The expression of the basement membrane zone (BMZ) components in the anagen hair follicles of the human scalp is similar to that of interfollicular epidermis. Expression of the BMZ components varies according to the different follicular portions. Blistering of the scalp, involving lamina lucida and below, usually leads to scarring alopecia secondary to the inflammatory process in the interfollicular epidermis and in the upper portion of the hair follicle. This article discusses the presence of alopecia in the most common acquired forms of bullous disorders.
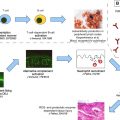
The expression of the basement membrane zone (BMZ) components in the anagen hair follicles of the human scalp is similar to that of interfollicular epidermis, with expression of plectin, 180-kD bullous pemphigoid antigen (BP180), 230-kD bullous pemphigoid antigen (PB230), a6b4 integrin, laminin 311, laminin 332, and type 4 and type 7 collagen. However, expression of the BMZ components varies according to the different follicular portions. In particular, the upper and middle portions of the hair follicle (infundibulum and isthmus), including the bulge region, show expression of all BMZ components with a labeling intensity under immunofluorescence similar to that found in the interfollicular epidermis. In the lower part of the follicle and in the hair bulb, expression of laminin 311 and collagen 4 is continuous, but labeling for other BMZ components shows a gradual decrease with discontinuous expression of a6b4 integrin and laminin 332, particularly outside the hair bulb. Between the dermal papilla and the epithelial cells inside the hair bulb, all of the BMZ components are evident, with the exception of the BP230. The reduced expression of all BMZ components outside the hair bulb and the complete absence of BP230 at the dermal papilla junction seem to be responsible for the incomplete ultrastructure of hemidesmosomes in these regions.
Desmosomes are important in hair structure and function. These components include the desmogleins 1 and 3 (Dsg 1 and Dsg 3), desmoplakins, plakophilin, and plakoglobin. Dsg 3 has been identified as a major component of murine and human hair follicle. In humans Dsg 3 shows the following pattern of expression in the outer root sheath (ORS): in the infundibulum, Dsg 3 immunopositivity is present predominantly in the basal cells, similar to the adjacent epidermis. In the isthmus, Dsg 3 immunopositivity in the suprabasal cells of the ORS is gradually lost toward the infundibulum. Below the isthmus, basal cells of the ORS show weak staining and Dsg 3 is present uniformly in all suprabasal cells of the ORS. This transition in Dsg 3 staining of the ORS correlates with the histologic onset of trichilemmal keratinization, which is characterized by abrupt keratinization lacking a granular layer, and a corrugated luminal surface.
Taken together, these findings show that in normal conditions the BMZ components show normal expression at the upper portions of the hair follicle and a gradual decrease in staining in the transient regions of the hair follicles (ie, at the level of the hair bulb). The complete structure of the hemidesmosomes is then responsible for the stabilization of the upper follicle to the surrounding connective tissues, whereas the incomplete hemidesmosome structure may facilitate the movement of the transient region.
Blistering of the scalp, involving lamina lucida and below, usually leads to scarring alopecia secondary to the inflammatory process in the interfollicular epidermis and in the upper portion of the hair follicle. This is the cause of alopecia in the junctional and dystrophic forms of epidermolysis bullosa (EB), as reviewed elsewhere by Tosti and colleagues. Herein, we discuss the presence of alopecia in the most common acquired forms of bullous disorders ( Table 1 ).
| Feature | Disease | Significance |
|---|---|---|
| Easily extractable anagen hairs | Pemphigus vulgaris Pemphigus foliaceus | Disease activity |
| Nonscarring alopecia | Pemphigus vulgaris Pemphigus vegetans Pemphigus foliaceus | — |
| Scarring alopecia | Mucous membrane pemphigoid Epidermolysis bullosa acquisita Bullous lupus erythematosus | — |
| Erosive cicatricial alopecia | Brunsting-Perry cicatricial pemphigoid | — |
| Tufted folliculitis | Pemphigus vulgaris | Scarring |
| Scalp scaling and crusting without alopecia | Pemphigus foliaceus | — |
| Scalp scaling and crusting with alopecia | Pemphigus foliaceus | — |
| Pruritic papules | Dermatitis herpetiformis | — |
| Alopecia areata | Pemphigus foliaceus Dermatitis herpetiformis | Coincidental |
Pemphigus group
Hair loss as a feature of pemphigus has been reported in several animal species such as dogs, cats, goats, and horses. On the other hand, although scalp involvement is common in pemphigus vulgaris (PV) and pemphigus foliaceus (PF), hair loss is rarely reported. Furthermore, the literature is not precise on the presentation and pathogenesis of hair loss in the reported cases.
Rodent Models
Dsg 3 knockout mouse model
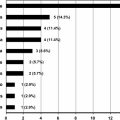
Genetically engineered mice that lack the desmosomal proteins Dsg 3 or desmocollin 3 have been used to study the pathologic mechanisms underlying acantholytic disorders. Koch and colleagues showed that mice without Dsg 3 (Dsg 3−/− knockout mice) not only developed mucous membrane and skin lesions like pemphigus patients but also developed hair loss. Hair was normal through the first growth phase around day 20; however, when the hair follicles entered the telogen phase, mice with a targeted disruption of the Dsg 3 gene lost hair in a wavelike pattern from the head to the tail. Hair then regrew and was lost again in the same pattern with the next synchronous hair cycle. Gentle hair pulls with adhesive tape showed that anagen hairs were firmly anchored but telogen hairs came out in clumps. In normal mice telogen hairs are retained until anagen hairs replace them underneath to prevent bald areas from forming and ascertain the synchronous cycling nature of the hair. Histology of bald skin areas in Dsg 3−/− mice showed cystic telogen hair follicles without hair shafts. Histology of hair follicles in early telogen, just before clinical hair loss occurred, showed acantholysis between the cells surrounding the telogen club and the basal layer of the ORS epithelium. The bald areas were still capable of regrowing hair, indicating that the stem cells in the bulge and the dermal papilla were not affected. The investigators concluded that Dsg 3 is necessary for anchoring the telogen hair club to the ORS and mice devoid of Dsg 3 develop acantholysis in the telogen hair with no defect in the anagen hairs. Telogen hair loss is usually not a feature of pemphigus in humans. However, it is important to consider that the human hair cycle is not synchronous and only 5% to 20% of the follicles in the scalp are in telogen; hair loss can then be subtle if only telogen hairs are affected by the acantholysis.
Balding phenotype mouse with bal mutations
Mice with spontaneous mutations of the Dsg 3 gene (balding phenotype mice with homozygous bal J and bal Pas mutations) develop alopetic lesions accompanied by vesicles on the ventral tongue, mucocutaneous junction of the eyelid, foot pads, and rarely the skin. Dsg 3 is located on mouse chromosome 18 in the region of the balding locus. In the hair follicle separation occurred between the outer layers of the ORS whereas the separation in the epidermis of the skin was clearly formed by cleavage between basal and suprabasal layer (a pattern characteristic for PV). As opposed to the finding that acantholysis developed between telogen club hairs and the ORS in Dsg 3 knockout mice bal J , in the balding phenotype mice separation of the inner and outer layers of the ORS was most prominent in anagen hair follicles, which resulted in poor anchorage of the hair fiber in the anagen follicle. This finding explains why hairs came out easily in tufts on gentle pulling. The bal mice rarely show cutaneous blisters and do not have circulating pemphigus antibodies against the desmosomes. This characteristic is believed to be because of their thicker hair density and thinner epidermis than humans; blistering was inducible with minor trauma. Murine models have provided compelling evidence that abnormalities in the Dsg 3 gene expression or protein adhesion are followed by defective anchoring of hair shafts within the follicles and alopecia. It is still unexplained why the phase of the hair cycle affected by acantholysis is different in the Dsg 3 knockout mice model (telogen) and the bal mutation model, which is the result of a premature stop codon (insertion of a thymidine in the Dsg 3 gene) (anagen).
Hair Plucking in the Diagnosis of Pemphigus
Even in patients without alopecia who have pemphigus, plucked hair shafts have been used in lieu of skin biopsies to diagnose pemphigus on direct immunofluorescence, because IgG and C3 are positive in between the ORS cells.
Hair Loss Patterns in Pemphigus
Scalp involvement is common in PV because the hair follicles contain many PV antigens and severe scalp involvement can be a feature of recalcitrant disease. However, hair loss or alopecia is not commonly reported. Different types of hair loss reported in PV include anagen shedding, telogen effluvium (TE), scarring alopecia, and tufted folliculitis.
Anagen shedding with and without alopecia
Anagen effluvium has been described in 3 patients with PV. In all 3 cases, hair loss was evident as easy shedding within and around erosive lesions on the scalp. All patients regrew hair completely with disease control. The pulled hairs appeared as anagen hairs with normal pigmentation and intact root sheaths. Direct immunofluorescence revealed deposits of IgG and C3 within the ORS where clefts were present. According to the author, the anagen shedding was not related to the erosions and crusts because normal anagen hairs were obtained also from the perilesional area of the scalp. The anagen hairs came out easily with their ORS because of the cleavage within the ORS of the follicles where the pemphigus antibodies bound to the overexpressed desmosomal proteins. The shedding of anagen hair in PV was referred to as Nikolsky sign of the scalp and is considered as a subclinical involvement of the follicle. It heralded pemphigus in one of the reported patients and can possibly be used to verify disease activity. Although this phenomenon has been described as anagen effluvium we believe that anagen shedding is the best term to describe loss of anagen hair in pemphigus. The diagnosis of anagen effluvium generally refers to acute anagen arrest with shedding of dystrophic or broken hair shafts, such as in cases of antimitotic chemotherapy treatment.
Telogen effluvium
TE is not commonly reported by patients with PV and in our experience is not a feature of the disease. According to Koch and colleagues. this finding may be because human follicles are not synchronized and that telogen loss becomes evident only when severe. Therefore, patients may have mild TE that goes unnoticed. However, these investigators found pathologic evidence of TE in a scalp biopsy of 1 patient.
Scarring alopecia and tufted folliculitis
One of the authors (DM) has seen a patient who developed scarring alopecia after PV persistently affected an area of his scalp ( Fig. 1 ).