20 Facial Trauma Abstract The face is one of the most commonly affected regions in a traumatized patient, occurring in approximately 10% of polytrauma cases. The craniofacial skeleton provides the framework for muscle attachment and defines facial dimensions, volumes, and contours; protects delicate structures (e.g., eyes, brain); and performs functional and structural roles in mastication and airway. In addition, the soft tissue component contains highly important aesthetic and functional elements, such as the ears, eyelids, nose, and lips. Maxillofacial injuries may include the soft tissues and the craniofacial skeleton, with each of these components needing proper assessment, accurate diagnosis, and timely and precise repair in order to optimize patient outcomes. Prior to maxillofacial evaluation, patients sustaining severe trauma should undergo more urgent interventions, namely airway management, bleeding control, and assessment of associated traumatic injuries. The main goals of facial fracture treatment include three-dimensional anatomical reduction, maximum immobilization at the fracture site, and the highest possible degree of freedom of movements that yields primary bone healing. Depending on the type of reduction and the degree of mobility of the fragments, treatment methods can be classified as conservative (e.g., interdental block, intermaxillary block, dental splints), with or without closed reduction, and surgical, comprising open reduction and internal fixation (rigid and semirigid). Finally, the rate of complications and sequelae are directly related to the complexity of the facial trauma and the difficulty of three-dimensional fracture reduction and fixation. Keywords: facial lacerations, frontal fractures, mandibular fractures, maxillofacial buttresses, midface fractures, osteosynthesis, polytrauma Trauma is defined as the damage sustained by tissues and organs by the acute or chronic action of energy. Maxillofacial trauma involves both the soft tissues and the bony skeleton of the facial region and occurs in approximately 10% of multiple trauma patients. Approximately 1.7 million head injuries occur annually in the United States. Alcohol is a contributing factor in almost 50% of head injuries. A review of the Maryland Shock Trauma Registry (1986–1994) reported that 11% of trauma patients (2,964 of 25,758) sustained maxillofacial fractures requiring subspecialty intervention. Variables affecting type and severity of injury include the area of impact (the specific anatomical location that receives the energy), a resistant force (resultant movement of the head), and angulation of the impact, with more severe injury occurring with perpendicular delivery of energy than with tangential delivery. The craniomaxillofacial skeleton is designed to protect vital soft structures, including the nervous system, eyes, and respiratory and digestive tracts. The head consists of the cranial vault and the maxillofacial skeleton with its vertical and horizontal buttresses ( • Primary: Without callus formation so that the process is shortened to one stage. For primary consolidation to ensue, a perfect reduction, good blood supply, rigid stabilization, and lack of micromovements are needed. Interfragmentary compression is important because the bone evolves according to the forces suffered and compression favors primary bone healing. Table 20.1 Horizontal and vertical buttresses of the facial skeleton
20.1 Introduction
20.2 Relevant Anatomy
 Table 20.1 and
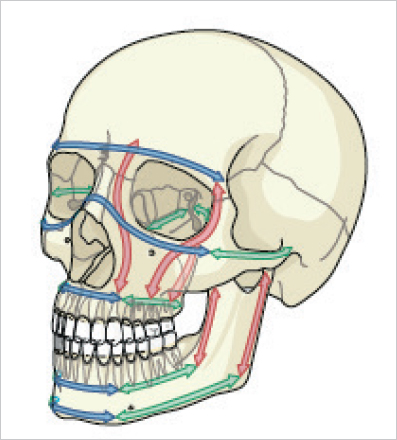
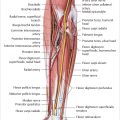
Table 20.1 and  Fig. 20.1). The buttresses are key elements that allow reconstruction of the facial skeleton and osteosynthesis fixation. Their proper reduction and stabilization guarantee optimal restoration of the volumes of the face. Bone healing after a fracture can occur through primary and secondary mechanisms:
Fig. 20.1). The buttresses are key elements that allow reconstruction of the facial skeleton and osteosynthesis fixation. Their proper reduction and stabilization guarantee optimal restoration of the volumes of the face. Bone healing after a fracture can occur through primary and secondary mechanisms:
Horizontal buttresses | Vertical buttresses |
Superior orbital rim | Ascending process of maxilla |
Inferior orbital rim | Lateral orbital ridge |
Zygomatic arch | Zygomatomaxillary union |
Maxillary alveolar ridge | Pterygomaxillary union |
Mandibular body |
• Secondary: Occurs with callus formation and is typically observed in fractures treated orthopaedically. It happens as a consequence of separation between fragments, a reduced vascular supply, poor stability, and lack of compression.
Remember 
The aim of osteosynthesis is to achieve primary bone healing of the maxillofacial fracture.
20.3 Soft Tissue Trauma
20.3.1 Classification
• Abrasion: scraped area of skin.
• Laceration: jagged cut or tear.
• Avulsion: tearing resulting in an area of skin lifted off the underlying tissue.
• Crush: damage caused by compression; often results in greater tissue injury.
• Miscellaneous: gunshot wound (substantial soft tissue injury may warrant early intubation, soft tissue deficits are often minimal); bite (associated with polymicrobial infections: Eikenella corrodens and Streptococcus viridans in human bites, Pasteurella canis in canine bites, Pasteurella multocida in feline bites).
20.3.2 Initial Evaluation
A thorough and systematic assessment of the traumatized face is essential to make an accurate and complete diagnosis of the injury and provide appropriate treatment. Particular attention should be given to the mechanism of injury and characteristics of the wound. Patients with a significant mechanism of injury may have associated critical injuries, which mandates evaluation following Advanced Trauma Life Support (ATLS) guidelines. Careful attention is given to soft tissue injuries near specialized facial structures, such as the external auditory meatus, lacrimal apparatus, facial nerve, and parotid duct.
General Management
The risk of infection increases the longer the wounds remain open; therefore, closure should be performed as soon as the patient is stabilized. Of note, the rich vascularity of the head and neck makes it more resistant to infection than other areas of the body.
Bleeding
The rich vascularity of the head and neck region can lead to significant blood loss from lacerations, though rarely resulting in hypovolemic shock. Hemorrhage can usually be controlled with local pressure. Avoid blind clamping to prevent iatrogenic injury to specialized structures.
Irrigation and Debridement
Irrigation and removal of foreign bodies from wounds is essential before closure to reduce the risk of infection. In addition, debris that is not removed from the dermis can result in permanent (traumatic) tattooing. All devitalized tissue should be removed by sharp debridement. The surgeon needs to be conscious about the extent of debridement in functional and aesthetically important areas, such as the nose, periorbital region, lips, ears, and hair-bearing skin. Excessive removal of tissue in these zones may lead to severe disfigurement.
Repair
Local flaps should be avoided in the acute setting until the extent of the devitalized tissue has declared itself. Layered closure is preferred to reduce tension but may increase the risk of subsequent infection in a dirty wound.
• Abrasions: Partial-thickness wounds should be treated with antibiotic ointment while they are still fresh and moisturizing lotion once epithelialization occurs. Full-thickness tissue loss should be managed with dressing changes until the wound is stable and clean enough to be resurfaced with skin grafts or local flaps.
• Lacerations/avulsions: Closure of these wounds should ensure obliteration of dead space by layered closure, which may include tension-free approximation of skin, muscle, and fascia. Sutures should be placed carefully and at the appropriate tightness to prevent strangulation of tissues.
• Bite wounds: Bite wounds elsewhere in the body should be left open, whereas in the face they may be loosely approximated following aggressive irrigation and debridement. For commonly associated organisms, extended-spectrum β-lactam (amoxicillin/clavulanate) or fluoroquinolone antibiotics are appropriate. Administration of human rabies immunoglobulin and human diploid cell rabies vaccine should be considered depending on animal follow-up and the local epidemiological situation.
Medications
Prophylactic antibiotics may provide benefit in grossly contaminated wounds, immunocompromised patients, open fractures, wounds contaminated with oral secretions, and those presenting for delayed wound closure. In addition, tetanus prophylaxis should be considered in the presence of risk factors including time since injury (> 6 hours), depth of injury (> 1 cm), mechanism of injury (crush, burn, gunshot, puncture), presence of devitalized tissue, and contamination (grass, soil, saliva, retained foreign body). History of immunization and local epidemiological situation should also be considered.
Note
General management includes bleeding control, irrigation and debridement, structures repair, and medications.
Specific Management by Anatomical Zones
The sensory innervation and regional anesthetic blocks of the face and scalp are described in Chapter 5. The following section focuses on the technical aspects of wound closure in the different areas.
Scalp
Scalp lacerations usually bleed profusely. The scalp is richly vascularized, and the vessels running in the plane between the subcutaneous layer and the galea are attached to the latter, which prevents them from retracting upon sectioning. Layered closure should be performed approximating the galea with interrupted 2–0/3–0 absorbable sutures and epidermis with 4–0 nonabsorbable monofilament sutures or staples.
Forehead
Forehead lacerations may injure the frontal branch of the facial nerve or the frontalis muscle directly, which may cause brow ptosis. Layered closure should be performed, repairing the frontalis with interrupted 3–0/4–0 absorbable sutures and skin with interrupted 5–0/6–0 nonabsorbable monofilament sutures.
Eyebrow
The eyebrow is a unique structure that is difficult to replace. Therefore, it is important to preserve it as much as possible by performing minimal debridement and avoiding shaving. Wounds should be closed in a layered fashion using interrupted 5–0 absorbable sutures for the dermis and interrupted 6–0 nonabsorbable monofilament sutures for the epidermis.
Eyelid
The eyelid contains different structures that may be lacerated and need repair, including the tarsal plate, orbicularis muscle, and skin. Special evaluation is required for injury to the septum and levator palpebrae muscle—if left unrepaired, levator disruption may result in eyelid ptosis. Sutures adjacent to the cornea should be avoided to prevent abrasions. Eyelid lacerations should be closed using 6–0 absorbable sutures for the tarsus and orbicularis and 6–0 or 7–0 nylon for skin. Lacerations through the lid margin require careful closure to prevent lid notching and misalignment. The lid margin should be precisely approximated and the palpebral borders everted to prevent notching.
Lacrimal Apparatus
Tears drain into puncta located on the medial half of the upper and lower lids. Injuries to the lacrimal punctum are therefore associated with medial eyelid lacerations and occur most commonly on the lower eyelid. If a canalicular injury is suspected, it should be cannulated with a lacrimal probe to identify the site of laceration. Direct repair over a Silastic or polyethylene lacrimal stent is performed using 8–0 absorbable sutures, leaving the stent in place for 4 weeks. If cannulation is impossible dacryocystorhinostomy may be necessary.
Ear
Traumatic ear injuries are normally repaired in one layer by approximation of skin only using 5–0 or 6–0 nylon sutures with proper eversion to avoid unsightly grooves. Cartilage is not usually sutured as a separate layer as long as correct alignment and preservation of important landmarks are achieved with skin suturing. If cartilage needs to be sutured, 5–0 absorbable material is recommended.
Two of the most serious complications following injury to the auricle are hematoma and cartilage infection (e.g., chondritis). Hematomas may develop from bleeding from a laceration or as a consequence of blunt trauma in which the cartilage is detached from the overlying soft tissues and blood accumulates in the space. Hematomas can lead to cartilage resorption or reactive chondrogenesis, which results in a permanent thickened fibrotic deformity referred to as cauliflower ear deformity. Hematomas should therefore be drained as quickly as possible and compressed with a bolster dressing with or without through-and-through sutures. Cartilage infection may result in significant resorption and should be treated promptly. Unfortunately, chondritis is sometimes difficult to treat due to the reduced blood supply to the ear that prevents proper reach of antibiotics. Finally, in circumferential external auditory canal lacerations, a stent should be placed to prevent stenosis.
Nose
Nasal lacerations may comprise skin, cartilage, and mucosa. These need to be evaluated and repaired in a layered fashion if required. Skin and soft tissue are approximated using absorbable sutures for the deep dermis and nonabsorbable for the skin. If the cartilaginous framework is damaged, the pieces should be properly reduced and sutured separately from the skin using monofilament nonabsorbable suture. Finally, mucosal lacerations are approximated with 4–0 absorbable sutures. Patients with nasal injuries should undergo intranasal examination to rule out septal hematomas. Treatment involves incising the mucosa and nose packing to prevent reaccumulation. If overlooked, a septal hematoma can lead to septal perforation and saddle nose deformity.
Salivary Glands
Injury to the salivary glands can result in sialocele or cutaneous fistula if untreated. Lacerations through the cheek may injure the parotid (Stensen’s) duct. If injury is suspected, the duct is located intraorally opposite the second maxillary molar and stented with a 24-gauge angiocatheter. Extravasation of saline after infusion indicates an injury, which should be repaired using microsurgical techniques. A direct repair over a Silastic stent may provide benefit. Submandibular gland lacerations should be marsupialized to the floor of the mouth.
Lip
The lips are an important aesthetic component of the face; therefore precise realignment of the structures involved is paramount. Full-thickness lacerations are repaired by approximating each layer separately, using 3–0/4–0 absorbable sutures for the mucosa and orbicularis muscle and 6–0/7–0 nylon for the skin and dry vermillion. The skin–vermillion border (white roll) must be exactly approximated to obtain the best cosmetic result. Discrepancies as little as 1 mm are noticeable at conversational distance.
Note
Align the lip injury at the level of the white roll to avoid obvious irregularities.
Nerves
Nerves at risk in any facial laceration are mainly branches of the trigeminal and facial nerves and should always be assessed prior to the administration of anesthesia. Facial nerve stumps can be identified with the aid of a nerve stimulator up to 72 hours after injury, after which the distal end may no longer be responsive, making stump identification more difficult. Also, it is important to note that facial nerve lacerations medial to the lateral canthus or the oral commissure may be too small to repair
Postoperative Care and Complications
Routine wound care of facial lacerations is indicated to prevent desiccation. Antibiotic ointment is applied until wounds are epithelialized, after which moisturizing lotion is recommended. Sutures are removed at 5–7 days for the face and neck and 2–3 weeks for the scalp.
As with any wound, head and neck lacerations may be complicated by hypertrophic scarring, hyperpigmentation, scar contracture, and alopecia. Sun exposure is the main cause of hyperpigmentation and should be avoided for up to 1 year after wounding, with the use of protective clothing and sunscreen. Scar contracture may lead to deformation of the normal anatomy and produce important functional deficits. Scar release and reconstruction with z-plasties or other procedures are usually performed once the scars have maturated. Alopecia can be associated with excessive use of cautery and traumatic tissue handling, which should be minimized during wound repair.
20.4 Maxillofacial Trauma
20.4.1 Classification
1. Depending on the type of fracture:
• Closed/open.
• Simple/comminuted.
• Displaced/nondisplaced.
• Stable/unstable.
2. According to the parts involved and their location:
• Soft tissue trauma (see previous section).
• Trauma of the facial skeleton.
○ Upper third (fronto-orbital fractures).
○ Middle third (nasoorbitoethmoidal [NOE], zygomaticomaxillary fractures).
○ Lower third (mandibular fractures).
20.4.2 Clinical Evaluation
Initial Evaluation
Initial assessment of the patient with facial trauma should follow the ABCDE principles and ATLS guidelines. The following are the most important issues related to maxillofacial trauma:
• Airway management: Patients with severe maxillofacial trauma are at risk of upper airway obstruction due to clots, teeth, bone fragments, edema (floor of mouth, pharynx, and larynx), hyoid retroposition (in mandibular fractures), and aspiration of fluids (saliva, gastric content). Establishing an artificial airway is mandatory in cases of clear obstruction, inability to clear secretions, or unconsciousness, and is most commonly obtained by endotracheal intubation. This and other maneuvers aimed at maintaining a patent airway should be done with care in patients with cervical spine injury or skull base fracture because manipulation may further aggravate these injuries.
• Bleeding control: Massive hemorrhage from maxillofacial trauma is uncommon and may be seen in cases of massive scalp injuries, penetrating soft tissue injuries, and midface fractures. In most cases, bleeding can be effectively controlled by compression and hemostasis in the operating room. Middle third fractures may bleed copiously from less accessible sources, including the ophthalmic, maxillary, and ascending pharyngeal arteries. The sequence of treatment in these cases is anterior and posterior nasal packing, intermaxillary fixation, selective angiography and embolization, and ligation of external carotid and superficial temporal arteries.
• Associated traumatic injuries: Patients with maxillofacial trauma often have other injuries, such as serious cervical spine injury in 2–4%; encephalocranial trauma in 50%, including intracranial injury in 5–10% and skull base fracture in 25%; eye injury in 25–29%; and blindness in 2–6%. In these cases ophthalmologic evaluation and intervention are paramount.
Maxillofacial Evaluation
• Anamnesis: The mechanism and time since injury can give an idea of the magnitude of the trauma and injuries. Among the patient’s history, it is important to consider associated pathologies and comorbidities, alcoholism, allergies, medications, previous facial fractures, visual disturbances, denture condition, malocclusion, and previous treatments. In addition, the awake patient may report localized pain, hypoesthesia, malocclusion, and diplopia.
• Physical examination: The traumatized face should be systematically and rigorously examined so as not to overlook any potential injuries. Assessment should include inspection and palpation together with ophthalmic, auditory, nasal, and oral examinations.
○ Inspection: should include pictures prior to trauma and documentation of any soft tissue injuries, facial asymmetry, contour deformities, localized swelling and bruising.
○ Palpation: must be done in a systematic and orderly fashion, in a cephalocaudal direction examining bilateral bony prominences, fracture irregularities, localized pain, pathological mobility, bone crepitus, and hypoesthesia, which is indicative of nerve damage associated with the fracture.
○ Ophthalmic examination: should include visual acuity, visual field, ocular motility, pupil response, and fundus as well as documentation of any eyelid, conjunctival, and corneal injuries or lacerations. Raccoon eyes (periorbital ecchymosis) are indicative of skull base fractures.
○ Auditory examination: should include the ear canal and periauricular region, which can give clues about underlying fractures. Discharge of cerebrospinal fluid (CSF), hemotympanum, and Battle’s sign (mastoid ecchymosis) are suggestive of skull base fractures. Otorrhea may also be present in condylar fractures.
○ Nasal examination: facial trauma involving the nose can present with epistaxis from a nasal fracture or CSF rhinorrhea, which is observed in cases of cribriform plate fracture in NOE fractures. Anterior speculoscopy must be done to rule out septal hematoma and CSF rhinorrhea.
○ Oral examination: should include assessment of edema, loose/displaced/fractured/missing teeth, bleeding from gingival lacerations or other lesions, dental occlusion, caries, and mouth opening in patients that have sustained maxillofacial trauma.
Remember 
Before maxillofacial evaluation, it is important to establish a patent airway, control bleeding, and rule out associated traumatic injuries.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree