Periorbital Synkinesis
Background
Eyelid paralysis, related to facial nerve injury, is a debilitating condition that causes significant functional impairment and cosmetic disfigurement. The most common eyelid and ocular sequelae resulting from facial paralysis include upper and lower lid retraction, lagophthalmos, exposure keratopathy, ectropion, ocular discomfort, visual deficit, and epiphora. Some of these changes can also contribute to corneal decompensation and psychosocial detriment. An additional potential long-term sequela is synkinesis due to aberrant regeneration of the facial nerve which can lead to differing cosmetic and functional impairments.
In non- or partially recovered eyelid paralysis with reduced neural input, the orbicularis muscle tone is deficient, which is what underlies the physical findings. This paralytic component, with resultant lack of orbicularis contraction, can lead to secondary cicatricial changes, manifesting as anterior lamellar shortage.
The upper eyelid has two retractors (levator aponeurosis and Mueller’s muscle) and a single protractor (orbicularis oculi). These two opposing muscle groups are in a state of equilibrium, which controls the upper lid position. In paralysis patients, eyelid position favors the retractors and the upper lid elevates and eyelid closure is reduced. In the lower eyelid, the orbicularis muscle provides resting tone to maintain eyelid position. Eyelid position is further maintained by supportive soft tissue structures including the tarsus and canthal tendons. The dynamic upward forces of these structures are in equilibrium versus gravity. As the orbicularis weakens in eyelid paralysis patients, unopposed gravitational pull leads to lower lid retraction and development of ectropion. The severity of the symptoms and clinical presentations of eyelid palsy depends on the varying changes of the upper and lower eyelid function.
The orbicularis oculi muscle also serves as a tear pump and thus contributes to tear film stability, which has an important protective role for the cornea and refractive role for visual acuity optimization. With paralysis, the upper and lower eyelid blink function is weakened. This can trigger symptoms related to tear film instability including tearing, red eyes, foreign body sensation, visual acuity fluctuations, and corneal breakdown or scarring. These latter issues can lead to permanent vision loss in severe cases of exposure keratopathy.
Although most of the literature has focused on managing complications related to acute and complete eyelid paralysis, many patients present with post-facial paralysis synkinesis, which can develop following any form of facial nerve injury. Although the exact mechanism of synkinesis is unknown, the most widely accepted theory is that of aberrant regeneration of axons at the site of injury. Newly sprouted or misdirected axons reinnervate both original and inappropriate facial muscles. This results in the involuntary contraction of muscles during volitional movement of another muscle group. Eyelid manifestations of synkinesis are therefore very different from acute or irreversible orbicularis deficit, as these patients develop no muscle weakness, but rather increased muscle tone.
One of the most common manifestations of synkinesis is involuntary eye closure with smiling, known as oral-ocular synkinesis. As opposed to the ocular symptoms associated with the paralytic component of eyelid paralysis, patients with synkinesis experience a different set of symptoms related to increased dynamic muscle tone. This in itself leads to functional impairment and cosmetic deformity which can significantly impact one’s quality of life. , Ocular synkinesis can manifest as excessive narrowing of eyelid aperture, pain, twitching, fatigue, or gustatory lacrimation that can be very distressing to the patient.
The degree of synkinesis may vary from slight asymmetry to significant deformity and severity often depends on the etiology and the grade of paralysis at onset. , Thorough evaluation and understanding of the patient’s disease process is crucial to counseling and treatment. Multiple tools for evaluation are available; however, there is no one reliable, validated measure to assess patients over time. Therapeutic measures for the treatment of synkinesis include physiotherapy, neuromodulation, and surgery. Management of ocular synkinesis is often challenging and optimal treatment can be limited.
Given the risk of adverse ocular consequences with facial palsy, appropriate management of the associated eyelid and ocular sequelae of this disease requires a thorough understanding of the biomechanics of eyelid function as well as facial anatomy and topography.
Anatomy
The eyelids are a delicate, intricate structure composed of three distinct lamellae: (1) anterior—composed of thin skin and the orbicularis oculi muscle; (2) middle—defined by the orbital septum; and (3) posterior—made up of conjunctiva tarsus and retractors depending on topographic location on the eyelid. Eyelid closure is mediated in both the upper and lower eyelids by the orbicularis oculi muscle, the sole protractor of the eyelids.
The orbicularis oculi is a concentric muscle which, depending on its subdivision, originates and inserts on the orbital rim, lateral raphe, or canthi. As it is a circular sphincter, it requires counter fixation at the canthi to allow appropriate vertical eyelid excursion. The muscle can be divided into three concentric sections: the pretarsal, preseptal, and orbital portions. The pretarsal orbicularis lies above and is densely attached to the tarsus. It continues to the lid margin as the “gray line” or muscle of Riolan. Along with the preseptal orbicularis, it contributes to involuntary blinking, which is often compromised and difficult to treat in facial paralysis. The orbital portion of the orbicularis is the largest segment of the muscle and controls voluntary eyelid closure as well as medial and lateral brow depression.
Both the pretarsal and preseptal orbicularis contribute to the lacrimal pump mechanism for tear drainage. As the eyelids close, the orbicularis muscle contracts. The pretarsal component compresses the canaliculi, driving tears to the lacrimal sac. As the preseptal orbicularis (which inserts into the lacrimal sac) contracts, it expands the lacrimal sac, creating a negative pressure that draws the tears into the sac. As the eyelid opens, the orbicularis muscle relaxes, which in turn opens the puncta, collapses the lacrimal sac, and the cycle repeats. Optimal function of the pretarsal and preseptal orbicularis is required to ensure patients do not have tearing issues.
The eyelids are anchored medially and laterally by the medial and lateral canthal tendons. The medial canthal tendon is formed by fibrous extensions of the orbicularis muscle and has both an anterior and posterior crura which attach to the anterior and posterior lacrimal crests, respectively. The anterior lacrimal crest is an extension of the frontal process of maxilla and the posterior lacrimal crest is part of the lacrimal bone. The lateral canthal tendon is similarly formed by fibrous extensions of the orbicularis muscle from the tarsal plate to the lateral orbital rim, and also has anterior and posterior crura. The anterior crus attaches to the anterior orbital rim, whereas the posterior crus attaches to the Whitnall tubercle, a bony prominence 3 mm posterior to the lateral orbital rim, and 10 mm below the frontozygomatic suture. There are four anatomic structures that attach to the Whitnall tubercle and include the lateral rectus check ligament, the levator aponeurosis, the Lockwood suspensory ligament, and the lateral canthal tendon. In addition, the lateral canthal tendon sits approximately 2 mm higher than the medial canthal tendon. This is known as the normal canthal tilt. It is critical to recreate the natural attachment of the lateral canthal tendon in surgery to ensure appropriate lid to globe apposition and maintain the vector and length of the horizontal palpebral fissure.
Clinical Examination
The next sections describe an algorithmic approach to examining a patient with facial palsy and synkinesis.
Ocular Examination
A thorough examination to assess ocular health and the tear film is important prior to performing any surgery. The authors recommend starting by assessing the corneal protective mechanisms (points 1 to 4 below) of the eye, and a slit lamp examination. These are described in the following section.
Corneal Protective Mechanisms
- 1.
Corneal sensation: Corneal sensation is assessed without placement of a topical anesthetic drop. A cotton tip applicator is used to create a small wick and the examiner gently touches the cornea. This should illicit an involuntary blink bilaterally when the corneal reflex is intact. A formal esthesiometer can also be used, although many examiners would likely not have this tool readily available in their office. Lack of or diminished corneal sensation results in reduced pain sensation. This in turn can lead to the progression of corneal exposure and predisposes to a greater risk for development of keratopathy and vision loss.
- 2.
Bell’s reflex: The Bell’s reflex is defined as an upward rotation of the globe upon eye closure. It serves to protect the cornea during eyelid closure. This is evaluated by asking the patient to close their eyes while the examiner forcefully opens the eye and assesses the globe position. An intact Bell’s reflex suggests the cornea is more protected especially at night as it is not exposed to the external environment. Of note, approximately 25% of the general population does not have a Bell’s reflex. In eyelid paralysis patients, an intact Bell’s reflex is critical to corneal protection.
- 3.
Tear film: Tear film quantity and quality can be assessed by performing a Schirmer test and a slit lamp examination. The Schirmer test measures tear production. It can be performed with or without topical anesthetic depending on whether basal (baseline) or reflex tear production is being measured. To assess basal tear production, a drop of topical anesthetic is placed in the eye. An absorbent filter strip with markings is placed in the inferior fornix. The distance of strip wetting is measured after 5 minutes. An abnormal test will demonstrate less than 10 mm of tear production. Baseline tear production is critical to a continued wetting of the corneal surface. Further, tear breakup time (TBUT), defined as the interval between the last complete blink and the first appearance of a dry spot or disruption in the tear film, is another objective measurement to document tear film quality (abnormal is < 10 seconds). Poor tear quality can also predispose to corneal breakdown even if the quantity of tears is sufficient.
- 4.
Orbicularis function: As described previously, the orbicularis muscle primarily functions as an eyelid protractor to close the eyes. When this is deficient, the globe is less protected. The subjective method of measuring function with attempted eyelid opening against forced closure was described previously.
Slit lamp examination: Lastly, a slit lamp examination should be performed to assess for any corneal breakdown or scarring, and abnormalities of tear quality. Significant corneal decompensation may warrant more urgent surgical management. Working in conjunction with a local ophthalmologist who can co-manage ocular health is extremely important if such tools are not readily accessible.
Besides corneal protective mechanisms, other critical examination points are required to help guide surgical and nonsurgical planning. Each part of this examination is meant to paint an overall qualitative clinical picture of the severity of paralysis and the potential interventions to help improve the biomechanical function of the paretic lid.
- 1.
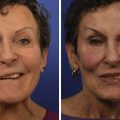
Lid closure: Lagophthalmos is defined as the inability to close the eyelids. It can be caused by a retracted upper and/or lower eyelid and is often present in eyelid paralysis patients. Its treatment will depend on the eyelid position and strength. Conversely, patients with post-facial paralysis synkinesis may have excessive closure upon activation of smile mechanism which may impair vision and cause cosmetic deformity ( Fig. 10.1 ). A complete evaluation of eyelid activity should include asking patients to animate their face.

Fig. 10.1
A patient with oral-ocular synkinesis who demonstrates excessive closure upon activation of smile mechanism on the left side. (Courtesy of Facial Paralysis Institute.)
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree