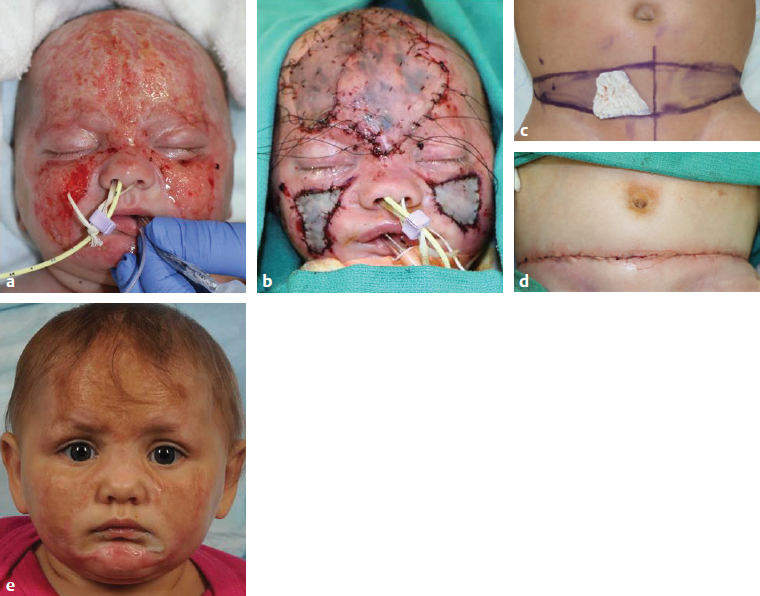
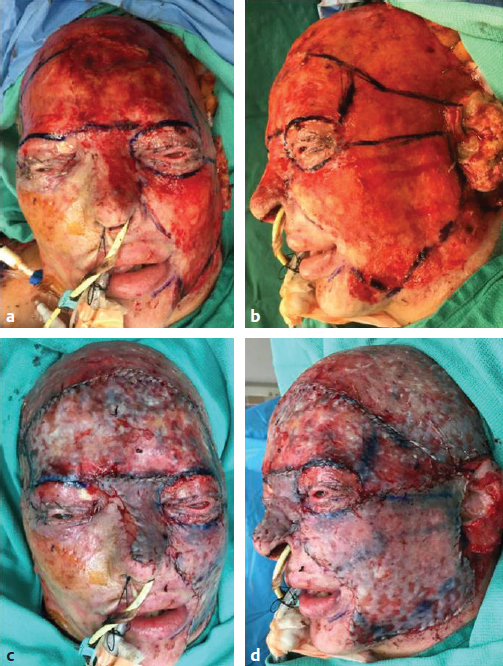
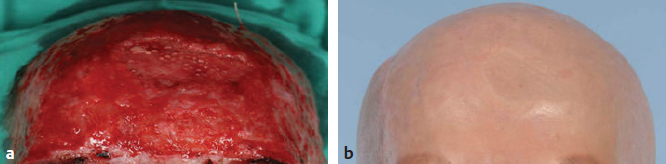
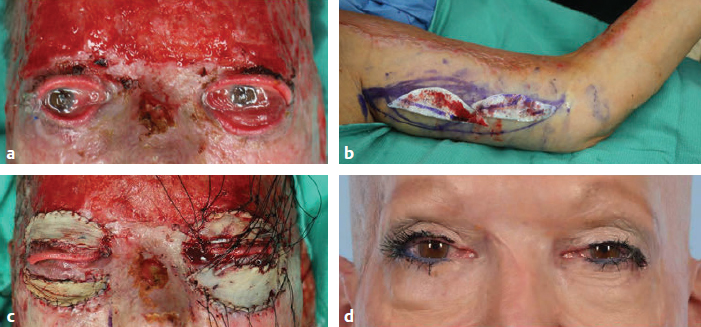
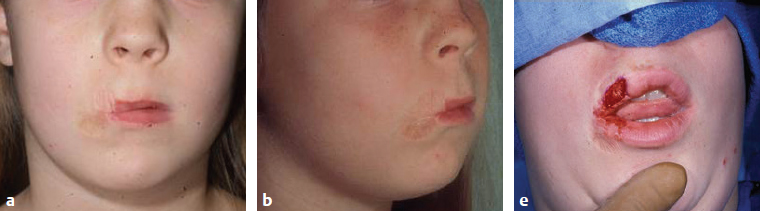
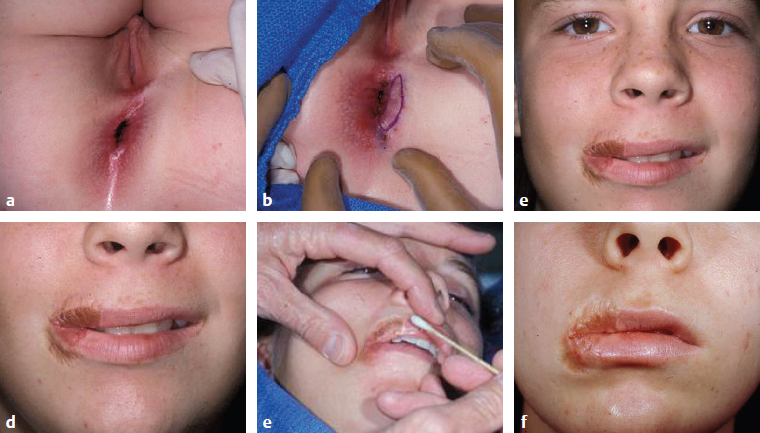
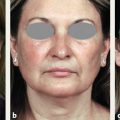
CHAPTER As improvements in the delivery of burn care and prevention resulted in greater survival of thermal injuries, patients are still left with a diverse range of challenges. These include physical, emotional, psychological, social, and religious functional impairments that often do not return to original levels even years after injury.1 These trends of delayed recovery in appearance and emotional health status are further exacerbated when injuries extend to the face.2 Thus lasting facial reconstructions are an essential focus for restoring patient quality of life and facilitating otherwise rare full recoveries to preinjury levels. In general, two main approaches are taken to burn reconstruction: (1) burn scar excision and (2) burn scar rehabilitation. Burn scar excision, especially on the face, can cause significant secondary deformities and introduce further burn scar tension, which was the reason for the original suboptimal scar. Until recently, only burn scar excision has been an option because of the lack of rehabilitative tools. The recent advent, optimization, and validation of laser treatments have revolutionized the way that plastic surgeons are able to rehabilitate burn scars of the face. Our preference is to rehabilitate scars by releasing scar tension with local tissue rearrangements and subsequent scar contour improvement with fractional carbon dioxide and pulsed-dye lasers (PDLs). We prefer to take a scar under tension, or an “unhappy scar,” and turn it into a scar without tension, or a “happy scar.” In some severe cases more invasive procedures are needed; however, surgeons must be cautious before making more incisions and creating more tension in the setting of burn scars. Summary Box Common Complications in Facial Burn Treatment • Poor graft appearance • Alopecia • Ectropion • Microstomia • Neck contracture • Graft complications Success with restoration of function and aesthetics from facial burn injury begins at the time of initial assessment. Once initial goals in terms of resuscitation are established, it is then vital to consider early inclusion of other specialties to optimize recovery. Focusing on facial burns, this includes ophthalmology if there is concern for corneal or globe injury, and otolaryngology for issues related to tympanic membrane or temporal bone fractures. The next step is determining whether the burns are superficial and can heal in less than 21 days or are full-thickness and will require excision. When large burns are being treated, facial burns are often among the first areas excised and grafted given their importance in function and appearance (Fig. 69.1). Fig. 69.1 Avoidance of complications from facial burns is contingent on proper identification of facial subunits requiring débridement and grafting. (a–d) This patient’s scalp, forehead, and cheeks were grafted from abdominal donor sites. (e) These areas recovered well, whereas omitted regions (chin) developed hypertrophic scarring and contracture. Facial areas that will not reepithelialize should be débrided within the first 10 days from the time of injury. They can be temporized with allograft for either future dermal substitutes or autografts. By placing a temporary skin substitute like allograft, the surgeon can learn which areas were débrided to the proper depth by looking at which areas have good allograft take. After approximately 5 days, once the allograft can be assessed for adequate débridement, the wound can be autografted using facial subunits (Fig. 69.2a,b). Then, at the second operation, regions with inadequate allograft should be débrided further, and areas with good take do not require further débridement. Often surgeons are hesitant to débride the face; however, failure to do so can lead to severe hypertrophic scarring and functional deficits such as ectropion and microstomia, which are difficult if not impossible to correct in the future. Deep burns that extend beyond underlying bone require further débridement through the cortex of the facial skeleton (Fig. 69.2c,d) to ensure the survival of local skin grafts, a process similar to documented protocols for calvarial burn injuries.3 For smaller areas, full-thickness grafts can be selected to decrease the effect of contracture, and for larger areas split-thickness grafts of .018 to .025 inches thick in adults and .008 to .012 inches thick in children can be applied.4 Consideration of facial subunits should also play into autograft design, but excision of additional tissue to conform to facial subunits is controversial. Optimal outcomes are also contingent upon appropriate selection of donor sites based on matching physical characteristics such as color, contours, and dermal thickness as well as underlying histology. Whereas local nearby donor sites are ideal, they are often scarce resources and commonly cannot support the entirety of a recipient site. Remote graft donor sites have been already identified as suitable candidates for a number of recipient sites and facial subunits.5 Sheet grafts or full-thickness grafts tend to have better aesthetic outcomes on the face, and meshed grafts should be avoided. Sheet grafts require close monitoring to ensure excellent take. The two most common reasons for graft failure are inadequate débridement and hematoma formation. To minimize the risk of hematomas resulting in graft loss, small openings in the skin graft can be created to drain any blood from beneath the graft; this is commonly done with a small needle (such as a 21- or 25-gauge) or no. 15 blade. Alternatively, very small holes can be made in the graft to allow egression of fluid, but one concern with “pie crusting” the graft is that they can heal with more prominent scars in that location. Fluid can be rolled out using cotton-tipped applicators; one trick is to use plastic ones, such as those used for culture swabs, because the shaft can be bent and used to roll along uneven surfaces on the face quite well. Another option is to fit the patient with a compression garment for the face to help minimize this risk. Monitoring these skin grafts on at least a daily basis for the first few days, until no further blood or fluid accumulates beneath it, helps ensure superior outcomes. For full-face grafts, some surgeons have also advocated sedation on the ventilator for around 5 to 7 days to allow for initial skin graft adherence to the wound bed. Fig. 69.2 (a,b) Recipient sites for autograft must respect facial subunits. After appropriate demarcations, early interventions include débridement of allograft, bilateral tarsorrhaphies to prevent lid contractures, and sheet grafts to facial subunits. (c,d) Second operations may require further débridement of regions with inadequate take, with additional bone débridement in deep burns. An Integra dermal regeneration template applied to the frontal scalp for a healthier wound bed is conducive to successive graft survival. It is important to avoid full-thickness excisions to avoid burn wound alopecia. In addition, when using the scalp as a donor site, it is crucial not to harvest a graft that is too thick to avoid removing the follicles. Offloading the patient from putting pressure on one region of the scalp will also help prevent alopecia. Early tarsorrhaphy, both temporary and permanent, is central to combatting the burn wound contractures that often pull on the lower lid. In addition, early débridement and grafting is central to decreasing the burn scar contracture force on the lower lid. If burn wound ectropion is present despite these measures, early tarsorrhaphy, canthoplasty, and midfacelift will add additional support to the lower lid (Fig. 69.3). A lateral canthotomy and canthoplasty should be performed to counteract the inferior pull of the burn scar. The surgeon should suspend the lateral canthus from the periosteum at the level of the upper limbus, making sure to overcorrect. The midfacelift can be performed through a lateral canthotomy incision. Dissection should be carried down below the infraorbital rim, taking care not to injure the infraorbital nerve by dissecting medial and lateral to this. The medial cheek adipose tissue should be suspended laterally from the periosteum providing support. After these steps a tarsorrhaphy should be performed.6 If severe ectropion is present a permanent tarsorrhaphy is performed. If minor ectropion is present and the goal is to temporarily offload the tension, a temporary tarsorrhaphy is placed (see Fig. 69.2a,b). In general, external burns do not require treatment of the internal lamella. The upper lid can often be treated with débridement and grafting alone given the decreased vector on the lid. Like ectropion, microstomia is extremely difficult to correct once it occurs, and thus prevention is crucial. Occupational therapy is the most important step to prevent microstomia early after a burn. In addition, early débridement and full-thickness grafts that take into account the facial subunits are key to preventing microstomia. Along with axillary contractures, neck contractures are one of the most common and challenging contractures encountered after burn injury. As in other regions, early débridement and grafting is important to prevent healing by secondary contracture and subsequent neck contracture. Concurrently, aggressive occupational therapy and nighttime splinting with a C-collar can help combat the pull on the neck. In the subacute setting, release and full-thickness grafting can be performed with release of the platysma. The release should be placed in a region that divides the facial subunits, such as at the junction of the chin and neck subunits. Postoperative splinting and early range of motion are crucial to preventing recurrent neck contractures. Surgical wound infections and incomplete excision of the underlying wound bed of the recipient site can lead to skin graft failures and burn wound contractures.4 For patients in whom infection and structural complications are controlled, grafts still are prone to contour defects and color mismatch.7 When grafting to the face, grafts must come from regions above the clavicles or on the inner arm if available to decrease hyperpigmentation. The surgeon should also be mindful of moving skin from hair-bearing regions to the face, especially in wounds. These irregular contours and erythema can be significantly reduced through ablative laser therapy. Furthermore, residual hypertrophic scars from prior untreated facial subunits and grafts themselves traditionally addressed by more invasive protocols such as excision are also amenable to more efficient ablative laser therapies.8 Ablative laser therapies provide the essential complementary strategy in optimizing facial burn injury management. Burn wounds of the forehead and eyelid ectropion are addressed similarly, sourcing grafts from the upper arm or supraclavicular area. Unique considerations related to the large surface area of the forehead include the use of a thick split-thickness graft under significant tension and grafting into the hairlines to hide borders that may be visible because of difficulty in matching color and textures.9 Further complicating scalp reconstruction are the unique layers contiguous to the skin in this region, particularly the aponeurosis galea of the anterior and posterior aspects of the cranium. Skin grafts in this region are particularly vulnerable, requiring healthy periosteum underneath for successful graft survival.10 External tissue expansion devices offer an alternate strategy for primary closure for reconstruction of this complex region.11 In addition, burring of the outer cortex and the use of Integra dermal regeneration matrix can help build up an appropriate wound bed for future grafting (Fig. 69.4). Additionally, with regards to eyebrows, the surgeon should avoid débridement of hair-bearing areas if possible. If this is not possible, future reconstruction with occipital grafts can be performed. When using these grafts, the surgeon must make sure to orient the hair in the proper direction. Fig. 69.4 (a) Severe deep burns may require cortical débridement and Integra placement to maximize successful graft survival. (b) Postoperative result. Fig. 69.5 (a) Burn wound ectropion leave the globe vulnerable to corneal damage. The anterior and posterior lamellae must be evaluated and addressed individually. (b) Full-thickness grafts from the inner arm destined for periorbital tissues. (c) Full-thickness grafts from the inner arm provide the best color matching for periorbital grafts. (d) The postoperative result. Burn wound ectropion leaves the globe vulnerable to corneal damage and potential future ophthalmic complications (Fig. 69.5a). Evaluation of the defect is based on whether it involves the anterior and posterior lamellae. Most flame burns affect the anterior lamella, whereas splash chemical burns may damage the anterior and posterior lamella. Anterior lamella structures including skin and the orbicularis oculi muscle along with the tarsal plates of the posterior lamella must be both addressed and structurally suspended. Anterior lamellar reconstruction relies on skin grafts, and the best match for eyelid defects usually comes from upper eyelid skin and is removed with traditional blepharoplasty techniques. For larger areas, full-thickness grafts from the inner arm (Fig. 69.5b) and supraclavicular regions were used for ectropion release to provide the best color matching for the periorbital tissues (Fig. 69.5c,d). At the same time, the surgeon must pay attention to supporting the lids to prevent corneal abrasions. Concurrent support procedures at the time of release and full-thickness grafts include a midfacelift and temporary or permanent tarsorrhaphy. For reconstruction of the posterior lamellae, retroauricular grafts and palatal grafts can also be applied to reconstruct the tarsal plate. Palatal grafts offer the benefit of a strong support. Lateral canthoplasties restore the physiological upward slant typically seen in an open eye and help fight the pull of the burn on the lower lid.12 For smaller defects in periorbital volume, fat autografting injections have recovered contours previously deformed by soft tissue atrophy or scar adhesions.13 Early treatment of the nose should focus on minimizing alar necrosis, which can be exacerbated by feeding tubes or nasogastric tubes. Also, if nasal mucosa is burned, early stenting can prevent intranasal contracture. Nasal reconstruction relies on accurate assessment of the skin, cartilaginous and bony support, and lining. The inner lining is usually provided by septal hinge flaps that can be used from the unilateral or contralateral side. The cartilage graft can be harvested from the septum or concha of the ear. The outer lining can be covered with a nasolabial, bilobe, or forehead flap, as are used in Mohs’ reconstruction. Often, however, these donor sites have been grafted, making their use more challenging. If using a previously grafted local flap, delay of the flap may decrease flap necrosis. Other distant alternatives include free tissue transfer. Composite grafts from the ear including the helical root and preauricular area have been histologically demonstrated to most closely resemble nasal dermal thickness and density of pilosebaceous units.5 When the ear is not available as a donor site, a three-unit construction sourcing inner and outer linings from the nasal septa and nasolabial folds with cartilage from the ear can be used to reconstruct the asymmetrical ala. Alternatives when no donor sites are available include the nasal turndown flap.14 Contractions of the lips produce eversion and exposure of the vermilion borders, which can manifest functional deficits and exposure of teeth. Early occupational or physical therapy to minimize contracture is crucial. The degree of lip eversion is often influenced by contractures of neighboring facial subunits, particularly the nose and chin. Further restrictions in oral function found contractures are commonly excised or lengthened with z-plasty.9 Contractures causing exposure of the wet vermilion are resolved through release grafts in the affected subunits (Fig. 69.6), such as the chin or nasolabial folds. Intraoral flaps such as tongue flaps are helpful for contracture of the commissure.15 The facial artery myomucosal (FAMM) flap is also an option for commissure or vermilion reconstruction. Issues with patient compliance pose challenges for use of this flap in pediatric patients, and less-invasive options are usually effective. When treating lip contractures acutely, it is important to take the subunits into account. In addition, it is crucial to avoid using skin to replace the lip vermilion, because this will cause a distorted appearance. The vermilion can be replaced with the other lip if it is not burned with an Abbé flap. Alternatively, the anal verge serves as a distant site to harvest transitional epithelium for a graft (Fig. 69.7a–c). Subsequent phenol peel of the anal verge skin graft can help refine pigmentation mismatch (Fig. 69.7d–f). Fig. 69.6 (a,b) Contractures causing microstomia and exposures of wet vermilion are resolved through release grafts. (c) An upper lip defect after release of the upper lip scar. Fig. 69.7 (a) The anal verge. (b) An area is marked out for full-thickness skin graft harvest in the region of the transitional epithelium. (c) The 2-year postoperative image demonstrates improved symmetry but noticeable hyperpigmentation. (d–f) Time-lapse series of phenol peel treatment on hyperpigmentation secondary to anal verge skin graft.
69
Facial Burns
Avoiding Complications during the Acute Burn Phase of the Face
 Graft failure
Graft failure
 Contracture
Contracture
 Contour defects
Contour defects
 Erythema
Erythema
 Hyperpigmentation
Hyperpigmentation
Poor Graft Appearance
Alopecia
Ectropion
Microstomia
Neck Contractures
Graft Complications
Facial Subunits
Forehead and Scalp
Eyelids
Nose
Lips
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree