which is seen more commonly in females. Such nonpatterned shedding of resting (telogen) hairs may be triggered by a major preceding stressor such as an illness (e.g., acute systemic lupus erythematosus), a personal tragedy, childbirth (postpartum effluvium), a drug reaction (Fig. 1-4), major surgery, a “crash diet,” or chronic anemia. The hair loss typically occurs 2 to 4 months after the insult and the hair usually regrows in a few months without treatment. Drugs reported to induce telogen effluvium include thyroid replacement drugs, anticoagulants, beta blockers, systemic retinoids, and NSAIDs, among others.
Distinguishing Features
Diffuse, nonpatterned alopecia due to loss of resting (telogen) hairs
Usually without obvious completely bald patches (Fig. 1-5)
Diagnosis
Clinical presentation
Comprehensive history
When indicated, appropriate blood tests (e.g., thyroid-stimulating hormone, complete blood count, ferritin, total iron-binding capacity)
Punch biopsy of scalp, if necessary
Management
Most often, reassurance that hair will grow back
Minoxidil 2% or 5%
If indicated, attend to underlying medical or nutritional problem
Chronic Telogen Effluvium
This diffuse, nonpatterned type of hair loss, an ongoing progression of alopecia, is likely to involve the entire scalp
Initially, it tends to be subtle and is often not obvious to the clinician; however, the patient reports recurrent periods of increased shedding
There is no scarring or inflammation and hair thinning ultimately manifests as a more visible scalp
Management
When the cause of acute or chronic telogen effluvium is not clinically apparent, the following laboratory tests should be assessed when warranted by the history or physical examination:
Baseline chemistries and liver function tests
A complete blood count, sexually transmitted disease testing, and antinuclear antibody tests
Thyroid-stimulating hormone level
Serum ferritin, zinc, and erythrocyte sedimentation rate (ESR) levels (a ferritin value greater than 50 µg/L is optimal)
Serum dehydroepiandrosterone-sulfate (DHEA-S), free testosterone, prolactin, and morning cortisol levels (especially if virilization is evident)
Anagen Effluvium
Anagen effluvium results from the shedding of growing (anagen) hairs. It is most often due to cancer chemotherapeutic drugs. Compared to telogen effluvium, anagen effluvium produces a more extensive, more rapid, and dramatic loss of hair. The hair loss usually starts 1 to 2 weeks after the precipitating event
Among the agents that have been commonly associated with anagen hair loss are:
Drugs used for cancer chemotherapy (e.g., doxorubicin, nitrosoureas, cyclophosphamide)
Immunotherapeutic medications (cyclosporine, methotrexate, colchicine)
Intoxication with thallium or mercury
Radiation therapy
Management
Anagen effluvium is entirely reversible, and patients should be reassured that the hair loss is temporary
New hair growth starts a few weeks after the termination of treatment; however, the color and texture of the new hair may be different
Senescent Alopecia
Aging results in a gradual decrease of scalp hair density. This type of alopecia affects men and women equally and is seen in patients 50 years and older.
Senescent alopecia is a diffuse, nonscarring, noninflammatory type of hair loss. It represents a diagnosis of exclusion.
INFANTS AND CHILDREN
Occipital Alopecia of the Newborn (Telogen Effluvium of the Newborn)
Occipital alopecia of the newborn occurs at 3 to 4 months of age. It is an asymptomatic patch of alopecia localized to the posterior occipital scalp (Fig. 1-6).
Shifting into the telogen phase begins sometime in the third trimester or shortly after birth, and as a result a higher proportion of occipital telogen scalp hairs are shed creating a noticeable patch of alopecia on the posterior scalp. Sometimes the alopecia can be more extensive.
Friction created by rubbing the posterior scalp on the pillow or mattress is also a factor.
Spontaneous complete recovery occurs within months; no treatment is required.
Telogen Effluvium in Infants and Children
Telogen effluvium (TE) is the most common type of alopecia in children. It is characterized by diffuse hair shedding and thinning.
As explained above, TE occurs when a triggering event results in the simultaneous shifting of a large number of hairs into the telogen (shedding) phase.
In children, TE is seen in certain clinical scenarios: during the newborn period, after a severe acute illness, a major trauma, surgery, or malnutrition.
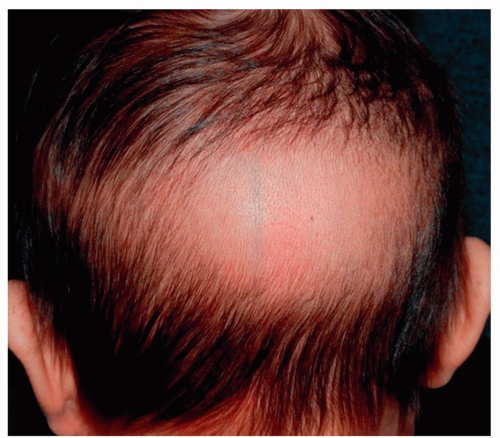 Figure 1-6 Occipital alopecia of the newborn (telogen effluvium of the newborn). Physiologic telogen effluvium presenting as alopecia localized to the posterior occipital scalp in young infants. |
Distinguishing Features
A subtle hair shedding and generalized thinning throughout the scalp occurs 2 to 4 months after the triggering event
Young children rarely notice a change in hair density
Affected adolescents and parents of young children may report an increased shedding as noted by an increased number of hairs on a brush or comb, on pillows or clothing
Clinical spectrum is variable and may go unnoticed
Management
If the cause of TE is not apparent, a workup may be necessary
Alopecia Areata
Alopecia areata (AA), an autoimmune disorder, is characterized by nonscarring hair loss. AA most commonly affects young adults and children. Persons with AA may also have a higher risk of atopy. In AA, biopsy findings demonstrate T-cell infiltrates surrounding hair follicles, reflective of autoimmune attack. AA may be associated with other autoimmune disorders, such as vitiligo, thyroid disease (Hashimoto disease), type I diabetes, Down syndrome, and pernicious anemia. AA is most often found on the scalp, eyebrows, eyelashes, and other hair-bearing areas of the face, such as the beard or mustache.
Distinguishing Features
One or many smooth oval, round, or geometric patches of alopecia
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree