Introduction
Facial paralysis and its sequela is a complex medical issue that can be both physically and emotionally distressing. Patients may present to us at any time along the continuum of their recovery or lack of recovery. In addition to the medical aspects of treatment, psychosocial impacts are common and must also be addressed. Here we discuss our approach to the evaluation and early management of patients with facial nerve dysfunction.
History
Upon initial evaluation for facial nerve dysfunction, there are a few key components of the history that are invaluable in diagnosing and ultimately guiding management. First, a timeline of the onset of facial paralysis is essential. It is important to understand if the paralysis occurred immediately or over the course of a few days or months. This needs to be followed up with further questioning about the severity of the weakness, to include partial or complete paralysis. If some time has passed since the onset of facial paralysis, a timeline of recovery is also needed. Certain etiologies, such as Bell’s palsy, are supported by recovery of facial function within 2 to 3 months. Failure to recover function within that period may indicate a different etiology and further workup with imaging and nerve conduction studies may need to be initiated.
The health care provider should also ask specific questions that might indicate more clearly the etiology of the dysfunction. Common causes are inflammatory post viral, neoplasms, trauma, congenital, and infection including otologic pathology. , Questions for diagnostic purposes can include personal history of past facial paralysis, family history, presence of vesicles or rashes, travel history, or recent surgery or trauma. The practitioner should also note other symptoms temporally associated with onset of facial paralysis such as hearing loss, dizziness, facial pain, facial twitching, or facial swelling.
The next part of the history should discern if the patient has received any prior treatments for their paralysis such as steroids or antivirals. Some patients may have participated in facial exercises or electrical stimulation to aid in their recovery. , , Questions regarding past imaging are necessary and may direct further workup. In the setting of tumor extirpation or oncologic causes of facial paralysis, radiation therapy may have been performed or may be planned in the future.
As each patient has a unique perception of their facial deficit, it is imperative to ask each patient to articulate what is most bothersome to them, as this may not always correlate to the most notable deformity to the clinician. Patient-driven care can be appropriate, especially in the partially recovered facial paresis or synkinetic patient.
The Role of Patient-Reported Outcome Measures
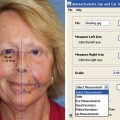
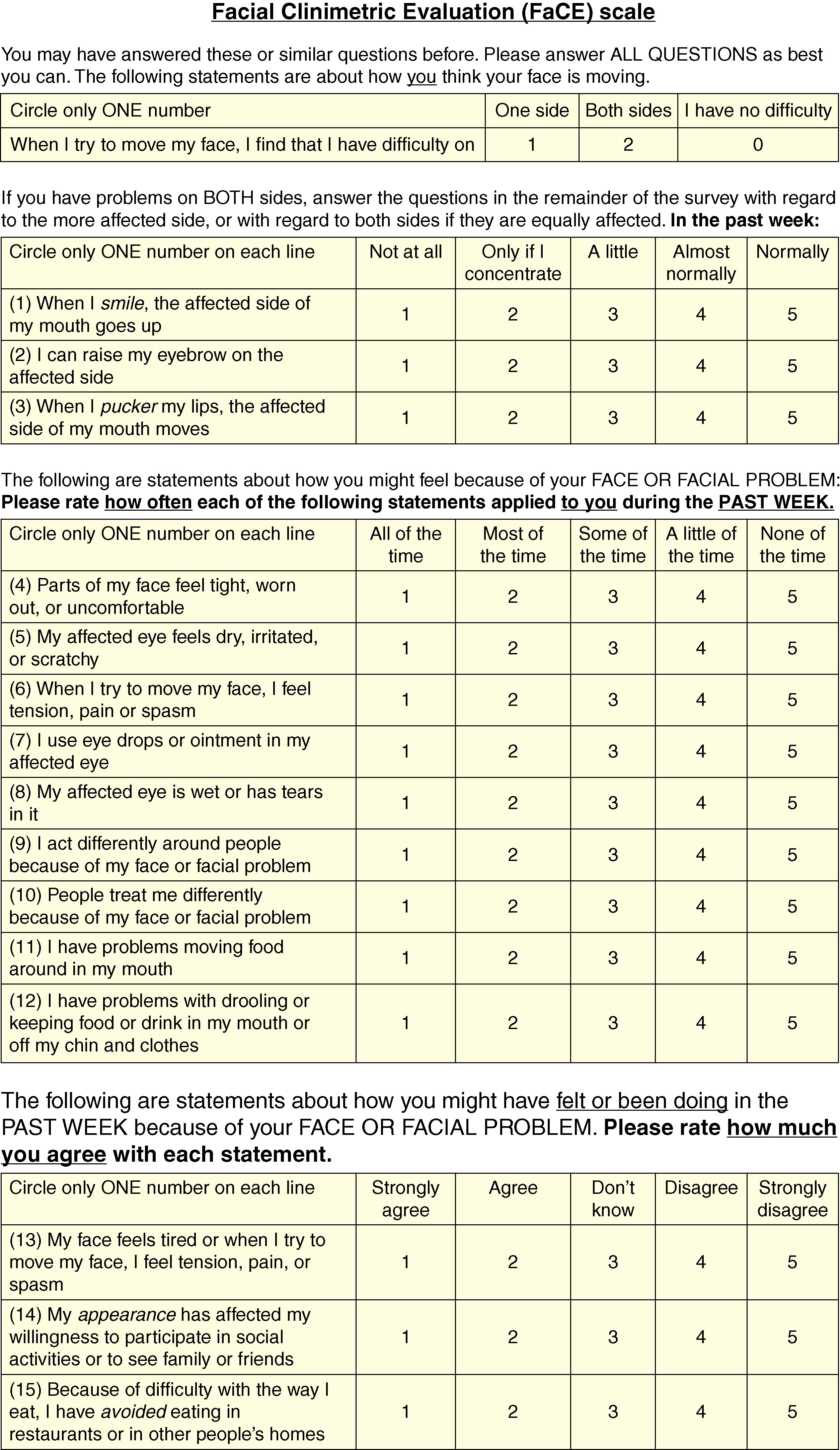
Facial nerve dysfunction can take a great emotional toll on patients, causing them to withdraw from social interactions. The psychosocial impact of the individual’s facial paralysis must be directly explored during the initial evaluation. Patients often have a negative self-image and low self-esteem. To the observers, these patients can be thought of as displaying a negative affect, which may lead to social isolation. Quality of life studies have shown that facial paralysis is significantly associated with depression. This profound emotional component must be part of the assessment of patients with facial nerve dysfunction. Some of the patient-reported outcome measures (PROMs), such as the Facial Disability Index (FDI) and Facial Clinimetric Evaluation (FaCE), are very useful in aiding the clinician in capturing additional and useful information about the patient’s quality of life ( Fig. 4.1 ). , , , , Furthermore, PROMs can be useful in research outcome studies to evaluate the efficacy of our treatment methods. It is useful to have resources such as online or in-person support groups and counseling to offer to facial nerve patients in addition to traditional treatment modalities.

Physical Examination
Once a thorough patient history is elicited, a detailed physical examination assessing the function of the facial nerve must be completed. Traditionally, the House-Brackmann scale has been an objective way to measure facial dysfunction. However, this scale is more of a broad overview of facial nerve function without assessing specific affected facial regions. , , , , A more detailed characterization of the defect is warranted. It is good practice to divide the face into five overall sections: forehead, periocular, midface, perioral, and cervical. From there, documenting the deficits associated with each division is ideal ( Table 4.1 ). Once there is a more precise characterization of deficits and symptoms, this will aid in the decision-making process for rehabilitation and treatment, as well as allowing for more precise assessment of treatment results.
| Facial Divisions | Facial Deficit |
|---|---|
| Forehead | Tone Synkinesis Brow elevation Brow ptosis |
| Periocular | Tone Synkinesis Visual acuity Corneal integrity Tearing Bell’s phenomenon Lagophthalmos Lower lid laxity Lacrimal puncta position |
| Midface | Tone Synkinesis Oral commissure excursion Nasal obstruction |
| Perioral | Tone Synkinesis Oral incompetence Articulation errors |
| Cervical | Tone Synkinesis |
A complete head and neck examination is necessary to evaluate prior incisions and deficits as well as the status of other cranial nerves. Injury to candidate donor nerves for reanimation may dictate the treatment options for a patient. Presence of palpable and/or visible extratemporal causes of facial paralysis must be ruled out. To the general practitioner, smaller parotid tumors may elude a rudimentary physical examination. The presence or history of skin cancer can be a concerning factor in patients with initially incomplete but progressive facial nerve paralysis.
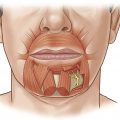
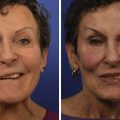
Another important aspect of assessing facial dysfunction is facial tone. Abnormal facial tone is evident to the casual observer, even when the patient is at rest, and therefore can have a profound impact on the patient’s ability to participate in the community. Facial tone may be either hypertonic or hypotonic, both of which may exist in the same individual ( Fig. 4.2 ) ( ![]() ). This distinction is important as there are different treatment approaches for both. , , , ,
). This distinction is important as there are different treatment approaches for both. , , , ,