Introduction
The facial nerve, also known as the seventh cranial nerve, combines motor, general sensory, special sensory, and autonomic (visceral) components. The intricate course of the facial nerve as it runs intracranially, intratemporally, and extratemporally is essential for any surgeon operating in the head and neck to understand. The facial nerve innervates the muscles derived from the second branchial arch and carries sensory and parasympathetic fibers of the nervus intermedius. The facial muscles, also known as mimetic muscles, function to protect the eye, maintain the nasal airway, provide oral continence, and articulate speech. Equally as important, these mimetic muscles provide humans the means for emotional expression and interpersonal communication. This chapter details an anatomic description of the facial nerve and musculature with a focus on anatomy and physiology as they relate to facial nerve disorder and treatment.
Facial Nerve
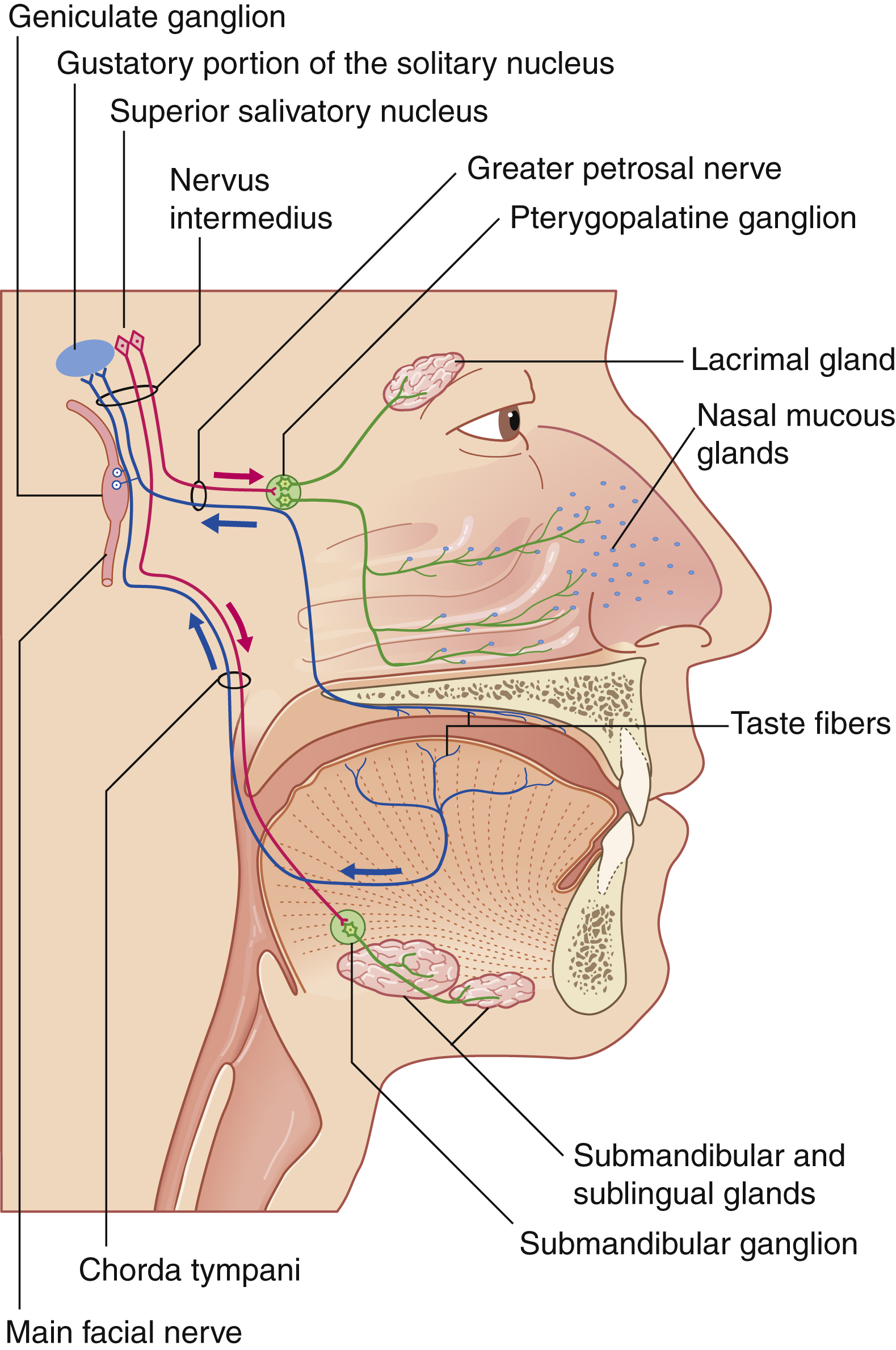
The facial nerve provides a diverse range of functions via efferent and afferent innervation to structures of the second branchial arch. The most well-associated function of the facial nerve is its innervation of striated muscles of facial expression. These functions will be the focus of this chapter. However, additional efferent motor fibers provide innervation to the stapedius muscle, the stylohyoid muscle, and the posterior belly of the digastric. Collectively, these motor fibers represent the special visceral efferents comprising the majority of the facial nerve fibers. The remaining efferent fibers of the facial nerve are general efferent fibers and form autonomic contributions. These autonomic nerves travel via the greater superficial petrosal nerve (GSPN) to the lacrimal gland and seromucinous glands of the nasal cavity and via the chorda tympani to the submandibular and sublingual glands. Traveling with this autonomic system, v isceral afferent fibers supply visceral sensation to the mucosa of the nose, pharynx, and palate. Additional afferent inputs include special sensory fibers and somatic sensory fibers. Special sensory fibers for taste to the anterior two-thirds of the tongue, tonsillar fossa, and palate originate from the geniculate ganglion cell bodies and travel within the chorda tympani and GSPN. Somatic sensory fibers provide touch sensation to the external auditory canal and conchal skin of the auricle as well as proprioceptive information from the facial muscles ( Fig. 1.1 ).
Intracranial
Facial muscle movement starts with a conscious or unconscious impulse in the motor cortex of the precentral gyrus of the cerebral hemispheres. The majority of cerebral fibers then project to the contralateral facial motor nucleus via the corticobulbar tract through the thalamus along the posterior limb of the internal capsule. However, a subset of cerebral fibers controlling movement of the frontalis and upper orbicularis oculi project to both the ipsilateral and contralateral facial motor nuclei. A central lesion will thus cause frontalis-sparing facial paralysis due to the bilateral contributions to the upper face. The precentral gyrus fibers synapse in the facial motor nucleus, residing in the pontine tegmentum. Postsynaptic fibers then travel dorsally within the brainstem, loop around the floor of the fourth ventricle at the facial colliculus, and exit the ventrolateral aspect of the brainstem at the caudal border of the pons in the cerebellopontine angle ( Fig. 1.2 ).
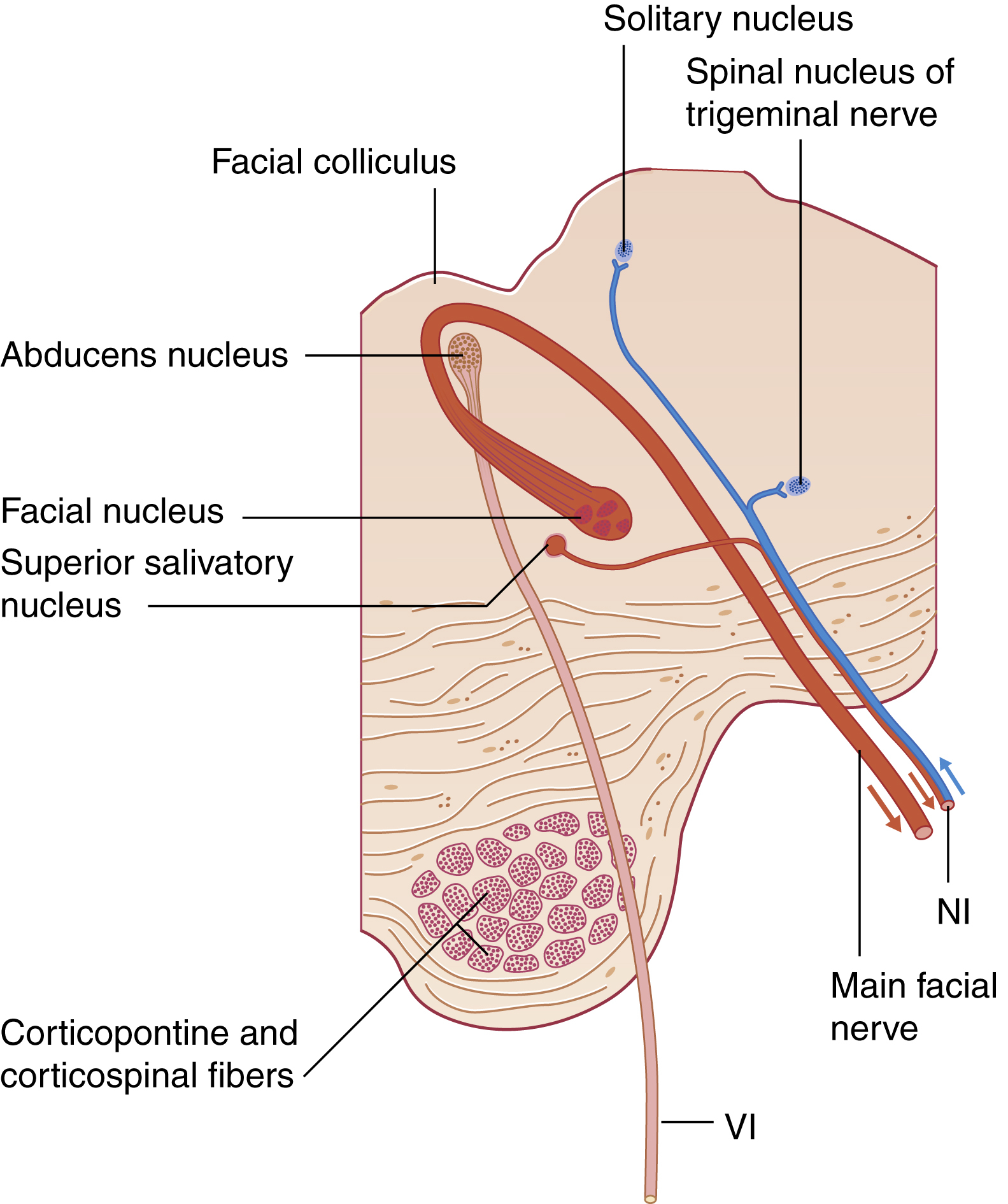
Collectively known as the nervus intermedius , preganglionic fibers of the superior salivatory nucleus and sensory fibers from the nucleus of tractus solitarius exit the brainstem directly lateral to the facial nerve motor root. Together, the facial nerve motor root and nervus intermedius enter the internal auditory canal (IAC) at the porus acusticus. For the purposes of this chapter, the facial motor root and nervus intermedius will be collectively referred to as the facial nerve.
Intratemporal
Meatal
The facial nerve travels through the temporal bone via a bony channel, the fallopian canal . The first segment of the fallopian canal is the meatal segment or IAC. The facial nerve travels in the superior anterior aspect of the IAC. The transverse (falciform) crest separates the facial nerve from the cochlear nerve inferiorly and Bill’s bar, a lateral ridge of bone, and separates the facial nerve from the superior vestibular nerve posteriorly. Within the IAC, the nerve lacks a fibrous sheath or endoneurium and is surrounded by a thin layer of arachnoid.
Labyrinthine
Exiting the IAC, the facial nerve turns gently anteriorly within the otic capsule bone between the cochlea and superior semicircular canal into the labyrinthine segment. This portion is on average 3 to 6 mm in length—the shortest and narrowest section of the fallopian canal. In this segment, the facial nerve is at its thinnest and particularly vulnerable to injury. The vascular supply is a watershed between the terminal arterioles of the vertebrobasilar system (via the labyrinthine branch of the anterior inferior cerebellar artery [AICA]) and the external carotid artery (via the petrosal branch of the middle meningeal artery). There is also a lack of epineurium vascular plexus along the labyrinthine segment.
At the distal end of the labyrinthine segment, the nerve travels superior to the cochlea and opens into the geniculate fossa. The geniculate fossa is separated from the middle fossa floor by a thin layer of bone, which is dehiscent in about 25% of cases. Here the first fibers leave the facial nerve as the GSPN. The GSPN carries preganglionic parasympathetic innervation to the lacrimal gland and nasal mucosa. These fibers join the deep petrosal nerve from the carotid plexus to become the Vidian (or pterygoid) nerve. The thin bone above the geniculate and anterior attachment of the GSPN exerting intraneural traction place the nerve at increased risk of traumatic injury at this location. After the geniculate fossa, the facial nerve makes an acute posterior and slightly inferior turn, nearly 180 degrees, to enter the tympanic segment or horizontal segment.
Tympanic (Horizontal)
The tympanic segment is located along the medial wall of the anterior attic, travels superomedial to the cochleariform process, and forms the superior wall of the oval window niche posteriorly. On average 8 to 11 mm in length, dehiscence of the horizontal fallopian canal occurs in up to 20% of patients, with 80% above the oval window and 12% anterior to the cochleariform process. At the pyramidal eminence, the facial nerve makes a second genu anteroinferior to the lateral semicircular canal and enters the mastoid or vertical segment.
Mastoid (Vertical)
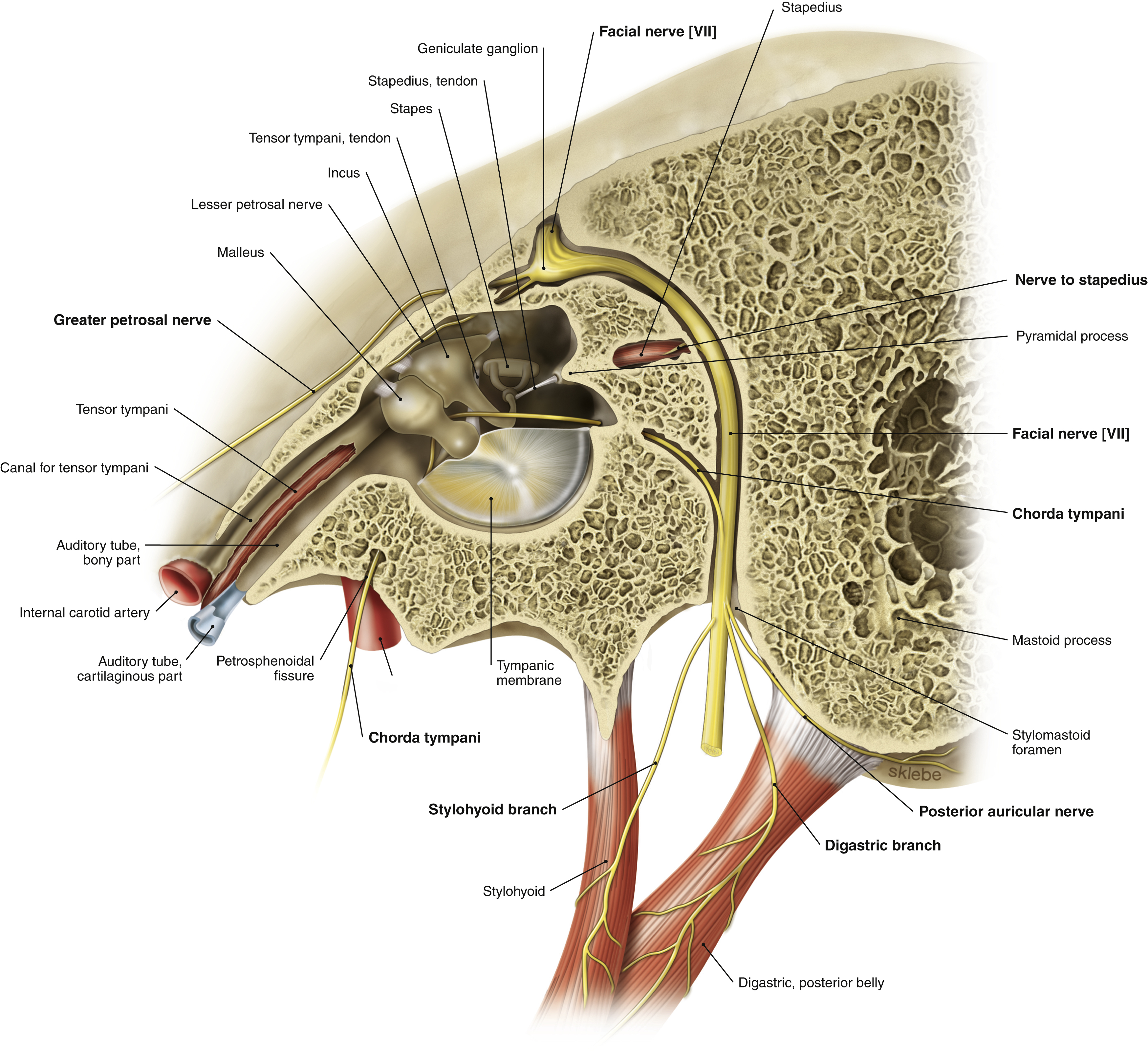
Greater anatomic variability is seen in the vertical segment prior to exiting the stylomastoid foramen than any other segment of the fallopian canal. In this segment, the facial nerve becomes more superficial as it travels within the mastoid bone. Between 9 and 18 mm in length, the mastoid segment contains the chorda tympani and stapedial branches ( Fig. 1.3 ). The chorda tympani has a variable take off from the mastoid segment but typically exits 6 mm above the stylomastoid foramen. Coursing superiorly nearly parallel to the facial nerve, the chorda angles anteriorly as it enters the mesotympanum. It exits the temporal bone via the petrotympanic fissure and joins the lingual nerve to convey taste information to the anterior two-thirds of the tongue and supplies preganglionic parasympathetic innervation to the submandibular, lingual, and minor salivary glands. This final segment ends at the stylomastoid foramen, which is lined by the aponeurosis of the posterior belly of the digastric muscle. This aponeurosis directly supplies blood to the facial nerve as it exits the fallopian canal.
Extratemporal
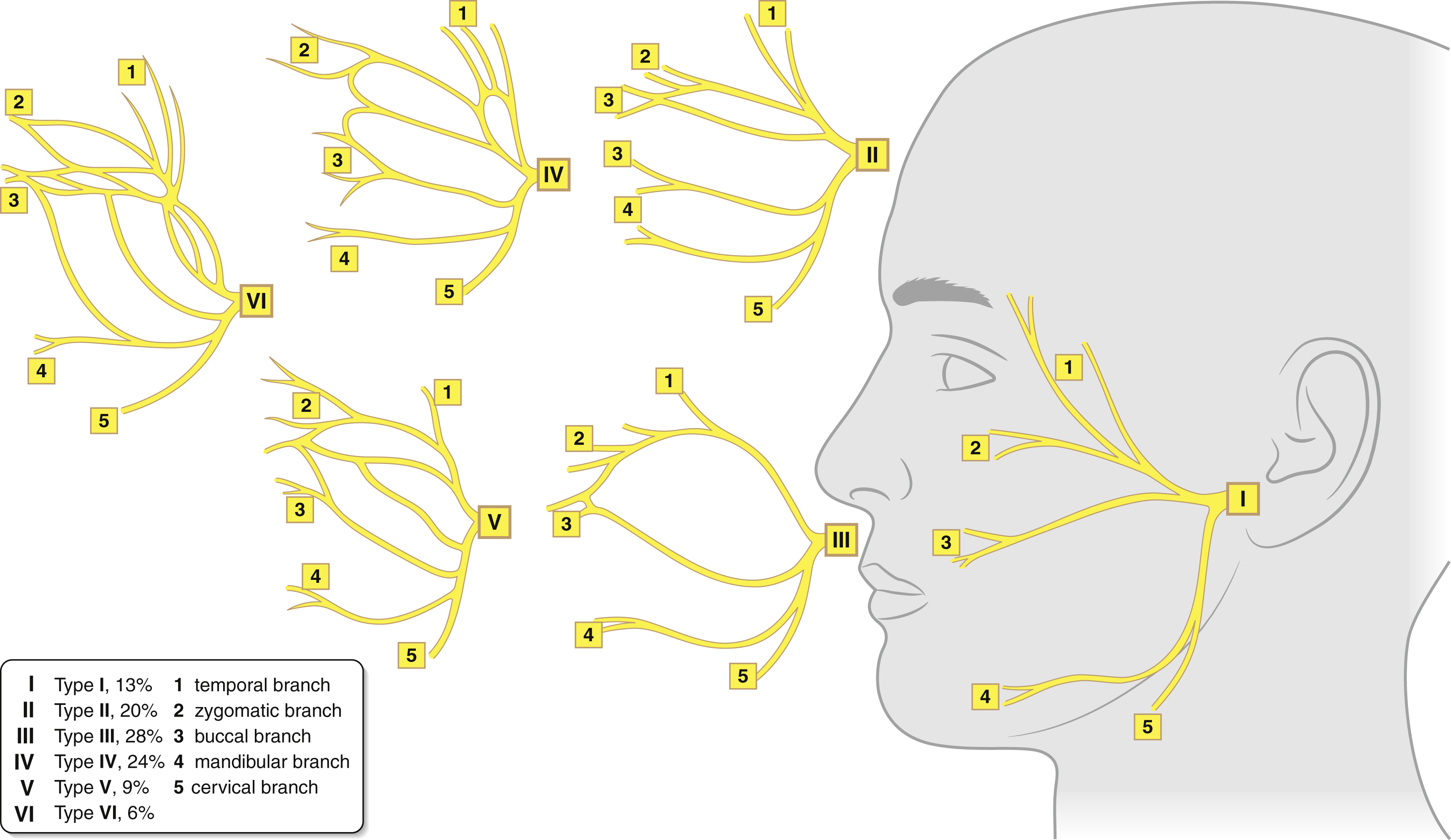
The facial nerve exits the stylomastoid foramen covered in tough connective tissue. At the stylomastoid foramen, the posterior auricular branch exits the facial nerve and supplies general sensory innervation to the posterior ear canal and concha, as well as motor innervation to the auricular muscles and occipitalis muscle. The digastric branch supplying motor innervation to the posterior belly of the digastric muscle and the stylohyoid branch to the stylohyoid muscle also exit the facial nerve prior to its entrance into the parotid gland. Within the parotid, the facial nerve branches into a larger zygomaticotemporal division and a smaller cervicomandibular division at the pes anserinus and terminates in five classic branches: temporal, zygomatic, buccal, mandibular, and cervical. In reality, the branching pattern of the facial nerve is highly variable with multiple communications and the majority of variations existing among the zygomaticobuccal divisions. Through the parotid gland, the nerve runs at the level of the retromandibular vein and separates the superficial and deep lobe of the parotid gland. As it exits the parotid, the nerve has on average 8 to 15 branches making up the five divisions ( Fig. 1.4 ). The nerve runs deep to the superficial musculoaponeurotic system (SMAS) and innervates the majority of facial muscles from their deep surface. The mentalis, buccinator, and levator anguli oris are innervated on their superficial surface as these are the deepest layer of facial muscles.
Temporal Division
The temporal division, also known as the frontal division or frontotemporal branch, consists of three to four branches traveling obliquely in between the temporoparietal fascia and the superficial layer of the deep temporal fascia. Branches entering the frontalis muscle at the level of the supraorbital ridge are located up to 3 cm above the lateral canthus. Branches entering the upper orbicularis oculi run along the undersurface for 3 to 4 mm before entering the muscle to innervate it.
One common estimate of the frontotemporal branch is Pitanguy’s line, defined by a line draw from 0.5 cm inferior to the tragus to 1.5 cm superior and lateral to the eyebrow. Numerous cadaveric studies have attempted to further define the course and branching patterns. Ishikawa demonstrated that three to four branches of the FTN were consistently found between 3.8 and 6.0 cm posterior to the lateral canthus along the superior zygomatic arch in both straight-line and curved trajectories.
Zygomaticobuccal Division
The zygomaticobuccal division consists of five to eight branches with significant overlap of muscle innervations. These nerves innervate the midfacial muscles spanning the lip elevators to the lower orbicularis oculi. Connections between the lower branches and marginal mandibular division also exist. Dorafshar et al. describe “Zucker’s point” as a reliable surface landmark for identifying the zygomaticobuccal nerve as it exits the parotid. The authors found that the midpoint of a line drawn from the root of the helix to the oral commissure predicted the nerve location within an average of 2.3 mm.
Marginal Mandibular Division
The marginal mandibular division consists of one to three branches beginning up to 2 cm below the ramus of the mandible and arcing upward to cross the mandible halfway between the angle and mental protuberance. Branches lie on the deep surface of the platysma and cross superficial to the facial vessels 3.5 cm from the parotid edge. There are separate branches to the depressor angularis, depressor labii inferioris (DLI), and mentalis, and variable superior ramus supplying upper platysma and lower orbicularis oris.
Cervical Division
The cervical division consists of one branch leaving the parotid and running on the deep surface of the platysma. The point of entry into the muscle is 2 to 3 mm caudal to the platysma muscle branch of the facial vessel. It enters the muscle at the junction of its cranial and middle thirds.
Microscopic Anatomy
The microanatomy of the facial nerve reveals a heterogenous organization that explains in part the difficulty of facial nerve repair. As described by Captier et al., the facial nerve lacks fascicular organization as well as epineural or perineural covering from its exit at the brainstem to the geniculate ganglion. Prior to the geniculate ganglion, the nerve is surrounded only by an arachnoid sheath. A thin epineural sheath arises within the tympanic segment and thickens as the nerve travels towards the stylomastoid foramen. The peri-geniculate facial nerve demonstrates one or two fascicular bundles that increase in number and decrease in size as the nerve travels distally through the fallopian canal. The number of fascicles and their spatial organization changes every 2 mm within the fallopian canal. At the stylomastoid foramen the facial nerve has on average 11 fascicles and up to 16. As individual fibers emerge, they are surrounded by perineurium and endoneurium. In the horizontal segment, the upper motor division has been reported to be more superficial (or lateral), whereas the lower motor division has been reported to lie deeper (or medial). The nerve bundles have a spatial organization as they traverse the mastoid segment: branches to the lower division lie within the anterior portion of the nerve and branches to the upper division course posteriorly within the epineurium. From the brainstem to the mastoid segment, an average of 7800 myelinated nerve fibers are maintained. A single neuron can innervate up to 25 muscle fibers.
Vascular Anatomy
The intracranial (brainstem and IAC) facial nerve receives blood supply from branches of the AICA arising from the vertebrobasilar system. The labyrinthine artery, a branch of the AICA, provides vascular input within the IAC segment. However, the remaining intratemporal segments receive blood supply through the middle meningeal artery, a branch of the maxillary artery from the external carotid. As described previously, the transition zone of vascular supply between the AICA and the external carotid centers on the labyrinthine segment and creates a watershed or weak zone of arterial supply.
The extrinsic vascular network consists of one or two main arterial trunks and accompanying venae comitantes running between the periosteum of the fallopian canal and the epineural sheath of the nerve. An intrinsic vascular network also exists within the epineurial sheath consisting of small arterioles, capillaries, and venules.
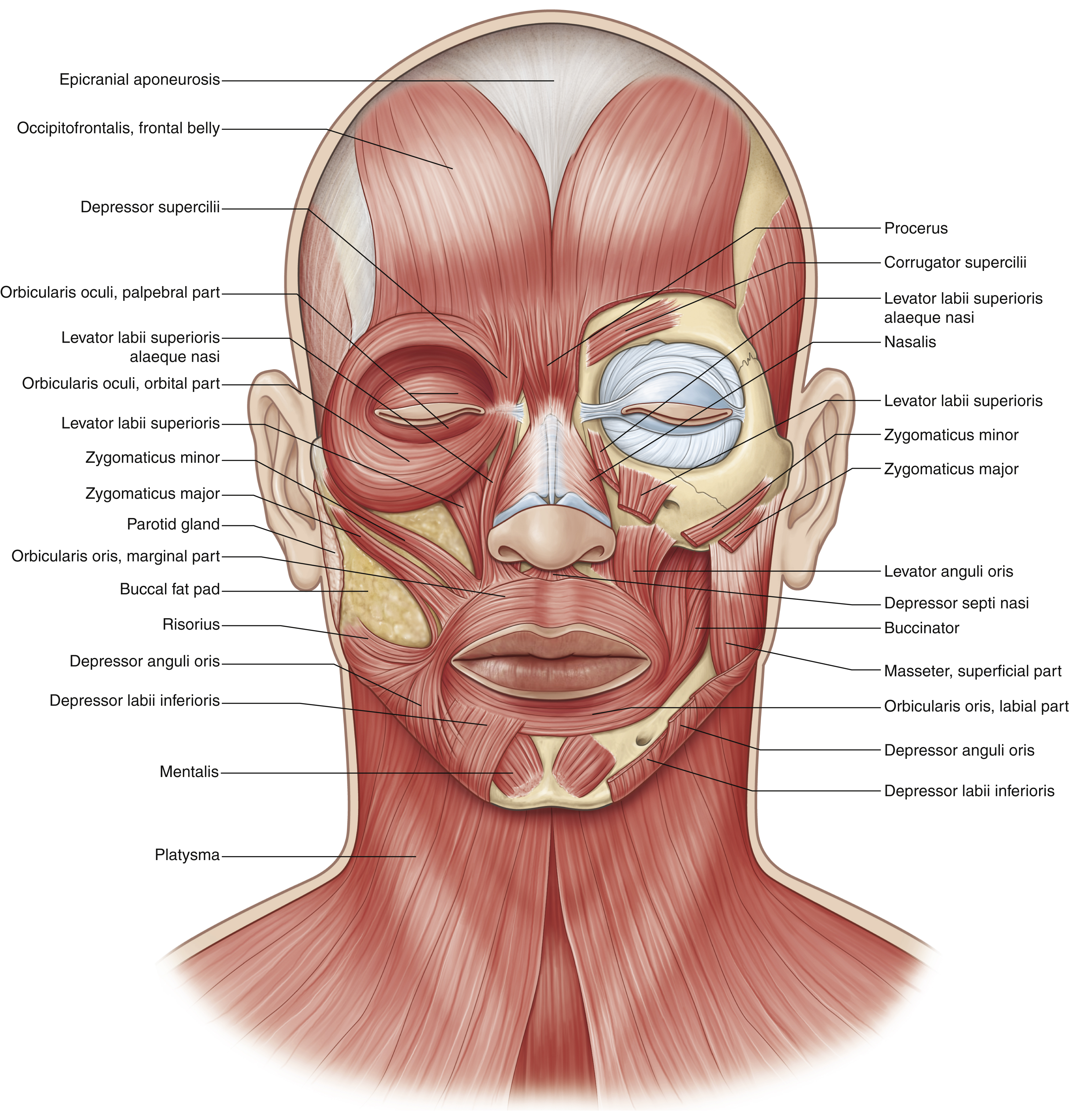
Facial Muscles
The striated muscles of facial expression derive from the second branchial arch mesoderm and reside within the SMAS layer. The SMAS layer continues superiorly with the galea aponeurotica and inferiorly with the platysma muscle. A total of 17 paired and 1 unpaired sphincter muscle constitute the facial musculature. These originate from the periosteum of the facial bones and insert into the skin, allowing for a limitless number of facial expressions ( Fig. 1.5 ).